Revenue Cycle Management Best Practices
4 Best Practices for Electronic Medical Billing Software in Clinics

Introduction
Healthcare facilities face significant challenges due to outdated billing systems that impede operational efficiency. The adoption of electronic medical billing software enables clinics to achieve streamlined operations, enhanced accuracy, and improved regulatory compliance. However, the challenge lies in selecting the right software and implementing best practices to maximize its potential.
What essential strategies can clinics implement to transform billing inefficiencies into a streamlined revenue cycle?
Identify Essential Features of Electronic Medical Billing Software
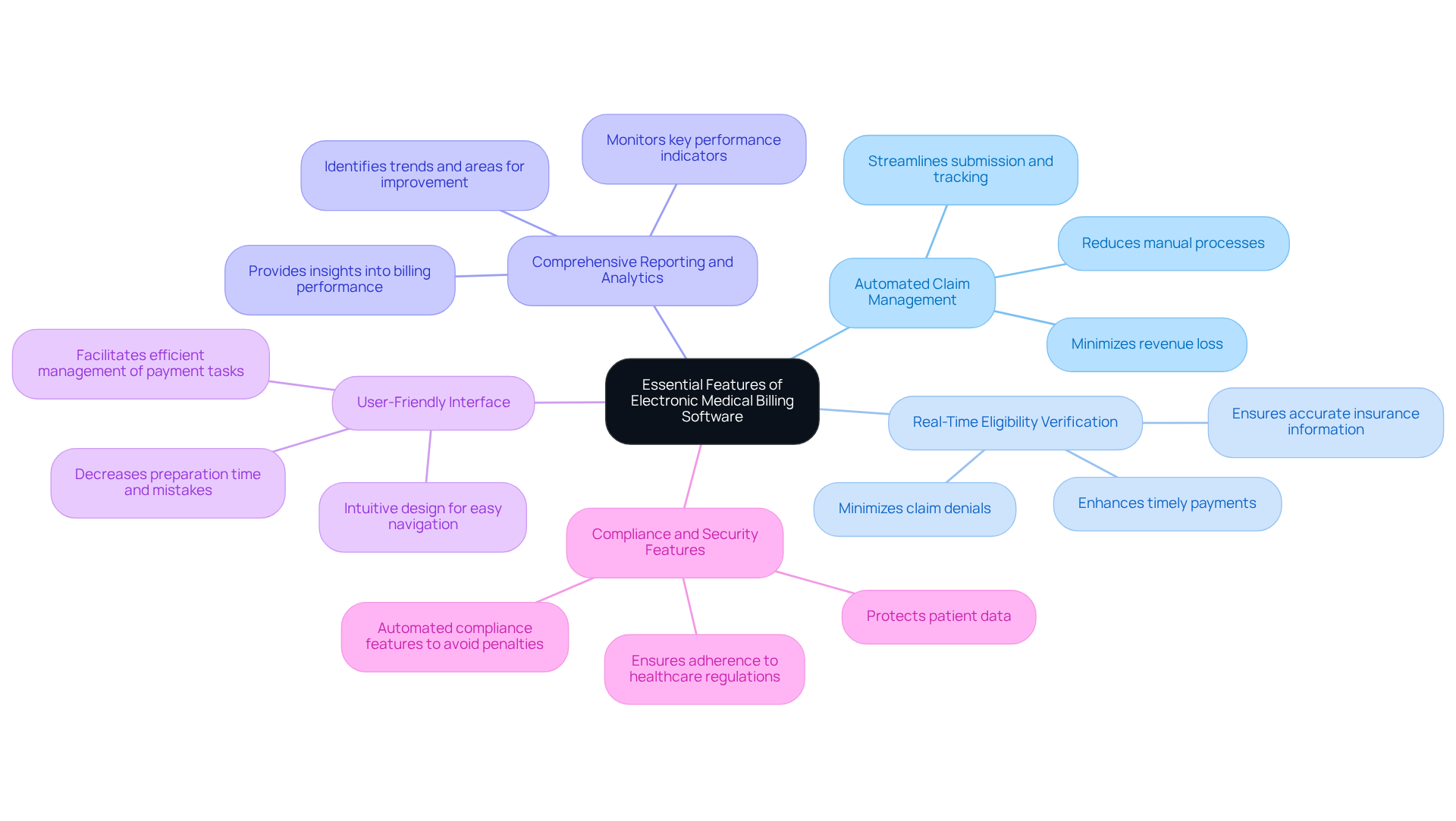
Healthcare facilities often struggle with inefficiencies in their invoicing processes, making the choice of electronic medical billing software critical. When selecting electronic medical billing software, healthcare facilities should prioritize features that significantly enhance efficiency and precision. Key features to consider include:
- Automated Claim Management: This feature streamlines the submission and tracking of claims, significantly reducing the time spent on manual processes. Automation minimizes revenue loss by addressing root causes in documentation and coding, allowing staff to focus on higher-value tasks that support patient care.
- Real-Time Eligibility Verification: This ensures that patient insurance information is accurate before services are rendered, which minimizes claim denials and enhances the likelihood of timely payments. Automated eligibility checks verify coverage details as soon as patient information is entered, reducing the risk of retroactive denials.
- Comprehensive Reporting and Analytics: This provides insights into billing performance, helping practices identify trends and areas for improvement. Effective reporting features enable clinics to monitor key performance indicators and adjust strategies accordingly.
- User-Friendly Interface: A simple, intuitive design enables staff to navigate the application effortlessly, decreasing preparation time and mistakes. This ease of use is essential for ensuring that all team members can efficiently manage payment tasks without extensive training.
- Compliance and Security Features: These are essential for protecting patient data and adhering to healthcare regulations, including HIPAA. Automated compliance features help practices avoid penalties and maintain alignment with evolving industry standards.
Ultimately, the right software choice can transform operational capabilities and ensure compliance in an ever-evolving regulatory landscape.
Ensure Compatibility with Existing EHR Systems
Clinics face significant challenges in integrating electronic medical billing software with their existing Electronic Health Record (EHR) systems, which can impact operational efficiency. Here are essential steps to achieve seamless integration:
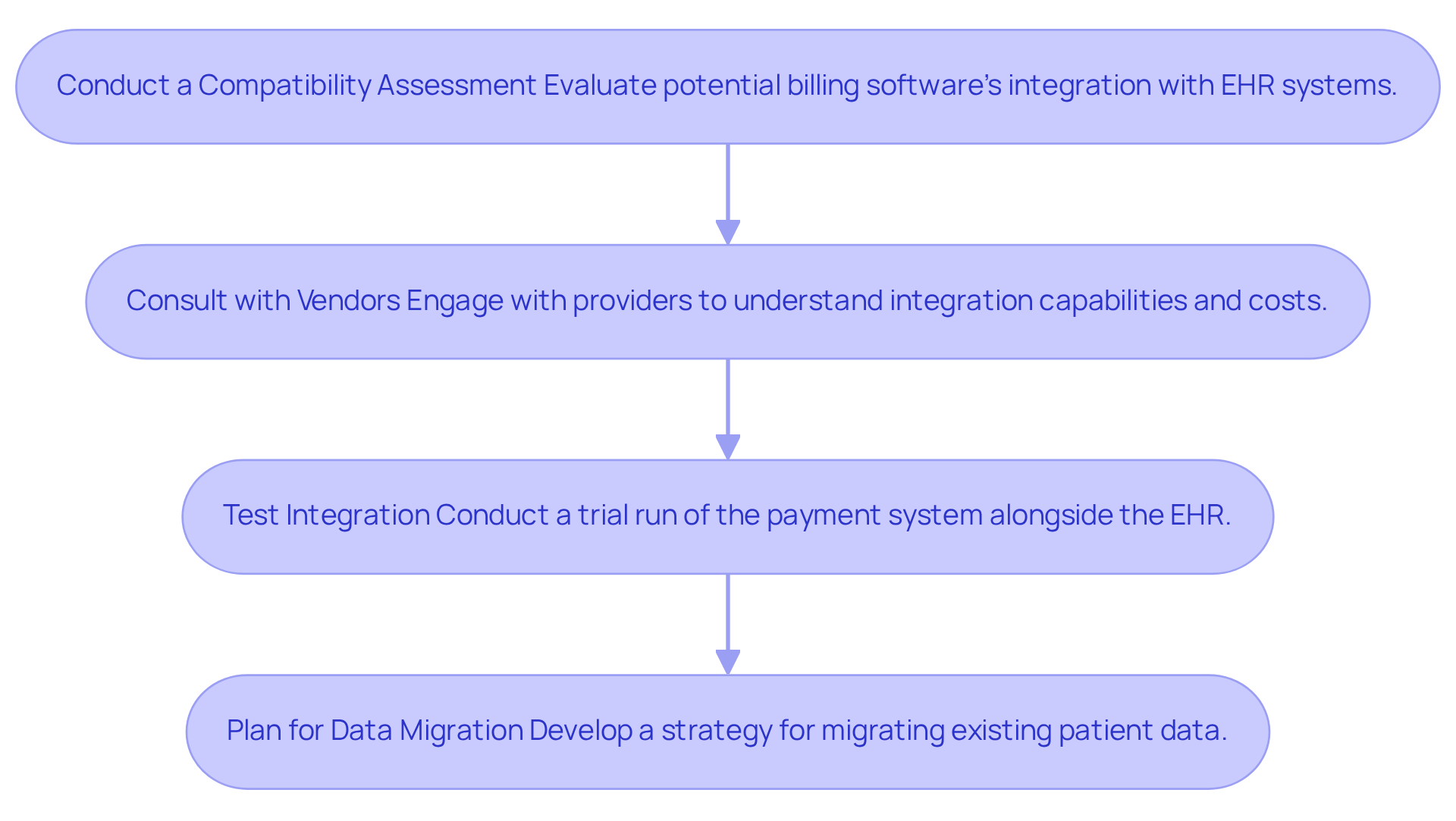
- Conduct a Compatibility Assessment: Evaluate how well potential billing software integrates with your current EHR system. Prioritize solutions that support widely accepted data exchange standards such as HL7 or FHIR, which facilitate smoother interoperability.
- Consult with Vendors: Engage with providers to gain insights into their integration capabilities. Inquire about any additional costs that may arise during the integration process to avoid unexpected expenses.
- Test Integration: If possible, conduct a trial run of the payment system alongside your EHR. This testing phase can help identify potential issues early, allowing for adjustments before full implementation.
- Plan for Data Migration: Develop a comprehensive strategy for migrating existing patient data to the new system. This plan should prioritize data integrity to prevent loss or corruption during the transition.
Failure to integrate effectively can result in increased administrative burdens and hindered financial performance. By concentrating on compatibility and ensuring HIPAA compliance, healthcare facilities can significantly improve operational efficiency through the use of electronic medical billing software. Effective denial management is crucial; for instance, a small primary care practice in Ohio achieved a 30% reduction in claim denials after implementing an FHIR-based integration platform. Ultimately, effective integration not only enhances operational efficiency but also safeguards the financial viability of healthcare practices.
Provide Comprehensive Training and Ongoing Support
Without a comprehensive training program, clinics risk facing significant billing inaccuracies that can disrupt operations. To maximize the effectiveness of electronic medical billing software, clinics must implement a comprehensive training program that encompasses several key components:
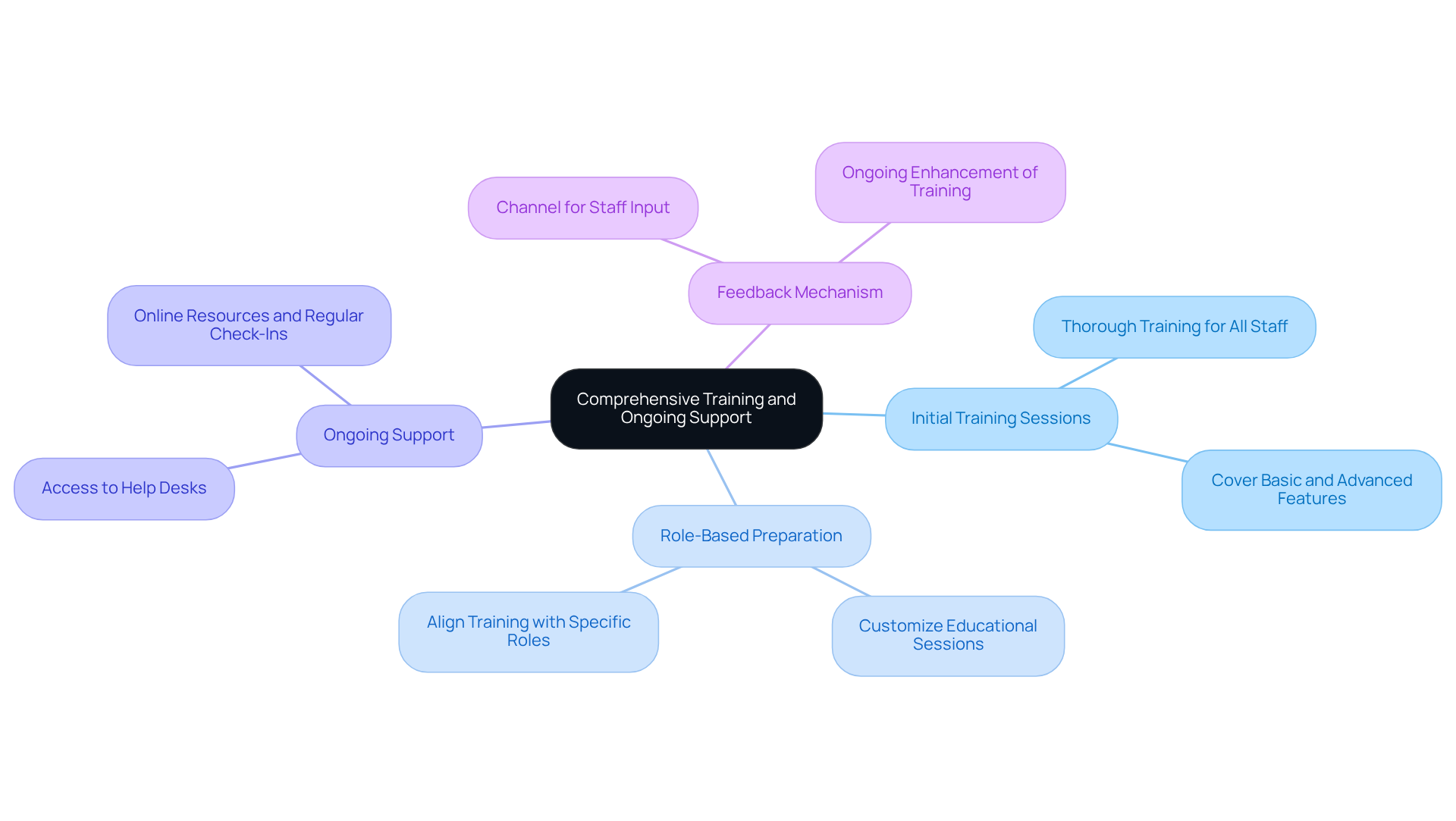
- Initial Training Sessions: Conduct thorough training for all staff members who will utilize the software, covering both basic functionalities and advanced features to ensure a solid foundation.
- Role-Based Preparation: Customize educational sessions to align with specific roles within the clinic. This approach ensures that each team member understands how to utilize the system effectively in relation to their unique responsibilities, enhancing both accuracy and efficiency in billing processes.
- Ongoing Support: Establish a robust support system that includes access to help desks, online resources, and regular check-ins. This ongoing support is crucial for addressing any issues that may arise after implementation, fostering a smoother operational flow.
- Feedback Mechanism: Establish a channel for staff to provide input on the software and the development process. This feedback loop is crucial for ongoing enhancement, enabling facilities to adjust and optimize their development and support approaches.
Ultimately, the right training and support can redefine a clinic’s operational success, leading to a more streamlined and effective billing process.
Monitor Performance and Optimize Usage of Billing Software
Without regular performance monitoring, clinics risk falling short of their billing potential. To maximize the effectiveness of electronic medical billing software, clinics should implement the following strategies:
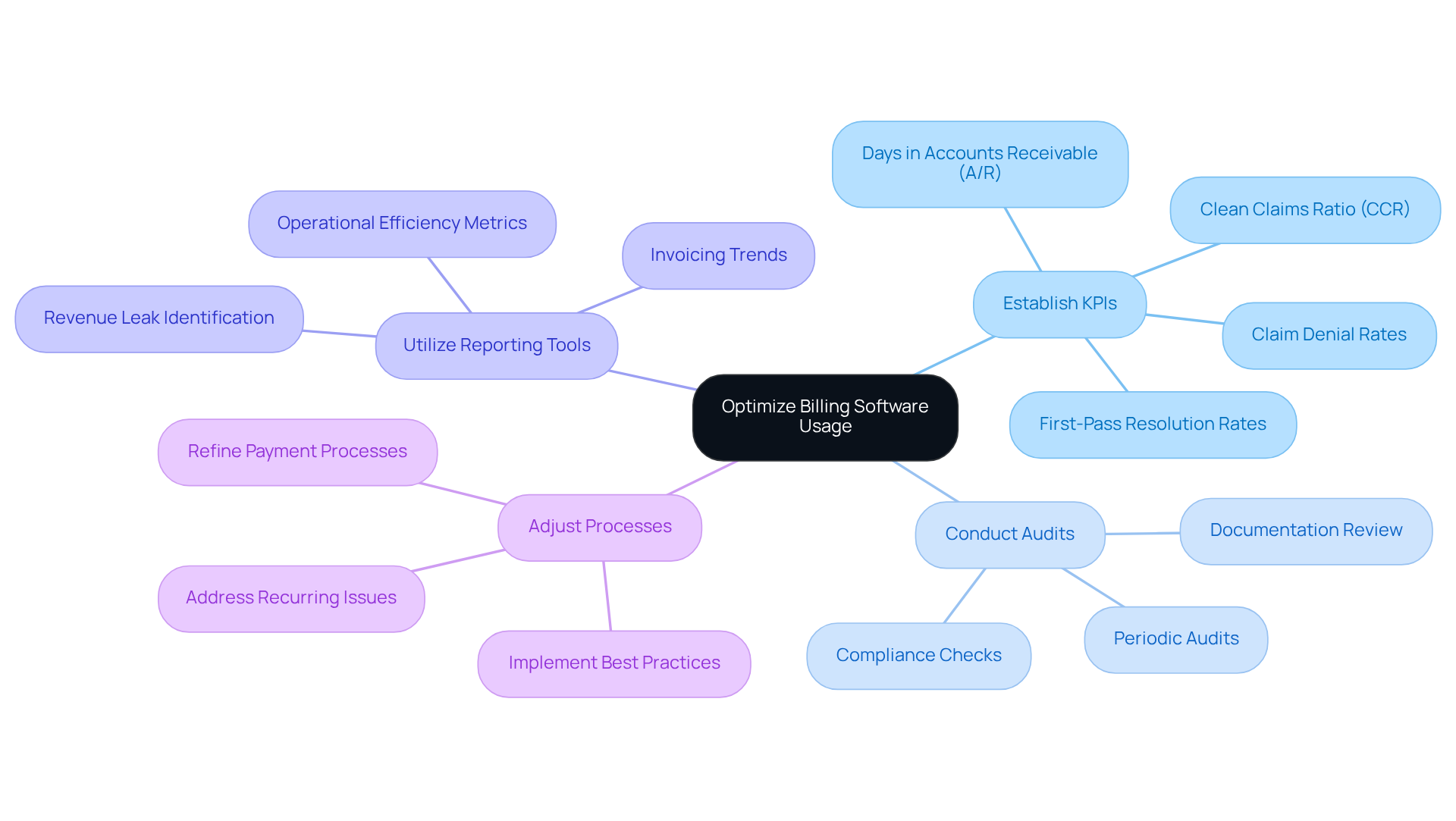
- Establish Key Performance Indicators (KPIs): Identify essential metrics such as claim denial rates, days in accounts receivable (A/R), and first-pass resolution rates. Practices with a robust KPI tracking system can achieve a 15% higher revenue collection rate compared to those without one. Maintaining a clean claims ratio (CCR) of 70% to 85% is also crucial, with a CCR above 90% indicating an effective revenue cycle management strategy.
- Conduct Regular Audits: Schedule periodic audits of invoicing processes to identify discrepancies, compliance issues, and areas for improvement. Stricter audits and AI flags for vague documentation have led to a 26% increase in outpatient denials from 2024 to 2025, highlighting the need for thorough documentation and compliance checks.
- Utilize Reporting Tools: Leverage the reporting capabilities of the invoicing software to generate insights into invoicing trends and operational efficiency. Consistent tracking of essential metrics, such as submission lag and unbilled charges, can assist facilities in identifying revenue leaks and enhancing staff productivity.
- Adjust Processes Based on Data: Use the data collected to refine payment processes, implement best practices, and address any recurring issues. For example, healthcare facilities should strive to gather 60% to 70% of patient responsibility at or before the time of service to reduce bad debt and enhance cash flow.
Neglecting these strategies could lead to significant revenue losses and hinder the financial stability of clinics.
Conclusion
Choosing the appropriate electronic medical billing software is crucial for healthcare clinics, impacting both efficiency and financial outcomes. By focusing on essential features such as:
- Automated claim management
- Real-time eligibility verification
- Comprehensive reporting
clinics can significantly enhance their billing processes. Additionally, ensuring compatibility with existing EHR systems and providing thorough training are critical for a seamless transition. Monitoring performance further enhances optimal software usage.
Throughout this article, key insights have been highlighted, including the importance of:
- Conducting compatibility assessments
- Engaging with software vendors
- Implementing a robust training program tailored to staff roles
Regular performance monitoring through established KPIs and audits empowers clinics to identify areas for improvement and refine their billing strategies. The cumulative effect of these best practices is a more efficient billing system that not only reduces errors but also maximizes revenue potential.
Adopting these best practices in electronic medical billing is vital for clinics seeking to excel in a competitive healthcare environment. As the industry evolves, prioritizing the right features, ensuring integration with existing systems, and committing to ongoing training and support will prove invaluable. By proactively implementing these strategies, healthcare facilities can ensure financial viability and improve patient care, fostering a sustainable practice.
Frequently Asked Questions
Why is choosing the right electronic medical billing software important for healthcare facilities?
Choosing the right electronic medical billing software is critical for healthcare facilities as it addresses inefficiencies in invoicing processes, enhances efficiency and precision, and ultimately transforms operational capabilities.
What is automated claim management in electronic medical billing software?
Automated claim management streamlines the submission and tracking of claims, reducing the time spent on manual processes and minimizing revenue loss by addressing documentation and coding issues.
How does real-time eligibility verification benefit healthcare facilities?
Real-time eligibility verification ensures that patient insurance information is accurate before services are rendered, which minimizes claim denials and enhances the likelihood of timely payments by verifying coverage details as soon as patient information is entered.
What role does comprehensive reporting and analytics play in electronic medical billing software?
Comprehensive reporting and analytics provide insights into billing performance, helping practices identify trends and areas for improvement, and enabling clinics to monitor key performance indicators to adjust strategies accordingly.
Why is a user-friendly interface important in electronic medical billing software?
A user-friendly interface is important because it allows staff to navigate the application effortlessly, decreasing preparation time and mistakes, thus ensuring that all team members can efficiently manage payment tasks without extensive training.
What compliance and security features should be considered in electronic medical billing software?
Compliance and security features are essential for protecting patient data and adhering to healthcare regulations, including HIPAA. Automated compliance features help practices avoid penalties and maintain alignment with evolving industry standards.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting