General
Why Credentialing is Necessary for Patient Safety and Compliance

Introduction
Credentialing acts as a vital gatekeeper within the healthcare system, ensuring that only qualified professionals are entrusted with patient care. By rigorously verifying the education, training, and experience of medical providers, credentialing not only enhances the quality of care but also cultivates trust between patients and healthcare organizations.
As the landscape of healthcare compliance continues to evolve, it raises pertinent questions regarding the effectiveness of current credentialing practices and their implications for patient safety. Medical institutions face significant challenges in upholding these standards. Navigating the complexities of credentialing is essential for safeguarding both compliance and patient outcomes.
Define Credentialing and Its Importance in Healthcare
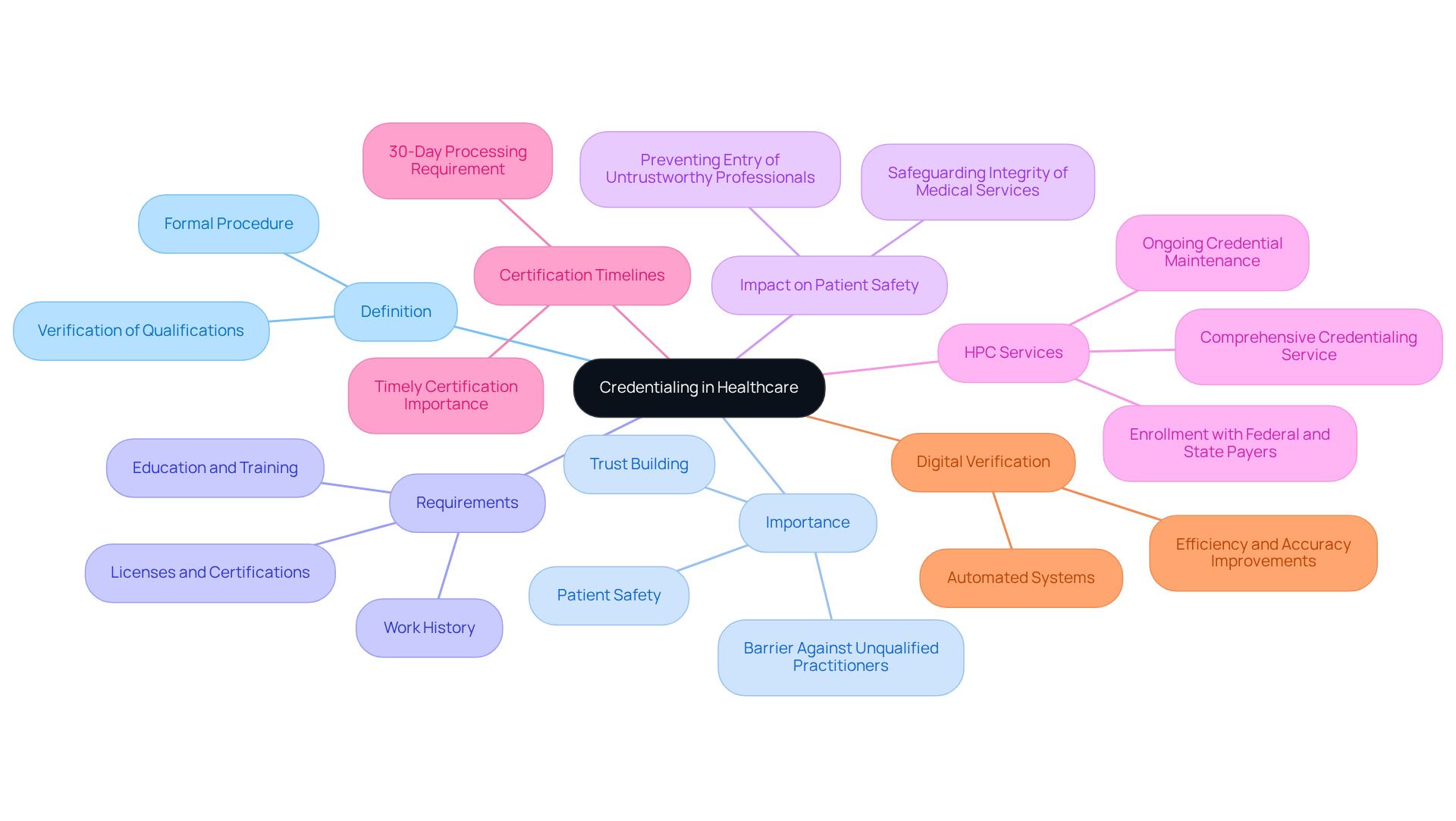
Credentialing is a formal procedure through which medical organizations confirm the qualifications, experience, and professional background of medical providers. This process involves evaluating education, training, licenses, certifications, and work history, ensuring that practitioners meet the necessary standards to provide safe and effective care. The significance of qualifications in medical care illustrates why credentialing is necessary, as it serves as a barrier against unqualified practitioners entering the medical system, thereby safeguarding patient safety and upholding the integrity of medical services.
A well-organized qualification system not only enhances the quality of care but also fosters trust between patients and medical providers, which is essential for achieving effective treatment outcomes. In 2026, the Centers for Medicare & Medicaid Services (CMS) and the National Committee for Quality Assurance (NCQA) will require payers to process clean certification applications within 30 days, underscoring the urgency and importance of timely certification.
Moreover, research indicates that a well-structured certification system highlights why credentialing is necessary to prevent the entry of untrustworthy medical professionals with questionable qualifications, which is vital for maintaining high standards in patient care. As medical institutions increasingly adopt digital verification systems, the efficiency and accuracy of this process are expected to improve, ultimately enhancing patient safety and compliance.
Healthcare Partners Consulting (HPC) provides a comprehensive credentialing service that encompasses enrollment with federal and state payers, CAQH profile setup and updates, primary source verification for education, licensure, and board certification, along with ongoing credential maintenance. Partnering with HPC not only streamlines the onboarding experience but also ensures compliance and reduces the administrative burden on medical practitioners, facilitating strategic growth in a competitive landscape.
Examine Credentialing’s Role in Protecting Patient Safety
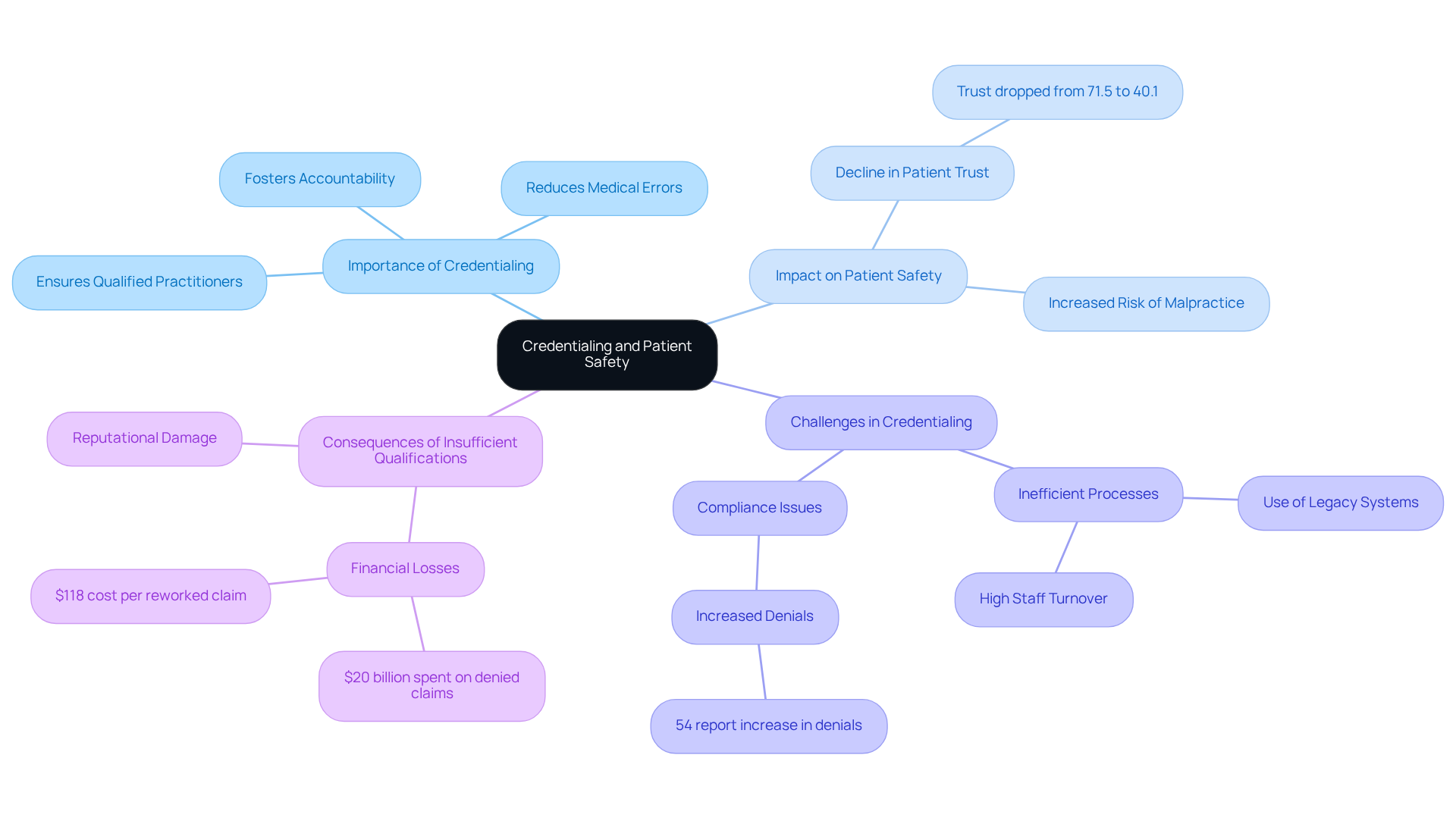
Credentialing is vital for ensuring patient safety, highlighting why credentialing is necessary to allow only qualified medical professionals to practice. This process involves thorough verification of a provider’s credentials, which significantly mitigates risks associated with medical errors and malpractice. Credentialing-related challenges are frequently cited as major compliance issues in the medical field, directly impacting patient safety. For instance, over fifty percent of medical practices have reported an increase in denials related to qualifications, underscoring the systemic problems that can arise from inadequate qualification processes.
The accreditation process highlights why credentialing is necessary by confirming that medical professionals are authorized and competent, which reduces the likelihood of unsafe practices and fosters accountability among practitioners. This is particularly crucial given the notable decline in patient trust in medical systems, which has dropped from 71.5% in April 2020 to just 40.1% by January 2024. Patients are more likely to feel secure in their care when they understand why credentialing is necessary, which highlights the importance of effective qualification practices.
Moreover, the consequences of insufficient qualifications can be severe, leading to reputational damage and financial losses for medical organizations. For example, hospitals and health systems spend nearly $20 billion annually addressing denied claims, many of which stem from authorization errors. Therefore, it is crucial to understand why credentialing is necessary for patient safety, as it serves as the first line of defense in maintaining high standards of care and ensuring that medical personnel possess the necessary qualifications to provide safe and effective treatment.
Analyze Legal and Compliance Standards in Credentialing
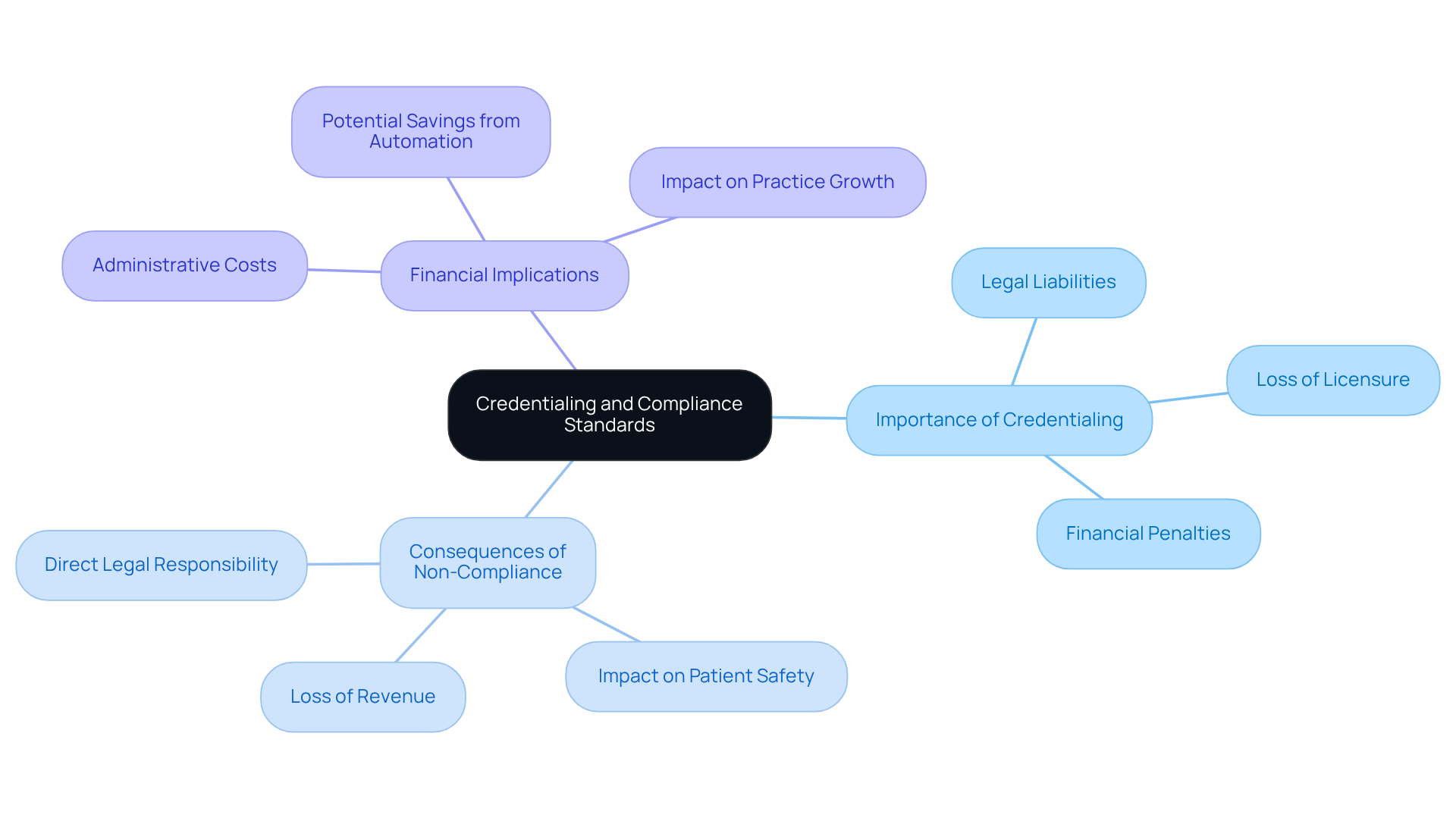
It is important to understand why credentialing is necessary to ensure that medical providers meet legal and compliance standards and possess the necessary qualifications to comply with regulatory requirements. These standards are established by governing bodies such as the National Committee for Quality Assurance (NCQA) and the Centers for Medicare & Medicaid Services (CMS). Understanding why credentialing is necessary highlights that compliance is not merely a best practice, but a legal obligation for medical organizations.
Non-compliance can lead to severe consequences, highlighting why credentialing is necessary, including:
- Legal liabilities
- Loss of licensure
- Significant financial penalties
For instance, negligent credential evaluation can expose medical organizations to direct legal responsibility that extends beyond individual doctor malpractice, as highlighted by cases discussed by Verisys.
In fact, medical organizations spend approximately $39 billion annually on administrative tasks related to regulatory compliance, underscoring the importance of robust verification procedures. By understanding and implementing these procedures, medical practitioners can mitigate risks, ensure adherence to legal standards, and ultimately safeguard patient safety and organizational integrity.
Highlight Operational Benefits of Effective Credentialing
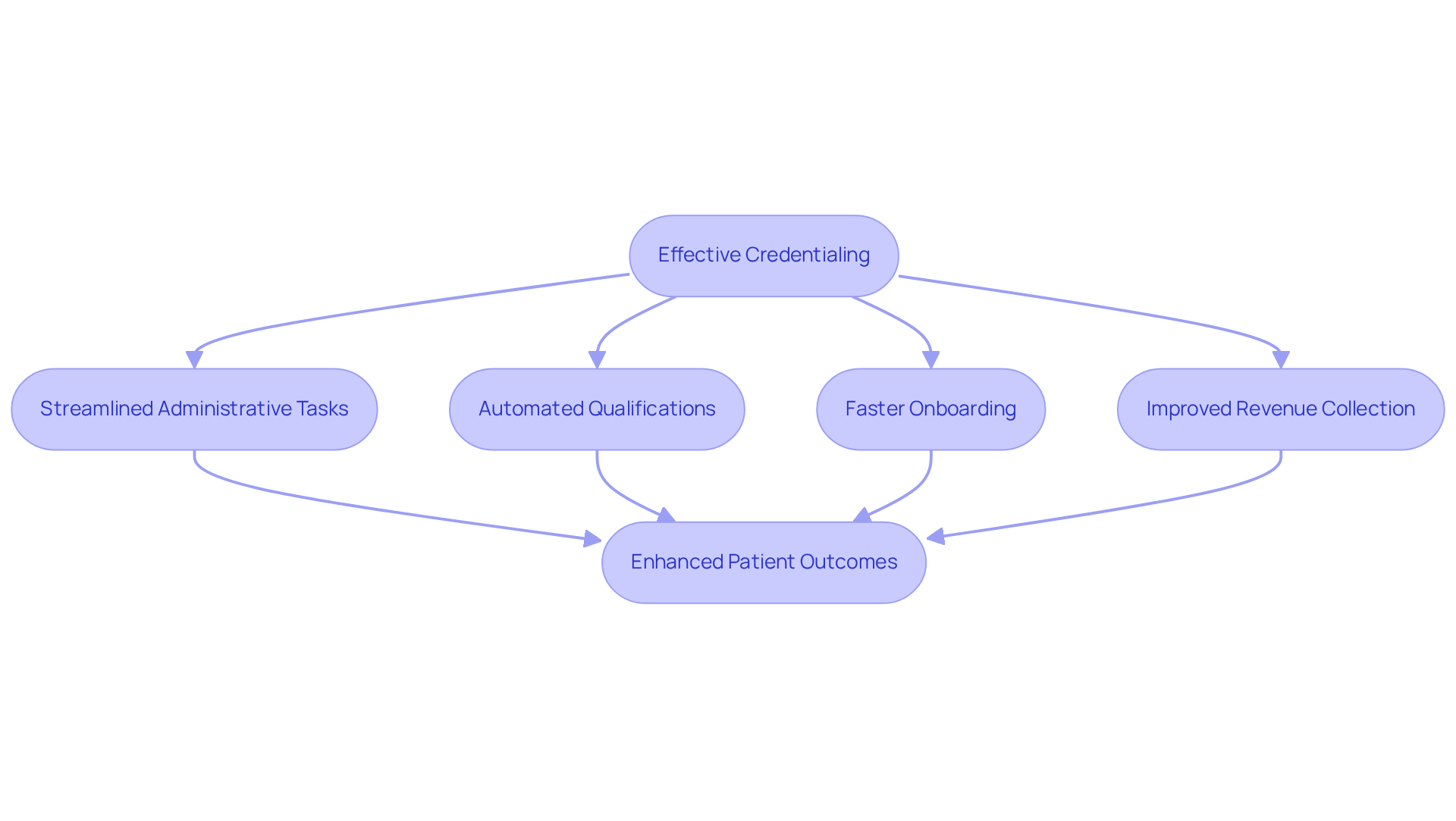
Efficient qualification processes are crucial for understanding why credentialing is necessary to ensure patient safety and provide substantial operational benefits to medical organizations. Healthcare Partners Consulting provides an Essential Credentialing Toolkit tailored for mental health practitioners, which streamlines administrative tasks for therapists and behavioral health organizations. By optimizing qualification processes, practices can significantly enhance management efficiency, allowing medical professionals to focus more on patient care rather than administrative duties.
For example, automating the cycles of qualifications and requalifications can markedly reduce the time and resources allocated to these tasks. This leads to faster onboarding of practitioners and improved revenue collection. Research indicates that medical organizations may incur losses of up to $9,000 per practitioner per day due to delays in obtaining qualifications, which emphasizes why credentialing is necessary for effective certification methods.
Moreover, efficient accreditation illustrates why credentialing is necessary, as it boosts provider morale and retention, making medical professionals feel valued in environments that prioritize compliance and quality assurance. Ultimately, the operational benefits of streamlined authorizing not only enhance healthcare systems but also contribute to better patient outcomes and organizational success. By utilizing the comprehensive credentialing and contracting services offered by Healthcare Partners Consulting-encompassing management of initial applications, ongoing maintenance, and rate negotiations-practices can optimize reimbursement and refine their administrative processes.
Conclusion
Credentialing is a vital process that ensures only qualified medical professionals are allowed to practice, thereby safeguarding patient safety and upholding the integrity of healthcare systems. By systematically verifying the qualifications, experience, and compliance of healthcare providers, credentialing serves as a crucial barrier against unqualified practitioners. This process ultimately fosters trust and enhances the quality of care delivered to patients.
The article underscores several key arguments that advocate for the necessity of credentialing. It highlights:
- The importance of adhering to legal and regulatory standards
- The operational advantages of efficient credentialing processes
- The significant risks tied to inadequate qualification verification
Furthermore, research demonstrates that effective credentialing not only reduces the likelihood of medical errors but also enhances patient trust, satisfaction, and overall outcomes.
Given these insights, it is imperative for healthcare organizations to prioritize robust credentialing practices. By doing so, they not only safeguard patient safety but also improve operational efficiency and compliance, leading to superior healthcare delivery. Embracing effective credentialing processes transcends mere regulatory obligation; it represents a fundamental commitment to quality care and patient well-being that should resonate throughout the entire healthcare landscape.
Frequently Asked Questions
What is credentialing in healthcare?
Credentialing is a formal procedure through which medical organizations confirm the qualifications, experience, and professional background of medical providers, evaluating their education, training, licenses, certifications, and work history.
Why is credentialing important in healthcare?
Credentialing is important as it serves as a barrier against unqualified practitioners entering the medical system, thereby safeguarding patient safety and upholding the integrity of medical services.
How does credentialing enhance patient care?
A well-organized credentialing system enhances the quality of care and fosters trust between patients and medical providers, which is essential for achieving effective treatment outcomes.
What upcoming requirement will the Centers for Medicare & Medicaid Services (CMS) and the National Committee for Quality Assurance (NCQA) implement regarding certification applications?
Starting in 2026, CMS and NCQA will require payers to process clean certification applications within 30 days.
What role does digital verification play in credentialing?
As medical institutions increasingly adopt digital verification systems, the efficiency and accuracy of the credentialing process are expected to improve, ultimately enhancing patient safety and compliance.
What services does Healthcare Partners Consulting (HPC) provide for credentialing?
HPC provides a comprehensive credentialing service that includes enrollment with federal and state payers, CAQH profile setup and updates, primary source verification for education, licensure, and board certification, along with ongoing credential maintenance.
How does partnering with HPC benefit medical practitioners?
Partnering with HPC streamlines the onboarding experience, ensures compliance, and reduces the administrative burden on medical practitioners, facilitating strategic growth in a competitive landscape.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting