Healthcare Compliance Strategies
Enhance Collaboration with City of Memphis EMS Services: Best Practices

Introduction
Effective collaboration between emergency medical services (EMS) and mental health providers is essential for addressing the complexities inherent in psychological crises. By implementing best practices, such as:
- Establishing clear communication channels
- Integrating mental health protocols into training
stakeholders can significantly enhance the quality of care delivered to individuals in distress. Despite these efforts, challenges persist in achieving seamless collaboration between these diverse teams to ensure timely and effective responses during critical moments. This article explores essential strategies for fostering successful partnerships between the City of Memphis EMS services and mental health professionals, which is critical for achieving improved outcomes in crisis situations.
Establish Clear Communication Channels with EMS
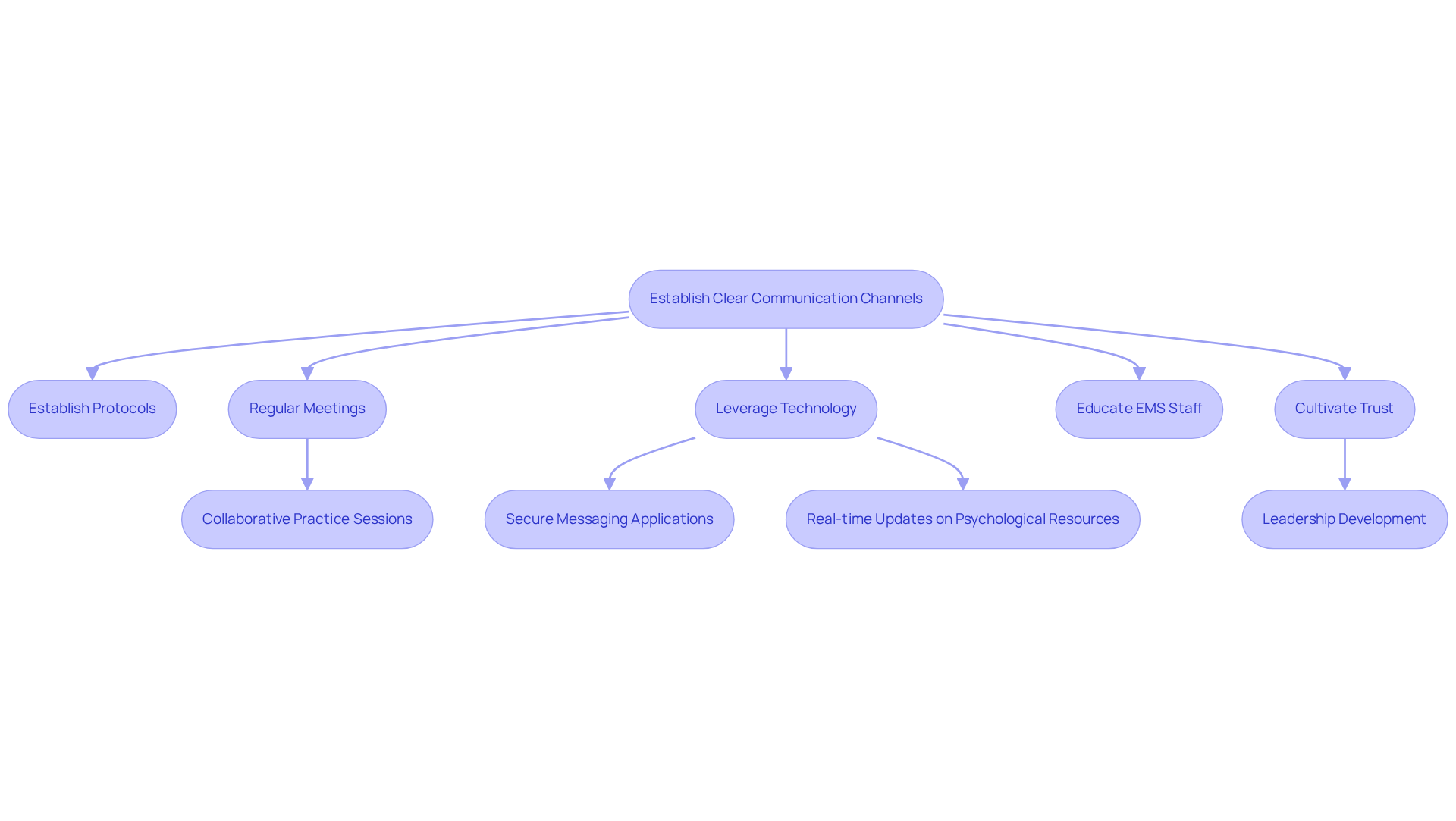
Effective collaboration with the city of Memphis EMS services hinges on establishing clear communication channels. This requires establishing protocols for sharing information between wellness providers and EMS personnel. Regular meetings and collaborative practice sessions are crucial for ensuring all parties understand these protocols. Leveraging technology, such as secure messaging applications or dedicated communication platforms, can facilitate efficient information sharing and minimize response times during emergencies. For instance, a collaborative digital platform that enables EMS to access real-time updates on psychological resources can greatly improve coordination during crises.
Moreover, educating EMS staff on psychological matters and the particular requirements of patients is essential. This not only enhances the quality of care delivered but also cultivates trust between EMS and psychological professionals, ultimately resulting in improved patient outcomes. Leadership plays a vital role in cultivating a culture of trust and inclusion, which is essential for long-term collaboration. By prioritizing effective communication strategies and tackling the challenges presented by increasing emergency incidents and limited workforce resources, both EMS and psychological services can collaborate more efficiently to handle the complexities of emotional crises. Integrating peer support and case management into the collaborative framework will significantly enhance the effectiveness of responses to psychological crises.
Integrate Mental Health Protocols into EMS Training
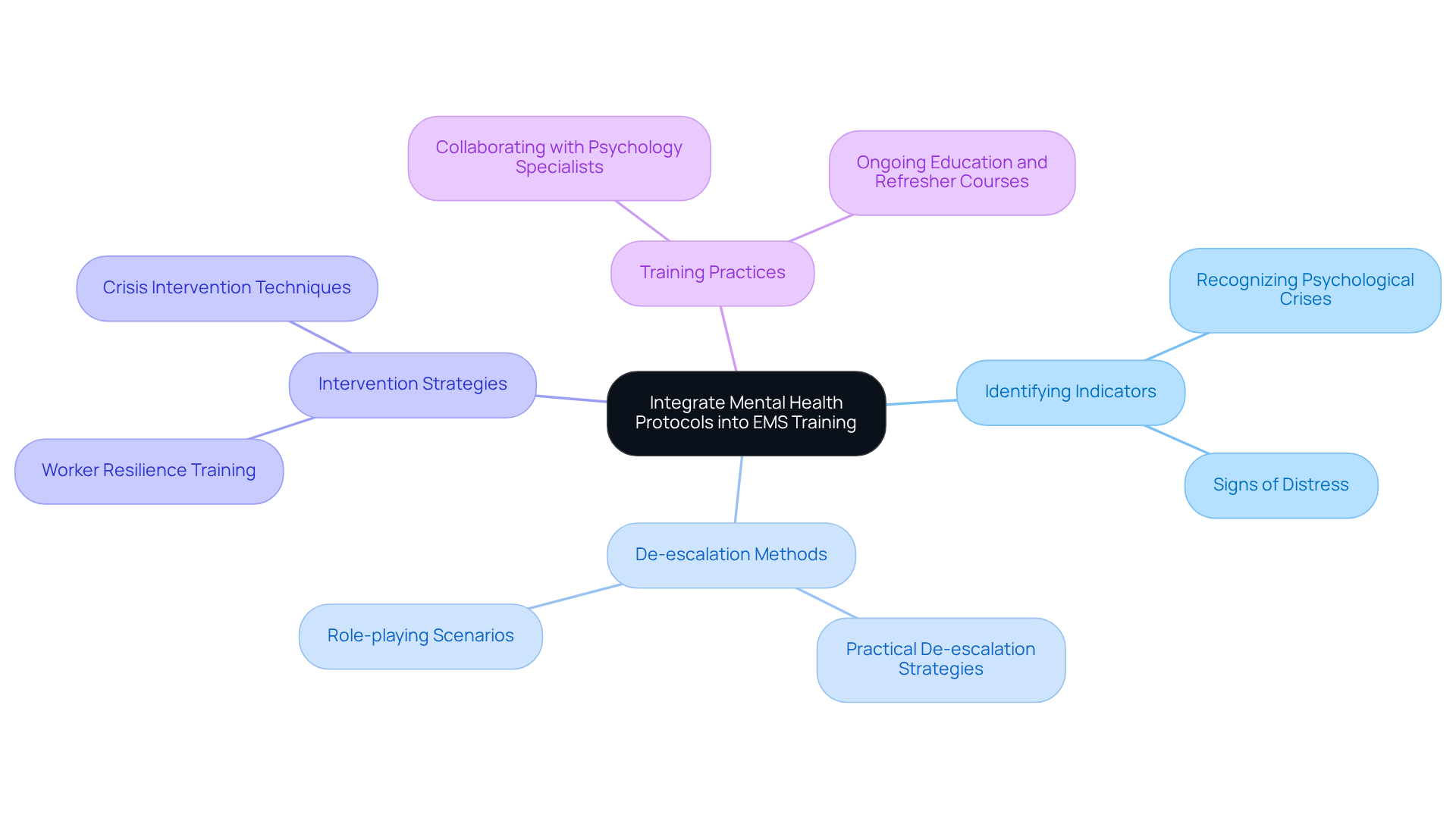
The integration of psychological protocols into EMS education is essential for equipping first responders to manage mental health crises effectively. Thorough instructional modules should encompass:
- Identifying indicators of psychological crises
- Utilizing de-escalation methods
- Applying suitable intervention strategies
Notably, EMS staff respond to an estimated 10-20% of all emergency calls involving a behavioral wellness crisis each year, underscoring the necessity for specialized instruction.
Educational programs should incorporate role-playing scenarios that simulate psychological crises, allowing EMS staff to practice their responses in a controlled setting. Collaborating with psychology specialists to develop educational content ensures its relevance and applicability. Furthermore, utilizing platforms such as Ninth Brain’s customizable learning management system (LMS) can support continuous wellness education programs, ensuring that EMS teams remain informed about best practices.
Regular refresher courses and updates on emerging psychological issues are vital for enhancing the skills of EMS personnel, enabling them to provide optimal care during crises. Effective instructional modules often include interactive components that engage participants and reinforce learning. Programs like the Worker Resilience Training and initiatives such as CAHOOTS in Eugene, Oregon, exemplify effective practices in psychological crisis intervention. Ultimately, prioritizing psychological wellness training can transform EMS responses, leading to more effective interventions for individuals in emotional distress.
Develop Joint Response Plans for Mental Health Emergencies
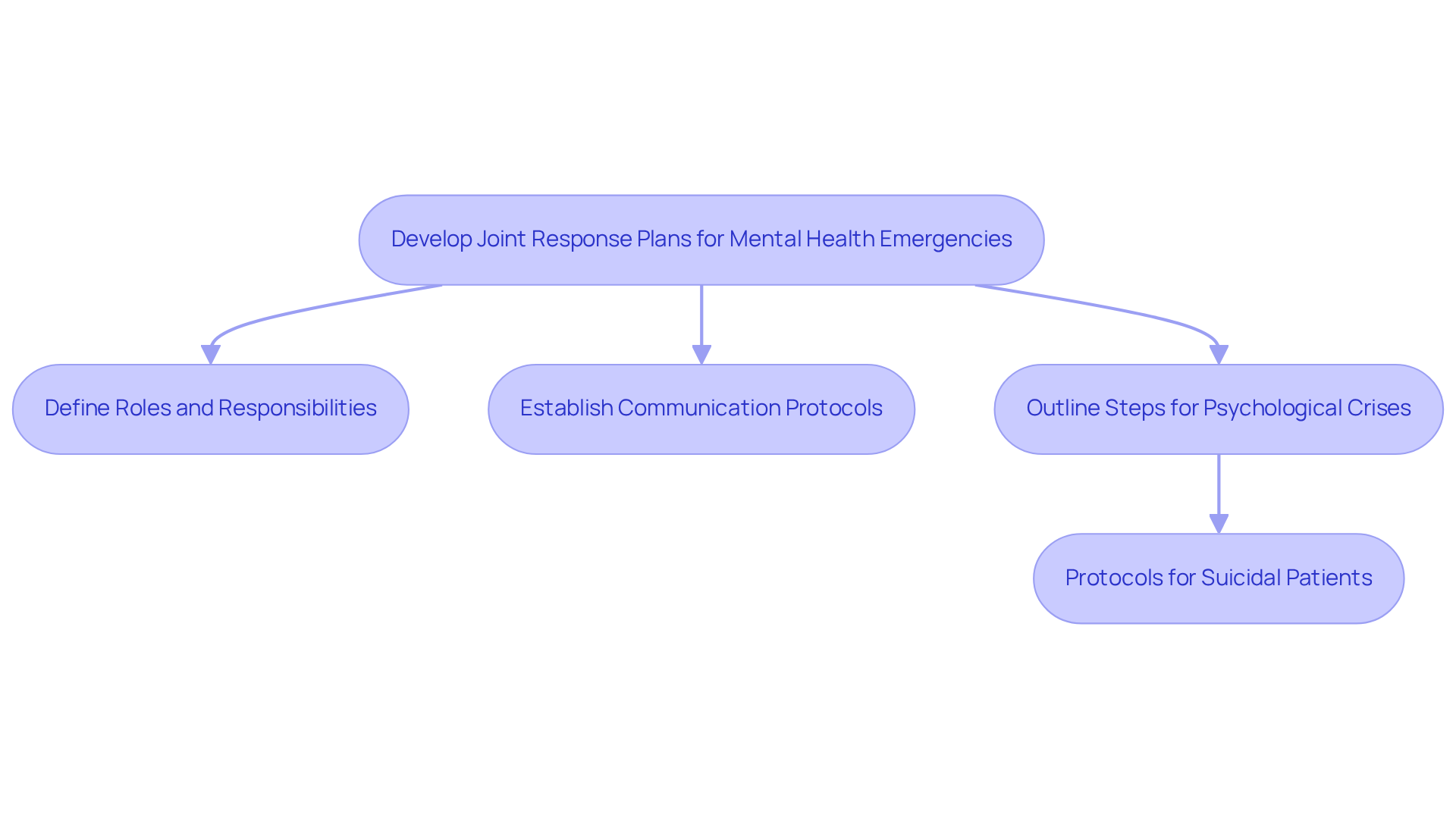
Current response strategies for psychological emergencies often lack clarity, hindering effective crisis management by EMS and psychological care providers. These plans must:
- Clearly define roles and responsibilities
- Establish communication protocols
- Outline steps for various psychological crises
For instance, protocols for suicidal patients should clarify when EMS should involve psychological specialists and how to ensure a smooth transition of care. Regular drills and simulations help EMS and psychological support teams practice these plans and identify areas for improvement. Cultivating collaboration and shared responsibility within these plans can lead to improved care quality for individuals in crisis. Ultimately, refining these collaborative strategies can transform crisis response, ensuring individuals receive timely and effective care when they need it most.
Implement Continuous Evaluation and Feedback Mechanisms
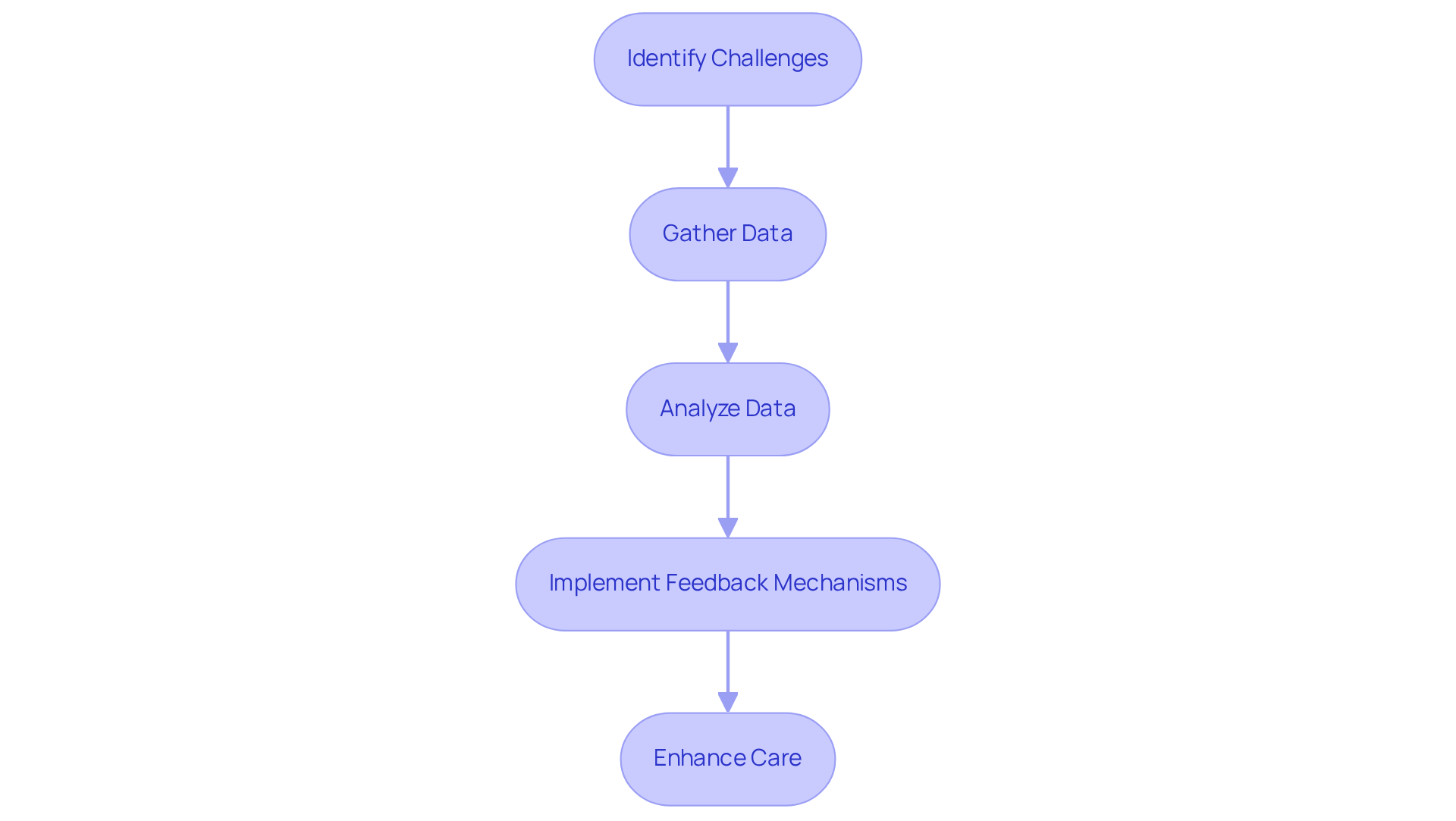
The collaboration between EMS and psychological services often encounters challenges that hinder effective response to mental health crises. Establishing a framework for regular assessment of joint response efforts is crucial for identifying areas for improvement and ensuring that both parties meet their objectives effectively.
Gathering data on response times, patient outcomes, and intervention effectiveness is crucial for assessing joint response efforts during psychological crises. Input from EMS staff and psychological service providers can be collected through surveys or debriefing sessions after incidents, enabling a thorough understanding of the collaboration’s strengths and weaknesses. By analyzing this data, organizations can implement structured assessment and feedback mechanisms, enabling informed decisions about training needs and resource allocation. This ultimately enhances care for individuals experiencing mental health crises.
Conclusion
Collaboration between EMS and mental health services is crucial for improving care during crises. Establishing clear communication channels, integrating mental health protocols into training, developing joint response plans, and implementing continuous evaluation mechanisms are critical steps in achieving this goal. Prioritizing these best practices enables EMS personnel to navigate emotional crises effectively and enhance patient outcomes.
Key insights from the article highlight the importance of structured communication, the necessity for specialized mental health training, and the value of collaborative response strategies. Regular meetings, the use of technology for information sharing, and role-playing scenarios are among the strategies that can significantly improve coordination between EMS and psychological professionals. Furthermore, ongoing evaluation and feedback loops are vital for identifying areas for improvement, ensuring that both EMS and mental health services can adapt and respond effectively to the evolving needs of the community.
Ultimately, prioritizing collaboration can transform crisis management into a proactive and compassionate response system. By embracing these best practices, stakeholders can create a more responsive and compassionate system that addresses the urgent needs of individuals in distress. This collaboration not only enhances patient outcomes but also fosters a more supportive environment for EMS personnel.
Frequently Asked Questions
Why is establishing clear communication channels important for collaboration with EMS?
Clear communication channels are vital for effective collaboration with Memphis EMS services as they ensure proper information sharing between wellness providers and EMS personnel, leading to improved coordination during emergencies.
What methods can be used to enhance communication between wellness providers and EMS personnel?
Methods to enhance communication include establishing protocols for information sharing, conducting regular meetings and collaborative practice sessions, and leveraging technology such as secure messaging applications or dedicated communication platforms.
How can technology improve communication during emergencies?
Technology can facilitate efficient information sharing and minimize response times by providing EMS personnel with real-time updates on psychological resources through collaborative digital platforms.
Why is it important to educate EMS staff on psychological matters?
Educating EMS staff on psychological matters and the specific needs of patients enhances the quality of care provided, builds trust between EMS and psychological professionals, and ultimately improves patient outcomes.
What role does leadership play in the collaboration between EMS and psychological services?
Leadership is crucial in cultivating a culture of trust and inclusion, which is essential for long-term collaboration between EMS and psychological services.
How can EMS and psychological services address challenges in emergency incidents?
By prioritizing effective communication strategies and integrating peer support and case management into their collaborative framework, EMS and psychological services can better handle the complexities of emotional crises, especially in the face of increasing emergency incidents and limited workforce resources.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting