
5 Steps to Handle Prior Authorizations for Your Mental Health Clinic
Introduction
Navigating the intricate landscape of prior authorizations has become increasingly vital for mental health clinics as insurance requirements continue to evolve. Effectively managing this process not only guarantees that patients receive timely care but also shields clinics from unforeseen financial burdens. Projections suggest that nearly half of mental health services will necessitate prior approval by 2026. This raises a critical question: how can clinics streamline this often cumbersome process while upholding high standards of patient care?
Understand Prior Authorization Requirements
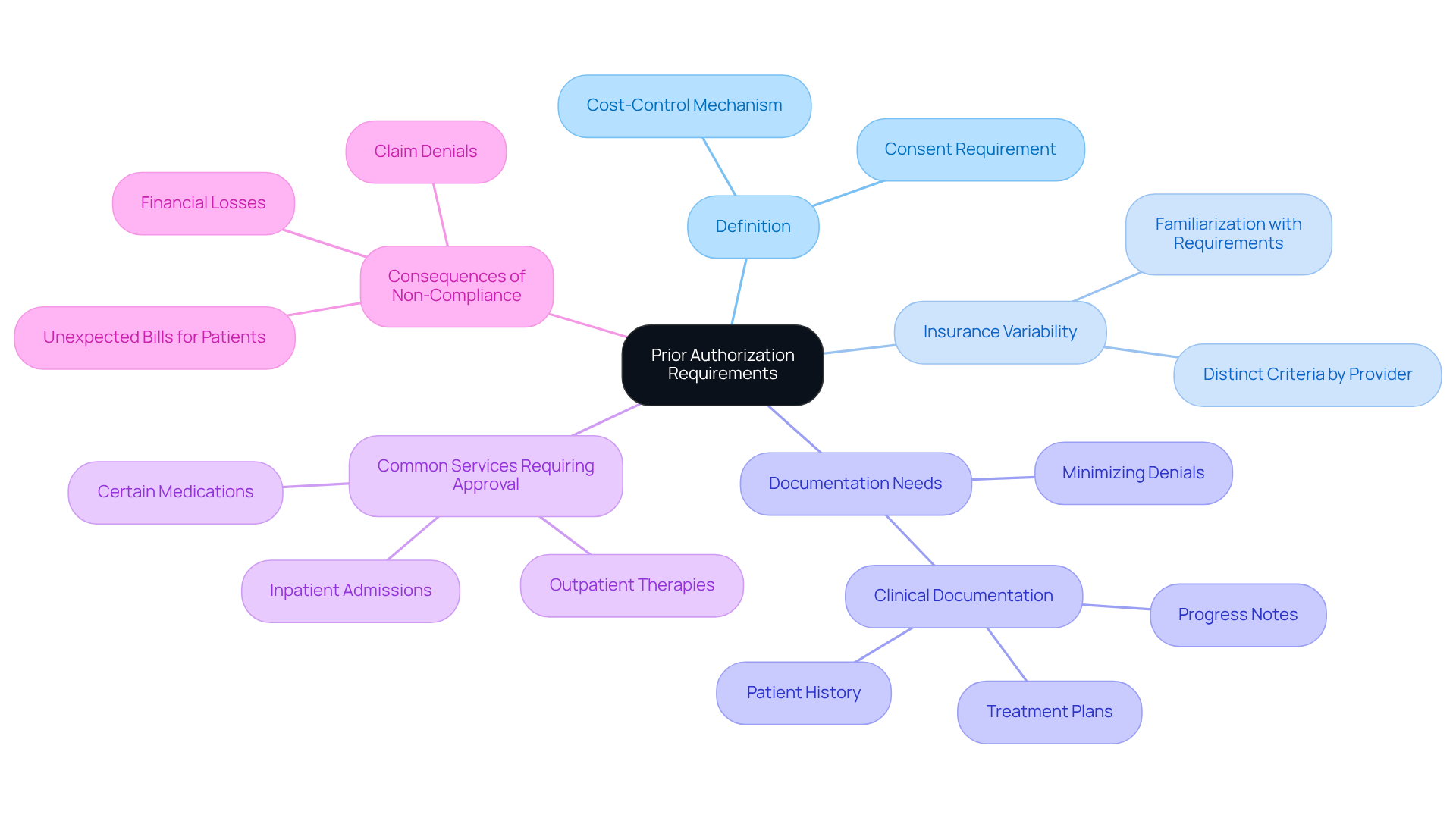
Prior approval is a critical procedure utilized by insurers to evaluate coverage for specific treatments or procedures prior to their delivery. For mental health facilities, knowing how to handle prior authorizations is vital to ensure that patients receive necessary care without encountering unexpected costs. The following are key components to consider:
- Definition: Prior approval serves as a cost-control mechanism, requiring healthcare providers to secure consent from the insurer before delivering certain services.
- Insurance Variability: Each insurance provider establishes distinct criteria for prior approval. It is essential to familiarize yourself with the specific requirements set by each insurer your clinic partners with.
- Documentation Needs: Insurers generally require clinical documentation that validates the medical necessity of the proposed treatment. This documentation may include patient history, treatment plans, and progress notes. Healthcare Partners Consulting specializes in ensuring that all requisite documentation is accurately collected and submitted, thereby minimizing the risk of denials.
- Common Services Requiring Approval: Services such as inpatient admissions, specific outpatient therapies, and certain medications often necessitate prior approval. Awareness of which services are affected can significantly streamline the process. Our team at Healthcare Partners Consulting excels at identifying these services and managing the approval process efficiently.
- Consequences of Non-Compliance: Neglecting to obtain necessary approval can result in claim denials, leading to financial losses for the clinic and unexpected bills for patients. Understanding how to handle prior authorizations is crucial to mitigate such risks. Our comprehensive denial management solutions ensure that coding, timely filing, and medical necessity are effectively addressed, thereby reducing the likelihood of denials.
By 2026, it is projected that approximately 50% of mental health services will require prior approval, underscoring the importance of staying informed about evolving insurance protocols. As emphasized by healthcare experts, understanding prior approval requirements is essential for ensuring timely patient care and alleviating administrative burdens. The successful implementation of these processes can enhance operational efficiency and improve patient outcomes.
Check Client Eligibility for Prior Authorization
To ensure your clients are eligible for prior authorization, adhere to the following essential steps:
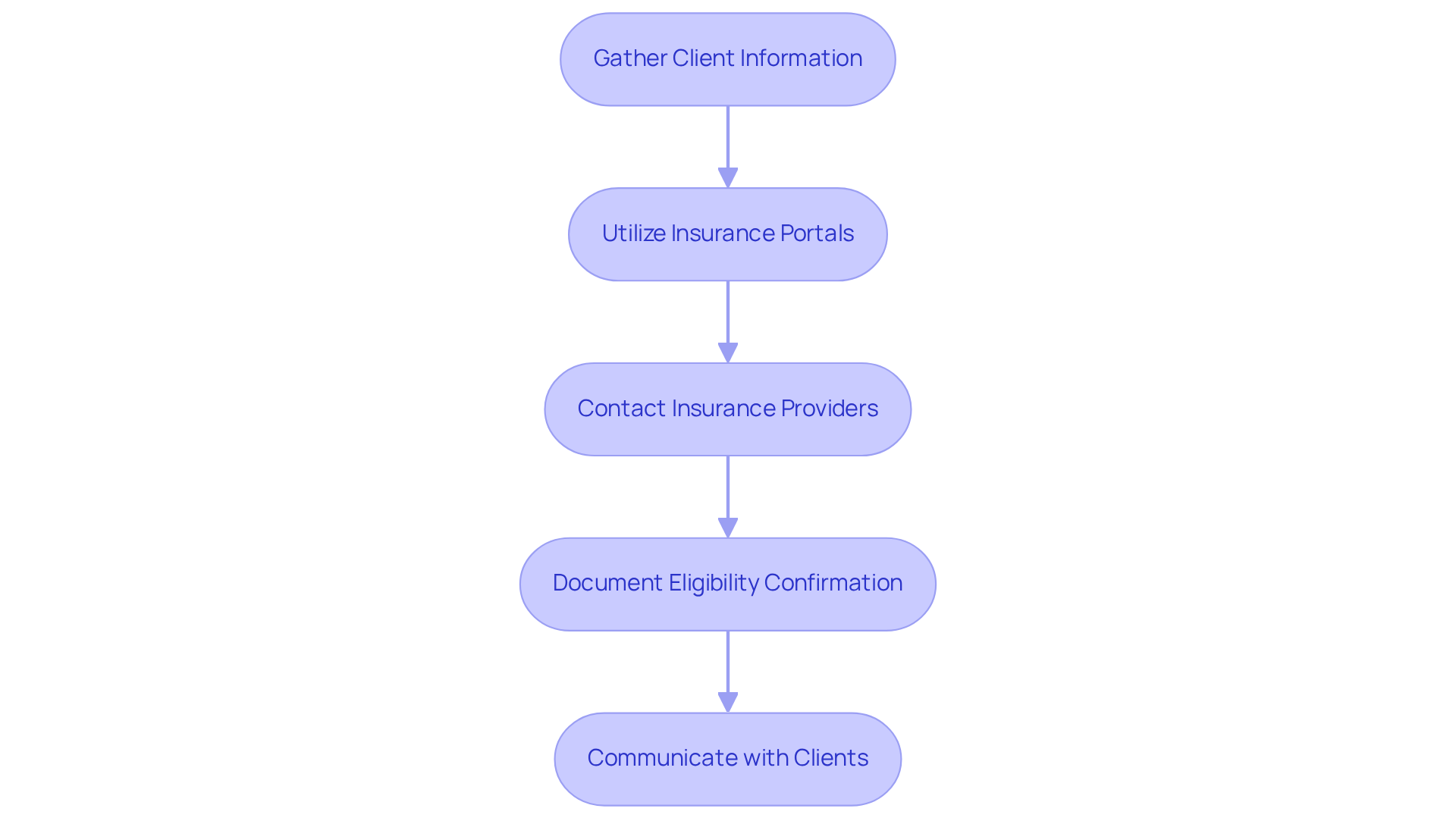
- Gather Client Information: Collect all necessary details, including the client's coverage information, policy number, and the specific services they require.
- Utilize Insurance Portals: Approximately 94% of verifications are now conducted electronically, many in real time. Most providers offer online portals for checking client eligibility. Log in to the portal and input the required information to verify coverage efficiently.
- Contact Insurance Providers: If online verification is not feasible, contact the insurance company directly. Be prepared to provide the client's information and inquire about coverage for the requested services. A single verification call may take up to 20 minutes or longer due to extended hold times, so plan accordingly.
- Document Eligibility Confirmation: Maintain a detailed record of the eligibility verification process, including dates, names of representatives spoken to, and any reference numbers provided. This documentation is vital for addressing any issues that may arise later, as 20% of all medical claim denials are attributed to eligibility or registration errors.
- Communicate with Clients: Inform clients about their eligibility status and any potential out-of-pocket costs they may incur. Clear communication is essential for managing expectations and fostering trust, especially when it comes to how to handle prior authorizations, which is crucial for sustaining strong client relationships.
Determine Service or Code Requirements for Prior Authorization
Recognizing the specific processes or codes requiring initial approval is crucial for a seamless procedure. Here’s how to approach this task:
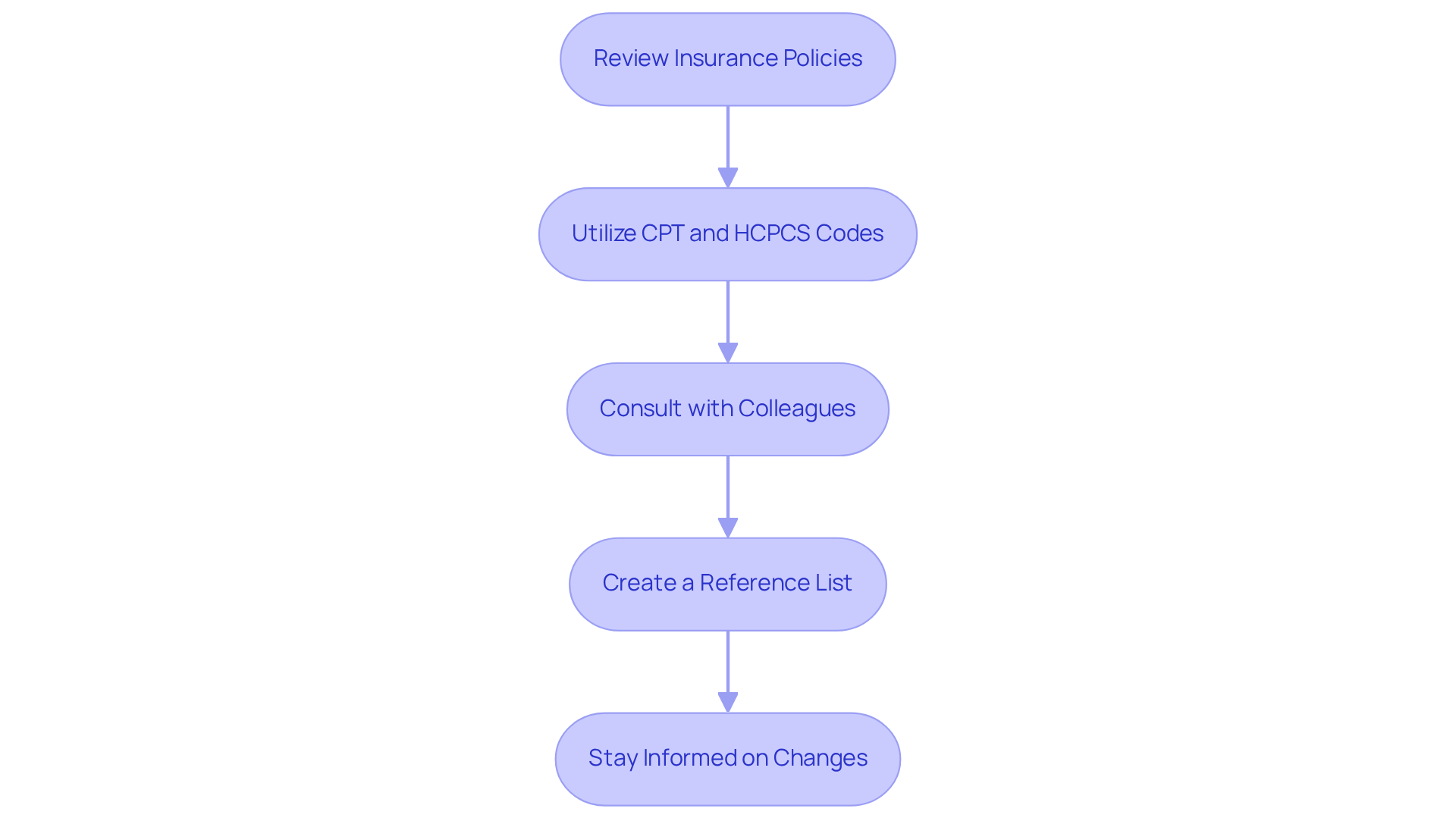
- Review Insurance Policies: Each insurance provider maintains a list of offerings that necessitate prior approval. Regularly reviewing these guidelines ensures you stay informed about any updates.
- Utilize CPT and HCPCS Codes: Familiarize yourself with the Current Procedural Terminology (CPT) and Healthcare Common Procedure Coding System (HCPCS) codes relevant to mental health services. Many insurers mandate specific codes for approval, making this knowledge essential. For instance, CPT codes such as 90834 and 90837 are frequently used for therapy sessions requiring advance approval.
- Consult with Colleagues: Collaborate with other mental health professionals or billing specialists to exchange insights on which offerings typically need advance approval. Jasmine Oliver, a Revenue Cycle Management Expert, emphasizes, "Networking can yield valuable information that enhances your understanding of the process."
- Create a Reference List: Compile a comprehensive list of services and their associated codes that require approval for each provider you work with. This reference can serve as a quick guide for your staff, streamlining the approval process.
- Stay Informed on Changes: Insurance policies are subject to frequent modifications. For 2026, be aware that certain codes may have updated requirements. Subscribing to updates from coverage providers or industry newsletters will help you remain informed about any changes in prior approval requirements, ensuring compliance and efficiency.
Additionally, consider leveraging the administrative assistance services offered by Healthcare Partners Consulting to understand how to handle prior authorizations and simplify your prior approval processes. Our expertise in medical billing and consulting can help you navigate the complexities of coverage requirements effectively.
Complete and Submit Prior Authorization Forms
Understanding how to handle prior authorizations involves correctly filling out previous approval forms, which is essential for obtaining prompt approvals. To enhance your submission process, follow these streamlined steps:
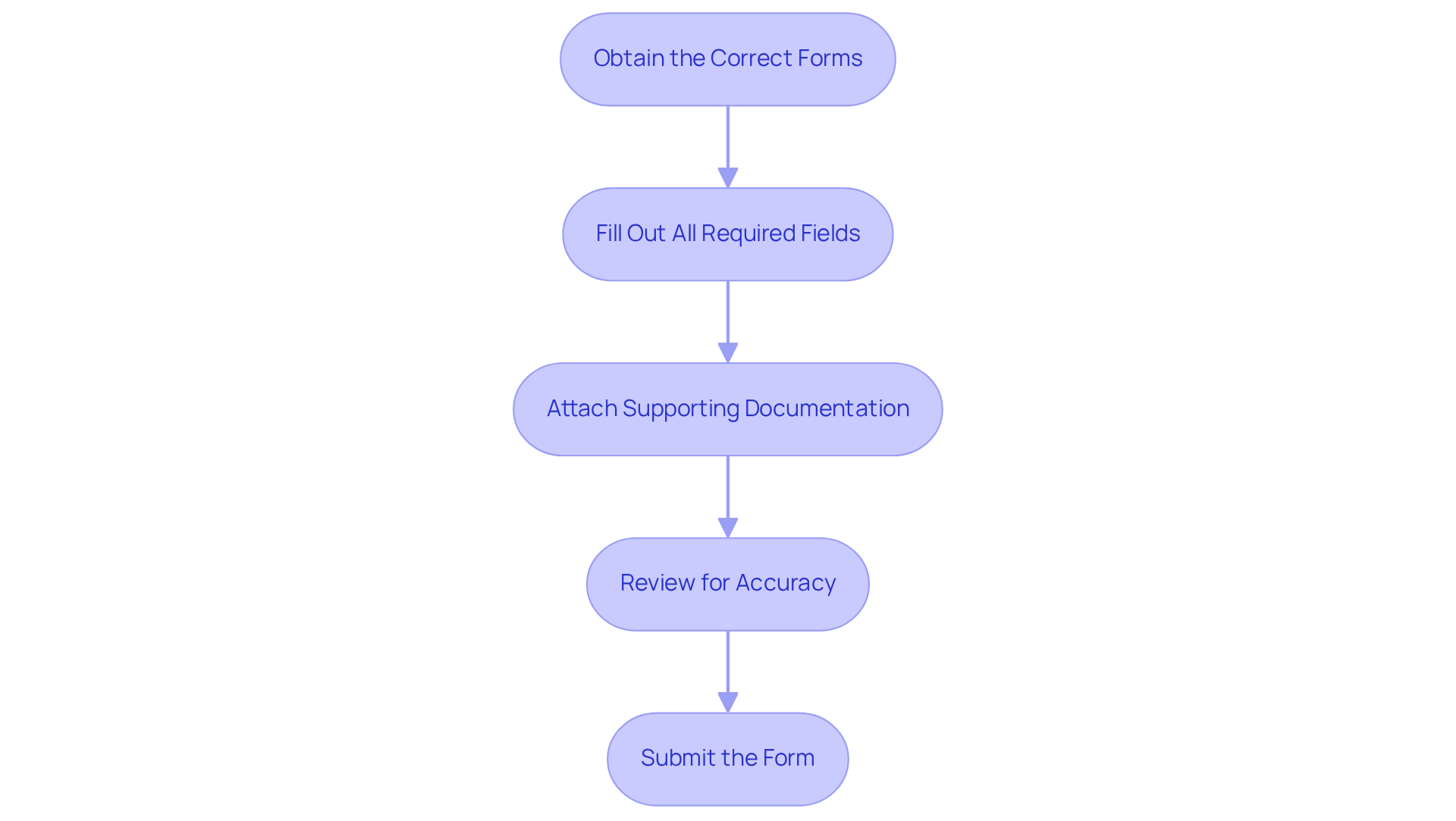
- Obtain the Correct Forms: Ensure you have the most recent version of the prior authorization forms required by the provider. These forms are typically accessible on the insurer's website.
- Fill Out All Required Fields: Carefully complete every section of the form, including patient information, specifics about the assistance provided, and clinical justification. Incomplete forms are a leading cause of delays, with 46% of claim denials attributed to missing or inaccurate information.
- Attach Supporting Documentation: Include all necessary clinical documentation that substantiates the request, such as treatment plans, progress notes, and diagnostic codes. Properly label and organize these documents to facilitate review.
- Review for Accuracy: Before submission, meticulously double-check all information for accuracy. Errors can lead to denials or processing delays, which 93% of physicians report as a significant barrier to timely care.
- Submit the Form: Adhere to the submission guidelines provided by the insurance company, whether via mail, fax, or an online portal. Retain a copy of the submitted form and any confirmation received for your records.
Additionally, consider utilizing the essential toolkit provided by Healthcare Partners Consulting, specifically designed for mental health providers. This toolkit simplifies credentialing and administrative tasks by offering features such as automated form filling, real-time eligibility checks, and denial risk predictions. By leveraging these tools, therapists and behavioral health groups can focus more on patient care and less on administrative burdens. Understanding the 'gold card' system, which exempts high-performing providers from previous approvals for certain services, can also enhance your clinic's efficiency.
By adhering to these steps and utilizing the resources from Healthcare Partners Consulting, mental health clinics can learn how to handle prior authorizations, significantly improving their approval rates for requests and ensuring that patients receive timely care.
Check Status of Prior Authorization Requests
Understanding how to handle prior authorizations is essential for overseeing the status of previous approval requests to ensure prompt patient care. Here’s how to effectively manage this process:
- Utilize Online Platforms: Most providers offer online platforms for checking the status of previous approval requests. Regularly logging in helps you stay informed about any updates.
- Establish Reminder Systems: Implement a tracking system for submission dates and follow-up reminders. This practice ensures that you understand how to handle prior authorizations by checking the status within the necessary timeframe, thereby reducing delays in patient care.
- Engage with Insurance Representatives: If a response is not received within the expected timeframe, proactively contact the insurance company. Be prepared with your request details to facilitate efficient communication.
- Document All Interactions: Maintain a thorough log of all communications regarding request approvals, including dates, names of representatives, and reference numbers. This documentation is invaluable for resolving any issues that may arise.
- Keep Clients Informed: Regularly update clients on the status of their previous approval requests. Transparency manages their expectations and strengthens trust in your practice.
Moreover, understanding how to handle prior authorizations through the simplified approval process by Healthcare Partners Consulting can enhance your efficiency. Their team identifies needs, gathers necessary documentation, and submits requests through electronic portals, ensuring immediate tracking. They also proactively follow up with payers until a determination is reached, significantly reducing the likelihood of denials. In the event of a denial, Healthcare Partners Consulting assists with appeals and next steps, focusing on coding, timely filing, prior authorization, and medical necessity denials to improve your revenue cycle efficiency.
Conclusion
Navigating the complexities of prior authorizations is crucial for mental health clinics that strive to deliver timely and effective care. A comprehensive understanding of requirements, eligibility checks, service codes, and submission processes enables clinics to secure necessary approvals without unnecessary delays. By implementing the outlined steps and utilizing available resources, clinics can significantly enhance their operational efficiency and improve patient outcomes.
Key insights from this guide highlight the importance of thorough documentation, clear communication with clients, and proactive management of prior authorization requests. Familiarity with the specific requirements of various insurance providers and the maintenance of accurate records can mitigate the risks of claim denials and financial loss. Furthermore, leveraging administrative support services can streamline the entire process, allowing healthcare providers to concentrate more on patient care rather than administrative hurdles.
The significance of mastering prior authorization processes cannot be overstated. As the landscape of mental health services evolves, remaining informed and adaptable to changes in insurance protocols will be essential for ensuring that patients receive the care they require. Clinics are encouraged to prioritize these strategies, fostering a more efficient workflow and ultimately enhancing the quality of care delivered to clients.
Frequently Asked Questions
What is prior authorization and why is it important?
Prior authorization is a procedure used by insurers to evaluate coverage for specific treatments or procedures before they are delivered. It is crucial for mental health facilities to manage prior authorizations effectively to ensure patients receive necessary care without unexpected costs.
How do insurance providers vary in their prior authorization requirements?
Each insurance provider has distinct criteria for prior approval. It is essential for healthcare providers to familiarize themselves with the specific requirements set by each insurer they work with.
What documentation is typically required for prior authorization?
Insurers usually require clinical documentation that validates the medical necessity of the proposed treatment, which may include patient history, treatment plans, and progress notes.
What types of services commonly require prior approval?
Services that often necessitate prior approval include inpatient admissions, specific outpatient therapies, and certain medications.
What are the consequences of not obtaining prior authorization?
Failing to obtain necessary approval can lead to claim denials, resulting in financial losses for the clinic and unexpected bills for patients. It is vital to manage prior authorizations to mitigate these risks.
How can clinics ensure their clients are eligible for prior authorization?
Clinics should gather client information, utilize insurance portals for verification, contact insurance providers directly if needed, document the eligibility confirmation process, and communicate with clients about their eligibility status.
What is the significance of documenting the eligibility verification process?
Keeping a detailed record of the eligibility verification process is important for addressing any issues that may arise later, as 20% of all medical claim denials are attributed to eligibility or registration errors.
How can clinics communicate effectively with clients regarding prior authorization?
Clear communication about clients' eligibility status and any potential out-of-pocket costs is essential for managing expectations and fostering trust in client relationships.
