
5 Steps to Optimize Revenue Cycle Management for Mental Health Clinics
Introduction
Effective revenue cycle management (RCM) serves as the backbone of financial health for mental health clinics, significantly influencing cash flow and the quality of care provided. By mastering the intricacies of RCM, clinics can realize substantial financial benefits, potentially increasing revenue by 10 to 20 percent. However, as the healthcare billing landscape grows increasingly complex, many clinics encounter challenges such as:
- Rising claim denials
- Inefficient processes
To navigate these obstacles effectively, facilities must optimize their revenue cycle to ensure sustainable growth.
Understand Revenue Cycle Management and Its Importance
Revenue Cycle Management (RCM) encompasses the entire financial workflow that healthcare providers utilize to manage care finances, beginning with the initial interaction with individuals and concluding with the final payment. For mental health clinics, effective RCM is essential, as it profoundly influences cash flow, operational efficiency, and the quality of care delivered.
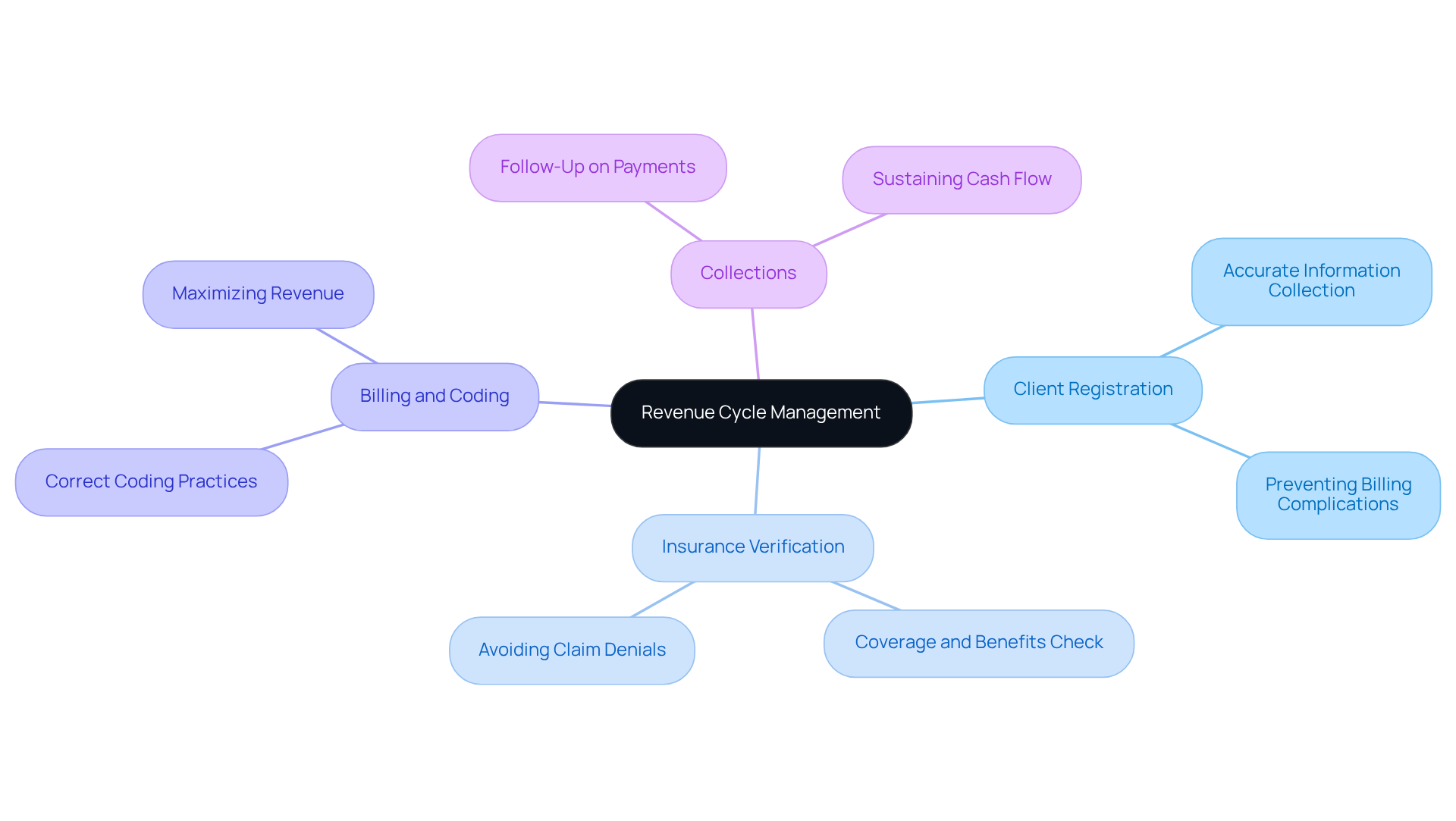
Key components of RCM include:
- Client Registration: Accurate collection of client information at the outset is critical to prevent future billing complications.
- Insurance Verification: Verifying coverage and benefits before service delivery is vital to avoid claim denials and ensure appropriate reimbursement for services rendered.
- Billing and Coding: Correct coding and billing of services to insurance providers are crucial for maximizing revenue and minimizing errors.
- Collections: Actively following up on outstanding payments is necessary to secure timely revenue and sustain cash flow.
Healthcare Partners Consulting provides comprehensive accounts receivable management solutions that enhance revenue cycle efficiency. Their proactive engagement with payers regarding unpaid or underpaid claims, along with appeal submissions for denied or incorrectly processed claims, enables mental wellness facilities to optimize their revenue activities. Furthermore, assigning dedicated accounts receivable specialists to each account ensures personalized service and effective management of billing processes.
By adeptly managing these components, mental wellness clinics can significantly reduce claim denials, improve cash flow, and enhance overall patient satisfaction. Research indicates that understanding how to optimize revenue cycle management can lead practices to achieve 10 to 20 percent more revenue compared to those employing standard medical billing methods, underscoring the importance of tailored strategies in the behavioral wellness sector. Additionally, the national average Days in Accounts Receivable for behavioral practices is approximately 52 days, highlighting the need for effective RCM processes to reduce this figure. Addressing challenges such as increasing denials and claims processing inefficiencies, while ensuring compliance with HIPAA and other regulations, is crucial for improving the financial health of mental health establishments.
Implement Pre-Service Registration and Collections Strategies
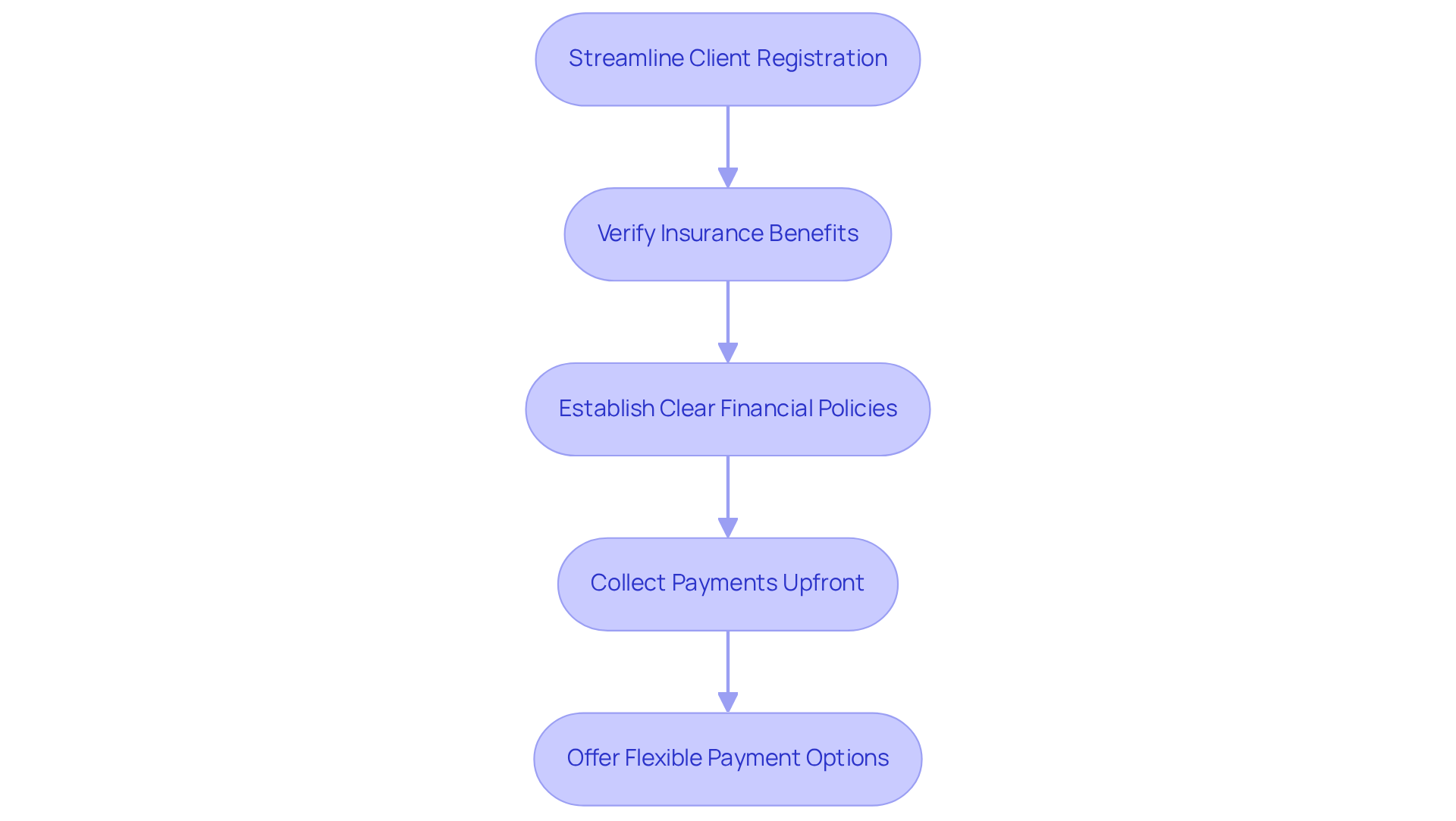
Mental wellness clinics should implement robust pre-service registration and collections strategies to learn how to optimize revenue cycle management. The following actionable steps can be taken:
- Streamline Client Registration: Utilize electronic health record (EHR) systems to enable swift and precise client registration. Collect all necessary information, including insurance details, upfront to minimize delays.
- Verify Insurance Benefits: Confirm the individual's insurance coverage and benefits before the appointment. This proactive strategy helps avoid unforeseen expenses for individuals and decreases the chances of claim rejections, which can significantly impact revenue.
- Establish Clear Financial Policies: Clearly communicate your clinic's financial policies during the registration process. Outline payment expectations, co-pays, and any out-of-pocket costs to set clear expectations and enhance understanding.
- Collect Payments Upfront: Encourage clients to pay their co-pays or a portion of their fees at the time of service. Implementing a point-of-service collections process can significantly improve cash flow and reduce outstanding balances.
- Offer Flexible Payment Options: Provide various payment methods, including credit cards, payment plans, and online payment portals. This flexibility facilitates patients in fulfilling their financial obligations, ultimately enhancing collection rates.
By utilizing extensive revenue cycle management services from Healthcare Partners Consulting, medical facilities can learn how to optimize revenue cycle management, improve their financial status, optimize accounts receivable management, and achieve a 20-40% decrease in accounts receivable days, resulting in enhanced cash flow.
Streamline Authorization Processes for Faster Revenue Collection
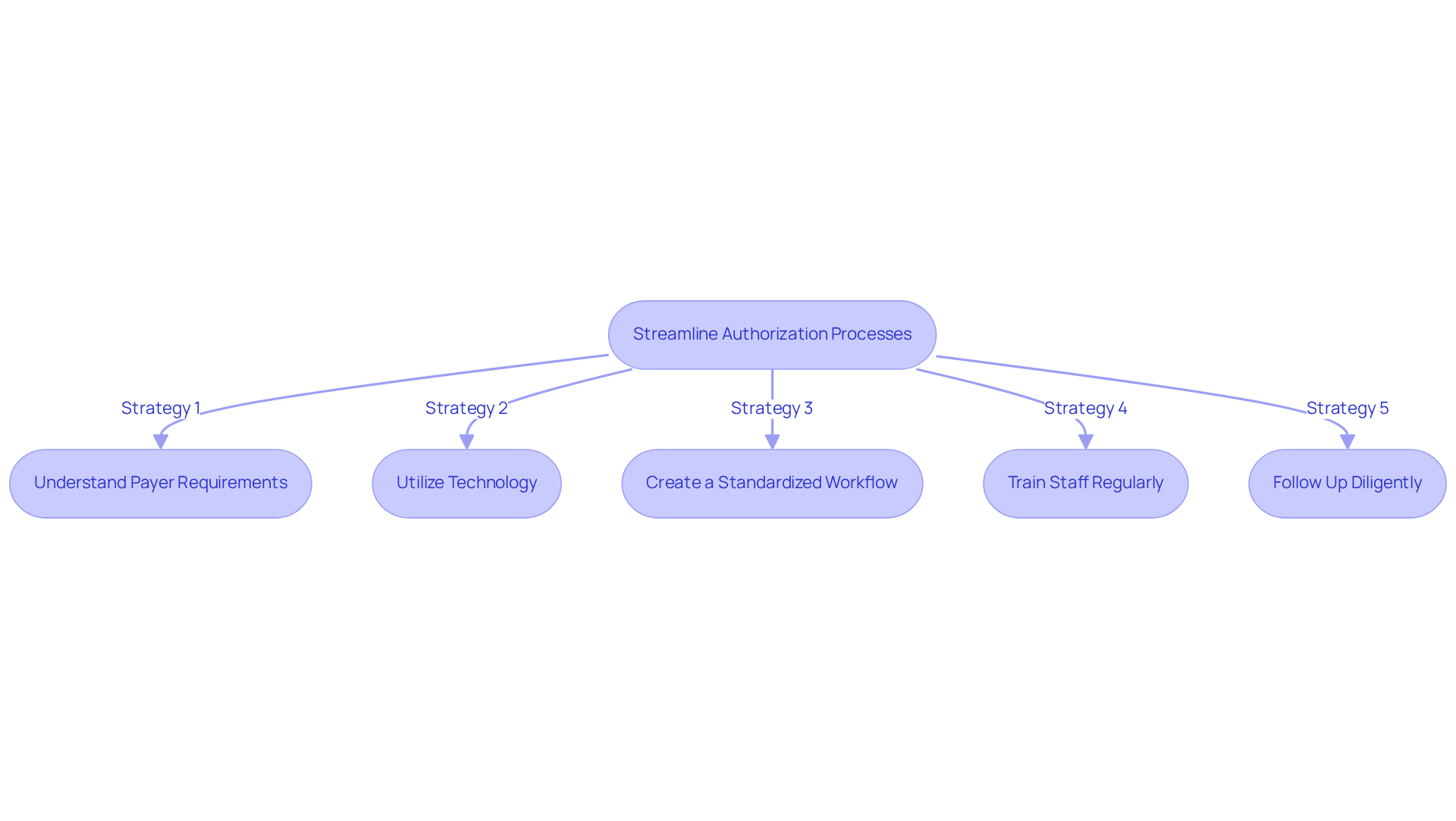
Authorization procedures can significantly obstruct the revenue cycle for mental health clinics. To enhance efficiency and expedite approvals, consider the following strategies:
- Understand Payer Requirements: Gain a comprehensive understanding of the specific authorization requirements for each insurance payer. This preparation enables the prompt collection of essential documentation, minimizing delays in the approval procedure.
- Utilize Technology: Leverage electronic prior authorization tools that automate the submission procedure and track request statuses. These systems can lead to a 56% reduction in review time and an 80% increase in documentation bundling efficiency, minimizing manual errors and accelerating approvals.
- Create a Standardized Workflow: Establish a standardized workflow for managing authorizations, complete with checklists for required documentation and timelines for follow-ups. This approach fosters consistency and enhances operational efficiency.
- Train Staff Regularly: Implement regular training sessions for your administrative team on the latest authorization requirements and best practices. Keeping staff informed is crucial for minimizing delays and ensuring compliance with evolving payer standards.
- Follow Up Diligently: Develop a robust follow-up protocol for pending authorizations. Regularly check in with payers to confirm that requests are being processed and to swiftly address any issues that may arise. This proactive approach can significantly reduce the time individuals wait for necessary treatments, ultimately improving outcomes and clinic revenue.
Additionally, it is important to note that beginning January 1, 2026, new regulations will reduce the standard turnaround time for decisions from 14 days to 7 days. This change underscores the urgency of streamlining authorization processes. Furthermore, a survey by the American Medical Association found that more than 90% of physicians believe prior authorization negatively impacts patient clinical outcomes, highlighting the critical need for improvements in this area. Insights from industry experts, like Davia Ward, highlight the ongoing mental wellness billing crisis, where 19% of physicians indicated that prior authorization led to serious adverse events resulting in hospitalization, underscoring the potential risks linked to delays in authorization.
For additional assistance, mental wellness providers can download the Free Toolkit created to streamline credentialing and administrative tasks, thereby learning how to optimize revenue cycle management more efficiently.
Educate Clinicians on Documentation Requirements
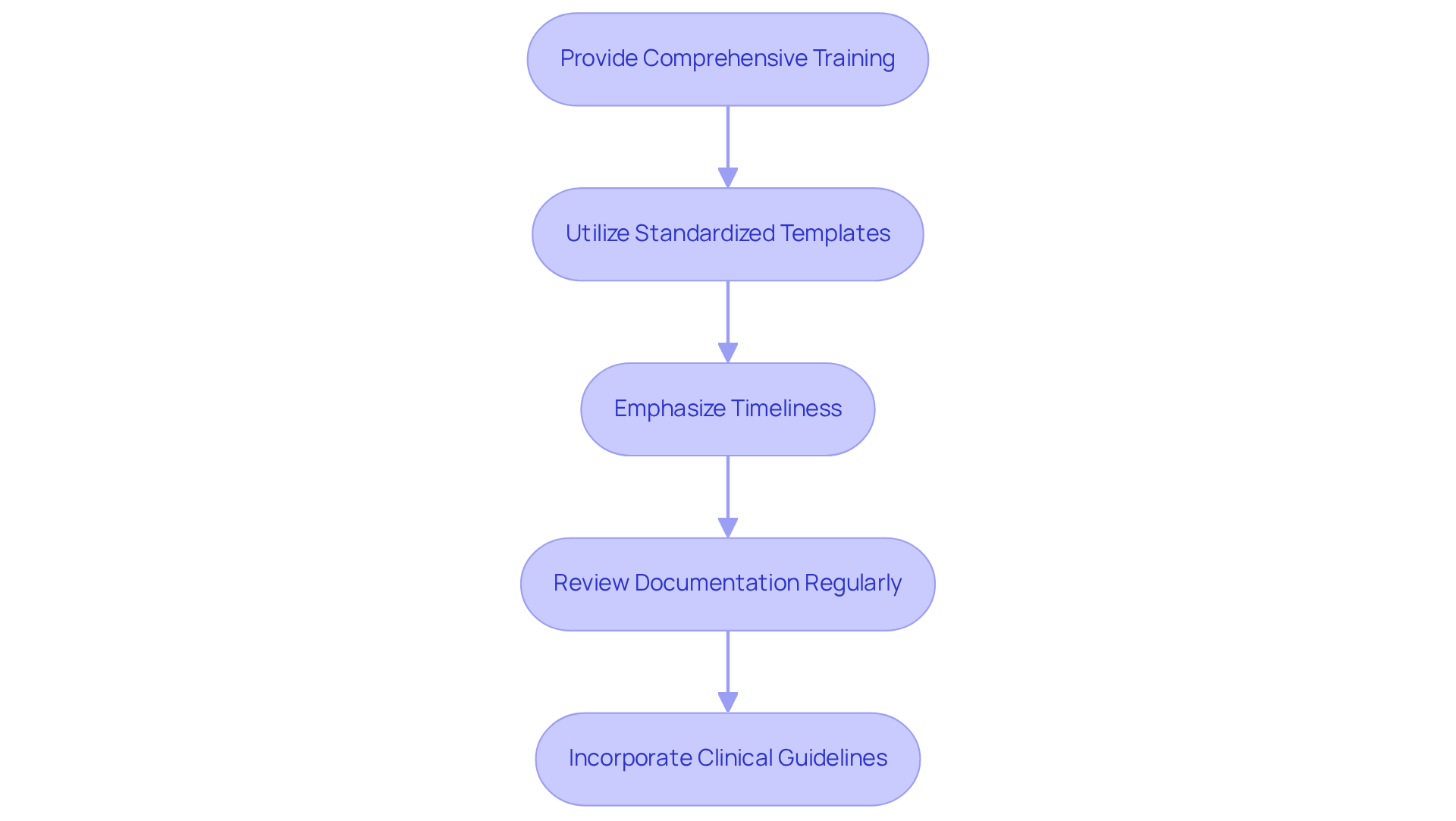
Precise documentation is crucial for effective revenue cycle management in mental health facilities. To ensure compliance and optimize billing, clinics should adopt the following strategies:
- Provide Comprehensive Training: Conduct training sessions for clinicians that focus on documentation standards, emphasizing the essential information required for billing and compliance. This training, offered by Healthcare Partners Consulting, aligns with payer-specific guidelines, equipping clinicians to meet evolving compliance expectations and reduce denial rates.
- Utilize Standardized Templates: Implement standardized documentation templates that assist clinicians in capturing all necessary information during client encounters. This approach enhances consistency and minimizes errors, which is vital for precise documentation to prevent avoidable denials. Our expert coding team reviews and corrects coding issues before claims are submitted, ensuring accuracy.
- Emphasize Timeliness: Encourage clinicians to complete documentation promptly after patient visits. Timely documentation is essential for ensuring that billing activities proceed without delays, particularly with the Transforming Episode Accountability Model (TEAM) running from January 1, 2026, through December 31, 2030. Our services are designed to support timely submissions, thereby reducing administrative burdens on in-house staff.
- Review Documentation Regularly: Conduct regular audits of clinical documentation to identify areas for improvement. Providing constructive feedback to clinicians can significantly enhance their documentation practices and help mitigate audit pressure. At Healthcare Partners Consulting, we incorporate quality assurance processes and peer reviews into our workflow to maintain high standards.
- Incorporate Clinical Guidelines: Ensure that clinicians are familiar with and adhere to clinical guidelines impacting documentation, such as those from the American Psychiatric Association. This adherence is essential as it aligns with our overall goal of how to optimize revenue cycle management, which is a core focus of our tailored coding support services.
Review and Optimize Administrative Support Utilization
Mental health facilities should regularly review and optimize their utilization of administrative support to understand how to optimize revenue cycle management. The following steps outline how to achieve this:
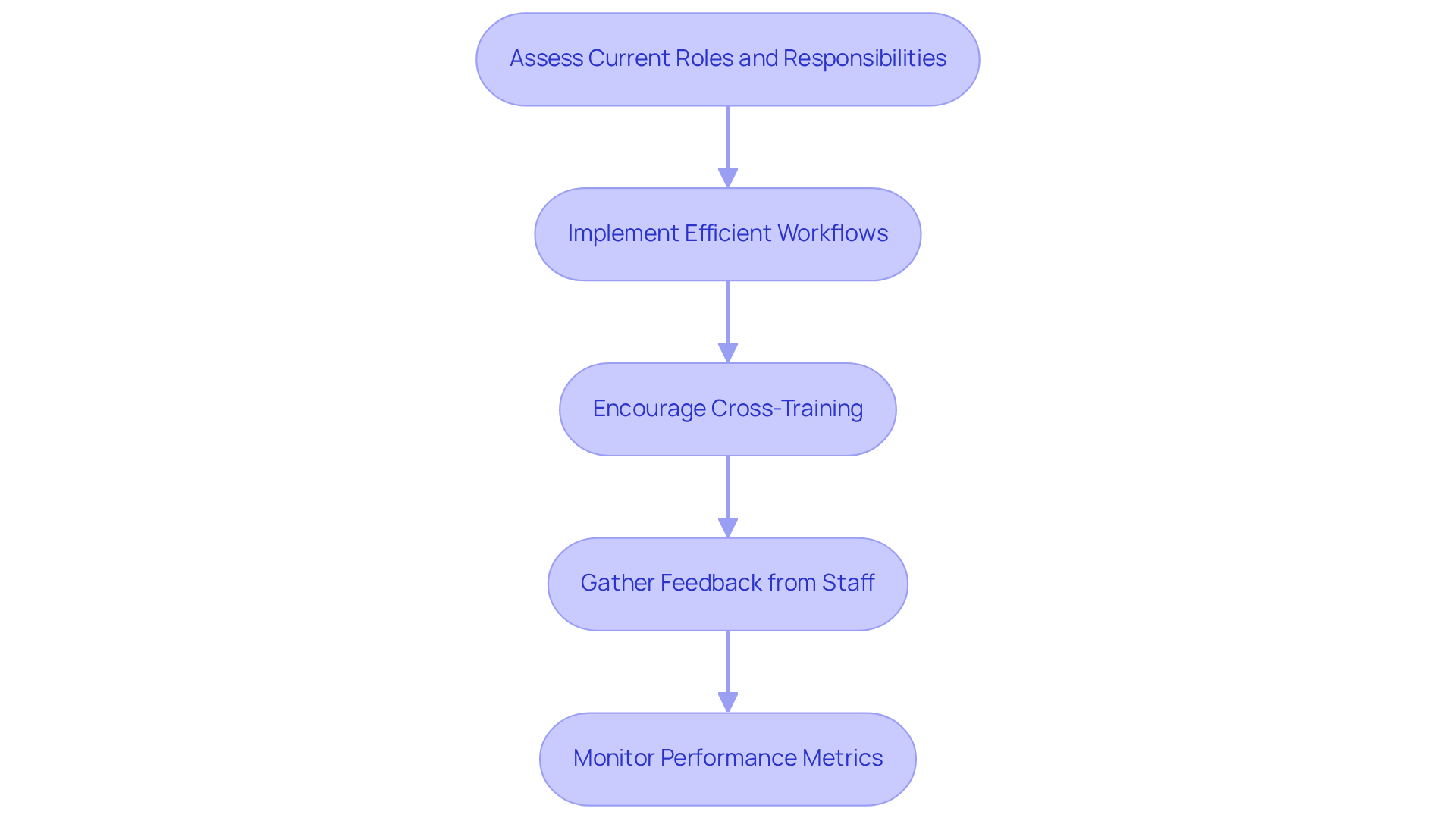
- Assess Current Roles and Responsibilities: Evaluate the roles of administrative staff to ensure that their responsibilities align with the clinic's needs. Identify any gaps or overlaps in duties that may hinder efficiency.
- Implement Efficient Workflows: Streamline workflows for administrative tasks such as scheduling, billing, and communication with clients. Leveraging technology to automate repetitive tasks can significantly reduce manual errors and improve overall efficiency.
- Encourage Cross-Training: Train administrative staff across multiple areas of the revenue cycle, including billing and patient registration. This flexibility enhances coverage during peak times or staff absences, ensuring continuity in operations.
- Gather Feedback from Staff: Regularly solicit feedback from administrative staff regarding workflow challenges and areas for improvement. Their insights can lead to more efficient methods and a more engaged workforce.
- Monitor Performance Metrics: Establish key performance indicators (KPIs) to measure the efficiency of administrative processes. Regularly reviewing these metrics helps identify trends and areas for further optimization, which is crucial for understanding how to optimize revenue cycle management and ensuring that the clinic remains responsive to changing needs.
Conclusion
Effective revenue cycle management (RCM) is essential for mental health clinics, acting as the foundation for financial stability and operational efficiency. By grasping the complexities of RCM, clinics can refine their workflows, boost cash flow, and ultimately enhance the quality of care they provide to patients.
This article has detailed five critical steps to optimize RCM:
- Streamlining client registration
- Verifying insurance benefits
- Improving billing and coding practices
- Establishing robust collections strategies
- Enhancing administrative support
Each component is crucial in reducing claim denials, speeding up revenue collection, and increasing patient satisfaction. Moreover, educating clinicians on documentation requirements is vital, as accurate and timely documentation is key for compliance and effective billing.
In summary, prioritizing revenue cycle management is not merely a financial necessity; it is a strategic imperative for mental health clinics. By adopting these best practices, clinics can enhance their financial health and operational success. As the healthcare landscape evolves, embracing these strategies will enable mental health providers to deliver high-quality care while sustaining a viable business model.
Frequently Asked Questions
What is Revenue Cycle Management (RCM)?
Revenue Cycle Management (RCM) is the financial workflow that healthcare providers use to manage care finances, starting from the initial interaction with clients and ending with the final payment.
Why is RCM important for mental health clinics?
Effective RCM is crucial for mental health clinics as it significantly impacts cash flow, operational efficiency, and the quality of care provided.
What are the key components of RCM?
The key components of RCM include Client Registration, Insurance Verification, Billing and Coding, and Collections.
How does client registration contribute to RCM?
Accurate client registration is essential to prevent future billing complications and ensure a smooth financial process.
What role does insurance verification play in RCM?
Verifying insurance coverage and benefits before service delivery is vital to avoid claim denials and ensure appropriate reimbursement for services rendered.
Why is billing and coding important in RCM?
Correct billing and coding of services to insurance providers are crucial for maximizing revenue and minimizing errors.
How can clinics improve collections in RCM?
Actively following up on outstanding payments is necessary to secure timely revenue and sustain cash flow.
What services does Healthcare Partners Consulting provide to enhance RCM?
Healthcare Partners Consulting offers comprehensive accounts receivable management solutions, proactive engagement with payers regarding unpaid claims, and dedicated accounts receivable specialists for personalized service.
What benefits can mental wellness clinics achieve by optimizing RCM?
By effectively managing RCM, clinics can reduce claim denials, improve cash flow, enhance patient satisfaction, and potentially achieve 10 to 20 percent more revenue compared to standard billing methods.
What is the average Days in Accounts Receivable for behavioral practices?
The national average Days in Accounts Receivable for behavioral practices is approximately 52 days.
What strategies can mental wellness clinics implement for pre-service registration and collections?
Clinics can streamline client registration, verify insurance benefits, establish clear financial policies, collect payments upfront, and offer flexible payment options.
How can electronic health record (EHR) systems aid in client registration?
EHR systems can facilitate swift and precise client registration by collecting all necessary information, including insurance details, upfront to minimize delays.
What is the impact of clear financial policies on RCM?
Clearly communicating financial policies during registration helps set expectations regarding payments, co-pays, and out-of-pocket costs, enhancing understanding and compliance.
How can upfront payment collections improve cash flow?
Encouraging clients to pay co-pays or a portion of their fees at the time of service can significantly improve cash flow and reduce outstanding balances.
What is the potential decrease in accounts receivable days when optimizing RCM?
Utilizing extensive revenue cycle management services can lead to a 20-40% decrease in accounts receivable days, resulting in enhanced cash flow.
