
Why Denial Management is Crucial for Mental Health Clinics' Success
Introduction
Denial management is a critical pillar in the operational success of mental health clinics, significantly influencing both their financial health and the quality of services provided. By systematically addressing the complexities associated with insurance claim rejections, these facilities can recover lost revenue while simultaneously enhancing their overall operational efficiency. Given that denial rates for behavioral health claims range from 10% to 20%, a pressing question emerges: how can clinics effectively navigate the intricate landscape of denial management to secure their financial future and improve patient care?
Define Denial Management and Its Role in Healthcare
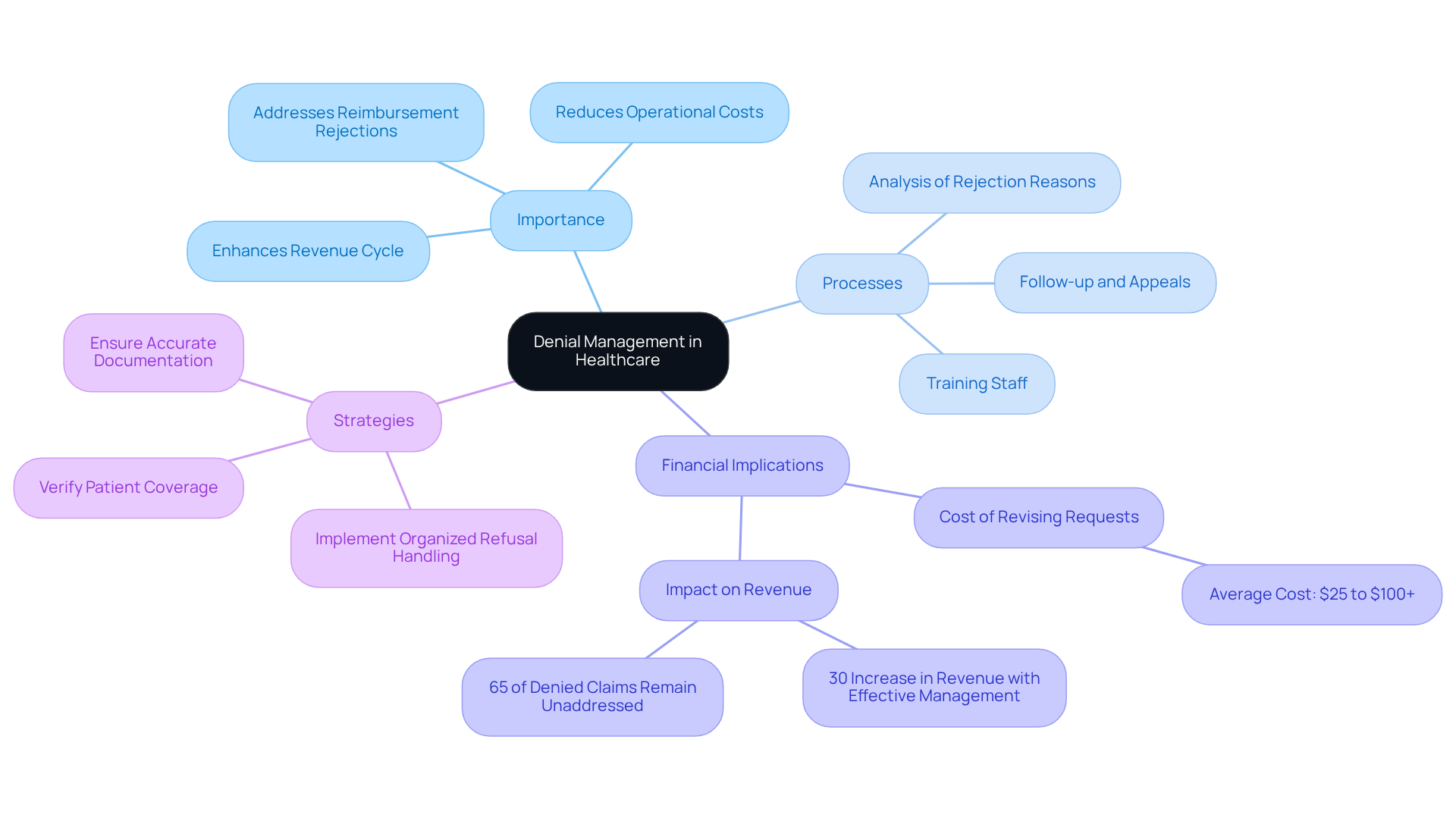
Denial oversight serves as a systematic approach for identifying, analyzing, and addressing denied requests from insurance providers, illustrating why denial management is crucial in mental health facilities. Effective oversight guarantees that providers receive appropriate payment for their services, addressing not only the immediate reasons for reimbursement rejections but also implementing strategies to prevent future occurrences. In 2026, the average rejection rate for behavioral health claims ranges from 10% to 20%, often exacerbated by more stringent evaluations of medical necessity. This highlights why denial management is crucial for facilities to adopt robust refusal handling strategies.
By understanding the complexities of oversight related to refusals, mental health facilities can significantly enhance their revenue cycle, which illustrates why denial management is crucial. For instance, clinics that implement organized refusal handling processes, such as those offered by Healthcare Partners Consulting, have reported improved reimbursement outcomes and reduced operational costs. Their comprehensive refusal handling services include:
- Detailed analysis of rejection reasons
- Timely follow-up and appeal submissions
- Trending reports to identify recurring issues
- Dedicated refusal specialists
These initiatives can lead to a 30% increase in revenue by identifying and rectifying persistent billing errors, resulting in higher clean submission rates and expedited reimbursements.
Moreover, understanding why denial management is crucial alleviates administrative burdens, enabling staff to focus on patient care rather than the complexities of unresolved issues. The financial implications are significant; the cost of revising a single rejected request can range from $25 to over $100, not including potential cash flow disruptions for smaller practices. Notably, 65% of denied claims remain unaddressed without proper oversight, which illustrates why denial management is crucial to prevent permanent revenue loss.
Integrating effective refusal handling techniques, such as those provided by Healthcare Partners Consulting, demonstrates why denial management is crucial for maintaining the operational health of a practice. This encompasses:
- Training staff on billing codes and insurance requirements
- Ensuring accurate documentation
- Verifying patient coverage prior to appointments
Additionally, understanding the categories of refusals-clinical and administrative-can further enhance the efficiency of refusal handling efforts. By prioritizing claim management, mental health clinics can secure a consistent revenue stream, bolster financial stability, and ultimately improve the quality of care delivered to patients.
Examine Types of Healthcare Claim Denials
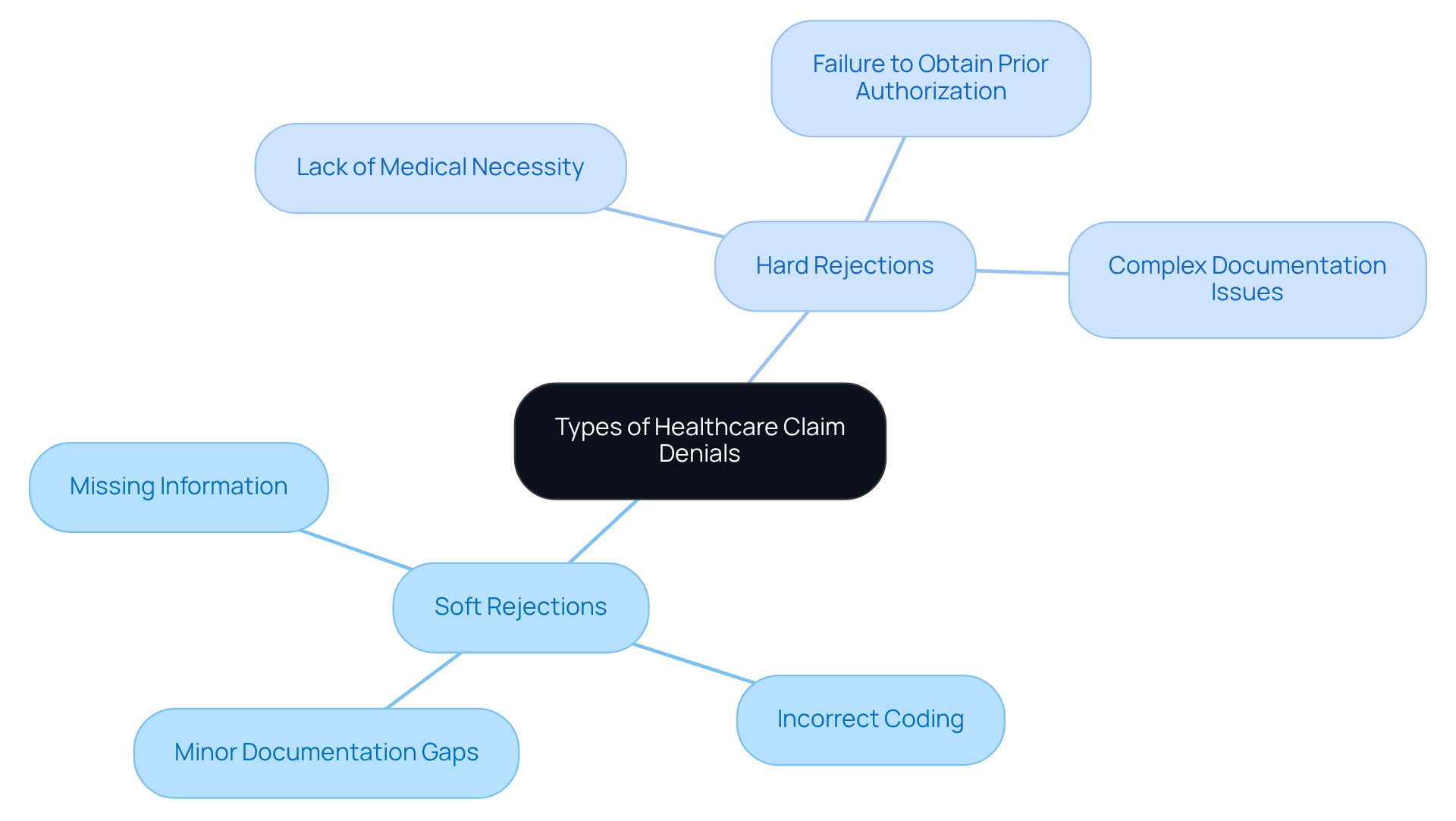
Healthcare requests for payment rejections can be categorized into two primary groups: soft rejections and hard rejections. Soft rejections typically arise from minor errors, such as missing information or incorrect coding, and can often be resolved with relative ease. For instance, a claim may be denied due to an incorrect CPT code or a minor documentation gap, which can be quickly corrected and resubmitted. In contrast, hard rejections present more significant challenges, often stemming from issues like lack of medical necessity or failure to obtain prior authorization. These rejections necessitate more extensive intervention, as they may involve complex documentation and justification processes.
For mental health clinics, understanding why denial management is crucial involves recognizing the distinction between these types of denial. The subjective nature of mental health services frequently results in requests being denied due to perceived deficiencies in documentation that justify the need for treatment. For example, a claim for a therapy session might be denied if the documentation does not clearly link the treatment to a specific DSM-5 diagnosis or fails to demonstrate measurable treatment goals.
By classifying rejections into soft and hard types, healthcare facilities can develop targeted strategies to address the underlying reasons for these issues. This proactive approach demonstrates why denial management is crucial, as it not only reduces future instances of rejections but also enhances the overall effectiveness of the revenue cycle process, ultimately supporting the facility's financial health and its capacity to deliver quality care.
Analyze Financial Impact of Denial Management on Practices
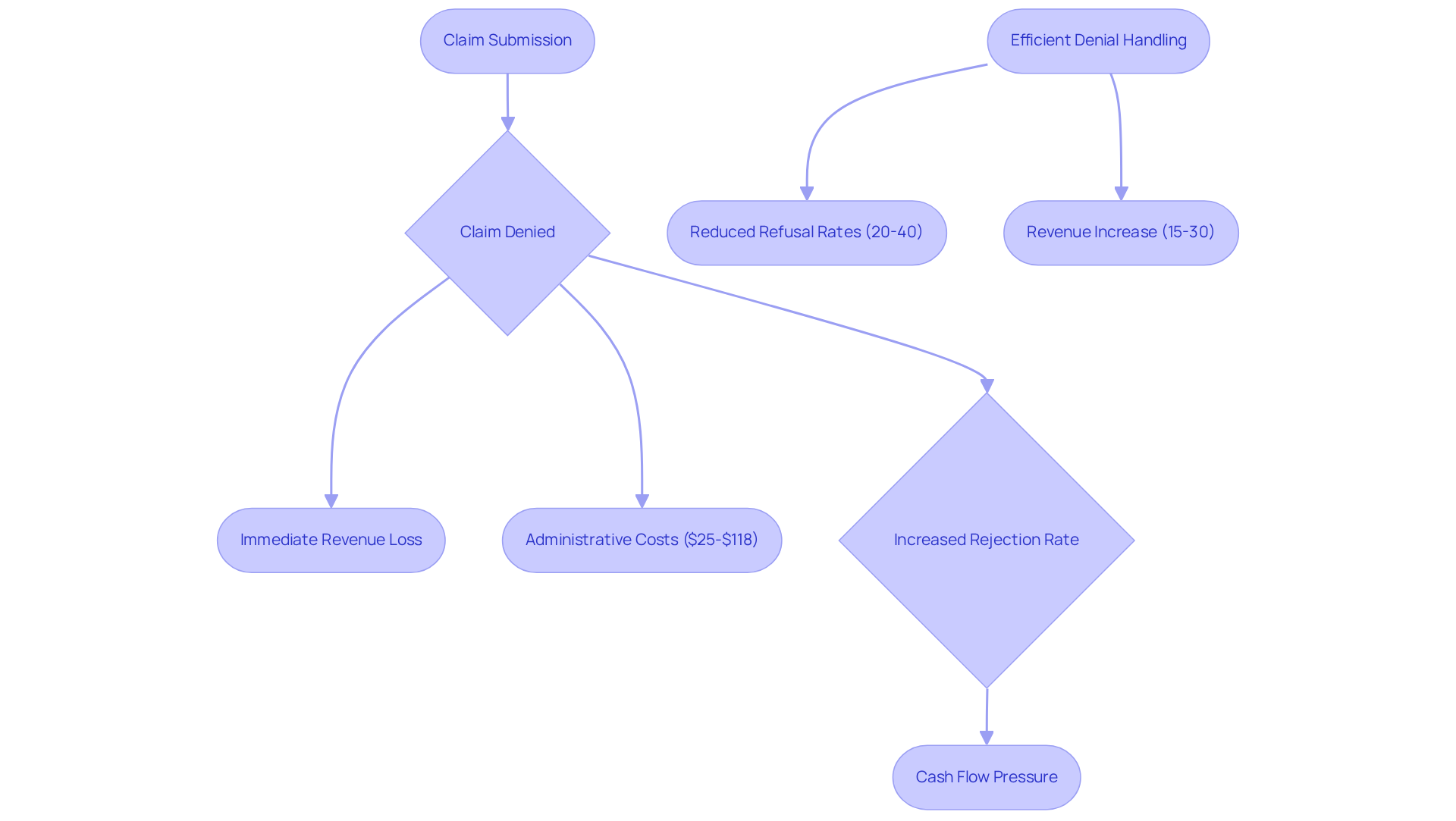
The financial consequences of denial management for mental health facilities are substantial. Rejected requests not only result in immediate revenue loss but also incur additional administrative expenses related to appeals and resubmissions. Each denied claim can cost healthcare facilities between $25 and $118 in administrative costs, excluding the potential revenue lost from delayed payments. Elevated rejection rates can exert significant pressure on cash flow, complicating the management of operational costs such as payroll and overhead. For example, a clinic facing a 20% rejection rate may encounter considerable financial difficulties, jeopardizing its capacity to deliver quality care.
Efficient denial handling techniques are essential for recovering lost income, minimizing administrative burdens, and enhancing the overall financial health of mental health practices. Case studies indicate that practices partnering with specialized denial management services can see refusal rates decrease by 20-40%, leading to a revenue increase of 15-30%. This underscores why denial management is crucial for mental health facilities to prioritize as a fundamental component of their operational strategy.
Assess Administrative Challenges in Denial Management
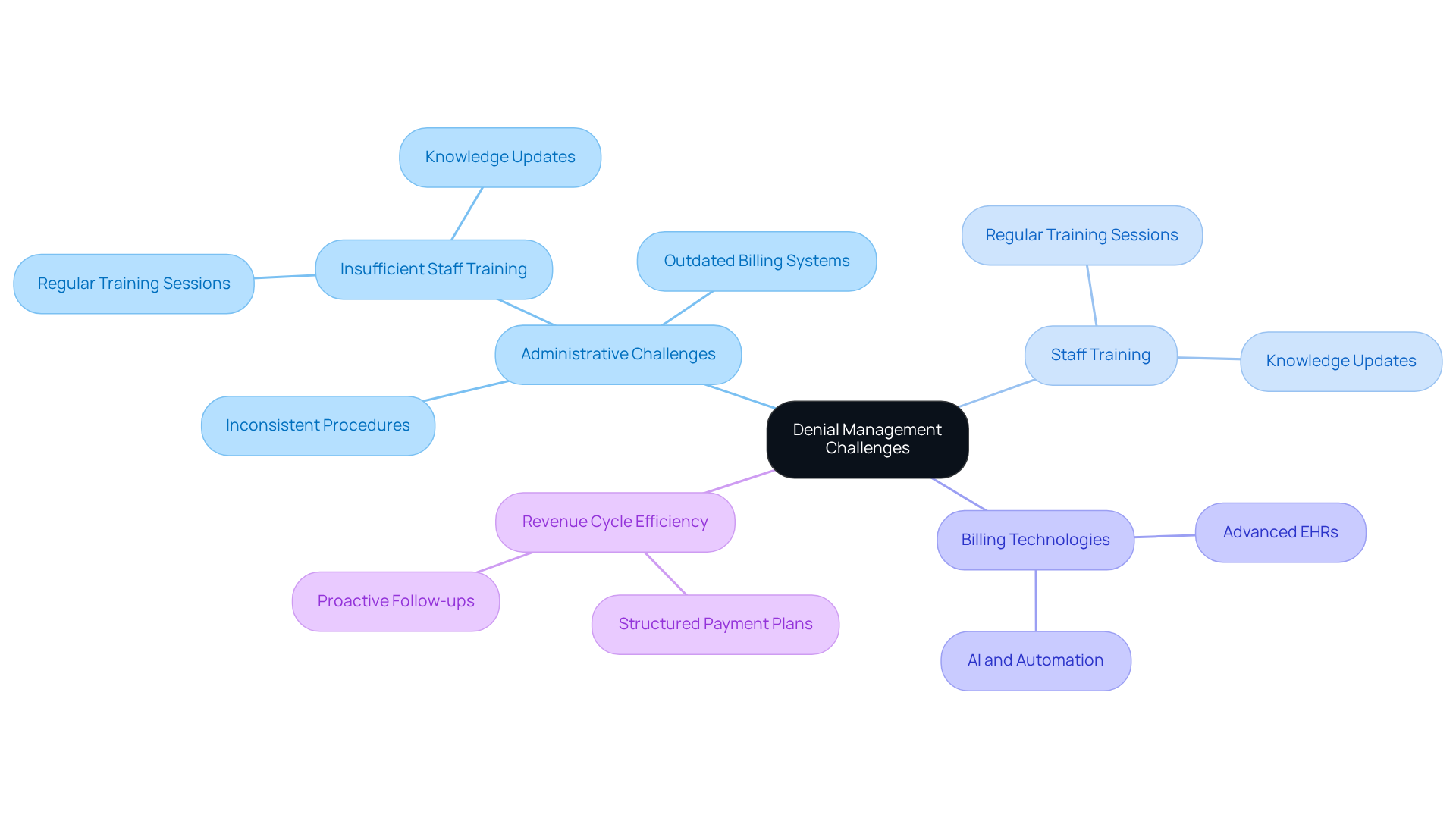
Mental health centers frequently face significant administrative challenges, including insufficient staff training, outdated billing systems, and inconsistent procedures for processing requests. A prominent issue is the shortage of qualified billing specialists, which can lead to errors in claim submissions and delays in resolving denied claims. The complex nature of mental health billing necessitates comprehensive documentation to support treatment, further complicating the denial management process. Additionally, healthcare facilities often struggle to keep pace with evolving payer demands and regulations, resulting in rising rejection rates.
To address these challenges, clinics should implement proactive strategies to improve their denial management processes, as this highlights why denial management is crucial. Investing in comprehensive staff training is essential, equipping billing teams with the necessary knowledge to navigate the complexities of mental health services effectively. For example, regular training sessions can ensure that staff remain informed about coding updates and payer policies, ultimately minimizing errors and enhancing claim submission accuracy.
Successful medical facilities demonstrate that meeting employee training needs can lead to significant improvements in claim management. By fostering a culture of continuous education and utilizing advanced billing technologies, such as artificial intelligence and automation, these clinics have optimized their operations and reduced rejection rates. Furthermore, establishing structured payment plans and proactively following up with payers on outstanding claims can enhance revenue cycle efficiency. As Debra Stall, a seasoned expert in healthcare management, notes, "Investing in a knowledgeable team can significantly decrease refusals." This highlights why denial management is crucial for training and ensuring financial stability in mental health practices.
Conclusion
In conclusion, denial management stands as a critical element for the success of mental health clinics, functioning as a systematic approach to guarantee that providers receive appropriate compensation for their services. By comprehensively understanding and implementing effective denial management strategies, clinics can markedly decrease claim rejection rates and enhance their overall revenue cycle. This proactive stance not only addresses immediate financial challenges but also establishes a foundation for sustainable operational health.
The article has presented key insights into the various types of healthcare claim denials, the financial ramifications of denial management, and the administrative hurdles encountered by mental health facilities. It has been highlighted that differentiating between soft and hard rejections enables clinics to tailor their strategies more effectively. Moreover, investing in staff training and embracing advanced billing technologies can yield significant improvements in claim resolution, ultimately promoting a more efficient revenue cycle.
The importance of denial management transcends mere financial recovery; it is essential for upholding the quality of care delivered to patients. By prioritizing effective denial management practices, mental health clinics can secure their financial stability while enhancing their ability to provide high-quality services. Adopting these strategies is a vital step toward ensuring the long-term success and operational efficiency of mental health practices, ultimately benefiting both providers and patients.
Frequently Asked Questions
What is denial management in healthcare?
Denial management is a systematic approach for identifying, analyzing, and addressing denied requests from insurance providers, ensuring that healthcare providers receive appropriate payment for their services.
Why is denial management crucial for mental health facilities?
Denial management is crucial for mental health facilities as it helps improve their revenue cycle by addressing reimbursement rejections and implementing strategies to prevent future occurrences, thereby enhancing financial stability.
What is the average rejection rate for behavioral health claims in 2026?
The average rejection rate for behavioral health claims in 2026 ranges from 10% to 20%.
What are some benefits of organized refusal handling processes?
Organized refusal handling processes can lead to improved reimbursement outcomes, reduced operational costs, and a potential 30% increase in revenue by identifying and rectifying persistent billing errors.
What services do comprehensive refusal handling initiatives typically include?
Comprehensive refusal handling initiatives typically include detailed analysis of rejection reasons, timely follow-up and appeal submissions, trending reports to identify recurring issues, and dedicated refusal specialists.
What are the financial implications of denied claims?
The cost of revising a single rejected request can range from $25 to over $100, and 65% of denied claims remain unaddressed without proper oversight, leading to potential permanent revenue loss.
How can denial management alleviate administrative burdens in healthcare practices?
Effective denial management can alleviate administrative burdens by allowing staff to focus more on patient care rather than the complexities of unresolved billing issues.
What techniques can enhance refusal handling efforts in mental health clinics?
Techniques that can enhance refusal handling efforts include training staff on billing codes and insurance requirements, ensuring accurate documentation, and verifying patient coverage prior to appointments.
What are the two categories of refusals that can impact denial management?
The two categories of refusals are clinical and administrative, and understanding these can further enhance the efficiency of refusal handling efforts.
