Mastering Medical Coding
Master E11.42 Coding: Best Practices for Mental Health Clinics

Introduction
Understanding the complexities of E11.42 coding is essential for mental health clinics managing diabetes care. This specific code, which relates to Type 2 diabetes with diabetic polyneuropathy, significantly influences treatment strategies and affects the financial sustainability of healthcare practices. As clinics aim to deliver comprehensive care, the challenge is to master effective documentation and billing practices that ensure accurate reimbursements and improve patient outcomes.
How can mental health providers adapt their coding strategies to align with evolving guidelines while maximizing both care quality and revenue?
Define E11.42: Understanding Its Role in Diabetes Management
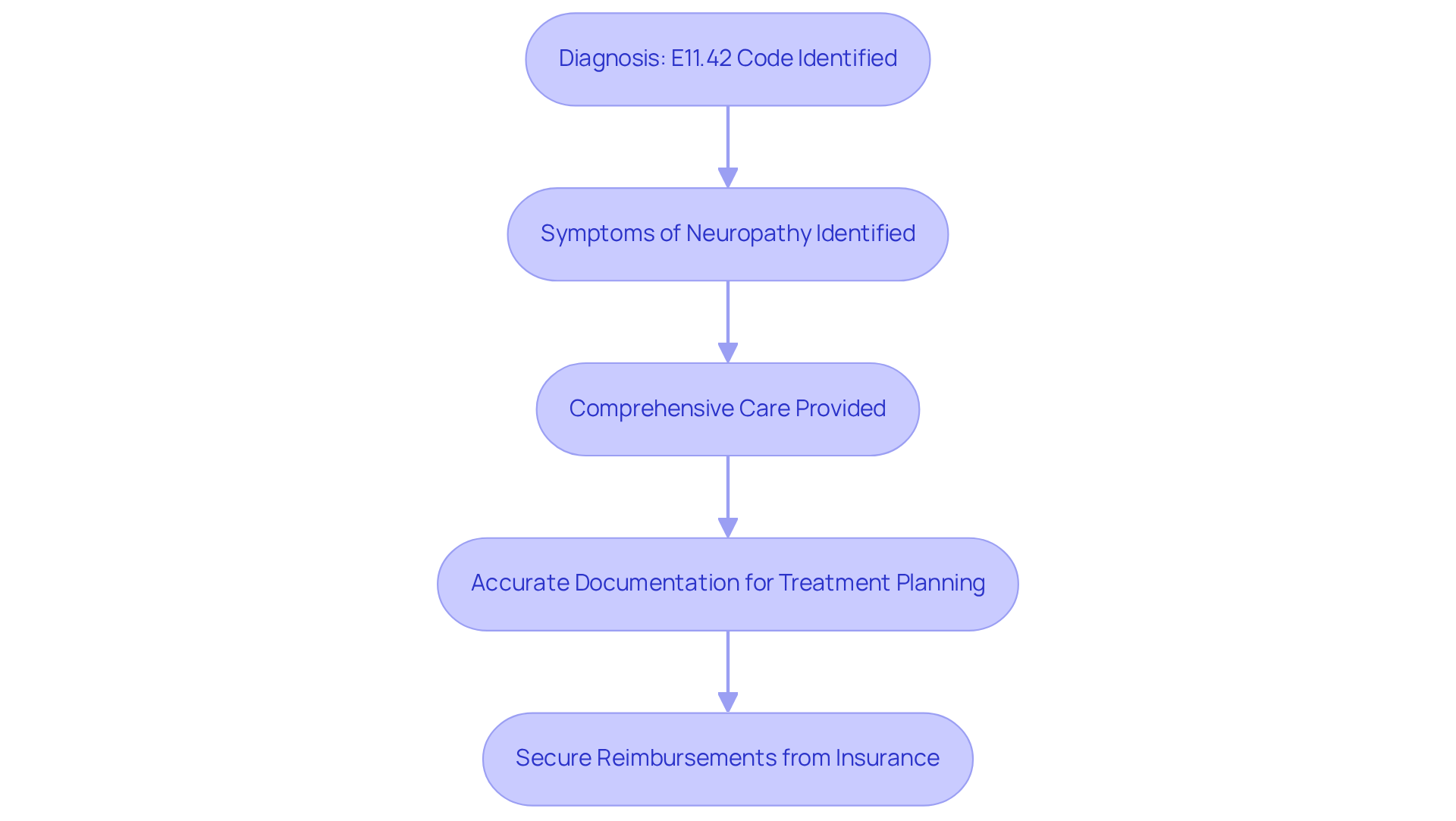
The E11.42 code identifies Type 2 diabetes mellitus with diabetic polyneuropathy, a condition marked by nerve damage resulting from prolonged high blood sugar levels. This diagnosis is essential for healthcare providers, as it significantly affects both the physical and mental health of individuals. A proper understanding and application of this code are crucial for accurate documentation, treatment planning, and billing processes.
For instance, when individuals present symptoms of neuropathy, such as numbness, tingling, or pain, correctly identifying E11.42 ensures they receive comprehensive care. This includes effective pain management and necessary psychological support, both of which are vital for their overall well-being. Furthermore, accurate coding is instrumental in securing reimbursements from insurance providers, thereby enhancing the financial health of the practice.
In 2026, the implications of E11.42 extend beyond mere compliance; they play a pivotal role in improving treatment outcomes and ensuring that individuals receive the comprehensive care they require. Effective documentation serves as the foundation for precise programming of E11.42, as emphasized by specialists in the field. This may also necessitate advanced treatments, such as insulin therapy, for individuals whose blood sugar levels are not adequately managed with oral medications alone.
Additionally, Healthcare Partners Consulting highlights that incorrect or incomplete coding can result in claim denials, delayed payments, and increased administrative burdens. Their comprehensive accounts receivable management solutions, which include proactive follow-up with payers on unpaid claims and the assignment of dedicated AR specialists, are designed to enhance revenue cycle efficiency and mitigate these risks.
Implement Best Documentation Practices for E11.42 Coding
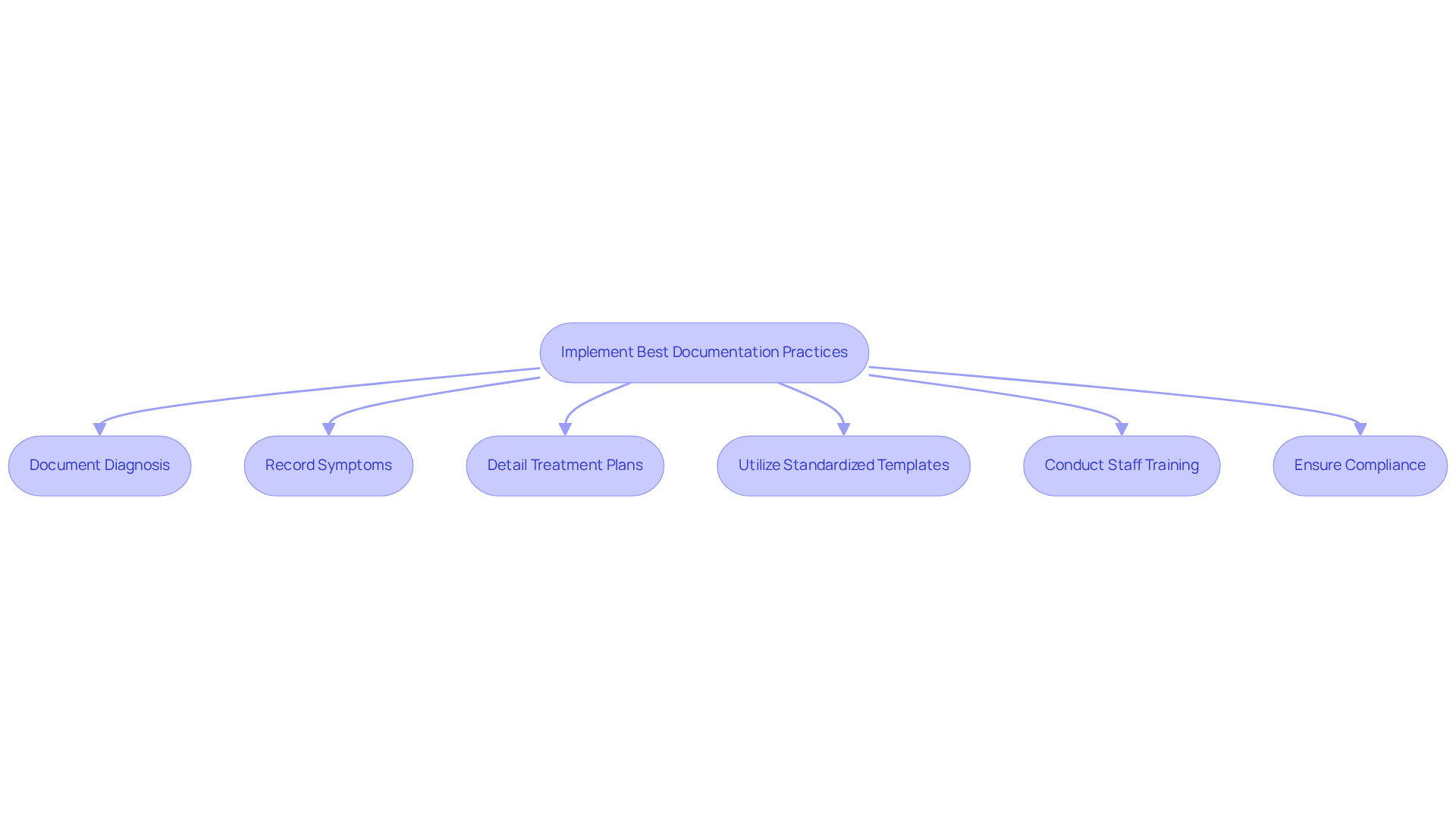
To effectively utilize the code e11.42, mental wellness clinics must implement stringent documentation practices that clearly connect the diagnosis of Type 2 diabetes with diabetic polyneuropathy to the individual’s clinical presentation. Providers should meticulously document all relevant symptoms, treatment plans, and responses from individuals. Clinical notes must specify any nerve-related symptoms experienced by the individual, such as pain or numbness, and articulate how these symptoms influence their mental well-being.
Utilizing standardized templates can facilitate the consistent capture of necessary information, thereby enhancing clarity and compliance. Furthermore, regular training sessions for staff on documentation standards are vital for improving accuracy and adherence to established practices. This proactive approach not only leads to better client outcomes but also significantly reduces the risk of claim denials. Accurate documentation is crucial in justifying billed services and ensuring timely reimbursements.
Maximize Revenue: Strategies for Effective E11.42 Billing
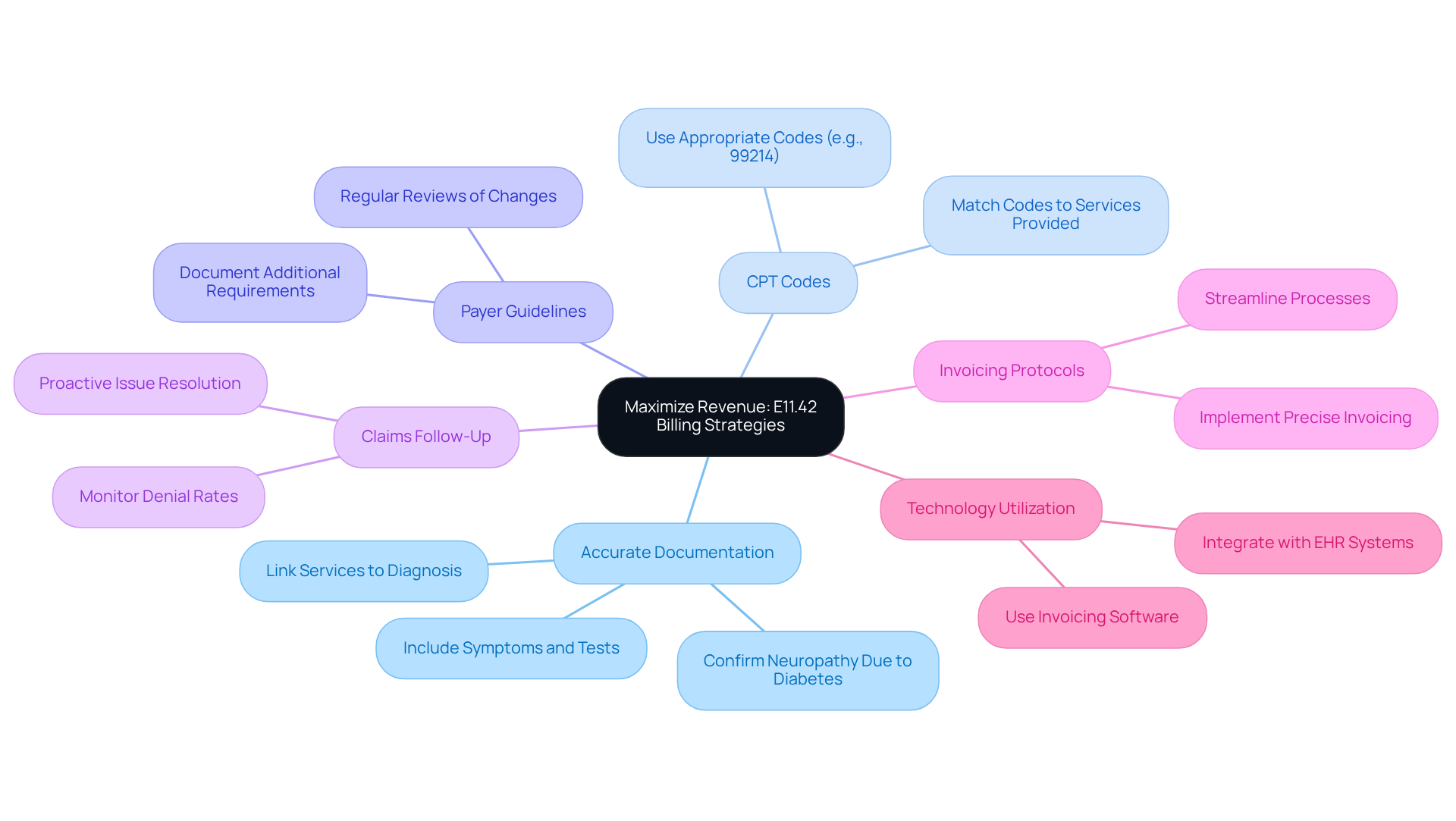
To maximize revenue associated with e11.42, mental health clinics should adopt several essential strategies. First and foremost, accurate documentation is paramount; all services rendered must be explicitly linked to the diagnosis E11.42. This includes psychotherapy sessions, medication management, and any treatments related to the individual’s diabetic condition. Employing suitable CPT codes, such as 99214 for established patient visits, enhances accuracy and compliance in financial transactions.
Regular reviews of payer guidelines are crucial to remain informed about changes that may impact reimbursement rates, as payer requirements can evolve. Additionally, proactive follow-up on claims is essential; addressing issues promptly can significantly enhance cash flow and reduce the risk of denials, which can occur at rates ranging from 15 to 25 percent nationally in behavioral services. Moreover, practices that implement precise invoicing protocols often report a 30-50% decrease in denial rates.
Utilizing technology, such as invoicing software that integrates seamlessly with electronic health records, can streamline the invoicing process, reduce administrative burdens, and enhance overall efficiency. Healthcare Partners Consulting offers comprehensive administrative support services, including benefits verification, claims submission, and customized reporting, to further assist clinics in optimizing their revenue cycle. Furthermore, HPC’s performance-aligned medical pricing structure, starting at a minimum of $500 for gross income up to $6,500, provides a cost-effective solution for clinics.
By implementing these practices and utilizing HPC’s services, clinics can not only improve their revenue cycle but also ensure compliance and enhance patient care. Insights from industry specialists, such as Davia Ward, underscore the ongoing mental wellness invoicing crisis, highlighting the significance of these strategies in managing the complexities of invoicing and reimbursement.
Stay Informed: Adapting to E11.42 Coding Updates and Payer Guidelines
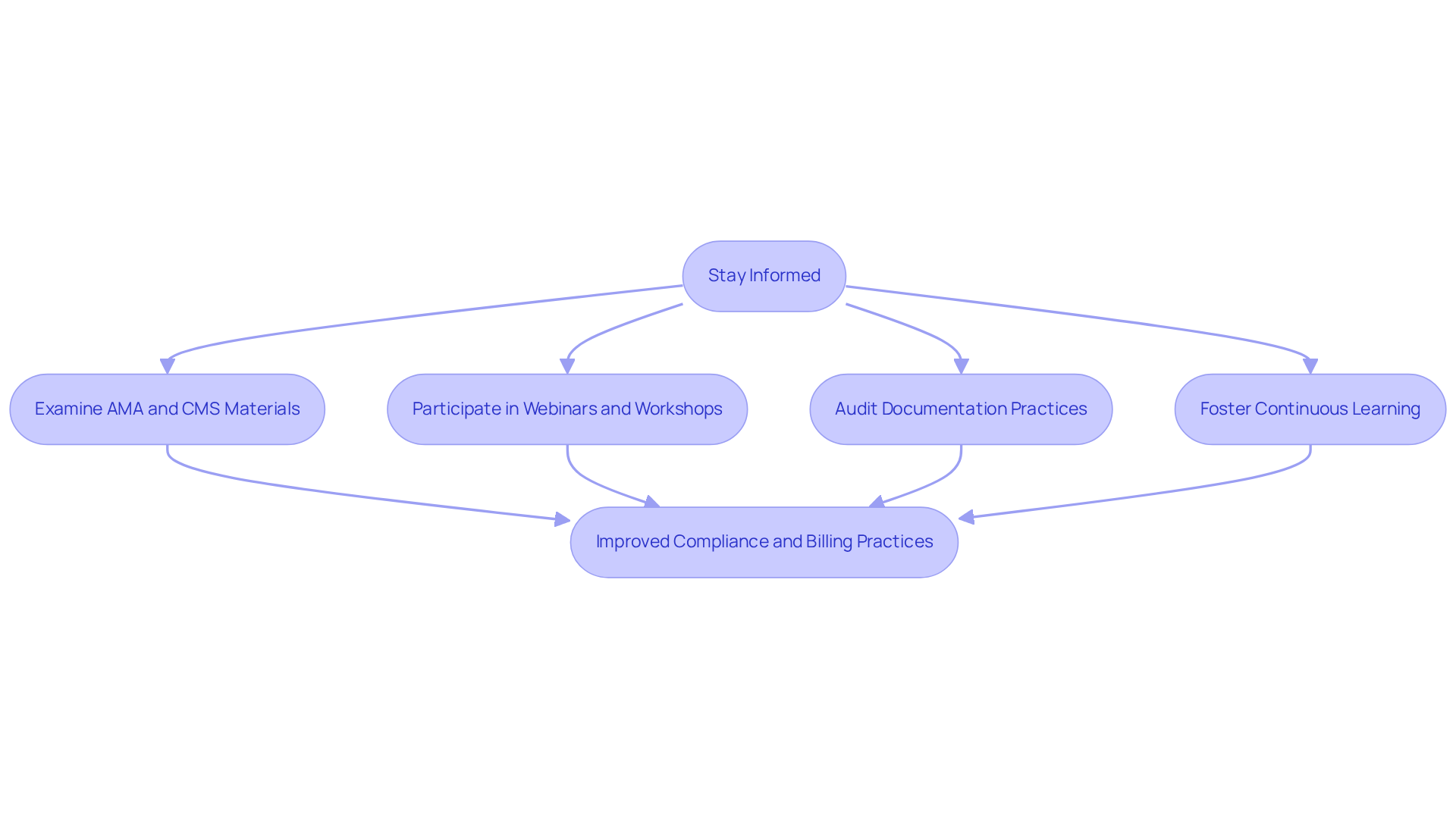
Mental health clinics must prioritize staying informed about updates to the e11.42 classification and payer guidelines. This is essential for ensuring compliance and optimizing billing practices. Regularly examining materials from organizations such as the American Medical Association (AMA) and the Centers for Medicare & Medicaid Services (CMS) provides critical insights into changes in billing requirements. Additionally, participation in programming webinars and workshops enhances staff knowledge and skills, which is particularly important given that approximately 32% of first-submission denials arise from programming issues.
Clinics should also establish a routine for auditing their documentation practices. This will help identify areas for improvement and ensure that all relevant diagnoses and treatments are accurately captured. By fostering a culture of continuous learning and adaptation, clinics can navigate the complexities of coding and billing more effectively. This proactive approach is vital, especially with the upcoming 2026 updates that will introduce new codes and specificity requirements, potentially impacting revenue capture significantly. Ultimately, these efforts lead to improved financial health and enhanced patient care.
Conclusion
Mastering E11.42 coding is not just a technical requirement; it is essential for delivering comprehensive care to individuals with Type 2 diabetes and diabetic polyneuropathy. The proper application of this coding enables mental health clinics to effectively document and manage the complexities of their patients’ conditions, ultimately leading to improved health outcomes and financial stability for the practice.
This article outlined key strategies that underscore the importance of:
- Accurate documentation
- Adherence to payer guidelines
- Ongoing education
By meticulously linking symptoms to the E11.42 code, clinics can enhance their billing processes, reduce claim denials, and improve overall patient care. Implementing robust documentation practices and leveraging technology can significantly streamline operations and optimize revenue cycles.
The importance of staying informed about coding updates and payer requirements cannot be overstated. As mental health clinics navigate the evolving landscape of healthcare billing, adopting a proactive approach is essential for maintaining compliance and maximizing reimbursement. Embracing these best practices not only strengthens the financial health of clinics but also ensures that patients receive the holistic support they require for their mental and physical well-being.
Frequently Asked Questions
What does the E11.42 code represent?
The E11.42 code identifies Type 2 diabetes mellitus with diabetic polyneuropathy, which is a condition characterized by nerve damage due to prolonged high blood sugar levels.
Why is the E11.42 code important for healthcare providers?
It is crucial for accurate documentation, treatment planning, and billing processes, significantly affecting both the physical and mental health of individuals with this condition.
What symptoms might lead to the identification of the E11.42 code?
Symptoms such as numbness, tingling, or pain can indicate neuropathy, prompting the need for the E11.42 diagnosis to ensure comprehensive care.
How does accurate coding impact patient care?
Accurate coding allows for effective pain management and necessary psychological support, which are vital for the overall well-being of individuals with diabetic polyneuropathy.
What are the financial implications of correctly using the E11.42 code?
Proper coding is instrumental in securing reimbursements from insurance providers, enhancing the financial health of healthcare practices.
What role does documentation play in the application of E11.42?
Effective documentation is essential for precise programming of E11.42 and may require advanced treatments, such as insulin therapy, for better blood sugar management.
What risks are associated with incorrect coding of E11.42?
Incorrect or incomplete coding can lead to claim denials, delayed payments, and increased administrative burdens for healthcare providers.
How can healthcare practices mitigate risks related to coding errors?
Healthcare Partners Consulting offers comprehensive accounts receivable management solutions, including proactive follow-up on unpaid claims and the assignment of dedicated AR specialists to enhance revenue cycle efficiency.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting