Mastering Medical Coding
Master CPT Code 99417: Best Practices for Mental Health Billing Success

Introduction
Mastering CPT Code 99417 is essential for mental health providers aiming to enhance billing accuracy and ensure fair compensation for their services. This code facilitates the documentation of prolonged outpatient services while enhancing billing accuracy and ensuring financial sustainability.
However, mental health providers face significant challenges in billing processes and the risk of claim denials. To ensure financial sustainability, mental health practices must adopt strategies that enhance billing accuracy.
Understand CPT Code 99417: Definition and Importance
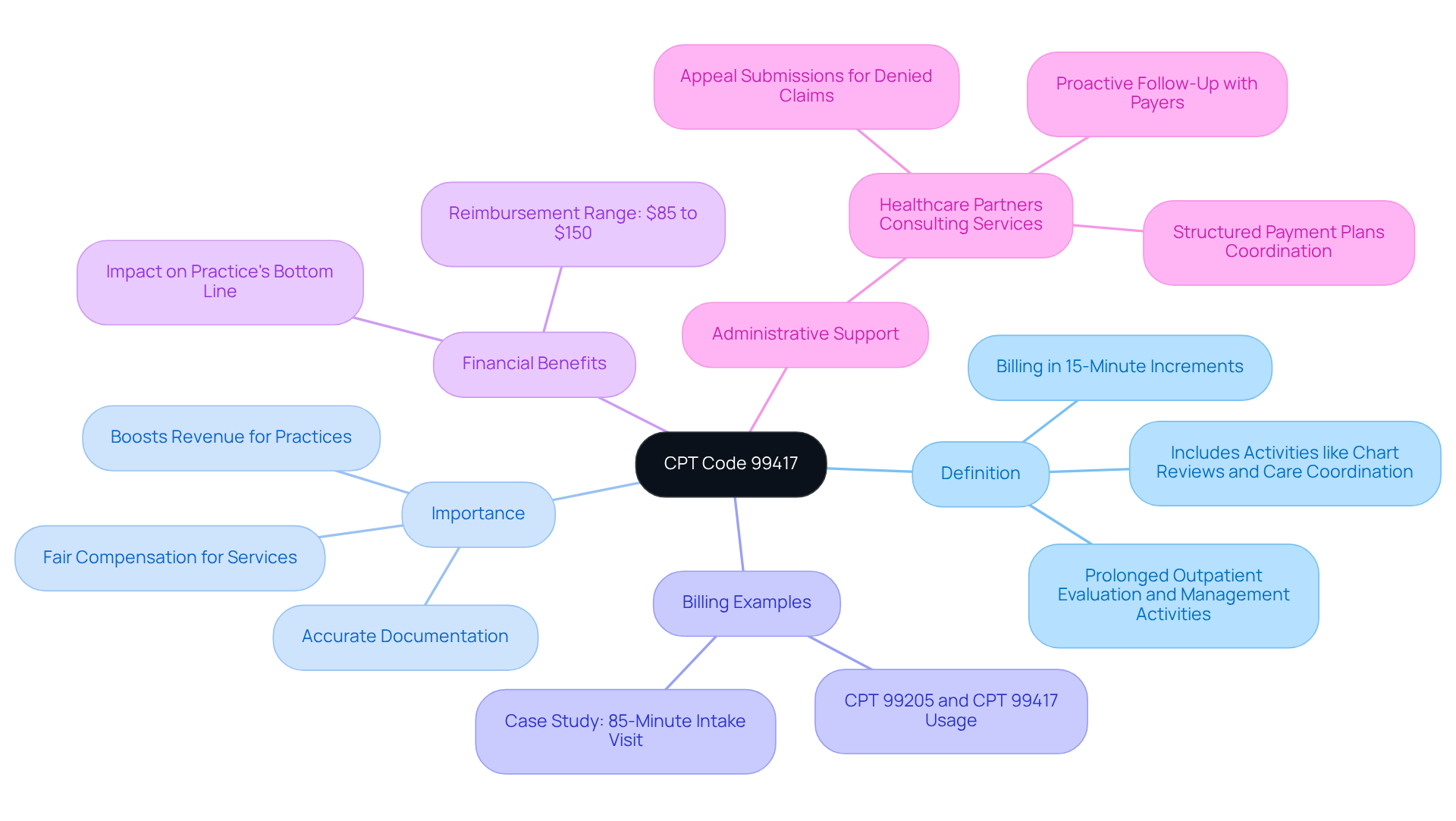
CPT Code 99417 is essential for accurately documenting prolonged outpatient evaluation and management activities, especially within mental health practices. This code applies when a provider exceeds the standard duration required for a primary E/M procedure, allowing billing in 15-minute increments for additional time spent, regardless of direct patient contact. Activities such as chart reviews and care coordination are included in this duration calculation.
For mental health providers, mastering CPT 99417 is crucial because it allows them to accurately capture the complete scope of their service delivery. This ensures fair compensation for the additional time spent on patient care and boosts revenue, particularly in practices with frequent extended interactions.
For instance, a recent case highlighted a provider who successfully billed for a comprehensive intake visit lasting 85 minutes using CPT 99205 and CPT 99417, demonstrating how effective billing can directly affect your practice’s bottom line. A properly billed unit of 99417 generates between $85 and $150 in reimbursement per visit, showcasing the financial benefits of proper code utilization.
By effectively implementing CPT 99417, mental health practices can enhance their invoicing processes and subsequently improve overall financial performance. Furthermore, with the comprehensive accounts receivable management solutions offered by Healthcare Partners Consulting, including proactive follow-up with payers, appeal submissions for denied claims, and structured payment plans coordination, mental health clinics can enhance their revenue cycle efficiency, reduce denials, and streamline compliance.
This is crucial in tackling the mental health billing crisis that experts like Davia Ward have pointed out. Practices that master coding 99417, supported by robust administrative services, will enjoy a significant competitive advantage in revenue cycle performance.
Document Time Accurately: Essential Guidelines for Compliance
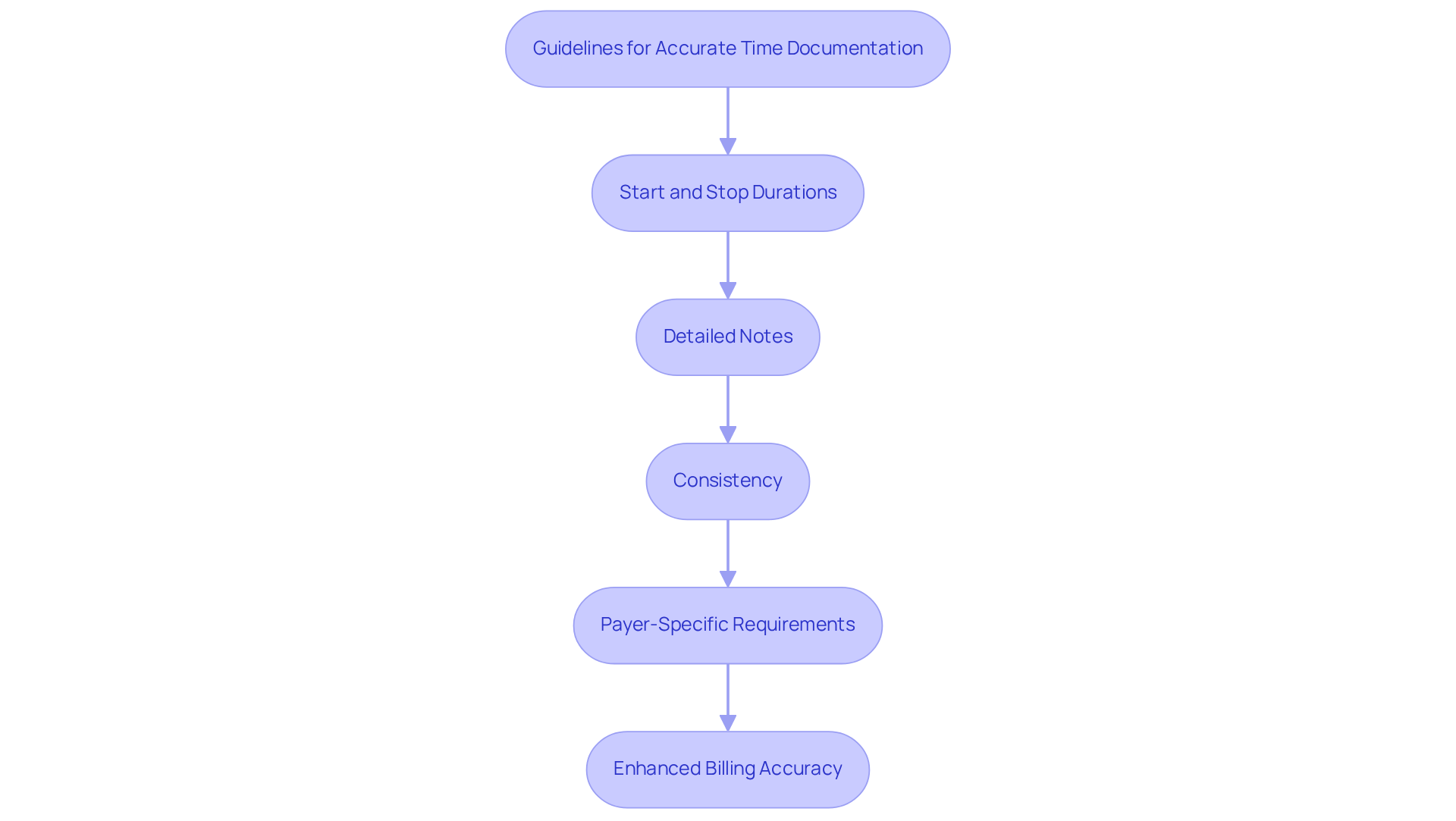
Accurate documentation of time spent during patient encounters is crucial for mental health providers using CPT Code 99417. This includes precise documentation of both direct patient interactions and any additional efforts related to associated activities. Here are essential guidelines for compliance:
- Start and Stop Durations: Record the precise start and stop moments for each session. This practice establishes a clear record of total duration spent, supporting the justification for billing 99417 CPT.
- Detailed Notes: Include thorough notes that describe the nature of assistance offered during the extended period. Activities such as care coordination, chart reviews, and other relevant tasks should be clearly specified to enhance the documentation.
- Consistency: Ensure that the documented time matches the billed services. Any discrepancies can lead to claim denials or audits, jeopardizing revenue.
- Payer-Specific Requirements: Acquaint yourself with the distinct documentation needs of each payer, as they may enforce particular rules concerning time-based invoicing.
Adhering to these guidelines ensures providers can significantly enhance billing accuracy and mitigate the risk of denials, ultimately leading to improved financial outcomes. Statistics indicate that documentation errors are a leading cause of claim denials, underscoring the necessity for meticulous record-keeping in mental health practices.
Avoid Common Billing Mistakes: Strategies for Success
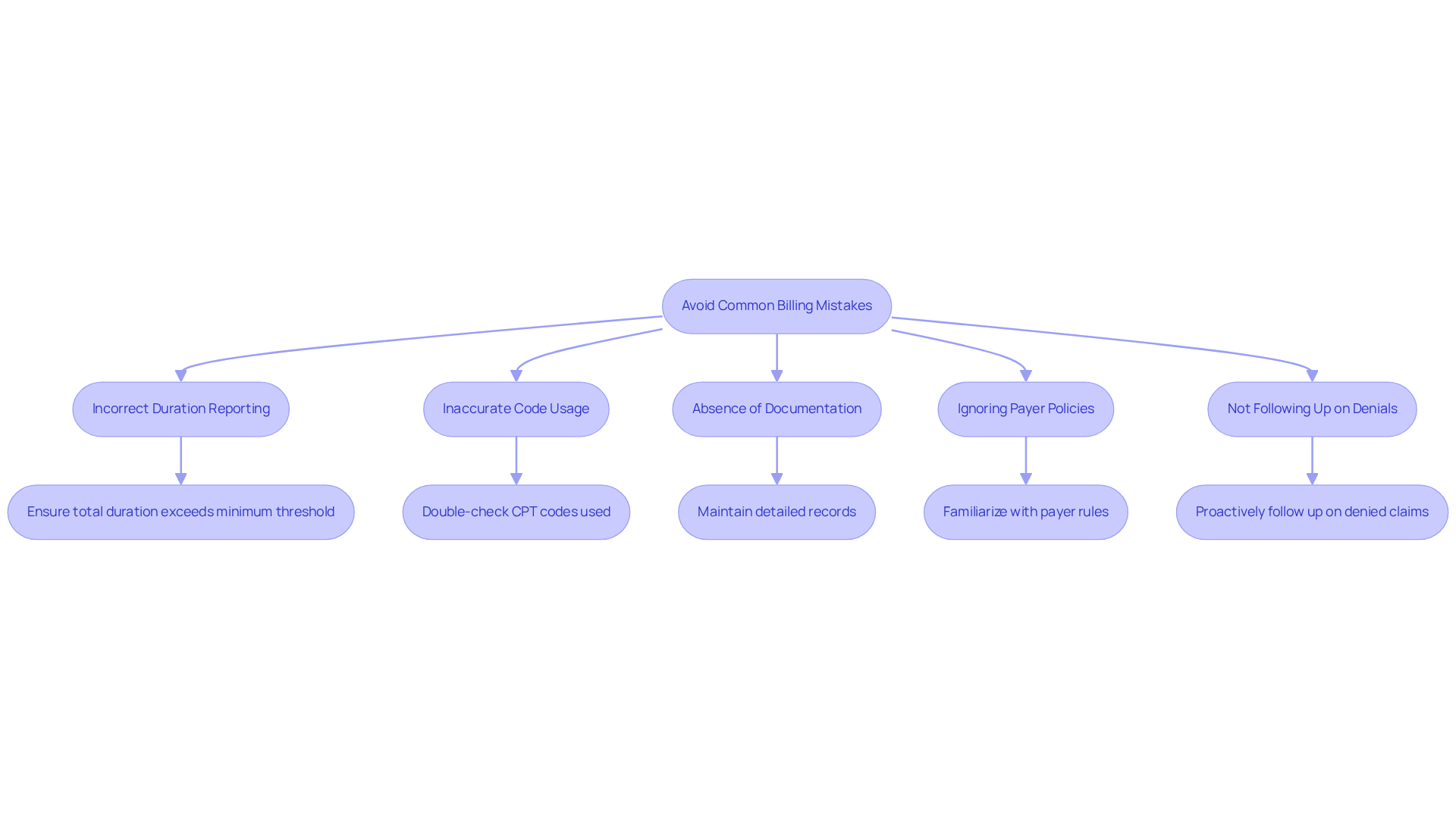
Billing for mental health care presents numerous challenges, especially with CPT Code 99417, which can complicate the reimbursement processes. Here are some common mistakes to avoid, along with strategies for success:
- Incorrect Duration Reporting: One of the most common mistakes is failing to meet the minimum duration threshold required for billing CPT code 99417. Ensure that the total duration spent surpasses the necessary duration for the primary E/M assistance plus an additional 15 minutes. According to industry data, improper time reporting can result in a significant percentage of denial of requests, emphasizing the importance of precise time tracking.
- Inaccurate Code Usage: Double-check that you are using the correct CPT codes for the services rendered. Misuse of codes can lead to claim denials and delayed payments. As mentioned by healthcare coding specialist Terry A. Fletcher, “the suitable moment should be recorded in the medical record when it is used as the basis for code selection.”
- Absence of Documentation: Without proper documentation, compliance issues can arise, jeopardizing reimbursement. Always keep detailed records that validate the billed work. Inadequate documentation is a frequent cause for rejections, and practices should ensure that they provide thorough notes on the work performed.
- Ignoring Payer Policies: Each insurance payer may have different rules regarding billing for prolonged services. Familiarize yourself with these policies to avoid denials. For example, some payers may need specific modifiers or documentation to process requests accurately.
- Not Following Up on Denials: If a request is denied, promptly follow up to understand the reason and rectify any issues. This proactive approach can help recover lost revenue. Many successful mental health clinics have implemented structured follow-up procedures, significantly improving payment efficiency and reducing denial rates. Additionally, partnering with Healthcare Partners Consulting can enhance your accounts receivable management, ensuring faster payments and reduced staffing burdens through dedicated AR specialists and ongoing updates on your claims.
By implementing these strategies, mental health providers can not only reduce errors but also enhance their financial sustainability.
Leverage Technology and Training: Enhance Billing Efficiency
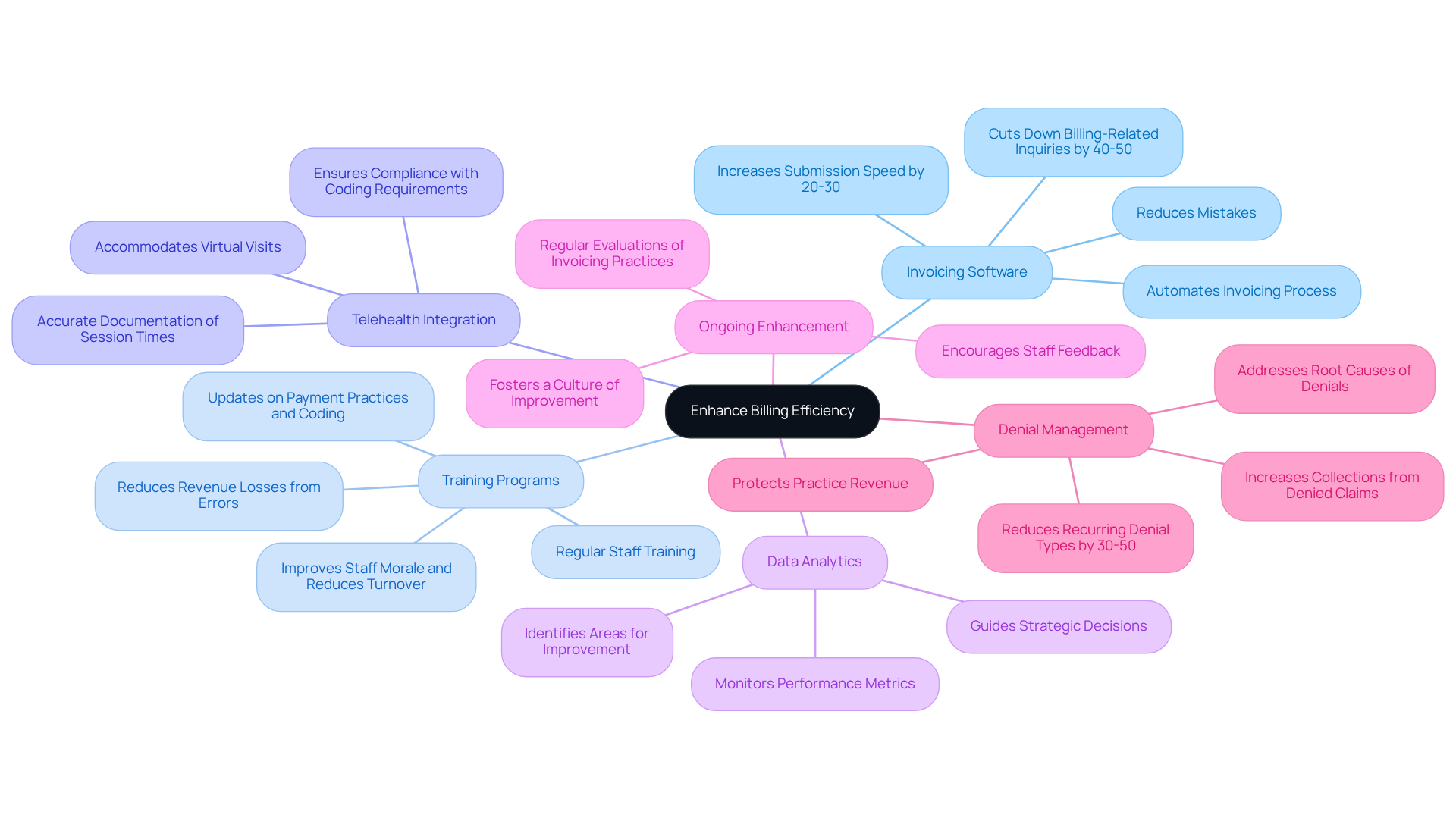
To enhance invoicing efficiency and accuracy, mental health practices must leverage technology and invest in staff training. Here are key strategies:
- Invoicing Software: Implement specialized invoicing software tailored for mental health practices. These tools automate various aspects of the invoicing process, significantly reducing mistakes and increasing submission speed. Adopting this technology can improve claims processing speed by 20-30% and cut down billing-related patient inquiries by 40-50%.
- Training Programs: Regularly train staff on the latest payment practices, coding updates, and compliance requirements. Investing in training is crucial; without it, practices risk significant revenue losses due to invoicing errors. Practices prioritizing ongoing training may also experience lower turnover rates and improved staff morale, as employees feel valued and supported.
- Telehealth Integration: With the rise of telehealth, ensure that your invoicing system accommodates virtual visits and adheres to the associated coding requirements. Accurate documentation of telehealth sessions, including exact start and stop times, is vital for compliance and reimbursement.
- Data Analytics: Utilize data analytics to monitor performance metrics, such as claim denial rates and reimbursement timelines. This data can pinpoint areas needing improvement and guide strategic decisions, ultimately enhancing financial performance.
- Ongoing Enhancement: Foster a culture of ongoing enhancement by motivating personnel to share insights and suggestions for refining invoicing processes. Frequent evaluations of invoicing practices based on feedback and performance data can lead to substantial operational improvements.
- Denial Management: Implement robust denial management strategies to protect practice revenue. Every denied request represents a lost opportunity, often recoverable through effective management. By examining trends and addressing root causes, practices can lessen administrative burdens and improve invoicing accuracy. This proactive approach can lead to a 30-50% reduction in recurring denial types and increased collections from previously denied claims.
By adopting these strategies, practices can not only streamline operations but also secure their financial viability in a competitive landscape.
Conclusion
Mastering CPT Code 99417 is essential for mental health providers aiming to enhance their billing practices and financial outcomes. Accurate documentation of prolonged evaluation and management activities ensures fair compensation for the comprehensive care provided by practitioners. This code helps with billing for extended patient interactions and plays a crucial role in the revenue of mental health practices.
The article highlights essential strategies for the successful implementation of CPT 99417, including:
- Meticulous time documentation
- Adherence to payer-specific requirements
- Avoidance of common billing mistakes
It emphasizes the importance of leveraging technology and ongoing training to streamline invoicing processes and reduce the likelihood of claim denials. Adopting these best practices enhances billing accuracy and strengthens financial sustainability for mental health providers.
In a landscape where mental health billing challenges are prevalent, the effective use of CPT Code 99417 can provide a competitive edge. By prioritizing accurate documentation, utilizing advanced billing technologies, and fostering a culture of continuous improvement within their practices, mental health providers can navigate the complexities of billing with confidence. Ultimately, the strategic implementation of CPT Code 99417 not only improves financial outcomes but also elevates the standard of care provided to patients.
Frequently Asked Questions
What is CPT Code 99417?
CPT Code 99417 is used for documenting prolonged outpatient evaluation and management activities, allowing providers to bill for additional time spent beyond the standard duration required for a primary evaluation and management (E/M) procedure.
How is CPT Code 99417 billed?
CPT 99417 is billed in 15-minute increments for additional time spent on activities related to patient care, which can include chart reviews and care coordination, regardless of direct patient contact.
Why is CPT Code 99417 important for mental health providers?
Mastering CPT 99417 is crucial for mental health providers as it helps them accurately capture the full scope of their services, ensuring fair compensation for the extra time spent on patient care and potentially increasing revenue.
Can you provide an example of how CPT 99417 is used?
An example includes a provider who billed for a comprehensive intake visit lasting 85 minutes using CPT 99205 and CPT 99417, illustrating how effective billing can positively impact a practice’s financial performance.
What is the potential reimbursement for a properly billed unit of CPT 99417?
A properly billed unit of CPT 99417 can generate between $85 and $150 in reimbursement per visit.
How can mental health practices improve their financial performance using CPT 99417?
By effectively implementing CPT 99417, mental health practices can enhance their invoicing processes, improve revenue cycle efficiency, reduce denials, and streamline compliance, leading to better overall financial performance.
What services does Healthcare Partners Consulting offer to support mental health practices?
Healthcare Partners Consulting provides comprehensive accounts receivable management solutions, including proactive follow-up with payers, appeal submissions for denied claims, and coordination of structured payment plans to enhance revenue cycle efficiency.
What is the significance of mastering CPT 99417 in relation to the mental health billing crisis?
Mastering CPT 99417, along with strong administrative support, gives practices a competitive advantage in revenue cycle performance, which is crucial in addressing the mental health billing crisis highlighted by experts.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting