
Understanding Diagnosis Codes for Mental Health vs. General Medical Coding
Introduction
The healthcare coding landscape presents a complex interplay between mental health and general medical classifications, each serving distinct purposes and executing processes differently. Grasping these differences is essential for healthcare providers, as the subtleties in diagnosis codes can significantly influence billing efficiency and patient care outcomes.
What specific challenges emerge when navigating the intricate requirements of mental health coding in contrast to the more straightforward nature of general medical coding?
This article examines the unique characteristics of these coding systems, shedding light on their implications for compliance and reimbursement within the dynamic healthcare environment.
Understand the Distinct Nature of Mental Health and General Medical Coding
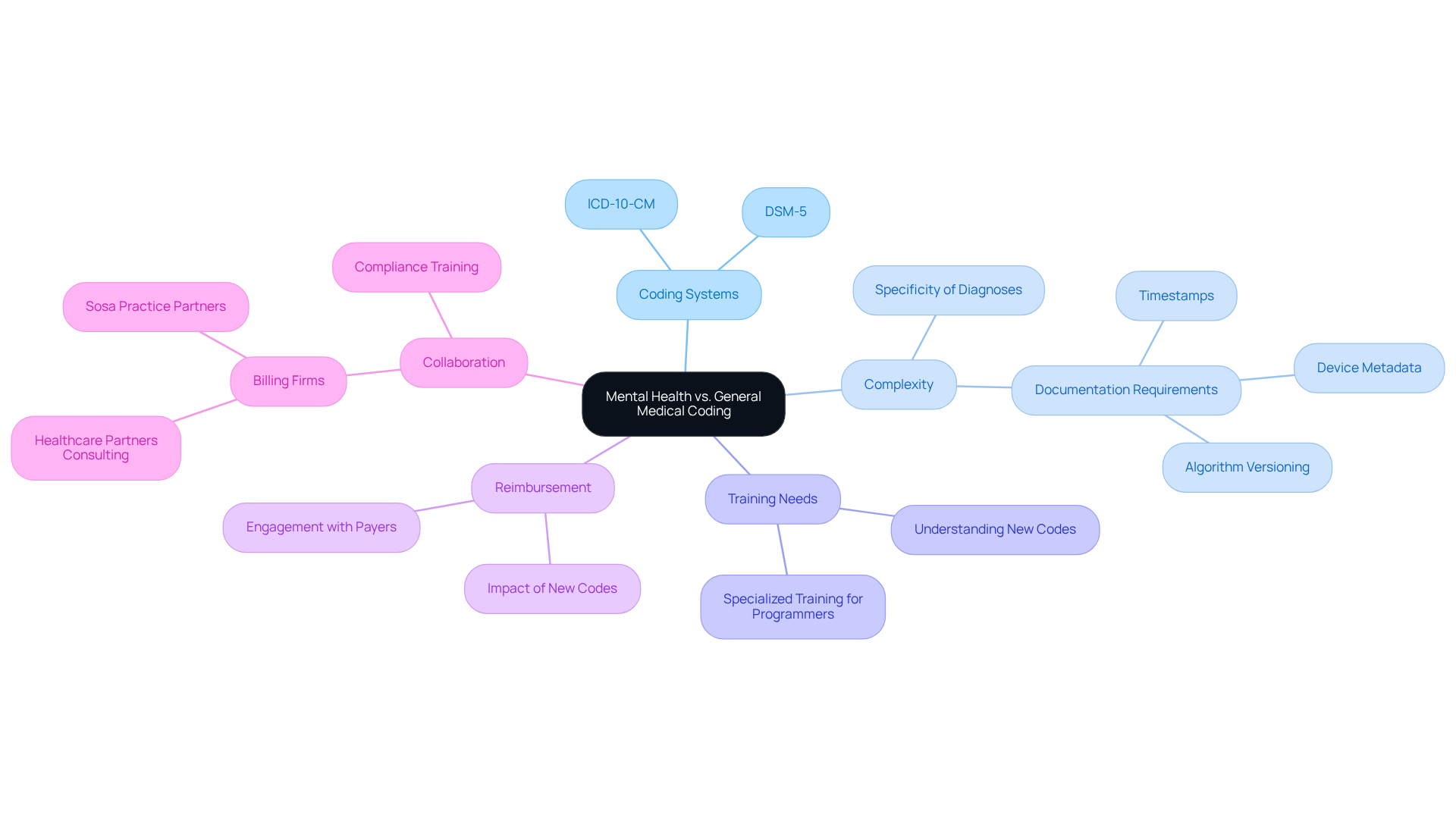
Mental wellness categorization and general medical classification serve distinct purposes, governed by unique sets of rules and guidelines. Psychological condition classification primarily utilizes the ICD-10-CM (International Classification of Diseases, 10th Revision, Clinical Modification) and DSM-5 (Diagnostic and Statistical Manual of Mental Disorders) identifiers, which serve as the diagnosis code for mental health counseling specifically designed for diagnosing psychological issues. In contrast, general medical classification predominantly employs ICD-10-CM classifications for a broader range of physical wellness conditions and procedures.
A considerable difference exists in the specificity and intricacy of psychological diagnoses, which frequently require a nuanced comprehension of psychological conditions and their manifestations. For instance, psychological condition standards often necessitate further specifics concerning the intensity and duration of symptoms, a level of detail that is less typical in general medical classification. This complexity underscores the necessity for specialized training for programmers in psychological environments to ensure precise billing and adherence to insurance standards.
As of 2026, a significant percentage of healthcare providers are utilizing the diagnosis code for mental health counseling as part of their psychological coding, reflecting its essential role in the billing process. The introduction of new regulations and updates necessitates continuous learning and adjustment to ensure compliance and enhance reimbursement. Real-world examples illustrate the challenges faced by care providers, such as the need for accurate documentation to justify ongoing support, including timestamps and clinical integration of data. Engaging with payers prior to 2026 is crucial for understanding their reimbursement plans for new classifications. These factors highlight the importance of collaborating with experienced billing companies like Healthcare Partners Consulting, which specializes in telehealth-specific coding, quality assurance procedures, and compliance training, to effectively navigate the complexities of behavioral coding.
Explore Mental Health Counseling Diagnosis Codes: Structure and Categories
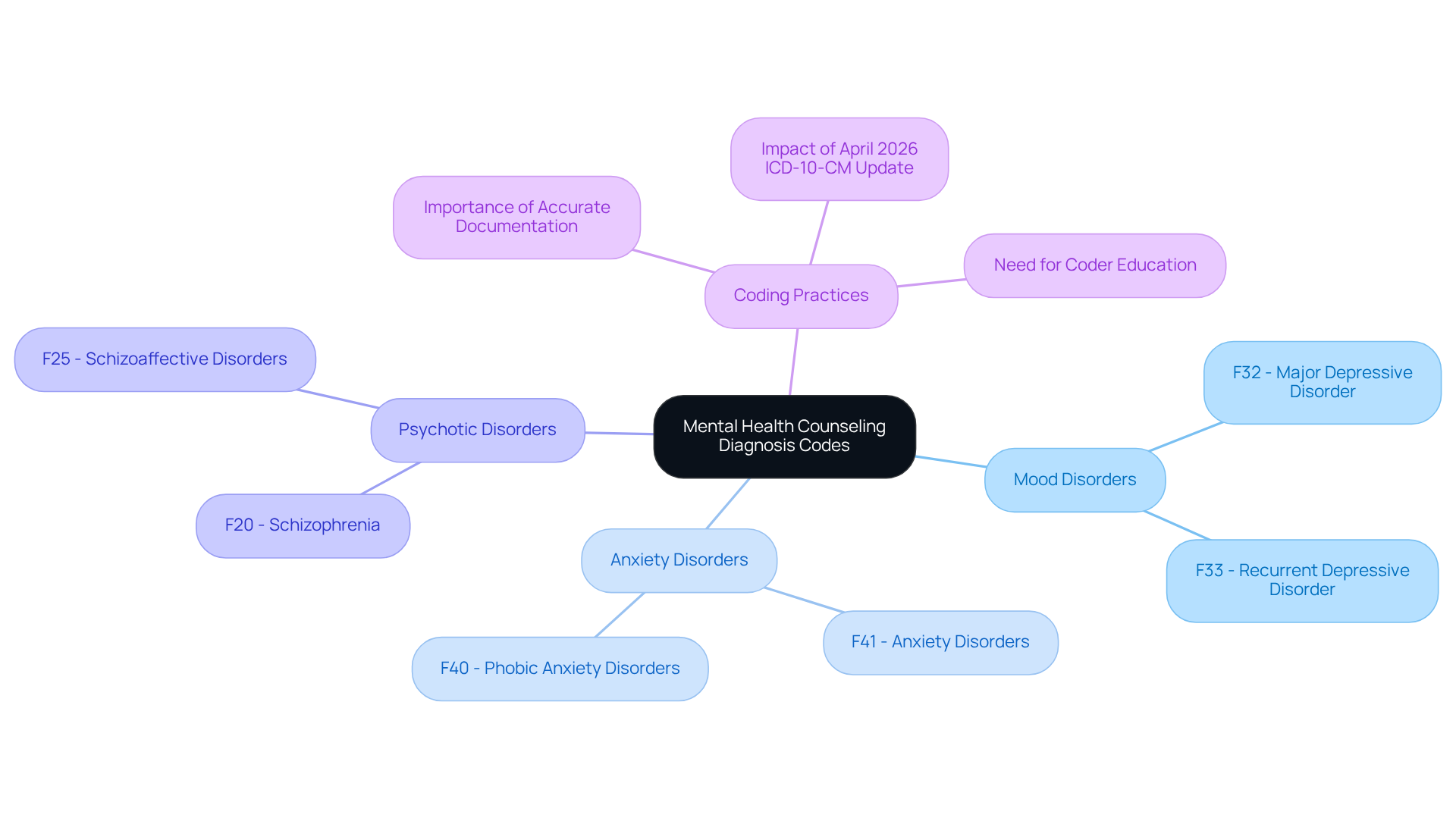
The diagnosis code for mental health counseling classifications primarily derive from the ICD-10-CM and DSM-5 frameworks, designed to encompass a broad spectrum of mental health disorders. These classifications are categorized into distinct groups, such as:
- mood disorders
- anxiety disorders
- psychotic disorders
For instance, the ICD-10 classification F32 corresponds to Major Depressive Disorder, whereas F41 denotes Anxiety Disorders.
Each identifier typically commences with a letter followed by a series of numbers that specify the diagnosis. This specificity is crucial for accurately documenting a patient's condition with the diagnosis code for mental health counseling, which is vital for effective treatment planning and securing insurance reimbursement. Additionally, mental health codes often require the use of modifiers to indicate the severity or specific characteristics of the disorder. This necessity adds a layer of complexity to the programming process, distinguishing it from general medical documentation, which may not require such detailed specifications.
As of April 2026, updates to the ICD-10-CM have introduced structural changes that enhance classification flexibility, permitting dual classification in certain scenarios. This development underscores the importance for psychological specialists to stay informed about billing practices to ensure compliance and improve revenue integrity.
Examine General Medical Coding: Structure and Key Differences
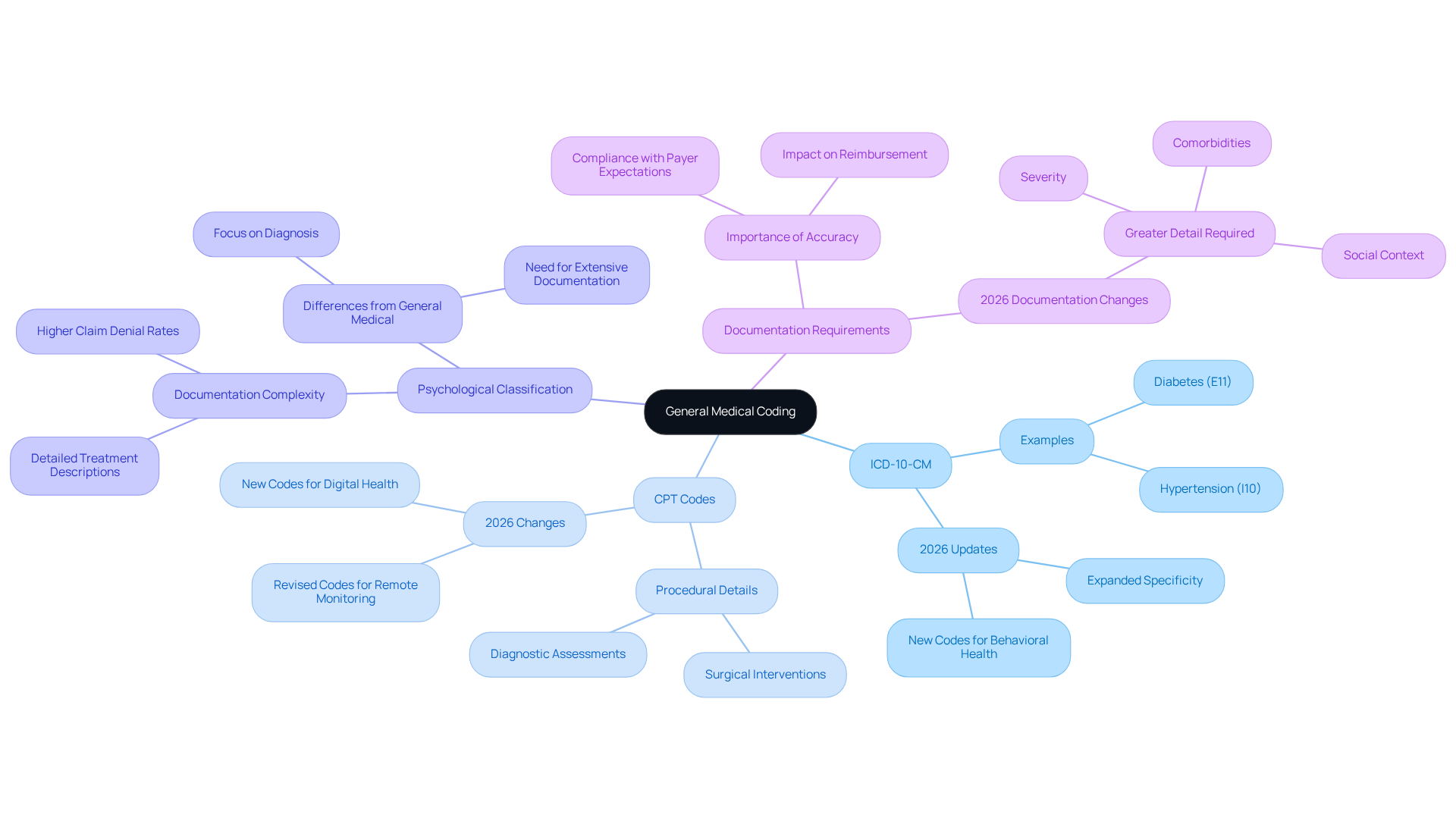
General medical classification primarily relies on the ICD-10-CM system, encompassing a broad spectrum of physical conditions and procedures. Unlike mental health classifications, general medical classifications typically focus on specific diagnoses and treatments, without the complexities of psychological factors. For example, identifiers for conditions such as diabetes (E11) or hypertension (I10) are straightforward and generally do not require modifiers to indicate severity.
Moreover, general medical classification utilizes Current Procedural Terminology (CPT) codes to detail the services provided, including surgical interventions and diagnostic assessments. This dual classification framework - ICD-10 for diagnoses and CPT for procedures - contrasts sharply with psychological categorization, which emphasizes the diagnosis itself. This focus underscores the distinct nature of psychological treatment, where meticulous documentation is crucial to capture the nuances of patient care.
Experts in medical classification emphasize that the differences between psychological care and general medical classification are significant. For instance, psychological condition classification often requires more extensive documentation to support claims, as payers expect detailed descriptions of treatment strategies and patient progress. This complexity can lead to higher claim denial rates in psychological care compared to general medical classification, where the straightforward nature of physical conditions typically results in fewer disputes over claims.
As the 2026 updates to ICD-10-CM are implemented, mental health providers will need to adapt to new classification requirements that include the diagnosis code for mental health counseling, demanding greater specificity in documentation about severity, comorbidities, and social context. This change underscores the importance of staying current with programming practices to ensure compliance and improve reimbursement. Furthermore, practices that do not update their programming processes risk facing higher denial rates for claims that utilize outdated or incomplete identifiers, highlighting the critical role of medical billing and software in improving first-pass acceptance rates by identifying issues prior to submission.
Healthcare Partners Consulting provides comprehensive administrative support services designed to enhance cash flow through expedited payments and reduced days in accounts receivable. By actively evaluating claims, ensuring accurate charge capture in line with documentation, and offering services such as monthly reconciliation and accounts receivable trending analysis, we assist clinics in minimizing denials and improving compliance. Our dedicated accounts receivable specialists concentrate on managing the tedious follow-up work, enabling your team to prioritize patient-centered tasks while ensuring transparency and sustainable growth in your revenue cycle.
Compare Practical Implications: Mental Health vs. General Medical Coding
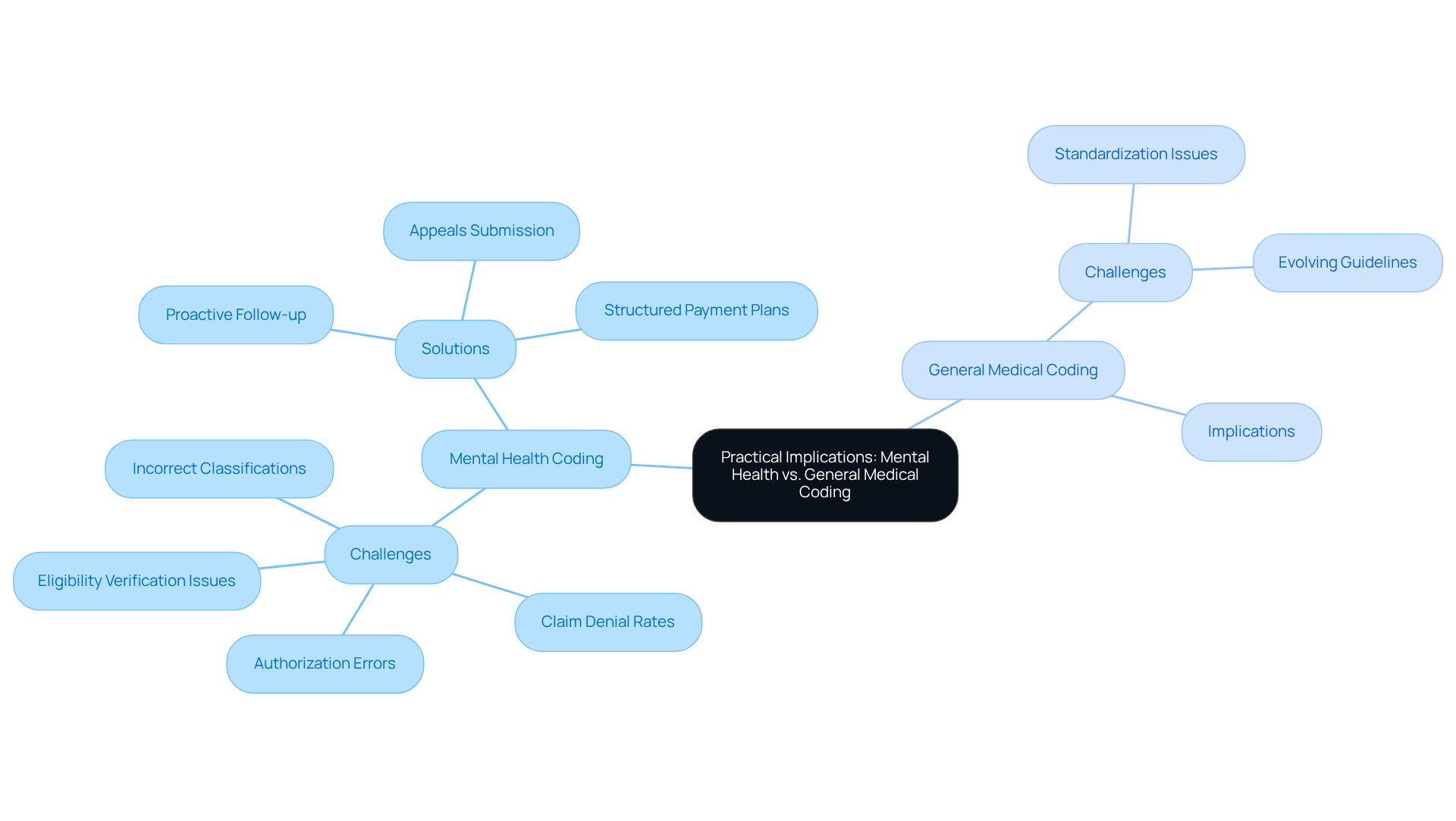
The practical consequences of the diagnosis code for mental health counseling classification, when compared to general medical classification, are significant, particularly regarding billing effectiveness and adherence. Thorough documentation is essential for mental wellness classification, which often requires a diagnosis code for mental health counseling, along with comprehensive treatment plans and progress notes to substantiate continuous care. This complexity can lead to claim denial rates ranging from 15 to 25 percent, which is notably higher than those observed in general medical classification. Common reasons for denials in psychological services include:
- Authorization errors
- Incorrect classifications related to the diagnosis code for mental health counseling
- Eligibility verification issues
All of which can diminish revenue and consume valuable staff time.
As highlighted by Davia Ward in her analysis of the mental health billing crisis, these challenges demand proactive solutions. Healthcare Partners Consulting provides comprehensive accounts receivable management solutions, which include:
- Proactive follow-up with payers on unpaid claims
- Submission of appeals for denied claims
- Structured payment plans
By adopting these strategies, practices can significantly alleviate administrative burdens and enhance cash flow.
In contrast, general medical classification typically adheres to more standardized procedures, which can streamline the billing process. However, it is not without its challenges; the rapid evolution of programming guidelines and payer policies can lead to confusion for providers. For instance, the introduction of new CPT and HCPCS codes effective January 1, 2026, requires providers to remain informed to avoid compliance issues.
Understanding these practical implications allows healthcare providers to refine their administrative strategies related to the diagnosis code for mental health counseling, ensuring compliance and optimizing revenue cycles. Investing in specialized billing expertise, such as that offered by Healthcare Partners Consulting, can substantially reduce administrative burdens and improve claim approval rates, enabling practices to concentrate more on patient care. As noted by billing specialists, the complexities of mental health coding necessitate ongoing training and monitoring to avert preventable denials and enhance financial performance.
Conclusion
Differentiating between mental health coding and general medical coding is essential for healthcare providers, as each serves distinct functions governed by specific regulations and guidelines. Understanding these differences not only enhances billing accuracy but also enables mental health professionals to navigate the complexities inherent in their field effectively.
Key insights reveal that mental health coding, primarily utilizing ICD-10-CM and DSM-5 classifications, requires a higher level of specificity and documentation compared to general medical coding. The need for detailed descriptions of symptoms, treatment plans, and progress notes in mental health coding significantly affects claim approval rates, often resulting in higher denial rates. In contrast, general medical coding typically follows more straightforward procedures, which can streamline the billing process; however, it still necessitates vigilance due to evolving guidelines.
Recognizing these distinctions underscores the importance of specialized training and collaboration with experienced billing professionals. By investing in tailored billing solutions, healthcare providers can alleviate administrative burdens, enhance compliance, and ultimately concentrate on delivering quality patient care. As the landscape of mental health and general medical coding continues to evolve, remaining informed and proactive is crucial for optimizing reimbursement and ensuring the sustainability of healthcare practices.
Frequently Asked Questions
What are the main differences between mental health coding and general medical coding?
Mental health coding primarily uses ICD-10-CM and DSM-5 identifiers for diagnosing psychological issues, while general medical coding primarily employs ICD-10-CM for a wider range of physical health conditions and procedures.
Why is mental health coding considered more complex than general medical coding?
Mental health coding requires a nuanced understanding of psychological conditions, often necessitating detailed specifics about the intensity and duration of symptoms, which is less common in general medical coding.
What is the significance of accurate documentation in mental health coding?
Accurate documentation is crucial for justifying ongoing support and ensuring compliance with insurance standards, including the need for timestamps and clinical integration of data.
How are healthcare providers adapting to changes in mental health coding as of 2026?
A significant percentage of healthcare providers are incorporating the diagnosis code for mental health counseling into their coding practices, reflecting its importance in the billing process and the need for continuous learning to comply with new regulations.
What role do billing companies like Healthcare Partners Consulting play in mental health coding?
Healthcare Partners Consulting specializes in telehealth-specific coding, quality assurance procedures, and compliance training, helping providers navigate the complexities of behavioral coding effectively.
Why is it important to engage with payers before 2026 regarding mental health coding?
Engaging with payers is essential for understanding their reimbursement plans for new classifications, which can impact the financial aspects of mental health services.

