General
5 Steps to Improve Patient Scheduling in Mental Health Clinics

Introduction
Improving patient scheduling in mental health clinics is not merely a logistical necessity; it is a critical factor that directly influences the quality of care and patient satisfaction. Research indicates that an alarming 30% of patients abandon healthcare facilities due to prolonged wait times, underscoring the urgency to optimize scheduling practices. This article examines actionable steps clinics can implement to enhance their scheduling processes, ranging from the adoption of advanced technologies to the implementation of best practices tailored to diverse patient needs. However, what occurs when traditional scheduling methods encounter the unique challenges inherent in mental health care? The following insights will elucidate how clinics can navigate these complexities to foster a more efficient and patient-centered scheduling experience.
Define Patient Scheduling and Its Importance
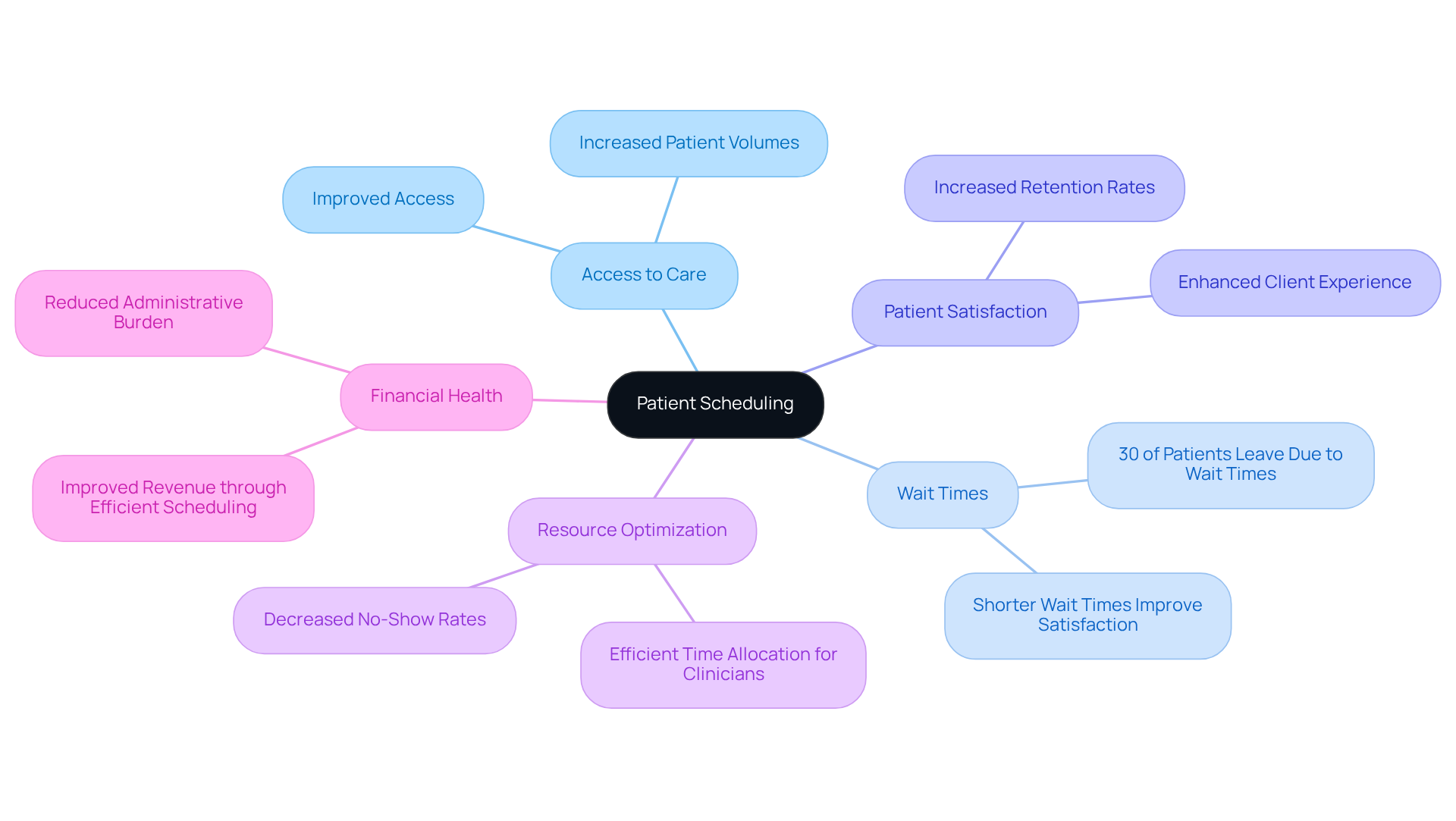
The arrangement of appointment times for individuals with healthcare providers represents a systematic organization. In mental health facilities, understanding how to improve patient scheduling is essential, as it significantly influences access to care, reduces wait times, and enhances the overall satisfaction of individuals receiving treatment. Research indicates that 30% of patients leave healthcare facilities due to extended wait times, emphasizing the importance of understanding how to improve patient scheduling through effective appointment management.
Effective planning enables clinicians to allocate their time efficiently, allowing them to concentrate on delivering quality care rather than being burdened by administrative tasks. Furthermore, understanding how to improve patient scheduling through efficient appointment management optimizes clinic resources, decreases no-show rates, and ultimately improves the financial health of the practice. By implementing effective planning techniques, mental wellness centers can learn how to improve patient scheduling, fostering a more favorable client experience and leading to increased satisfaction and retention rates.
Healthcare Partners Consulting offers essential tools and comprehensive administrative support tailored specifically for mental wellness providers, streamlining credentialing and administrative responsibilities. By utilizing automated reminders and confirmations, mental wellness clinics can further enhance appointment efficiency, ultimately resulting in improved client engagement and satisfaction.
Identify Common Scheduling Challenges in Mental Health Clinics
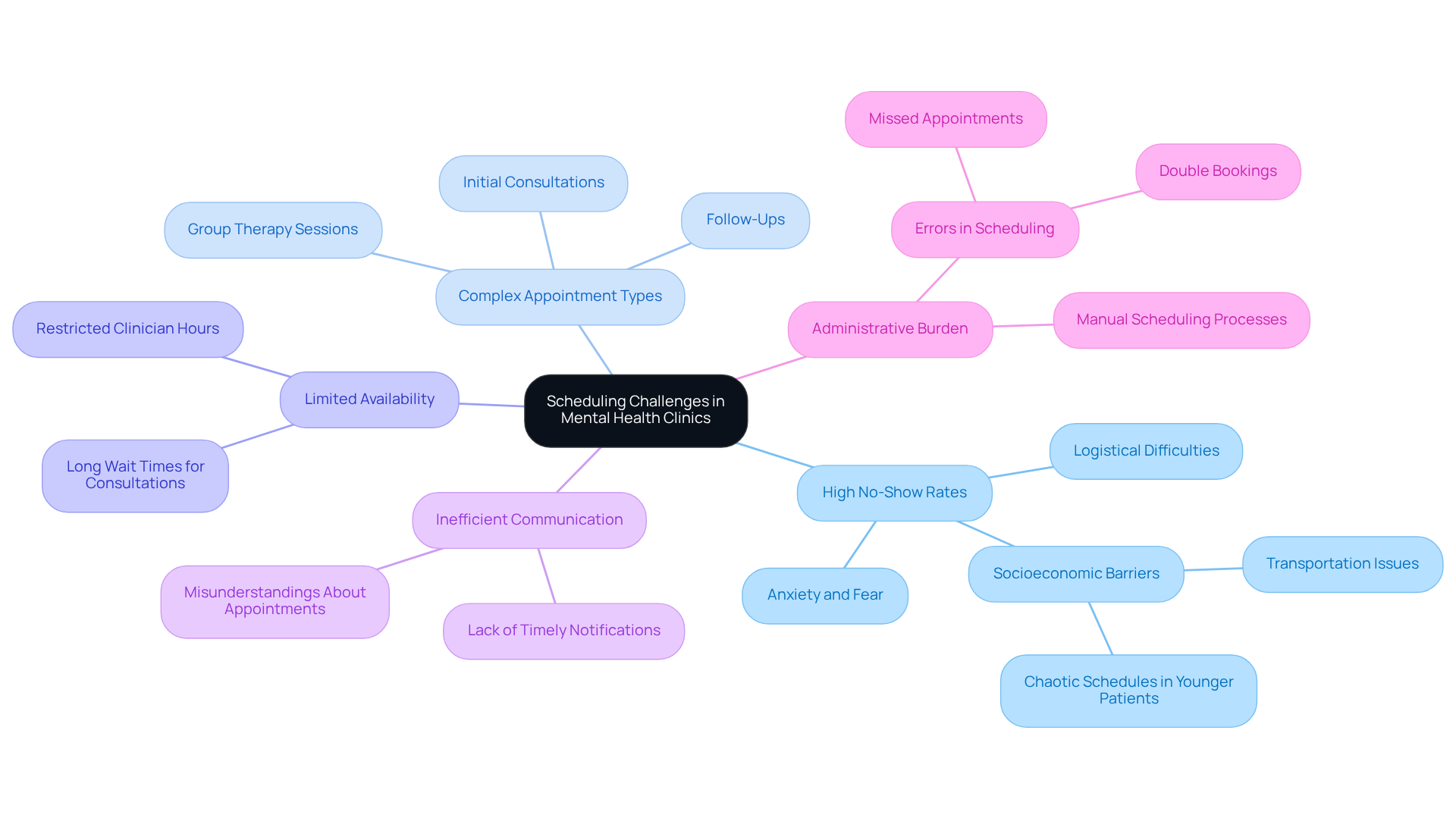
Mental health clinics frequently face a variety of scheduling challenges that demonstrate the importance of understanding how to improve patient scheduling, which can significantly affect patient care and operational efficiency.
High No-Show Rates: A persistent issue, no-show rates for mental health appointments can reach as high as 60% in certain outpatient programs. Contributing factors include individual anxiety, logistical difficulties, and socioeconomic barriers. For example, younger individuals often demonstrate higher no-show rates due to chaotic schedules, while elderly patients may encounter transportation issues or memory challenges.
Complex Appointment Types: The diversity of appointment types – such as initial consultations, follow-ups, and group therapy sessions – requires tailored scheduling strategies. Each type demands specific attention to detail to ensure that individuals receive appropriate care at the right time.
Limited Availability: Clinicians frequently operate under restricted hours, complicating efforts to accommodate the varied needs of individuals seeking care. This limitation can result in longer wait times for consultations, further exacerbating no-show rates.
Inefficient Communication: Ineffective communication between staff and patients can lead to misunderstandings regarding scheduled times and requirements. For instance, patients may not receive timely notifications or may be unclear about what to expect during their visits, which can heighten anxiety and lead to missed appointments.
Administrative Burden: Manual scheduling processes are not only time-consuming but also susceptible to errors, such as double bookings or missed appointments. Implementing automated scheduling systems can alleviate this burden, enabling staff to focus more on patient care rather than administrative tasks.
Addressing these challenges with evidence-based strategies can enhance access for individuals and improve overall clinic efficiency, which is essential for understanding how to improve patient scheduling and ultimately leads to better outcomes for patients.
Implement Best Practices for Effective Patient Scheduling
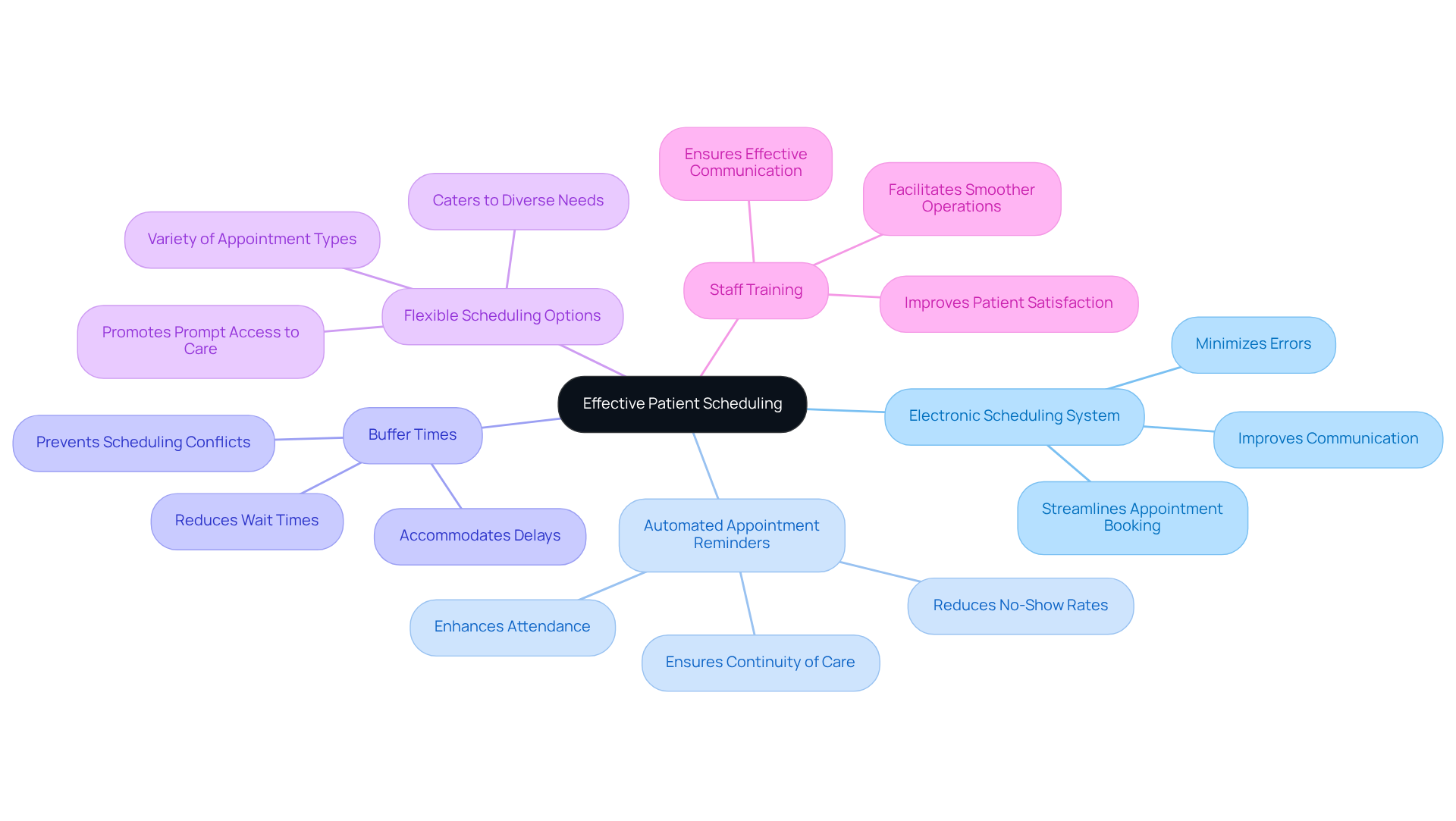
To enhance patient scheduling in mental health clinics, consider implementing the following best practices:
- Utilize an Electronic Scheduling System: Adopting a digital scheduling platform can significantly streamline the appointment booking process, minimize errors, and improve communication between staff and patients. These systems provide real-time visibility of available slots, enabling better management of visitor flow.
- Automate Appointment Reminders: Implementing automated reminders via text or email effectively reduces no-show rates. By keeping patients informed about their upcoming visits, clinics can enhance attendance and ensure continuity of care. Research indicates that automated reminders can illustrate how to improve patient scheduling by leading to a substantial decrease in missed visits and thereby improving overall clinic efficiency.
- Build Buffer Times: Integrating buffer periods between meetings accommodates delays and prevents scheduling conflicts. This practice not only enhances the experience for individuals by reducing wait times but also enables staff to manage unexpected situations more effectively.
- Offer Flexible Scheduling Options: Providing individuals with a variety of appointment types – such as in-person, telehealth, and same-day appointments – caters to diverse needs and preferences. Adaptability in scheduling is increasingly crucial for knowing how to improve patient scheduling, as individuals now expect prompt access to care.
- Train Staff on Appointment Protocols: Ensuring that all team members are well-trained on the appointment system and understand the importance of effective communication with clients is essential. An informed team facilitates smoother operations and improves satisfaction, ultimately leading to better wellness outcomes.
Utilize Tools and Technologies for Streamlined Scheduling
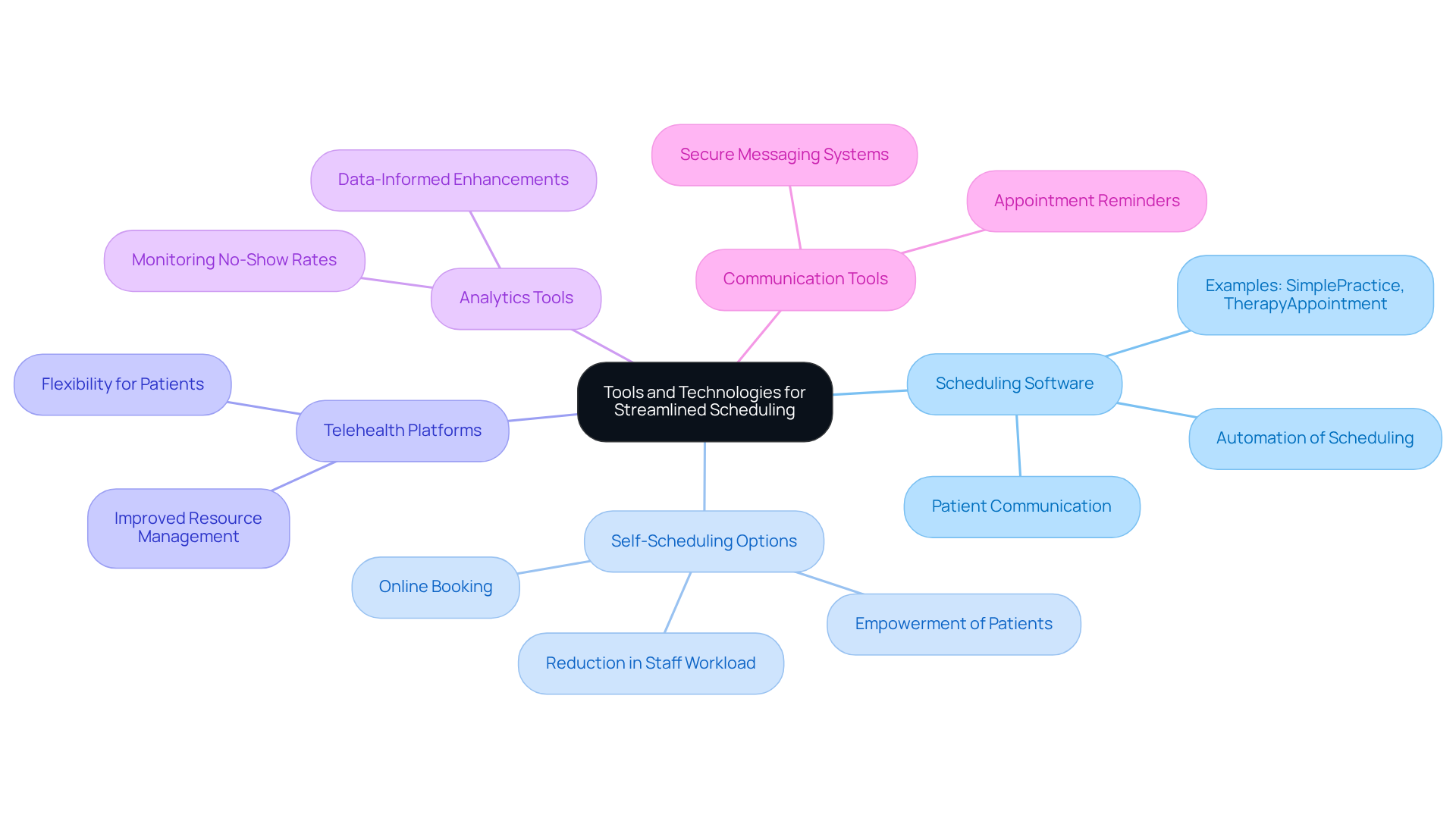
To enhance scheduling efficiency, mental health clinics should consider several key tools and technologies:
- Scheduling Software: Platforms such as SimplePractice or TherapyAppointment can automate scheduling, reminders, and patient communications. This automation significantly reduces the administrative workload, allowing staff to focus on patient care.
- Self-Scheduling Options for Individuals: By enabling individuals to schedule their visits online, clinics can enhance accessibility and decrease the workload on staff. This approach empowers patients and shows how to improve patient scheduling.
- Telehealth Platforms: Integrating telehealth solutions offers flexibility for individuals and assists clinics in managing their schedules more effectively. This adaptability can lead to improved patient satisfaction and better resource allocation, which is crucial for learning how to improve patient scheduling.
- Analytics Tools: Utilizing analytics to monitor metrics such as no-show rates and duration of visits facilitates data-informed enhancements. These insights enable clinics to make strategic adjustments on how to improve patient scheduling and enhance overall efficiency.
- Communication Tools: Implementing secure messaging systems enhances interaction between individuals receiving care and staff. This ensures clarity regarding scheduled visits and fosters a more supportive environment for patients.
Monitor and Evaluate Scheduling Effectiveness
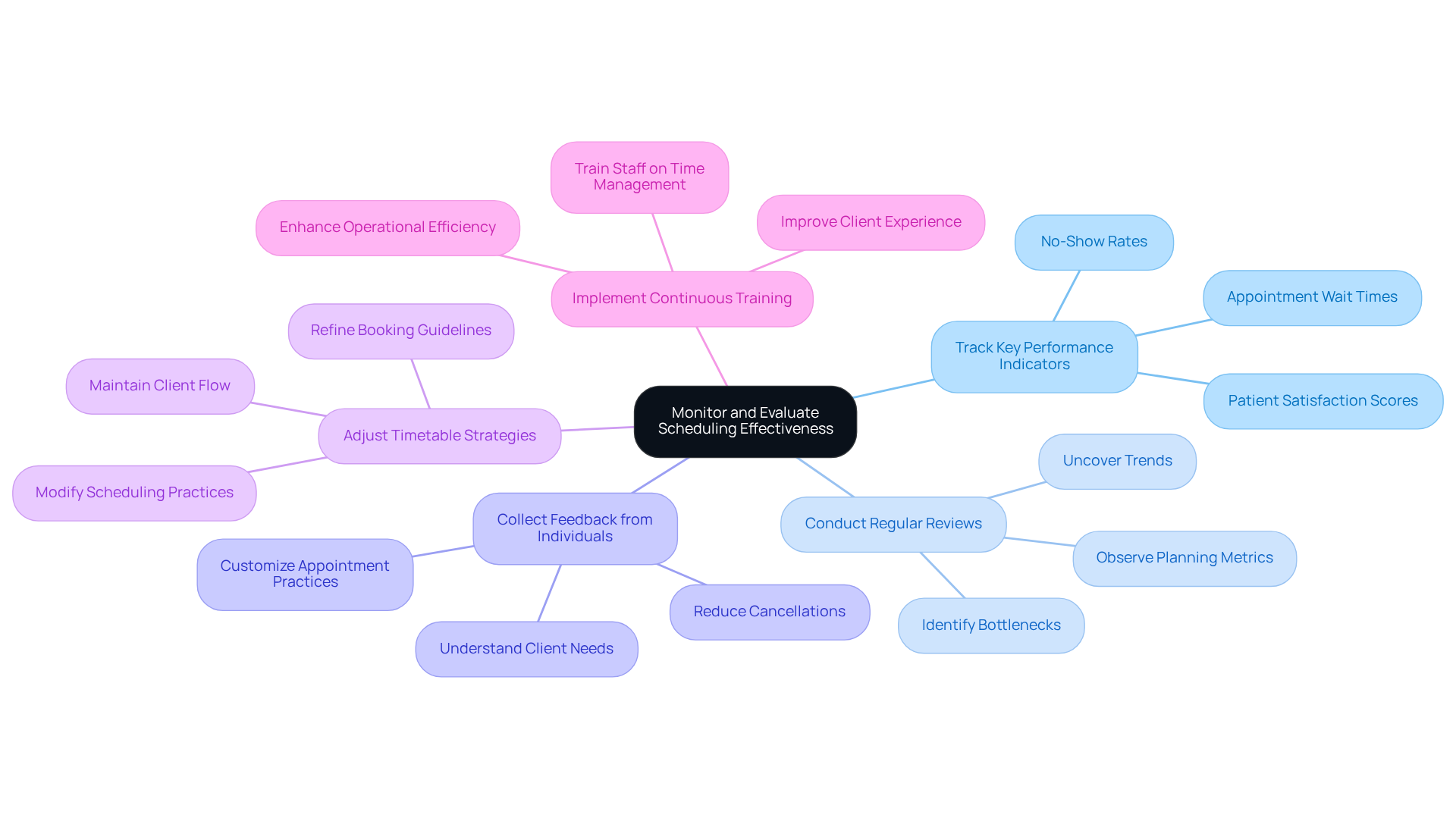
To enhance the effectiveness of scheduling practices in mental health clinics, it is essential to focus on several key strategies:
- Track Key Performance Indicators (KPIs): Regular monitoring of critical metrics such as appointment wait times, no-show rates, and patient satisfaction scores is vital. Approximately 78.5% of individuals report a positive evaluation of their booking experience, indicating that efficient monitoring can significantly enhance client perceptions and operational effectiveness.
- Conduct Regular Reviews: Implementing periodic assessments of the scheduling process allows for the identification of bottlenecks and areas needing improvement. By consistently observing planning metrics, clinics can uncover trends that inform necessary modifications, ultimately improving access and satisfaction for individuals.
- Collect Feedback from Individuals: Actively seeking opinions from individuals regarding their appointment experiences is crucial. Understanding the needs and preferences of clients enables the customization of appointment practices, thereby reducing cancellations and enhancing overall satisfaction.
- Adjust Timetable Strategies: Clinics must be prepared to modify scheduling practices based on the data collected. For instance, refining booking guidelines can lead to fewer reservation conflicts and a more seamless process, which is essential for maintaining client flow and satisfaction.
- Implement Continuous Training: Regular training for staff on new time management practices and technologies is necessary. Well-trained staff are more likely to enhance operational efficiency and improve the client experience, resulting in higher performance levels in managing appointments.
By concentrating on these strategies, mental health clinics can discover how to improve patient scheduling effectiveness, leading to better patient outcomes and operational success.
Conclusion
Improving patient scheduling in mental health clinics transcends mere logistical challenges; it stands as a crucial element that profoundly influences patient care and clinic efficiency. By grasping the complexities of scheduling, mental health providers can enhance access to services, minimize wait times, and ultimately cultivate a more satisfying experience for individuals seeking treatment.
This guide has highlighted several key strategies, including:
- The adoption of electronic scheduling systems
- The implementation of automated reminders
- The provision of flexible scheduling options
Furthermore, addressing prevalent challenges such as high no-show rates and ineffective communication can lead to more efficient appointment management. The utilization of tools and technologies, such as telehealth platforms and analytics, further streamlines the scheduling process, ensuring that clinics can meet the diverse needs of their patients.
As mental health clinics pursue operational excellence, prioritizing effective scheduling practices becomes essential. By continuously monitoring performance metrics and gathering patient feedback, clinics can adapt and refine their scheduling approaches. Embracing these strategies not only enhances patient satisfaction but also contributes to improved overall health outcomes, underscoring the critical role of effective patient scheduling in mental health care.
Frequently Asked Questions
What is patient scheduling and why is it important?
Patient scheduling refers to the arrangement of appointment times for individuals with healthcare providers. It is important because it influences access to care, reduces wait times, and enhances overall patient satisfaction. Effective scheduling can lead to improved client experiences and better retention rates.
What impact do long wait times have on patients?
Research indicates that 30% of patients leave healthcare facilities due to extended wait times. This highlights the need for effective patient scheduling to minimize wait times and improve access to care.
How can effective planning improve patient scheduling in mental health clinics?
Effective planning allows clinicians to allocate their time efficiently, focus on delivering quality care, optimize clinic resources, decrease no-show rates, and enhance the financial health of the practice.
What common scheduling challenges do mental health clinics face?
Common challenges include high no-show rates, complex appointment types, limited clinician availability, inefficient communication, and administrative burdens.
What are the reasons behind high no-show rates in mental health appointments?
High no-show rates can reach up to 60% due to factors like individual anxiety, logistical difficulties, and socioeconomic barriers. Younger individuals may have chaotic schedules, while elderly patients may face transportation issues or memory challenges.
Why is it important to tailor scheduling strategies for different appointment types?
Different appointment types, such as initial consultations, follow-ups, and group therapy sessions, require specific attention to detail to ensure that patients receive the appropriate care at the right time.
How does limited clinician availability affect patient scheduling?
Limited clinician hours can complicate efforts to meet the varied needs of individuals seeking care, resulting in longer wait times for consultations and potentially increasing no-show rates.
What role does communication play in patient scheduling?
Ineffective communication between staff and patients can lead to misunderstandings about scheduled times and requirements, increasing patient anxiety and leading to missed appointments.
How can automated scheduling systems benefit mental health clinics?
Automated scheduling systems can alleviate the administrative burden of manual processes, reduce errors like double bookings, and allow staff to focus more on patient care rather than administrative tasks.
What solutions can be implemented to improve patient scheduling in mental health clinics?
Evidence-based strategies such as utilizing automated reminders, improving communication, and addressing the specific challenges of appointment types can enhance access and overall clinic efficiency.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting