Mastering Medical Coding
Mastering Code for Skin Tag Removal: Best Practices for Clinics

Introduction
Coding errors in skin tag removal can significantly impact clinic revenue and operational efficiency. With a substantial portion of claim denials resulting from these errors, mastering the relevant CPT and ICD-10 codes is crucial for enhancing revenue cycle management and ensuring compliance.
Navigating the differences between billable and non-billable codes, along with documenting medical necessity, presents challenges for healthcare providers. Clinics must ask themselves how they can code accurately and justify procedures to reduce denials and increase reimbursements.
Understand Skin Tag Removal Coding Basics
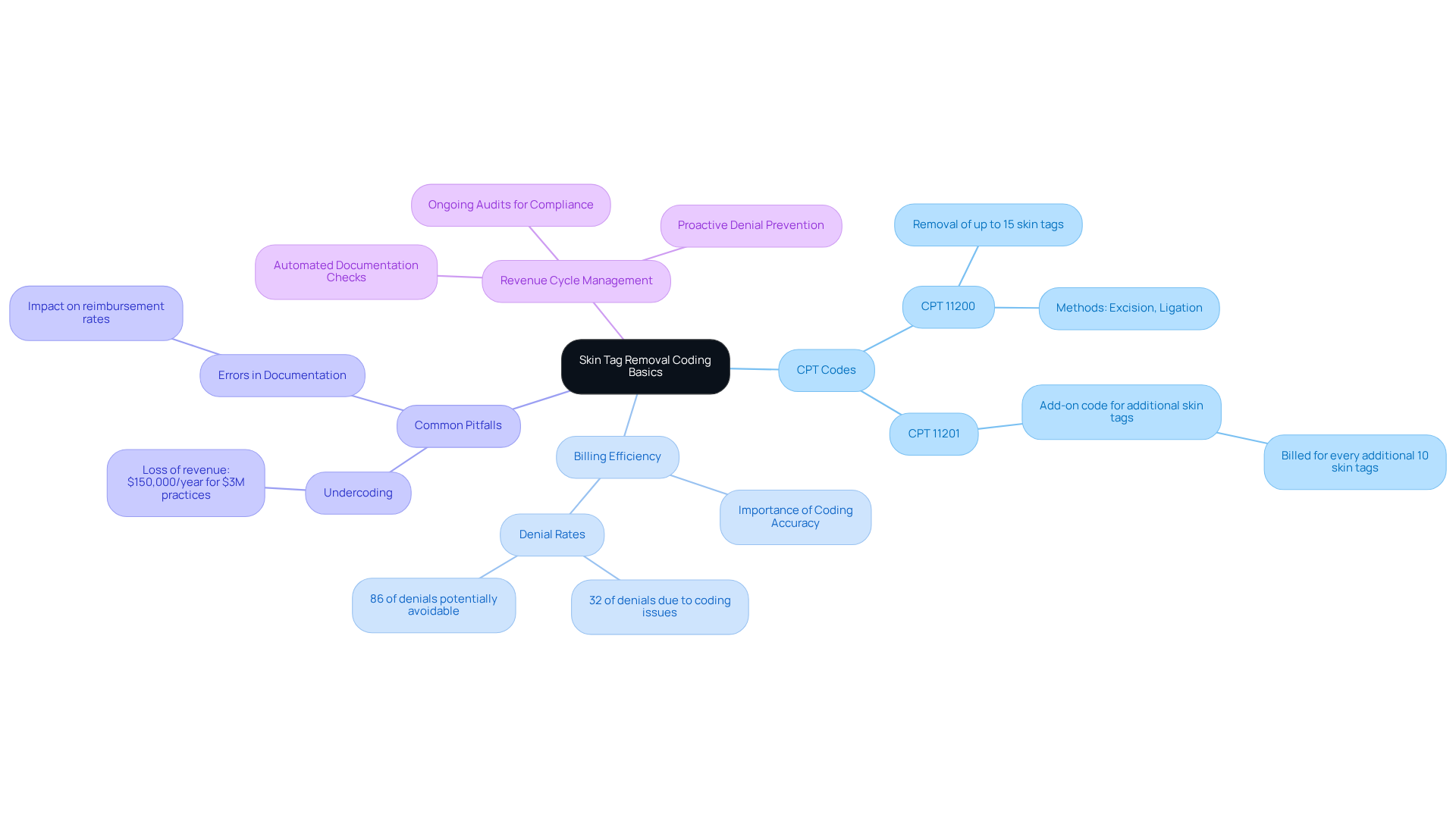
Understanding the code for skin tag removal is crucial for effective billing and operational efficiency. The code for skin tag removal is fundamentally rooted in the Current Procedural Terminology (CPT) and International Classification of Diseases (ICD) coding systems. The relevant CPT codes for skin tag removal include:
- CPT 11200: This code applies to the removal of up to 15 skin tags in a single session, covering various removal methods such as excision and ligation.
- CPT 11201: This add-on code for skin tag removal is used for the removal of additional skin tags beyond the initial 15, typically billed for every additional 10 skin tags removed.
A precise understanding of the code for skin tag removal is essential for efficient billing. It also helps reduce the likelihood of denial of requests. Roughly 32% of denials arise from coding mistakes, and significantly, 86% of these denials are possibly preventable. This highlights why clinics must stick to precise coding guidelines. Familiarity with these guidelines not only ensures compliance with insurance requirements but also enhances the clinic’s revenue cycle management.
As Healthcare Partners Consulting highlights, their committed AR specialists examine and rectify coding problems prior to submissions, greatly minimizing errors from the outset. Additionally, proactive follow-up with payers on unpaid or underpaid claims and appeal submissions for denied claims are essential services that further support clinics in optimizing their revenue cycle. Ongoing audits of high-impact areas are important for CPT compliance. Mastering these coding fundamentals and recognizing common pitfalls, like undercoding, can significantly enhance clinics’ financial outcomes and operational efficiency.
Identify Billable and Non-Billable ICD-10 Codes for Skin Tags
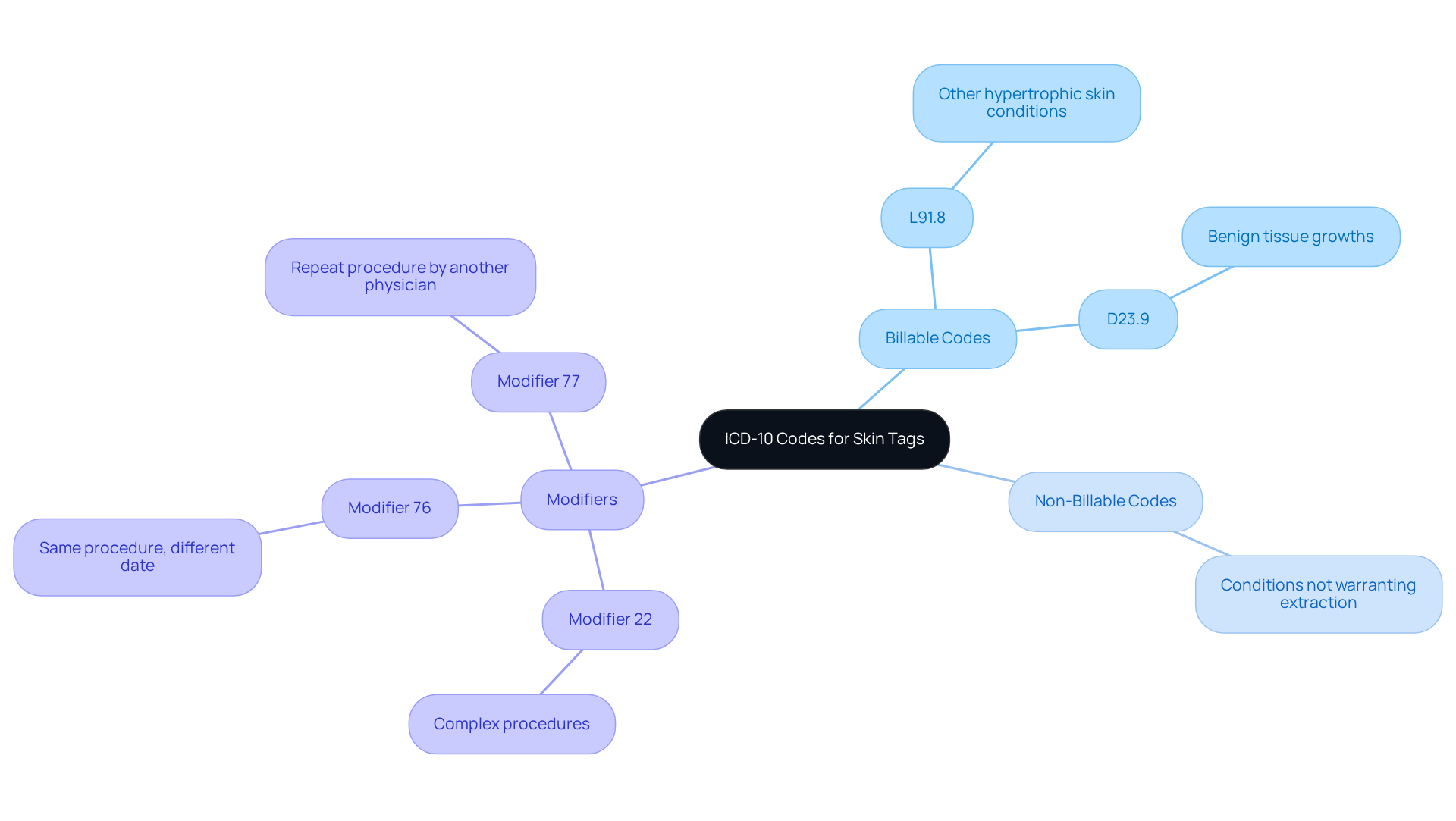
Understanding the nuances of billable versus non-billable ICD-10 codes is essential for effective coding, particularly when it comes to the code for skin tag removal. The primary billable code for skin tag removal is L91.8, which encompasses other hypertrophic disorders of the epidermis, including dermal tags (acrochordons). Additionally, the code for skin tag removal, D23.9, can be utilized for benign tissue growths that are not further specified, applicable in certain scenarios.
Clinics must navigate these distinctions to ensure efficient processing of requests and appropriate compensation for their services. Non-billable codes, particularly those linked to conditions that do not warrant extraction or are deemed purely cosmetic, can lead to reimbursement denials. This is particularly evident when coding asymptomatic lesions that do not require extraction, which may result in denied submissions. Understanding these distinctions ensures that requests are processed efficiently, allowing clinics to secure appropriate compensation for their services.
Modifiers such as 22 and 76 are also critical to consider. Modifier 22 applies when the skin tag removal procedure is more complex due to factors like excessive bleeding or multiple large skin tags, while Modifier 76 is used when the same provider performs the same procedure on a different date for the same patient.
Healthcare Partners Consulting examines and amends coding problems prior to submissions, adhering to payer-specific guidelines and remaining updated on CPT, ICD-10, and HCPCS revisions. Detailed medical records supporting the diagnosis and procedure are crucial to avoid coding errors and ensure compliance with billing guidelines. By implementing these practices, clinics can significantly reduce the risk of claim denials and enhance their overall billing accuracy. Ultimately, precise coding practices are vital for safeguarding clinic revenue and ensuring compliance with billing standards.
Document Medical Necessity for Skin Tag Removal Claims
To secure reimbursement for tag excision, clinics must prioritize meticulous documentation of medical necessity. This documentation should encompass several critical elements:
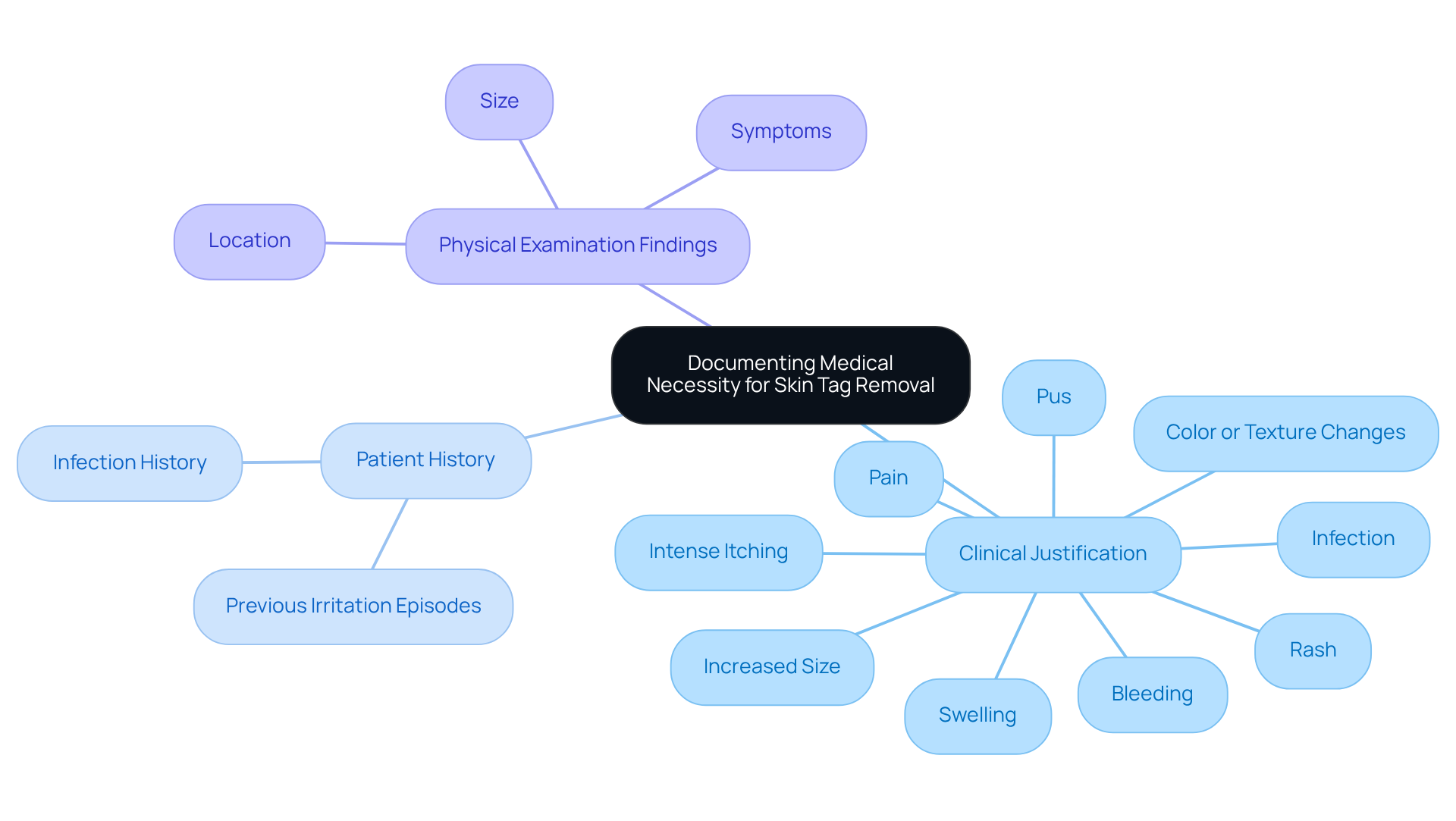
- Clinical Justification: Clearly articulate the reasons for extraction, such as discomfort, irritation, or potential complications arising from friction with clothing or jewelry. Symptoms indicating medical necessity include bleeding, increased size, pain, intense itching, color or texture changes, infection, pus, swelling, and rash. The ICD-10 code for tag excision is L91.8, which must be utilized for precise billing.
- Patient History: Include pertinent patient history that supports the need for removal, such as previous episodes of irritation or infection. This context is essential for illustrating the ongoing problems related to the growths on the epidermis.
- Physical Examination Findings: Document findings from the physical examination that indicate the skin tags are symptomatic rather than purely cosmetic. This may involve noting the size, location, and any symptoms experienced by the patient, which are essential for justifying the medical necessity of the procedure.
Thorough documentation can greatly reduce the likelihood of request denials for clinics. The high rejection rate of over 2.7 million requests in Connecticut underscores the challenges clinics face in securing reimbursements. Adhering to these best practices not only enhances approval rates but also contributes to the clinic’s operational efficiency. Additionally, by partnering with Healthcare Partners Consulting, clinics can leverage structured payment plans, proactive follow-up with payers, and aging report reviews to further streamline their billing operations and enhance revenue cycle efficiency. Ultimately, effective documentation practices can transform the reimbursement landscape for clinics, ensuring they receive the funds necessary to operate efficiently.
Utilize Modifiers Effectively in Skin Tag Removal Billing
Modifiers play a critical role in ensuring precise billing during procedures involving the code for skin tag removal, directly influencing claim approval rates. Key modifiers to consider include:
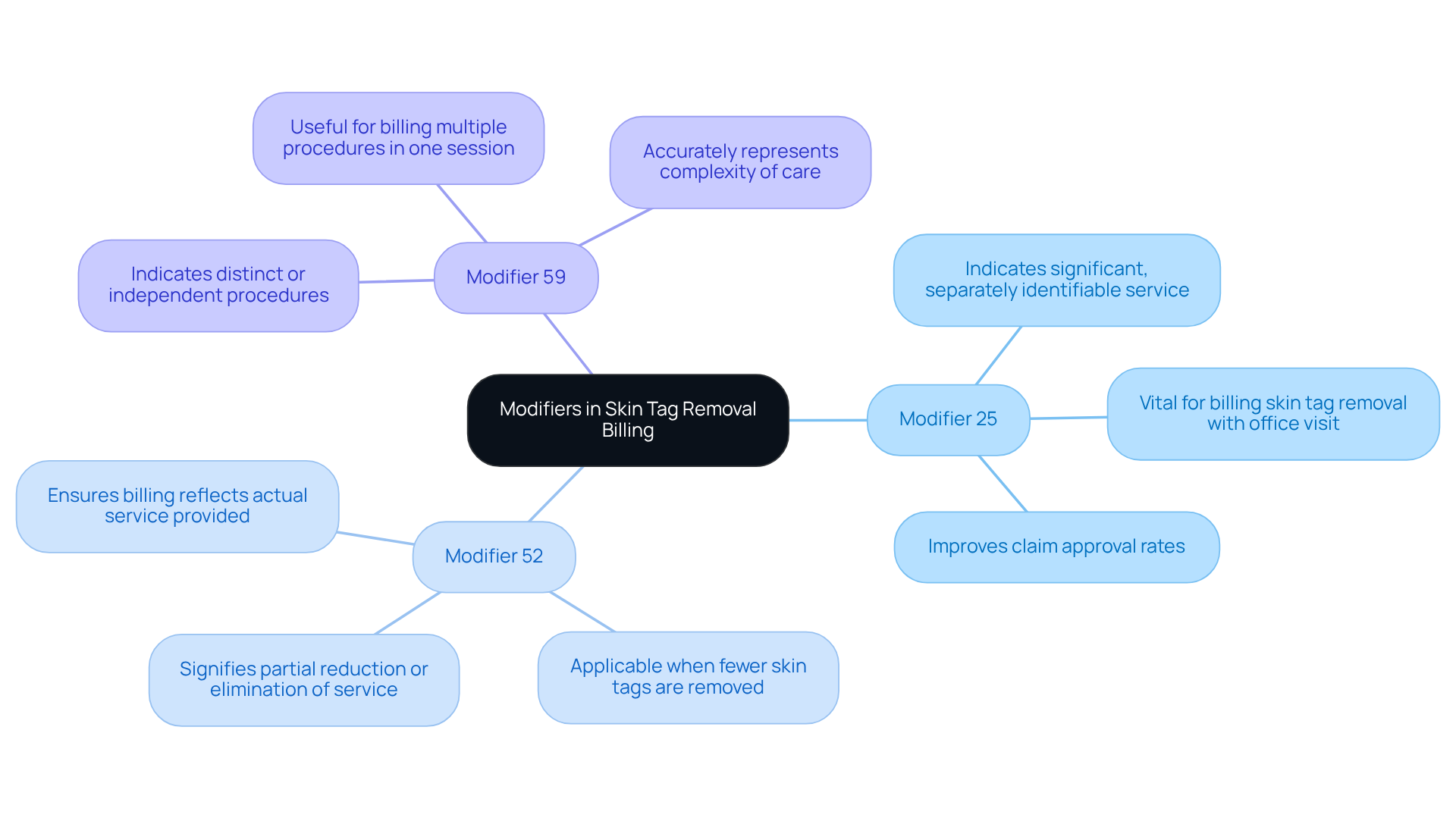
- Modifier 25: This modifier indicates that a significant, separately identifiable evaluation and management service was performed on the same day as the procedure. Its use is vital when charging for the code for skin tag removal along with an office visit, as it assists in validating the need for both services.
- Modifier 52: This modifier signifies that a service was partially reduced or eliminated. It is applicable when fewer skin tags are removed than initially planned, ensuring that the billing reflects the actual service provided.
- Modifier 59: This modifier indicates that procedures are distinct or independent from one another. It is particularly useful when billing for multiple procedures performed during the same session, allowing clinics to accurately represent the complexity of care delivered.
Using these modifiers correctly ensures requests are processed efficiently and boosts reimbursement for clinics. Clinics that effectively use Modifier 25 have seen improved claim approval rates, underscoring its significance in the billing process. Medical billing specialists emphasize that thorough documentation and appropriate modifier usage are key to avoiding denials and enhancing revenue cycles in dermatology practices.
Conclusion
Understanding the complexities of coding for skin tag removal is crucial for clinics seeking to enhance their billing accuracy and operational efficiency. By understanding the relevant CPT and ICD-10 codes, clinics ensure compliance with insurance requirements and reduce the risk of claim denials, which contributes to a stronger revenue cycle.
The article outlines key coding practices, including:
- The distinction between billable and non-billable ICD-10 codes
- The importance of documenting medical necessity
- The effective use of modifiers
Emphasizing the need for accurate coding and thorough documentation, clinics can significantly reduce the likelihood of reimbursement issues while ensuring they are fairly compensated for their services.
In light of the complexities surrounding skin tag removal coding, it is imperative for clinics to adopt best practices that enhance their billing accuracy and operational success. By investing time in coding guidelines and utilizing available resources, clinics can improve their billing practices and navigate skin tag removal confidently.
Frequently Asked Questions
Why is understanding skin tag removal coding important?
Understanding skin tag removal coding is crucial for effective billing and operational efficiency, helping to reduce the likelihood of denial of requests.
What are the relevant CPT codes for skin tag removal?
The relevant CPT codes for skin tag removal are CPT 11200, which applies to the removal of up to 15 skin tags in a single session, and CPT 11201, an add-on code for the removal of additional skin tags beyond the initial 15.
How does CPT 11200 differ from CPT 11201?
CPT 11200 covers the removal of up to 15 skin tags in one session, while CPT 11201 is used for each additional 10 skin tags removed beyond the initial 15.
What percentage of billing denials are due to coding mistakes?
Roughly 32% of billing denials arise from coding mistakes, with 86% of these denials potentially being preventable.
How can clinics minimize coding errors?
Clinics can minimize coding errors by adhering to precise coding guidelines, conducting ongoing audits of high-impact areas for CPT compliance, and utilizing the expertise of coding specialists.
What services do AR specialists provide to support clinics?
AR specialists examine and rectify coding problems before submissions, follow up with payers on unpaid or underpaid claims, and submit appeals for denied claims to optimize the clinic’s revenue cycle.
What common pitfalls should clinics be aware of in skin tag removal coding?
Clinics should be aware of common pitfalls such as undercoding, which can negatively impact their financial outcomes and operational efficiency.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting