Mastering Medical Coding
Master ICD-10 Code for Lipid Panel: Best Practices for Clinics

Introduction
Understanding the complexities of ICD-10 coding is essential for clinics that seek to optimize their billing practices. This is particularly true for lipid panels, which are crucial in evaluating cardiovascular health. This article explores best practices that empower healthcare providers to navigate the intricacies of ICD-10 classification.
- Accurate documentation and compliance are vital for minimizing claim denials and enhancing revenue cycle management.
- As changes to coding guidelines approach, clinics must consider how to adapt their processes effectively.
- This adaptation is key to safeguarding their financial health while continuing to deliver quality patient care.
Understand ICD-10 Coding Fundamentals for Lipid Panels
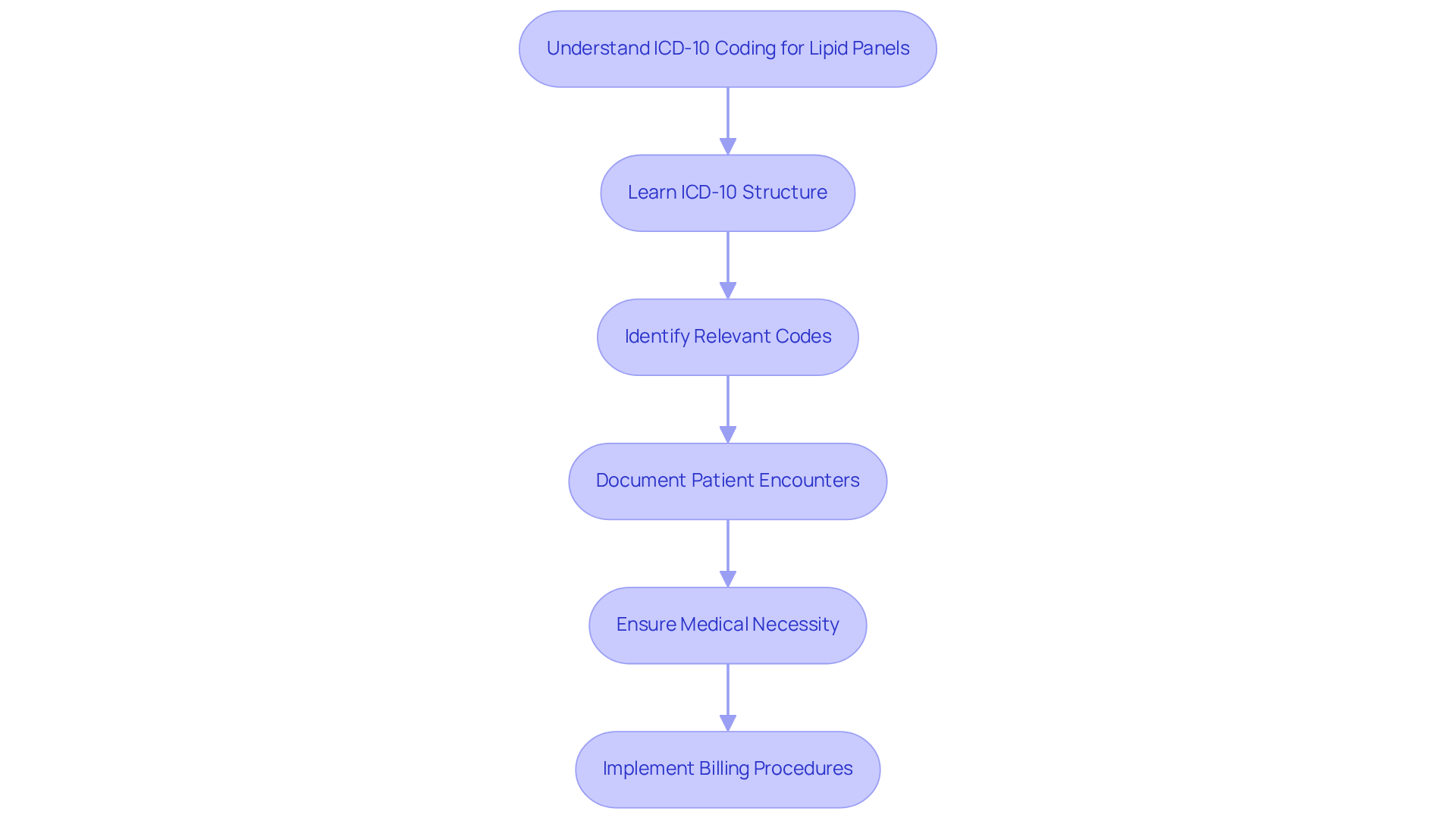
ICD-10 coding is essential in healthcare financing, especially when using the ICD 10 code for lipid panel, which is vital for assessing cardiovascular health. The ICD-10-CM (Clinical Modification) system classifies diagnoses into specific identifiers that healthcare providers must utilize for billing purposes. For lipid panels, identifiers like Z13.220, which is designated for screening lipoid disorders, are crucial. This guideline specifically applies to asymptomatic individuals undergoing lipid screening, ensuring that charges accurately reflect the clinical needs of the patient.
Clinics must grasp the structure of ICD-10 codes, which includes categories, subcategories, and specific codes. This understanding is critical for accurately documenting patient encounters and justifying the medical necessity of the tests performed. Effective programming not only streamlines invoicing processes but also enhances compliance with insurance standards, significantly reducing the likelihood of claim rejections. Inadequate programming can lead to substantial financial repercussions; for instance, a study indicated that hospitals could face losses of up to £29,000 due to incorrect patient classification. Therefore, clinics should prioritize training and resources to ensure the successful implementation of the ICD 10 code for lipid panel billing, ultimately improving their revenue cycle management.
Healthcare Partners Consulting provides comprehensive accounts receivable management solutions that tackle these challenges. Their services include:
- Proactive follow-up with payers on unpaid or underpaid claims
- Appeal submissions for denied requests
- Coordination of structured payment plans
By emphasizing precise programming and offering ongoing updates and reporting, HPC assists clinics in enhancing their revenue cycle management, improving cash flow, and fostering sustainable growth. Leveraging HPC’s expertise enables clinics to navigate the complexities of medical classification and claims processing effectively.
Identify Key ICD-10 Codes for Lipid Panel Billing
Precise ICD-10 classification, particularly the ICD-10 code for lipid panel, is essential for ensuring appropriate compensation when billing for lipid panels, especially in light of the 2026 revisions that introduced 614 new diagnosis identifiers effective October 1, 2025. Key codes to utilize include:
- Z13.220: Encounter for screening for lipoid disorders, applicable for patients undergoing lipid screening without symptoms.
- E78.5: Dyslipidemia, unspecified, used when dyslipidemia is documented without further specification.
- E78.0: Pure hypercholesterolemia, designated for cases where specific lipid abnormalities are identified.
Clinics should develop a comprehensive reference guide that incorporates these essential codes to streamline the billing process. Routine training sessions for programming personnel are crucial to enhance precision and adherence, ensuring that all claims are supported by appropriate documentation. This proactive strategy not only minimizes claim denials but also improves reimbursement rates, as accurate classification directly influences financial outcomes for healthcare practices. Furthermore, monitoring early programming and invoicing information is vital for identifying patterns associated with the new classifications, enabling clinics to adapt effectively to the evolving classification landscape. As noted by the American Medical Association, “Accurate selection of classifications relies on understanding not just what has changed, but why,” underscoring the importance of thorough training and awareness in classification practices.
Ensure Proper Documentation and Compliance for Claims
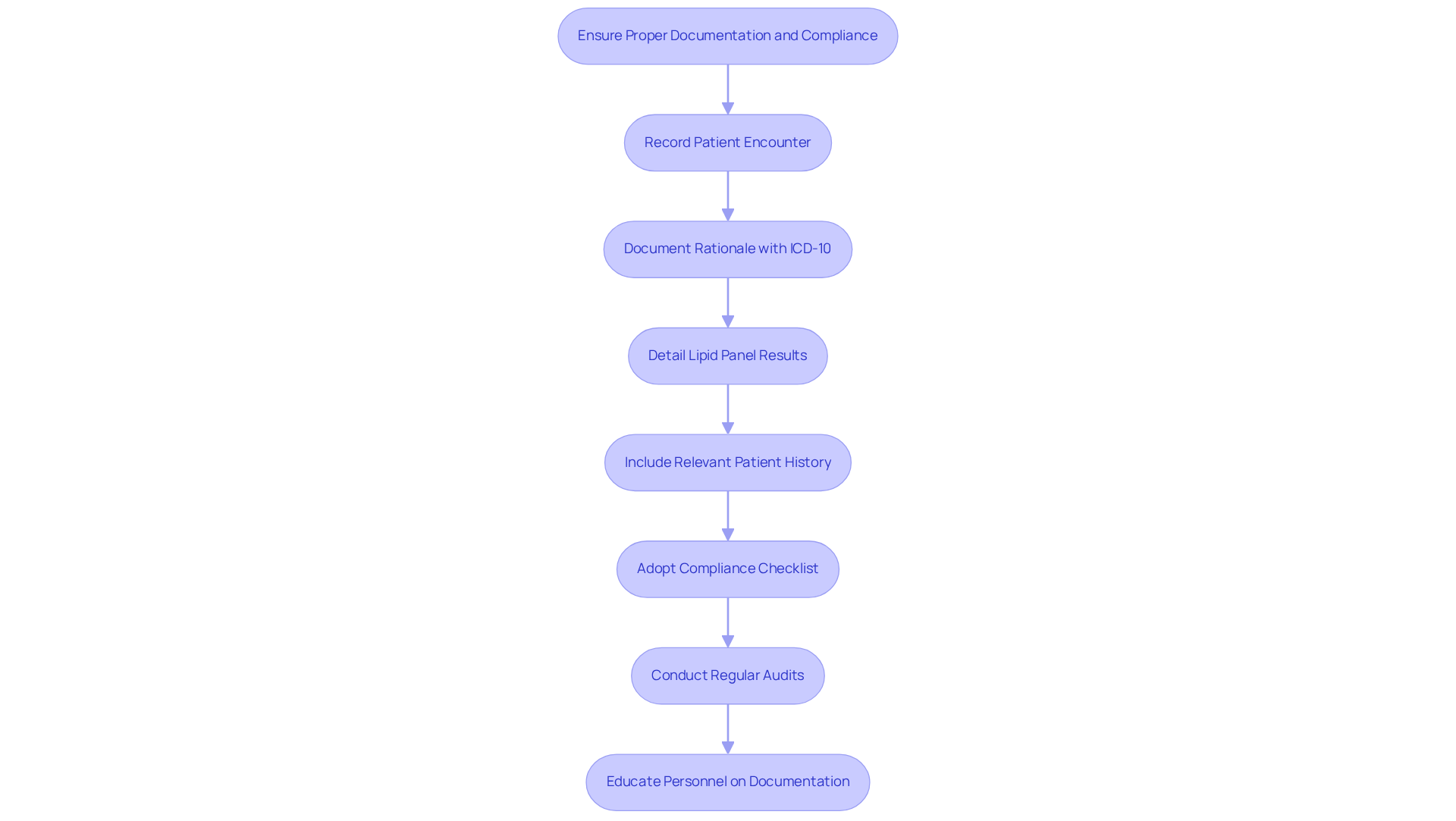
Accurate documentation is crucial for the successful billing of lipid panels. Clinics must ensure that every patient encounter is meticulously recorded. This includes:
- The rationale for conducting the lipid panel test, which must correspond with the ICD-10 code utilized.
- Comprehensive results of the lipid panel, detailing total cholesterol, LDL, HDL, and triglycerides.
- Relevant patient history that substantiates the medical necessity of the test.
To enhance compliance and minimize claim denials, clinics should adopt a compliance checklist that aligns with payer requirements. This checklist should include primary source verification and HIPAA-compliant document handling. Conducting regular audits of documentation practices can identify areas needing improvement, thereby reducing the risk of denials. Furthermore, educating personnel on the importance of documentation and compliance is essential for enhancing the clinic’s revenue efficiency. As compliance specialists emphasize, “Clear documentation safeguards revenue and enhances compliance in the revenue cycle,” underscoring the significance of meticulous record-keeping in healthcare invoicing. With outpatient denials having increased by 26% from 2024 to 2025, the urgency for precise documentation cannot be overstated.
Healthcare Partners Consulting (HPC) highlights the necessity of maintaining up-to-date knowledge of payer-specific guidelines and managing re-credentialing processes to ensure providers remain compliant. A case study of Urgent Care Center XYZ illustrates this point; after improving their invoicing processes and compliance measures, they experienced a significant decrease in denial of requests and enhanced operational confidence. Additionally, clinics must prepare for the forthcoming requirement of electronic prior authorization systems, which will further influence payment practices in 2026.
Optimize Billing Processes for Lipid Panels
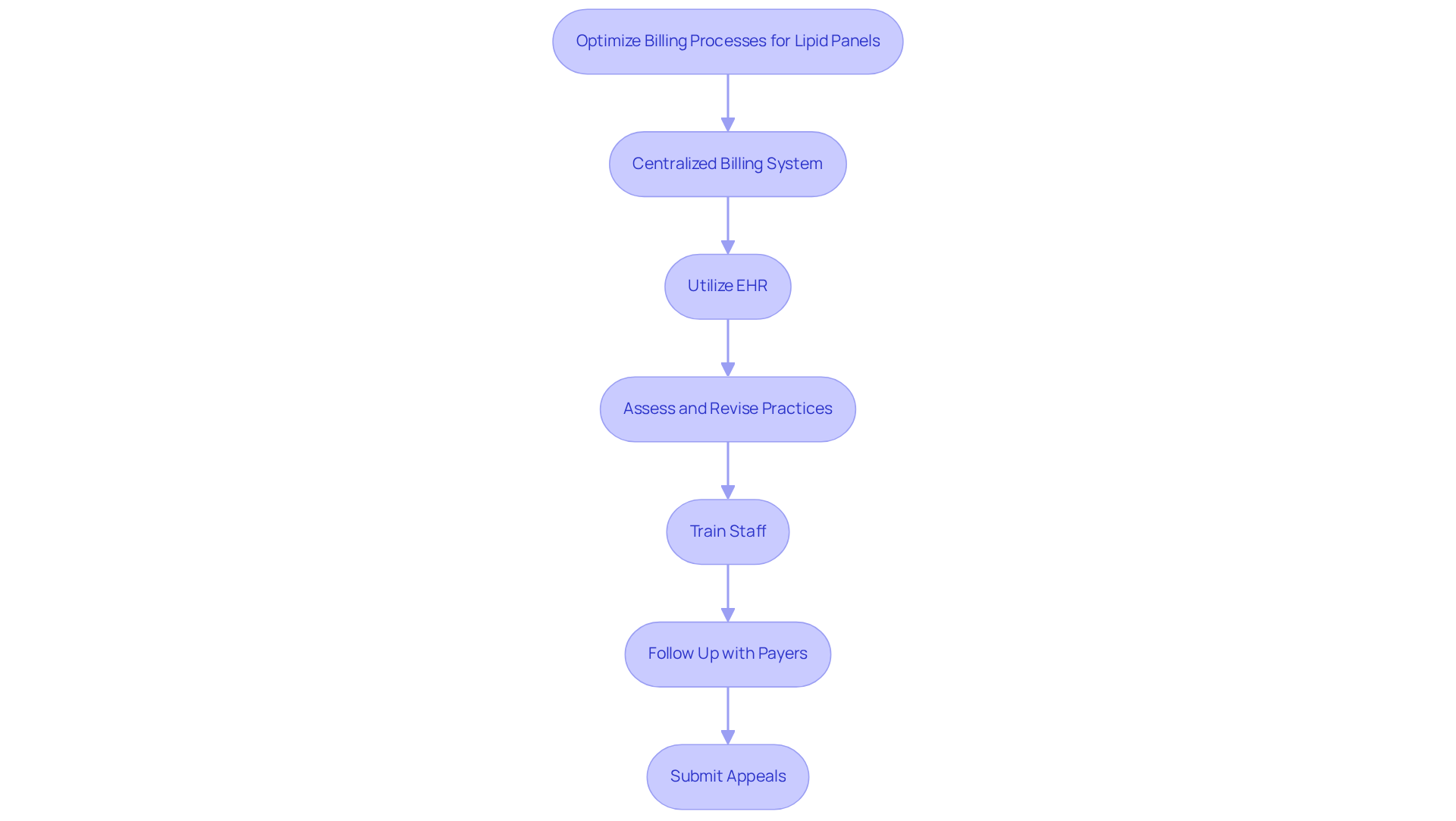
To optimize billing processes for lipid panels, clinics should consider several key strategies:
- Implement a centralized billing system: A centralized system streamlines the billing process, ensuring that all claims are submitted accurately and promptly. This is crucial for protecting practice revenue.
- Utilize electronic health records (EHR): EHR systems facilitate better documentation and classification by integrating clinical data with payment processes. This integration reduces errors and enhances payment accuracy.
- Consistently assess and revise programming practices: Staying informed about modifications in the ICD 10 code for lipid panel and payer requirements is essential for ensuring compliance and maximizing revenue. This vigilance can assist in minimizing denials.
- Train staff on billing best practices: Regular training sessions enhance staff knowledge and skills, leading to improved accuracy in coding and billing. This ultimately reduces administrative burdens.
- Proactively follow up with payers: Regular follow-ups on unpaid or underpaid invoices help recover lost revenue and ensure timely payments.
- Submit appeals for rejected requests: Establishing a structured process for appealing denied requests can significantly enhance recovery rates and lessen the impact of rejections on revenue.
By adopting these practices, clinics can enhance their billing efficiency, reduce the denial of requests, and ultimately improve their revenue cycle management. Furthermore, partnering with Healthcare Partners Consulting can provide expert denial management and recovery solutions, further streamlining claims and enhancing revenue for healthcare providers.
Conclusion
Mastering the ICD-10 code for lipid panels is essential for clinics seeking to improve their billing processes and secure accurate compensation for services rendered. A thorough understanding of ICD-10 coding fundamentals not only aids in proper documentation and compliance but also plays a significant role in the revenue cycle management of healthcare practices. By adopting effective coding practices, clinics can reduce claim denials and enhance their financial outcomes.
This article underscores the necessity of precise coding, comprehensive documentation, and continuous staff training. Key ICD-10 codes, including Z13.220 for screening lipoid disorders and E78 codes for dyslipidemia, are critical for appropriate billing. Furthermore, implementing strategies such as centralized billing systems and electronic health records can streamline operations and alleviate administrative burdens. Regular audits and compliance checklists are vital in ensuring that clinics uphold high standards in documentation, ultimately protecting revenue.
In summary, the importance of accurate ICD-10 coding for lipid panels transcends mere compliance; it is a fundamental component of the financial health of clinics. By emphasizing education, leveraging effective tools, and collaborating with experts like Healthcare Partners Consulting, clinics can adeptly navigate the complexities of billing. Embracing these best practices not only improves operational efficiency but also enhances patient care and outcomes.
Frequently Asked Questions
What is the importance of ICD-10 coding in healthcare?
ICD-10 coding is essential for healthcare financing, as it classifies diagnoses into specific identifiers needed for billing purposes.
What is the ICD-10 code for lipid panels?
The ICD-10 code for lipid panels includes identifiers like Z13.220, which is used for screening lipoid disorders in asymptomatic individuals.
Why is understanding the structure of ICD-10 codes important for clinics?
Understanding the structure of ICD-10 codes, which includes categories, subcategories, and specific codes, is critical for accurately documenting patient encounters and justifying the medical necessity of tests.
What are the consequences of inadequate programming in ICD-10 coding?
Inadequate programming can lead to significant financial repercussions, including potential losses for hospitals, which could amount to up to £29,000 due to incorrect patient classification.
How can clinics improve their revenue cycle management related to ICD-10 coding?
Clinics can improve their revenue cycle management by prioritizing training and resources for successful implementation of ICD-10 codes for lipid panel billing.
What services does Healthcare Partners Consulting provide to assist clinics?
Healthcare Partners Consulting offers proactive follow-up on unpaid claims, appeal submissions for denied requests, and coordination of structured payment plans to enhance revenue cycle management.
How does precise programming benefit clinics?
Precise programming streamlines invoicing processes, enhances compliance with insurance standards, and reduces the likelihood of claim rejections, ultimately improving cash flow and fostering sustainable growth.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting