Mastering Medical Coding
Understanding the New Patient Exam CPT Code for Mental Health Clinics

Introduction
Navigating the complexities of mental health billing is crucial for practitioners who seek to deliver quality care while maintaining financial stability. The introduction of the new patient exam CPT code has transformed how mental health services are documented and reimbursed, offering a structured approach to initial assessments. Practitioners must develop strategies to navigate the complexities of these coding requirements, ensuring both revenue optimization and compliance.
Define the New Patient Exam CPT Code
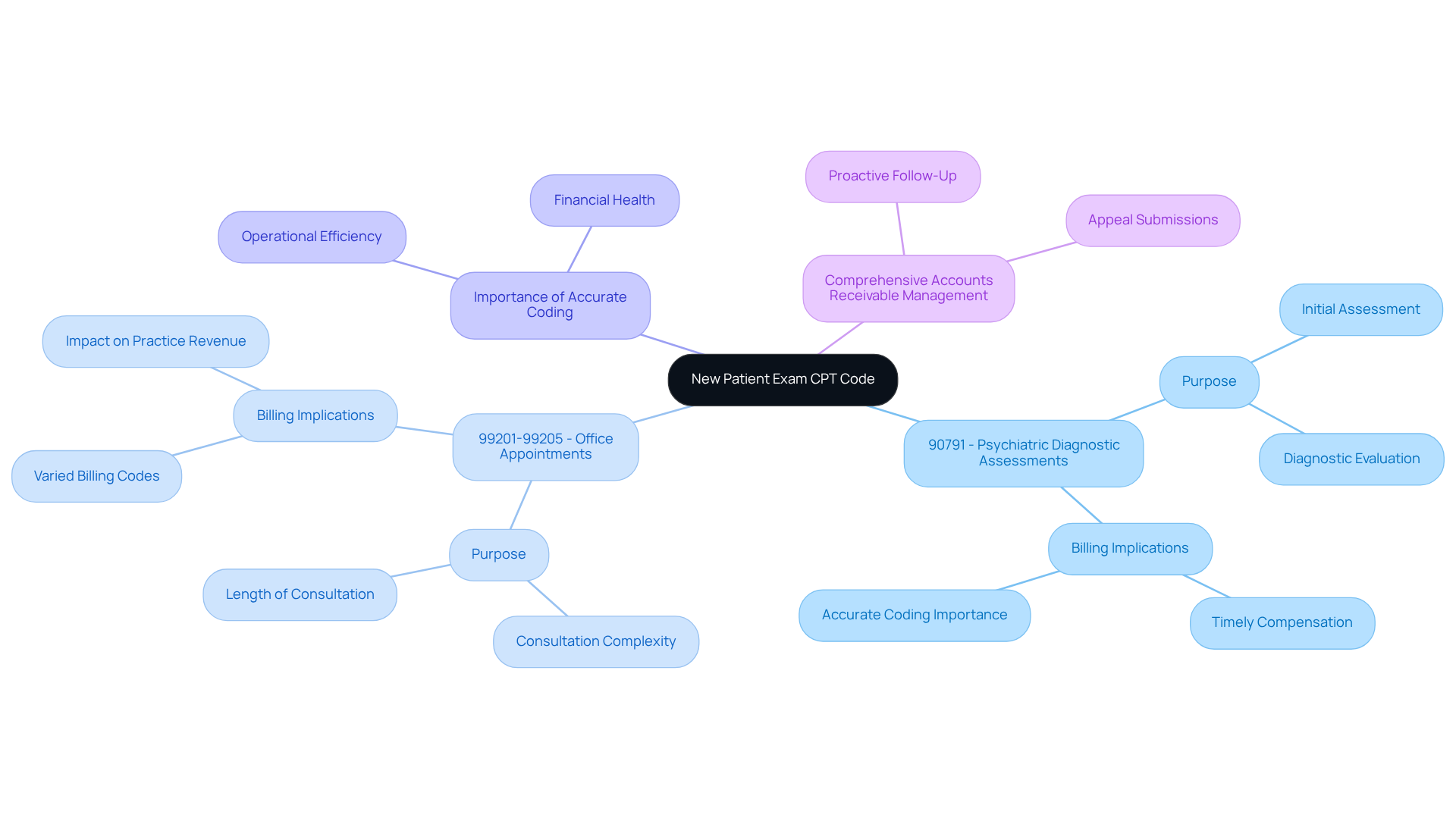
The new patient exam cpt code specifies numbers for billing initial assessments of individuals who have not received services from the same provider or specialty in the past three years. In the field of psychological well-being, these designations mainly encompass:
- 90791 for psychiatric diagnostic assessments
- 99201-99205 for office appointments, which differ depending on the intricacy and length of the consultation, including the new patient exam cpt code.
Accurate coding ensures mental health practitioners receive timely compensation for their evaluations. Such evaluations are crucial for formulating effective treatment plans and gaining a comprehensive understanding of the patient’s needs. Staying updated on these codes can significantly improve a practice’s financial health and operational efficiency.
By utilizing comprehensive accounts receivable management solutions from Healthcare Partners Consulting, including proactive follow-up with payers and appeal submissions for denied claims, clinics focused on psychological services can enhance cash flow, decrease denials, and simplify compliance, ensuring that precise coding facilitates prompt reimbursements and promotes sustainable growth.
Contextualize the New Patient Exam CPT Code in Mental Health Billing
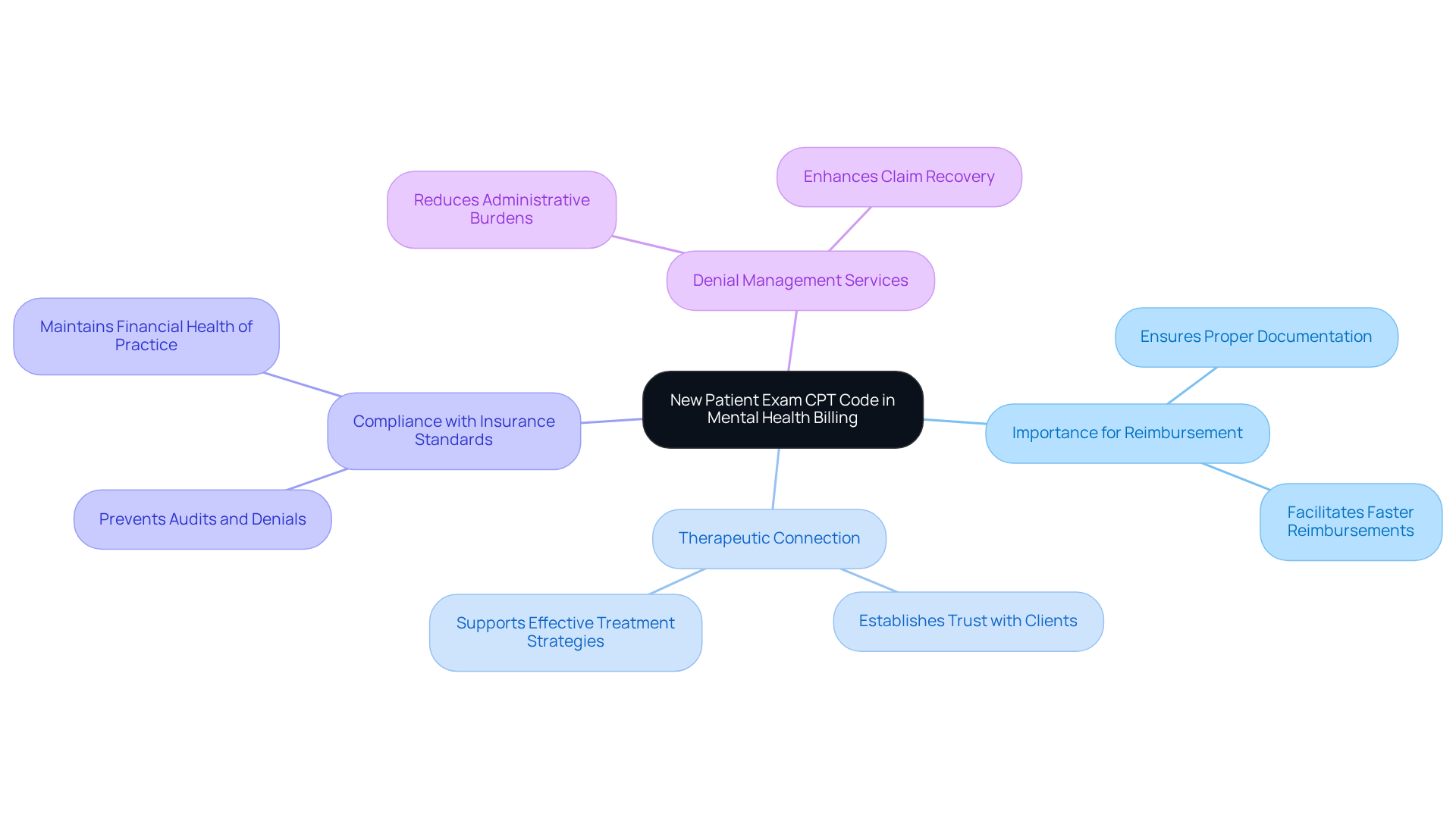
In psychological billing, the new patient exam cpt code is crucial for ensuring proper reimbursement for practitioners. It allows psychological professionals to document and charge for the comprehensive evaluation of new clients, specifically utilizing the new patient exam cpt code. Without a thorough evaluation, establishing a therapeutic connection becomes challenging, which is crucial for developing an effective treatment strategy.
The utilization of the new patient exam cpt code ensures that providers receive compensation for their time and expertise. This is particularly important given the increasing demand for psychological services. Moreover, precise coding that includes the new patient exam cpt code assists practices in maintaining compliance with insurance standards and preventing potential audits or denials. Accurate coding, particularly the new patient exam cpt code, not only ensures compliance but also directly contributes to the financial health of the practice.
By leveraging Healthcare Partners Consulting’s denial management services, including claim recovery and streamlined workflows, practices can protect their revenue and reduce administrative burdens. This maximizes practice revenue while ensuring accurate and compliant coding. Consequently, practices experience faster reimbursements and improved financial outcomes.
Trace the Origin and Development of the New Patient Exam CPT Code
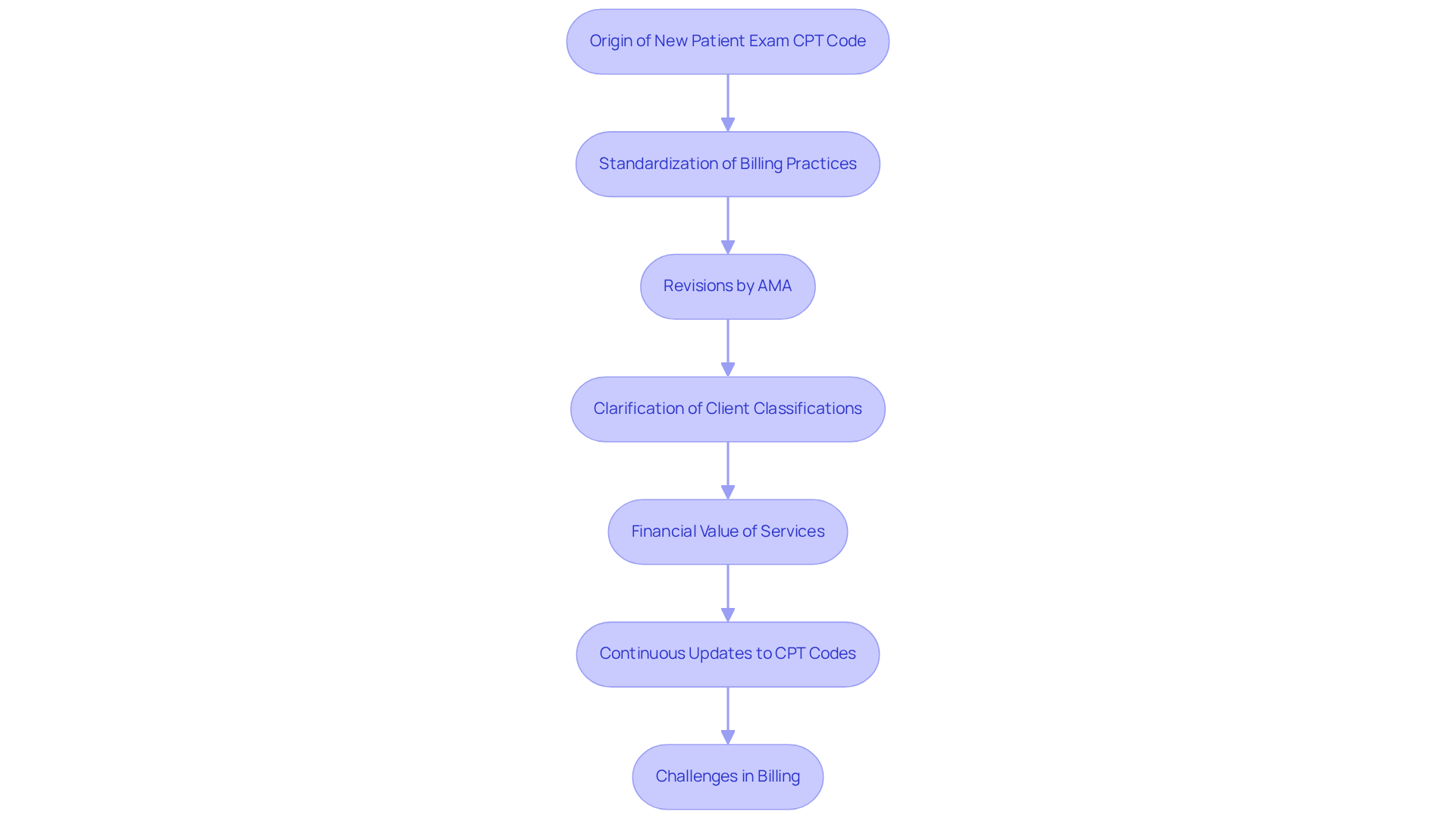
The evolution of the new patient exam CPT code underscores the ongoing challenges and advancements in psychological care. Initially established to standardize billing practices across various medical specialties, the coding system has undergone significant revisions by the American Medical Association (AMA) to align with advancements in clinical practices and treatment methodologies.
The implementation of specific classifications for psychiatric assessments has clarified the distinction between new clients and existing clients, which is essential for precise documentation and billing, including the new patient exam CPT code. This evolution highlights a broader acknowledgment of the complexities inherent in psychological care, emphasizing the necessity for appropriate compensation for providers.
For example, the 2026 Medicare rate for the initial psychiatric assessment 90792 is approximately $171.77, while the rate for group psychotherapy (CPT 90853) is around $30.39 per individual, demonstrating the financial value of these services. Moreover, the AMA’s continuous updates to CPT codes, including recent changes that improve definitions and documentation requirements, reflect a commitment to enhancing the representation of psychological services.
These changes not only promote improved billing practices but also assist providers in delivering high-quality care, ultimately enhancing patient outcomes. Despite these advancements, providers still face significant challenges in navigating the complexities of psychological billing, with frequent mistakes such as time-code mismatches and insufficient documentation resulting in higher denial rates, which can reach 15-20%-more than double the rate of general medical claims.
As emphasized by Davia Ward, tackling the billing crisis in psychological services necessitates thorough accounts receivable management solutions, including proactive follow-up with payers on outstanding claims and appeal submissions for rejected claims. For instance, a case study shows how these CPT classification changes can positively impact a psychological practice by demonstrating how precise labeling and documentation, coupled with effective accounts receivable strategies, can enhance cash flow and reduce denials.
Ultimately, the effectiveness of these changes hinges on the ability of providers to adapt and implement robust billing practices.
Identify Key Characteristics of the New Patient Exam CPT Code
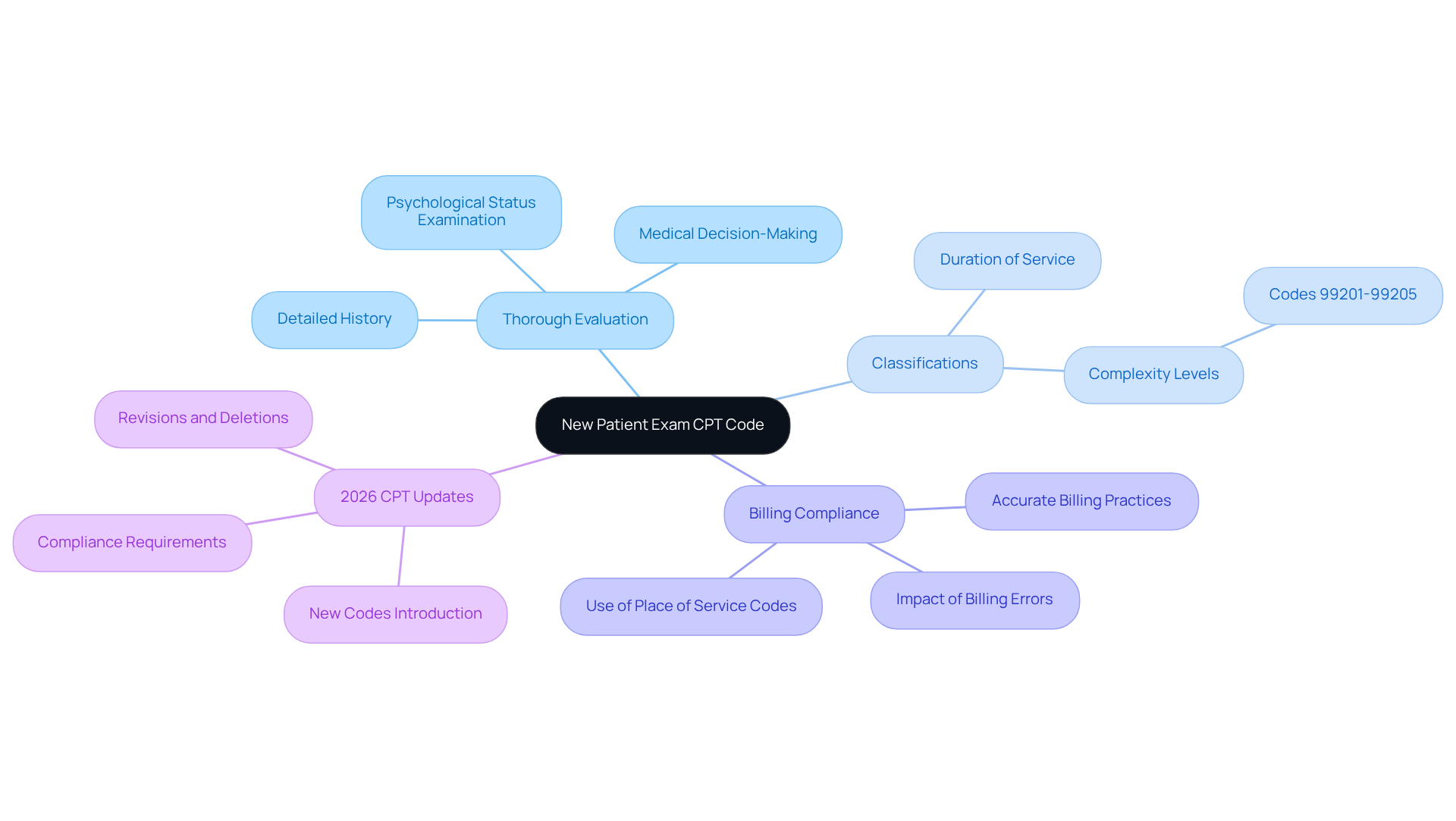
For mental health providers, a comprehensive understanding of the new patient exam CPT code is crucial to ensure accurate billing and compliance with insurance regulations. Key characteristics of this code include the necessity for a thorough evaluation, which typically encompasses a detailed history, psychological status examination, and medical decision-making. These classifications reflect the complexity of the initial client interaction, including the individual’s mental health history, current symptoms, and relevant psychosocial factors.
Furthermore, the classifications vary depending on the duration spent with the patient and the intricacy of the medical decision-making involved. For instance, codes 99201-99205 are tiered based on the level of service provided, with higher numbers indicating more complex evaluations. Understanding these characteristics is essential for mental health providers to ensure accurate billing, particularly with the new patient exam CPT code, and compliance with insurance regulations.
The 2026 CPT updates, effective January 1, 2026, highlight the significance of comprehensive assessments and precise billing practices, as billing errors can result in significant financial losses for practices, underscoring the need for precise coding and billing practices. Additionally, using the correct Place of Service (POS) codes is essential, as it can significantly affect reimbursement rates.
At Healthcare Partners Consulting, we specialize in providing tailored coding support and comprehensive revenue cycle management services, ensuring that mental health providers can navigate these complexities effectively and optimize their patient revenue activities. Ultimately, the right coding practices not only safeguard revenue but also enhance the overall sustainability of mental health services.
Conclusion
Navigating the complexities of the new patient exam CPT code is crucial for mental health clinics aiming for operational efficiency and financial stability. This code facilitates accurate billing for initial assessments. It also highlights the importance of thorough evaluations for effective treatment plans. By grasping the nuances of these codes, mental health providers can ensure they receive appropriate compensation for their expertise, ultimately benefiting both their practice and their clients.
The article highlighted several key aspects of the new patient exam CPT code, including its specific classifications, the historical context of its development, and its critical role in mental health billing. Accurate coding, particularly for initial psychiatric assessments, is vital for compliance with insurance standards and for minimizing the risk of claim denials. Moreover, the ongoing evolution of these codes reflects the complexities and advancements in psychological care, emphasizing the need for mental health professionals to stay informed and adaptable.
In conclusion, the significance of the new patient exam CPT code extends beyond mere billing; it is a fundamental element that can enhance the quality of care provided to clients. Mental health practitioners should invest in robust billing practices and seek support from specialized consulting services to navigate these complexities effectively. By mastering these billing practices, mental health practitioners can ensure their services remain viable and responsive to the increasing demand for psychological care.
Frequently Asked Questions
What is the new patient exam CPT code?
The new patient exam CPT code specifies numbers for billing initial assessments of individuals who have not received services from the same provider or specialty in the past three years.
What are the specific codes used for new patient exams in psychological services?
The specific codes include 90791 for psychiatric diagnostic assessments and 99201-99205 for office appointments, which vary based on the complexity and length of the consultation.
Why is accurate coding important for mental health practitioners?
Accurate coding ensures that mental health practitioners receive timely compensation for their evaluations, which are essential for creating effective treatment plans and understanding patient needs.
How can staying updated on CPT codes benefit a practice?
Staying updated on these codes can significantly improve a practice’s financial health and operational efficiency.
What solutions can help clinics improve their cash flow and decrease claim denials?
Comprehensive accounts receivable management solutions from Healthcare Partners Consulting, including proactive follow-up with payers and appeal submissions for denied claims, can enhance cash flow and decrease denials.
How does precise coding contribute to a clinic’s growth?
Precise coding facilitates prompt reimbursements and promotes sustainable growth within clinics focused on psychological services.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting