Mastering Medical Coding
Master the E78.2 ICD-10 Code for Better Mental Health Billing

Introduction
In the evolving healthcare landscape, the interplay between physical and mental health significantly impacts billing practices. The E78.2 ICD-10 code, which denotes ‘Mixed Hyperlipidemia,’ serves as a pivotal point for healthcare providers seeking to enhance their billing accuracy and ensure optimal patient care. Mastering the E78.2 code presents significant challenges that can lead to claim denials. By effectively leveraging the E78.2 code, practices can not only streamline billing but also enhance patient outcomes.
Understand the E78.2 ICD-10 Code: Definition and Relevance
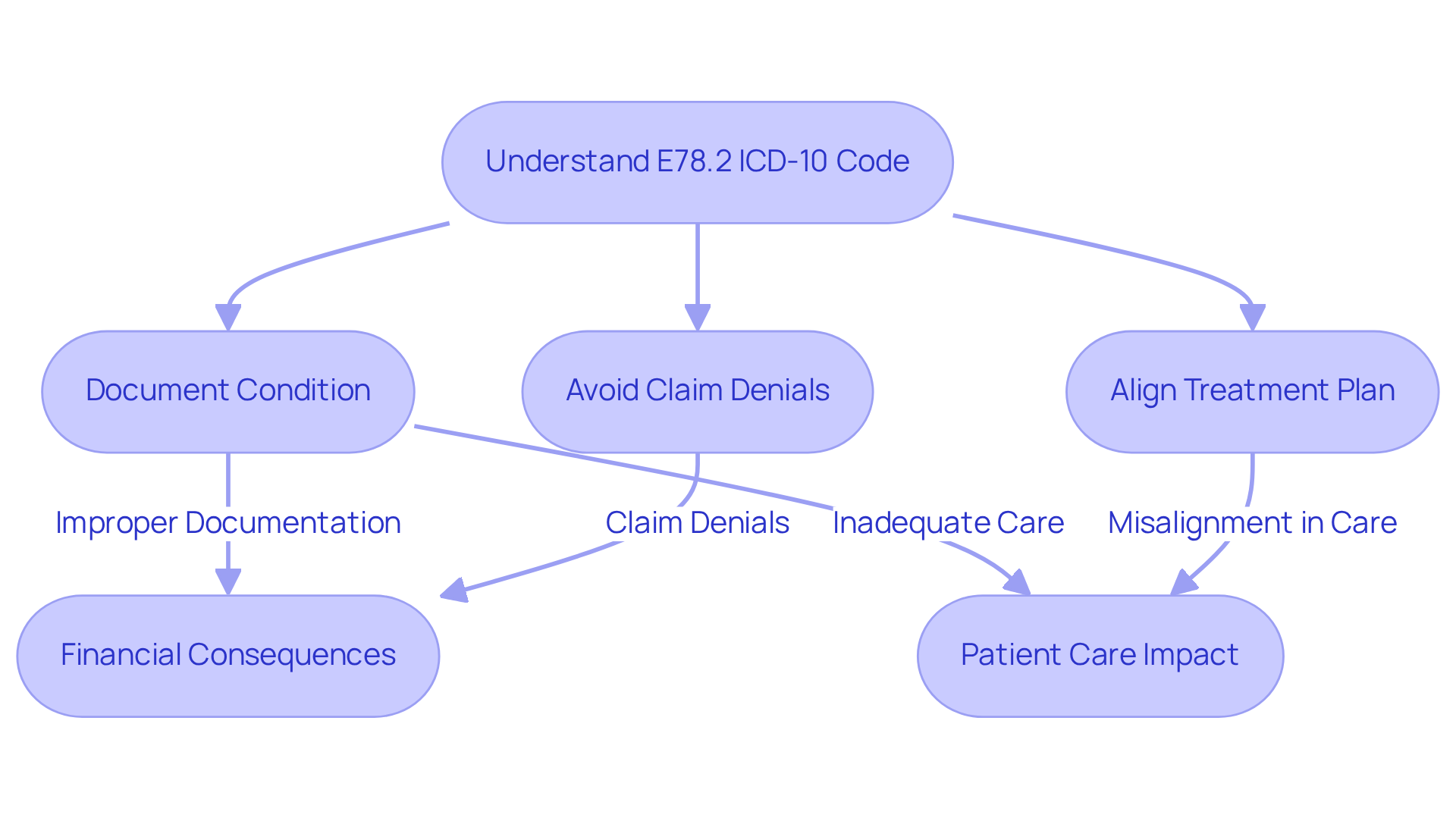
The e78.2 icd 10 code classification indicates ‘Mixed Hyperlipidemia,’ which is a critical diagnosis for managing cholesterol and triglyceride levels in patients. Understanding this diagnosis is vital for healthcare providers, given its classification under endocrine, nutritional, and metabolic diseases.
Individuals with metabolic disorders often display concurrent psychological conditions, making precise coding essential. Without precise coding, healthcare providers face the risk of claim denials, complicating patient care and financial stability.
For instance, when a patient is identified with mixed hyperlipidemia, careful documentation of this condition is crucial to avoid claim denials and to ensure that the treatment plan aligns with the patient’s overall well-being needs.
The financial consequences of invoicing inaccuracies associated with this identifier can be considerable, with ongoing errors costing behavioral wellness establishments between $25,000 and $45,000 each year. These inaccuracies not only jeopardize patient care but also threaten the financial health of practices.
Thus, effective utilization of the e78.2 icd 10 code designation is essential for enhancing patient outcomes and ensuring the financial sustainability of mental wellness practices.
Apply E78.2 in Mental Health Billing: Best Practices for Accuracy
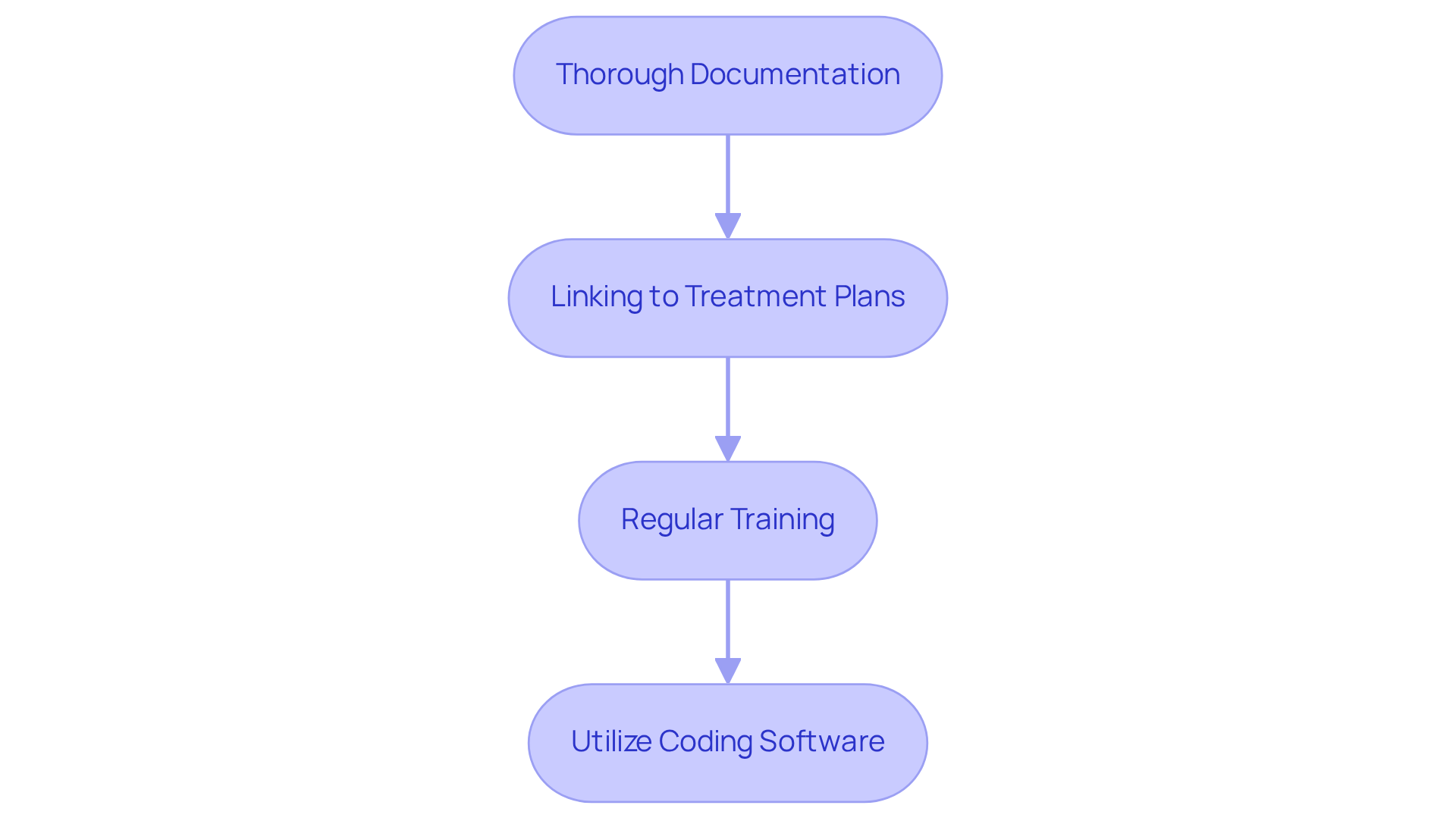
To optimize the application of the E78.2 code in mental health billing, it is essential to adopt a structured approach that emphasizes accuracy and compliance:
- Thorough Documentation: Ensure that all clinical evidence supporting the diagnosis of mixed hyperlipidemia is meticulously documented in the patient’s medical record. This includes lipid panel results and pertinent medical history, as accurate documentation is essential for justifying claims and ensuring compliance with payer requirements. At Healthcare Partners Consulting, our certified medical charge specialists meticulously review and correct coding issues prior to claim submission. This proactive approach significantly reduces errors from the outset.
- Linking to Treatment Plans: Clearly connect the treatment plan to the e78.2 icd 10 code. For instance, if a patient is prescribed medication to manage their lipid levels, document this connection explicitly to substantiate the use of the code. This linkage is crucial for demonstrating the medical necessity of the treatment, which is a key factor in our tailored coding support.
- Regular Training: Conduct ongoing training sessions for invoicing personnel to keep them updated about coding modifications and optimal methods. Regular training minimizes errors and enhances compliance, as many healthcare providers face substantial financial losses due to billing inaccuracies, with studies indicating that a staggering 80% of medical claims are prone to errors. By investing in ongoing training, practices can significantly reduce the risk of claim denials and enhance their overall financial health.
- Utilize Coding Software: Implement coding software that assists in identifying the correct codes based on the documentation provided. This technology can significantly reduce the likelihood of human error and streamline the invoicing process, ultimately improving the accuracy of claims submissions. Furthermore, performing regular audits of documentation and invoicing processes can aid in recognizing patterns of errors early, further improving accuracy. Our quality assurance processes and peer reviews are built into our workflow to support this effort.
Implementing these best practices enables mental health practices to improve billing accuracy, minimize claim denials, and streamline revenue cycle management, thereby maximizing both revenue and operational efficiency.
Avoid Common Pitfalls: Challenges in Using E78.2 and How to Overcome Them
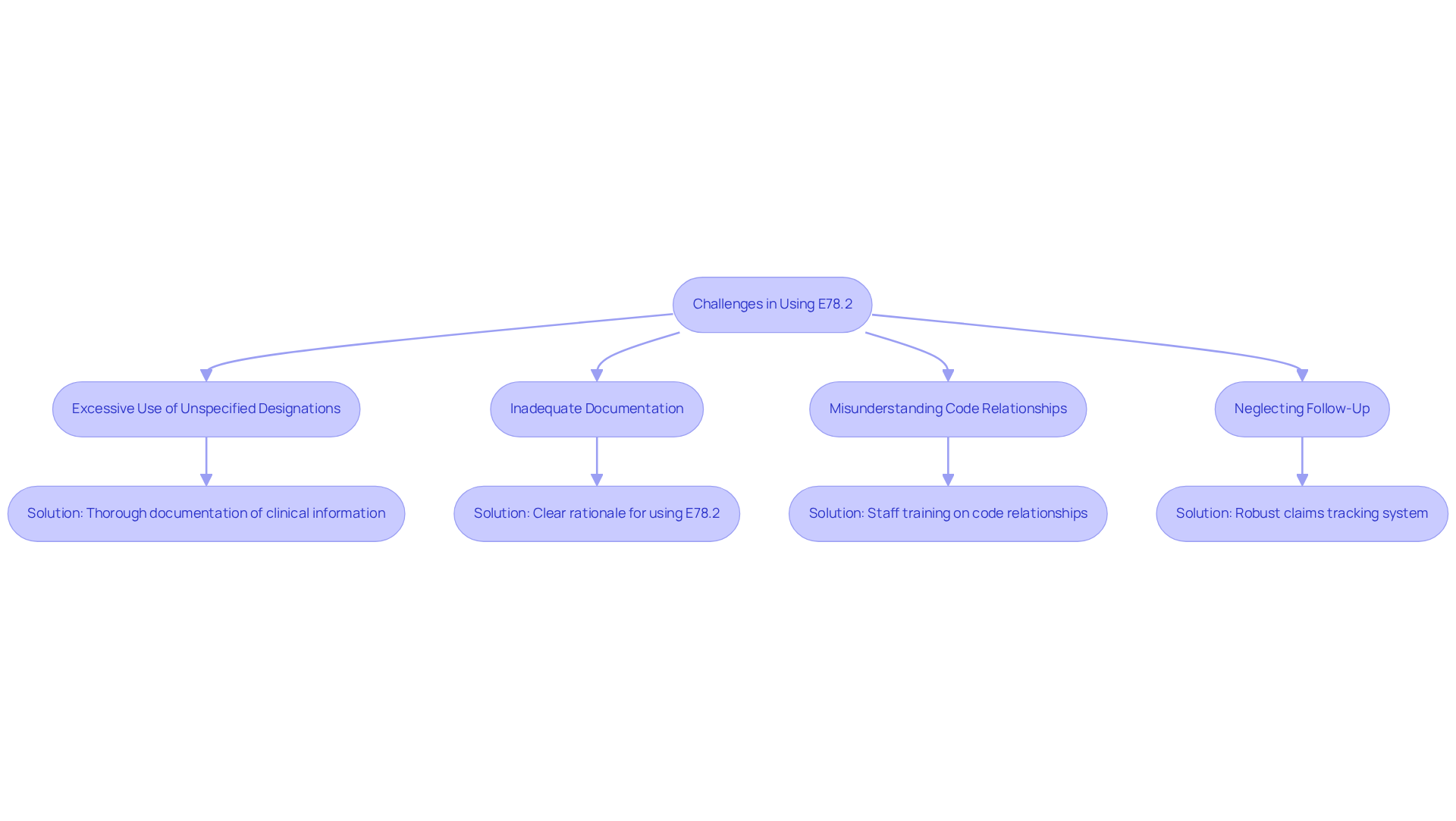
Providers often encounter significant challenges when using the E78.2 designation, leading to potential claim denials.
- Excessive Use of Unspecified Designations: Inadequate documentation often leads providers to use unspecified designations like E78.5, significantly increasing the risk of claim denials. To mitigate this, thorough documentation of all relevant clinical information is essential.
- Inadequate documentation: A clear rationale for using the E78.2 ICD 10 code is essential to avoid audits and denials. Detailed notes justifying the diagnosis are crucial for compliance and successful claims processing.
- Misunderstanding the relationship between codes can occur, as some providers may not understand that the E78.2 ICD 10 code cannot be used with certain other codes, which can lead to billing errors. Training staff on the relationships between codes is essential to prevent billing errors.
- Neglecting Follow-Up: Following claims submission, it is crucial to follow up on denials or requests for additional information. A robust claims tracking system ensures timely resolutions and prevents revenue loss.
Maximize Revenue and Efficiency: The Impact of E78.2 on Mental Health Practices
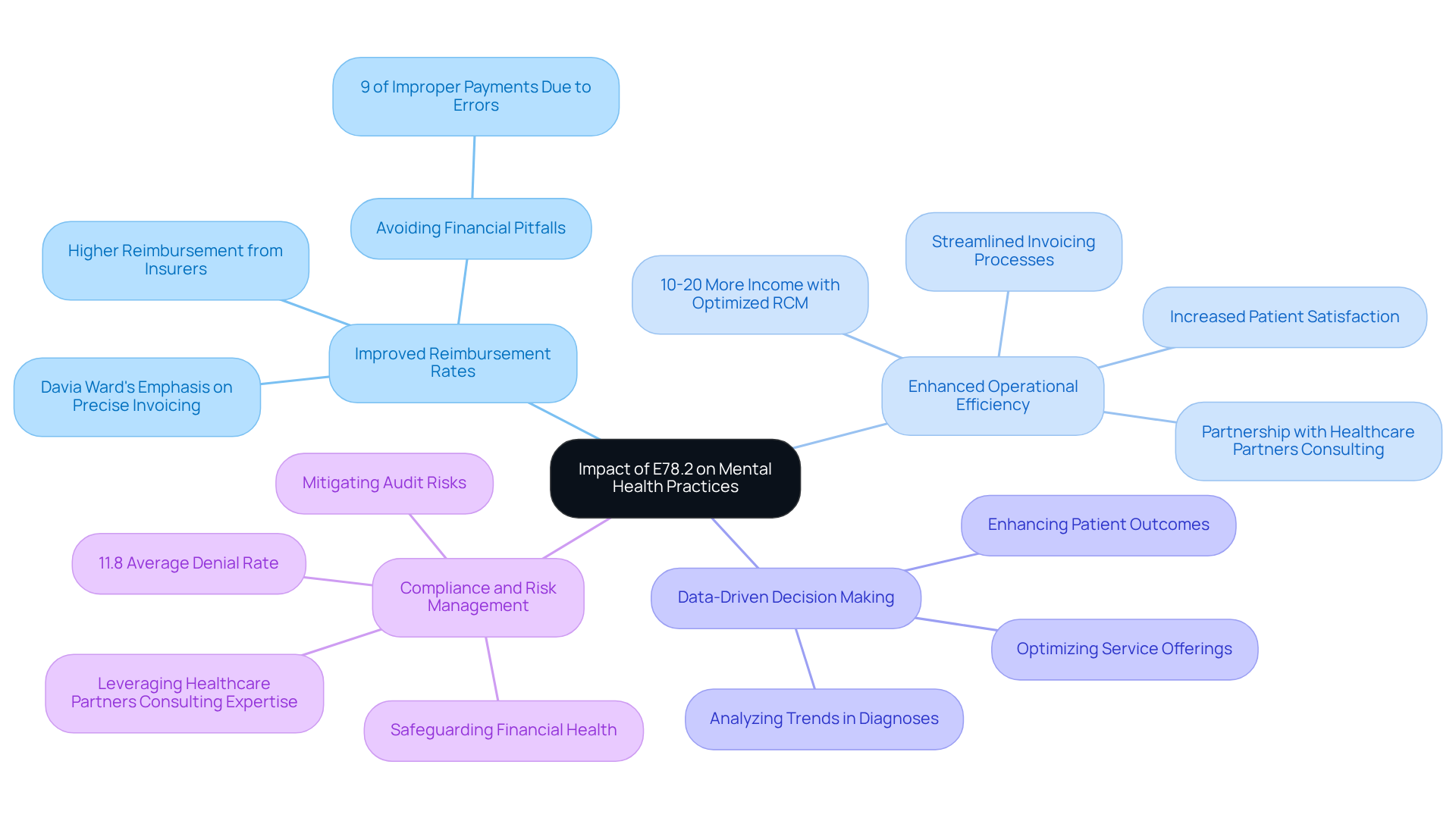
The effective utilization of the E78.2 code is pivotal in transforming mental health practices in several ways:
- Improved Reimbursement Rates: Accurate coding leads to higher reimbursement rates from insurance providers. By accurately using the e78.2 icd 10 code for mixed hyperlipidemia, facilities can ensure they are reimbursed for the full range of services provided to patients, thereby enhancing their financial well-being. This statistic underscores the critical need for accurate coding to avoid financial pitfalls, as the e78.2 icd 10 code is an important classification in medical coding. 9% of improper payments in 2020 were due to missing documentation or coding errors. As Davia Ward emphasizes, addressing the mental health payment crisis requires a focus on precise invoicing practices to ensure that providers receive the compensation they deserve.
- Enhanced Operational Efficiency: Streamlined invoicing processes reduce the administrative burden on staff, enabling them to focus on patient care. This change enhances patient satisfaction and promotes higher retention rates, as providers can devote more time to addressing patient needs instead of dealing with intricate financial issues. Behavioral health approaches typically gather 10 to 20 percent more income with optimized revenue cycle management compared to general medical billing, demonstrating the financial benefits of accurate coding. Partnering with Healthcare Partners Consulting can further enhance these efficiencies through comprehensive administrative support.
- Data-Driven Decision Making: Precise coding produces valuable information that guides management choices. By analyzing trends in diagnoses and treatments, practices can pinpoint areas for improvement, optimize service offerings, and ultimately enhance patient outcomes. This data-driven method is crucial for navigating the complexities of the mental health financial landscape.
The e78.2 icd 10 code is an important classification in medical coding. Compliance and Risk Management: Proper use of the e78.2 icd 10 code helps mitigate the risk of audits and penalties associated with incorrect billing. This proactive approach not only safeguards the organization financially but also enhances its reputation within the healthcare community, ensuring compliance with industry standards and regulations. The average denial rate for behavioral health facilities is approximately 11.8 percent, underscoring the importance of accurate coding to avoid unnecessary financial losses. By leveraging the expertise of Healthcare Partners Consulting, practices can ensure compliance and reduce the risk of billing-related issues.
Ultimately, organizations that embrace precise coding practices position themselves for sustainable growth and improved patient care.
Conclusion
Mastering the E78.2 ICD-10 code is not just beneficial; it is crucial for mental health billing and treatment planning. Correct application of this code enhances patient outcomes and protects financial health by reducing claim denials and billing inaccuracies.
Throughout this article, we have emphasized key practices such as:
- Thorough documentation
- Linking treatment plans to the E78.2 code
- Regular training for staff
- Utilizing coding software
These practices ensure compliance and enhance operational efficiency, enabling providers to prioritize patient care over administrative tasks.
Effectively using the E78.2 code leads to improved reimbursement rates, operational efficiency, and data-driven decisions that enhance care quality. Embracing precise coding practices is necessary for mental health practices aiming for sustainable growth and improved patient care. The future of mental health practices hinges on the commitment to precise coding, which ultimately shapes the quality of care delivered to patients.
Frequently Asked Questions
What does the E78.2 ICD-10 code represent?
The E78.2 ICD-10 code classification indicates ‘Mixed Hyperlipidemia,’ which is important for managing cholesterol and triglyceride levels in patients.
Why is understanding the E78.2 diagnosis important for healthcare providers?
Understanding this diagnosis is vital for healthcare providers as it falls under endocrine, nutritional, and metabolic diseases, and precise coding is necessary to avoid claim denials and ensure proper patient care.
What are the potential consequences of inaccurate coding related to the E78.2 code?
Inaccurate coding can lead to claim denials, complicating patient care and financial stability, with ongoing errors costing behavioral wellness establishments between $25,000 and $45,000 each year.
How does mixed hyperlipidemia relate to mental health?
Individuals with metabolic disorders, such as mixed hyperlipidemia, often display concurrent psychological conditions, making accurate documentation and coding essential for their overall treatment.
What is the financial impact of invoicing inaccuracies associated with the E78.2 code?
Invoicing inaccuracies can significantly impact the financial health of practices, jeopardizing patient care and leading to considerable financial losses.
How can effective utilization of the E78.2 code enhance patient outcomes?
Effective utilization of the E78.2 ICD-10 code is essential for aligning treatment plans with patients’ health needs, ultimately enhancing patient outcomes and ensuring the financial sustainability of mental wellness practices.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting