General
Master the Prior Authorization Request Process for Your Clinic

Introduction
Healthcare clinics encounter significant challenges in managing prior authorization requests, which can impede operational efficiency and patient care. With increasing administrative burdens and the risk of denied claims, understanding the nuances of the process is essential for maintaining effective operations. This guide provides a structured overview of the essential steps involved in:
- Verifying client eligibility
- Submitting requests
- Monitoring their status
Addressing these challenges is crucial for enhancing patient outcomes and ensuring the sustainability of healthcare operations.
Check Client Eligibility
- Gather Patient Information: Collect essential details such as the patient’s full name, date of birth, policy number, and any other relevant information to assist the verification procedure.
- Contact the Insurance Provider: Utilize the insurance company’s customer service number or online portal for verification. Having the necessary patient information prepared can significantly speed up this procedure. Healthcare Partners Consulting helps you tackle credentialing delays and denials, allowing your practice to adapt to patient needs effectively.
- Confirm Coverage Details: Inquire about the specific services covered under the patient’s plan, including any limitations or exclusions. Understanding these details is crucial for determining what can be included in the prior authorization request. Accurate documentation of these details is essential for preventing future denials, as our expert coding practices ensure that all claims are compliant and justified.
- Document the Findings: Record the eligibility confirmation details, including the date, time, and representative’s name. This documentation is essential for addressing any potential issues that may emerge during the prior authorization request process. Implementing strategies to prevent modifier errors, such as using internal checklists and automated tools, enhances accuracy and minimizes denials. This leads to quicker payment turnaround and better audit protection.
Ultimately, thorough documentation and proactive management can significantly enhance the efficiency of the prior authorization request process, thereby safeguarding your practice’s financial health.
Determine Service Authorization Requirements
- Review Coverage Guidelines: Start by visiting the provider’s website or reaching out to them directly to acquire the most up-to-date guidelines on service approval requirements. Staying informed about policy updates is vital for preventing delays in patient care.
- Identify Specific Services: Start by listing the services that typically require advance authorization. Common examples in healthcare include certain medications, diagnostic tests, and specialized treatments. In mental health care, services such as psychotherapy sessions, medication management, and inpatient care often require a prior authorization request.
- Understand Medical Necessity Criteria: Familiarize yourself with the criteria that providers use to assess medical necessity for the services in question. This usually involves documenting the patient’s condition and providing a clear rationale for the proposed treatment. Understanding these criteria can significantly enhance the likelihood of approval for a prior authorization request, as denials often stem from insufficient documentation.
- Create Standardized Procedures: Implement standardized procedures and checklists for clinical notes, diagnostic codes, and treatment plans. This approach leads to quicker approvals and reduces denials, benefiting your clinic’s operations. Using the toolkit created for mental health providers by Healthcare Partners Consulting can streamline these tasks, ensuring clear action and fewer surprises.
- Consult with Colleagues: If uncertainties arise, consult with experienced colleagues to clarify approval methods. Their perspectives can be essential in managing approval methods and enhancing your clinic’s operations. Regular training for staff on payer-specific requirements can also optimize workflows and reduce administrative burdens.
- Consider Retro Approval: Be aware of the retro approval method, which is essential for ensuring providers receive proper reimbursement for services delivered without prior consent. Understanding this aspect can help mitigate revenue loss.
- Utilize Available Resources: If you face challenges with medical billing and approval processes, consider contacting the No Surprises Help Desk at 1-800-985-3059 for assistance. This resource can offer valuable assistance in navigating complex approval issues. Additionally, leveraging Healthcare Partners Consulting’s denial management services can protect your practice’s revenue by recovering previously denied claims and improving billing accuracy. Understanding these processes not only safeguards your practice’s revenue but also enhances the quality of care provided to patients.
Complete Required Forms
- Acquire the appropriate documents: access the specific forms for the prior authorization request required by the provider. These forms are typically available on their website or through their provider portal, ensuring you have the most current version.
- Fill Out the Forms Thoroughly: Ensure that all necessary information is included, such as patient demographics, insurance details, and specific service codes. Providing a clear rationale for the prior authorization request based on medical necessity is crucial. In fact, 89% of doctors report that earlier approval can help reduce burnout, which often arises from incomplete submissions.
- Attach Supporting Documentation: Include essential medical records, test results, or notes from the healthcare provider that substantiate the request. Supporting documentation is vital; 87% of pharmacists and 89% of prescribers believe that the prior authorization request adversely affects health outcomes, emphasizing the necessity for thorough evidence to support your case.
- Review for Accuracy: Before submission, meticulously double-check all entries for accuracy and completeness. Mistakes can lead to frequent setbacks or refusals. In 2023, Medicare Advantage insurers rejected 3.2 million earlier requests, either partially or completely. Ensuring everything is correct is essential to streamline the process and enhance approval rates.
Submit the Prior Authorization Request
- Choose the submission method: Selecting the most efficient method for prior authorization requests is crucial for optimizing healthcare operations. Options include electronic submissions through the insurance provider’s portal, fax, or traditional mail. Electronic submissions are generally preferred, as they can expedite the process significantly. As of 2026, only 35% of health plans utilize complete electronic pre-approval systems. This statistic highlights a significant opportunity for improvement in the prior authorization request process. Healthcare Partners Consulting (HPC) is committed to helping practices evolve by adapting to these changes and ensuring that your submissions are handled swiftly and effectively.
- Follow Submission Guidelines: It is essential to comply rigorously with the submission guidelines specified by the provider. This includes adhering to any specified formats and providing all necessary documentation. Recent changes in submission guidelines emphasize the importance of clarity and completeness to avoid delays in processing. HPC’s proactive issue management ensures that any potential credentialing delays or denials are addressed promptly, allowing your practice to focus on patient care.
- Keep a Copy of the Submission: Always retain a copy of your submitted request along with any accompanying documents. This practice is essential for tracking your submissions and can be invaluable if you need to follow up or appeal a denial later. Doctors indicate that investing an average of almost $83,000 each year engaging with coverage plans emphasizes the challenge of the prior authorization request process. With HPC’s administrative support, practices can streamline these interactions, improving cash flow and reducing denials.
- Confirm Receipt: If you submit your request via fax or mail, it is advisable to confirm receipt with the insurance provider. This can typically be done by calling their customer service line. Confirming that your request has been acknowledged can prevent unnecessary delays and promote a smoother approval experience. Beginning in 2026, payers must provide specific justifications for every denial, which can further influence the submission procedure. HPC’s comprehensive administrative support helps navigate these complexities, ensuring that your practice remains compliant and efficient.
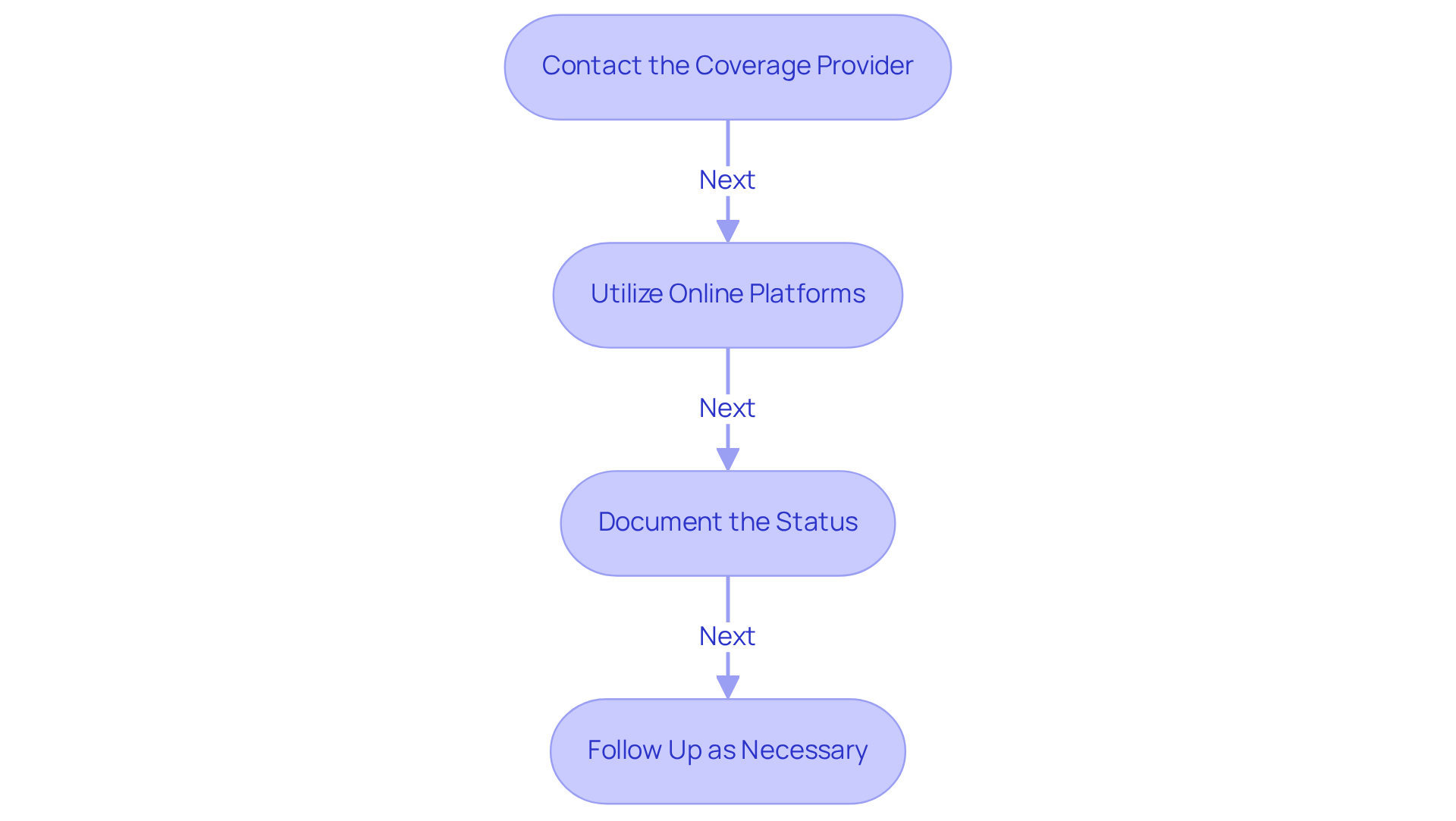
Check Authorization Status
- Contact the Coverage Provider: Reach out to the coverage company using the contact details provided during the submission procedure. Be prepared with the patient’s information and the details of the request.
- Utilize online platforms: If accessible, log into the provider’s online platform to verify the status of the prior authorization request. Many insurers offer real-time updates through their systems, which can expedite the process.
- Document the Status: Maintain a detailed record of the approval request status, including notes from any conversations with insurance representatives regarding timelines or additional information required.
- Follow Up as Necessary: If the approval is delayed or denied, follow up promptly to resolve any issues. Delays or denials in approval requests can create significant challenges for healthcare providers. This may involve submitting additional documentation or clarifying the medical necessity of the requested service. Research indicates that 94% of doctors find it necessary to follow up on prior authorization requests, highlighting the importance of persistence. As Dr. Jack Resneck, former AMA President, noted, physicians spend approximately 15 hours a week just filling out forms and waiting on hold for insurance companies, illustrating the challenges posed by administrative tasks. Additionally, the 2024 AMA survey revealed that doctors handle an average of 39 requests for pre-approval each week, emphasizing the importance of thorough follow-up. Collaborating with Healthcare Partners Consulting can enhance onboarding efficiency, ensure consistent payor compliance, and reduce administrative burdens, allowing providers to focus more on patient care rather than paperwork. With upcoming changes in 2026 aimed at streamlining the prior authorization request process, staying proactive in follow-ups will be crucial for ensuring timely patient care.
Conclusion
Navigating the complexities of prior authorization is crucial for clinics striving to enhance operational efficiency and patient care. Implementing a systematic approach to client eligibility verification and understanding service authorization requirements allows healthcare providers to reduce delays and denials effectively. This proactive management safeguards the practice’s financial health while ensuring timely patient access to necessary treatments.
Throughout the article, key strategies have been highlighted, including:
- The importance of thorough documentation
- The use of standardized procedures
- Effective follow-up practices
Gathering accurate patient information and consulting with colleagues enables clinics to navigate prior authorization complexities more efficiently. Additionally, staying informed about the latest policy updates and submission guidelines is crucial in preventing potential setbacks.
Ultimately, the significance of a well-structured prior authorization process cannot be overstated. As healthcare continues to evolve, embracing best practices in prior authorization not only enhances operational efficiency but also improves patient outcomes. Clinics are encouraged to prioritize these strategies and consider partnering with specialized consulting services to further optimize their workflows. Prioritizing these strategies will not only streamline administrative processes but also elevate the standard of patient care delivered.
Frequently Asked Questions
What information is needed to check client eligibility?
Essential details include the patient’s full name, date of birth, policy number, and any other relevant information to assist the verification procedure.
How can I verify a patient’s insurance coverage?
You can verify coverage by contacting the insurance provider through their customer service number or online portal, using the prepared patient information to speed up the process.
Why is it important to confirm coverage details?
Confirming coverage details is crucial for understanding the specific services covered under the patient’s plan, including any limitations or exclusions, which helps in preparing accurate prior authorization requests.
What should be documented after confirming eligibility?
Document the eligibility confirmation details, including the date, time, and representative’s name, to address any potential issues during the prior authorization request process.
What are the steps to determine service authorization requirements?
Steps include reviewing coverage guidelines, identifying specific services that require authorization, understanding medical necessity criteria, creating standardized procedures, consulting with colleagues, considering retro approval, and utilizing available resources.
What types of services typically require advance authorization?
Common services that often require advance authorization include certain medications, diagnostic tests, specialized treatments, psychotherapy sessions, medication management, and inpatient care.
How can I enhance the likelihood of approval for a prior authorization request?
Familiarize yourself with medical necessity criteria, document the patient’s condition clearly, and ensure that your documentation meets the requirements to avoid denials.
What resources are available for assistance with medical billing and approval processes?
You can contact the No Surprises Help Desk at 1-800-985-3059 for assistance, and consider leveraging Healthcare Partners Consulting’s denial management services to recover denied claims and improve billing accuracy.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting