Revenue Cycle Management Best Practices
Master Medication Injection CPT Code Billing: Best Practices for Clinics

Introduction
Understanding the complexities of CPT coding is crucial for clinics that seek to optimize their billing processes and enhance revenue streams. The medication injection CPT code, specifically 96372, is integral to ensuring accurate invoicing and compliance with healthcare regulations.
As the landscape of medical billing continues to evolve, clinics encounter challenges such as:
- Frequent coding errors
- Insufficient documentation
These challenges can result in significant financial losses. To navigate these complexities effectively, healthcare providers must employ strategic approaches that safeguard their revenue while maintaining a commitment to quality patient care.
Understand the Basics of CPT Coding for Medication Injections
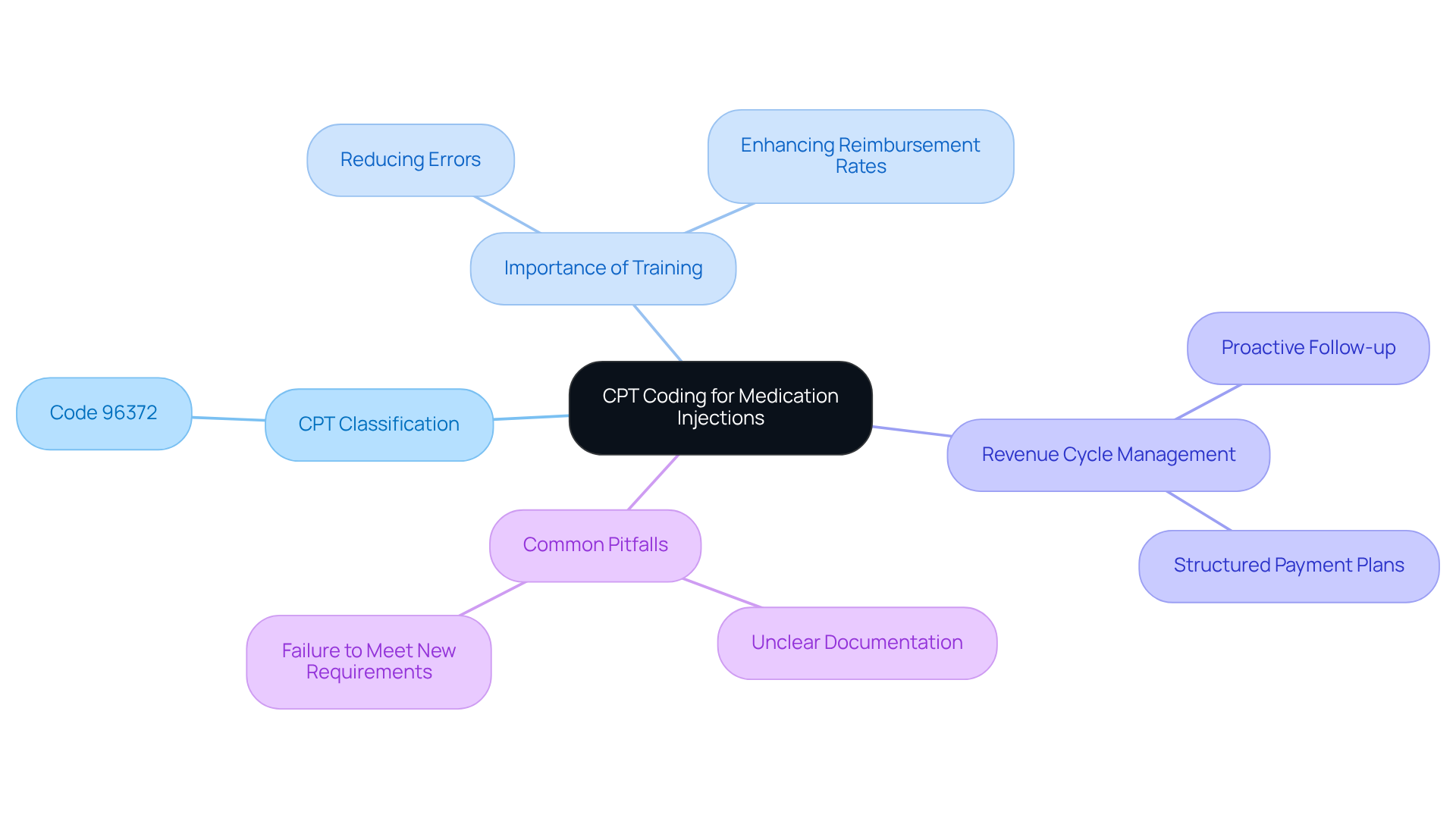
CPT (Current Procedural Terminology) classification serves as a standardized framework for detailing medical, surgical, and diagnostic services. This framework is essential for accurate invoicing and reimbursement within the healthcare sector. Specifically, the medication injection CPT code is designated as 96372 for therapeutic, prophylactic, or diagnostic injections administered subcutaneously or intramuscularly.
Understanding the hierarchy of codes and the specific requirements associated with each is crucial for optimizing revenue cycle management in clinics. Training all financial personnel in these fundamental principles can significantly reduce errors and enhance reimbursement rates. As healthcare billing specialists emphasize, effective CPT classification streamlines the billing process and ensures compliance with evolving regulations, ultimately supporting the financial sustainability of practices.
Healthcare Partners Consulting underscores the importance of proactive follow-up with payers regarding unpaid or underpaid invoices, which is vital for maximizing revenue. Furthermore, implementing structured payment plans can enhance cash flow. Real-world examples indicate that facilities adopting robust CPT training and techniques to prevent modifier errors – such as using internal checklists and reviewing high-risk claims – have seen substantial improvements in their revenue cycle management. This underscores the necessity of staying current with coding practices, particularly as we approach 2026 and beyond.
Moreover, healthcare facilities must be aware of potential pitfalls in CPT coding practices, including unclear documentation and failure to meet new requirements. Recognizing these issues is essential to avoid common errors that could adversely impact revenue.
Implement Effective Strategies for Billing CPT Code 96372
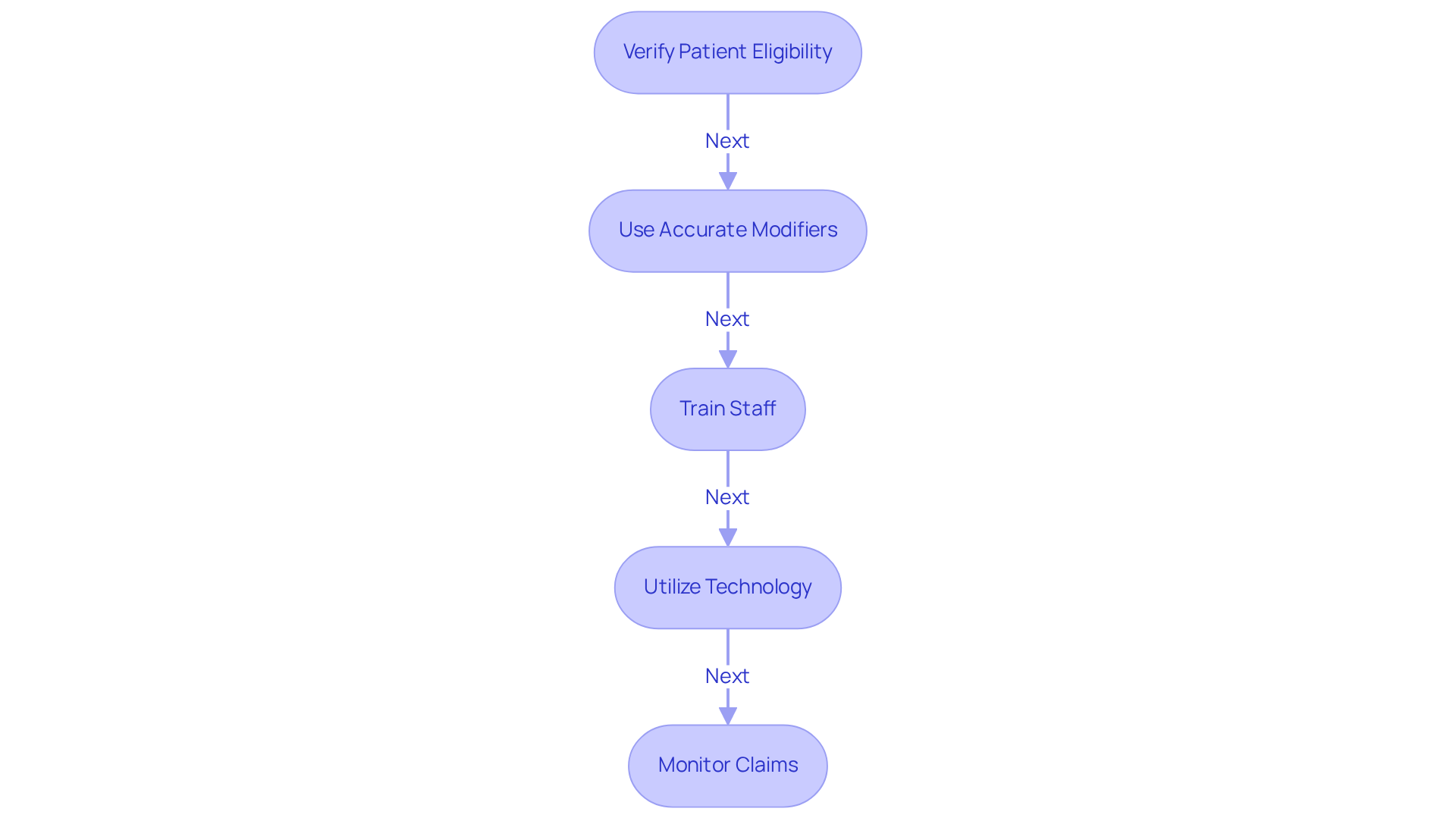
To effectively bill CPT code 96372, clinics should adopt several key strategies:
- Verify Patient Eligibility: Before administering injections, it is essential to confirm the patient’s insurance coverage and benefits for the specific medication. This step is crucial, especially since, starting July 1, 2026, Medi-Cal Rx will deny pharmacy claims if the prescribing provider is not enrolled. Verifying eligibility is vital to avoid claim denials.
- Use Accurate Modifiers: It is important to apply appropriate modifiers, such as modifier 25, when charging for additional services rendered on the same day. This practice ensures that the invoicing accurately reflects the distinct nature of the services, which is critical for adequate reimbursement.
- Train Staff: Regular training sessions for invoicing personnel on the latest coding updates and payer requirements can significantly reduce errors. A thorough understanding of the nuances of the medication injection CPT code 96372 and its documentation requirements is essential for compliance and minimizing audit risks.
- Utilize Technology: Implementing invoicing software that integrates with electronic health records (EHR) can streamline the payment process. This integration enhances billing efficiency by reducing manual entry errors and ensuring that all necessary documentation is readily available.
- Monitor Claims: Regularly reviewing submitted claims for denials and promptly following up to resolve issues is crucial. Conducting regular internal audits can help identify issues before they escalate, ensuring that facilities maintain a healthy cash flow.
By employing these strategies, clinics can enhance their payment efficiency and ensure prompt payments, ultimately supporting their financial sustainability.
Ensure Accurate Documentation and Compliance for Successful Billing
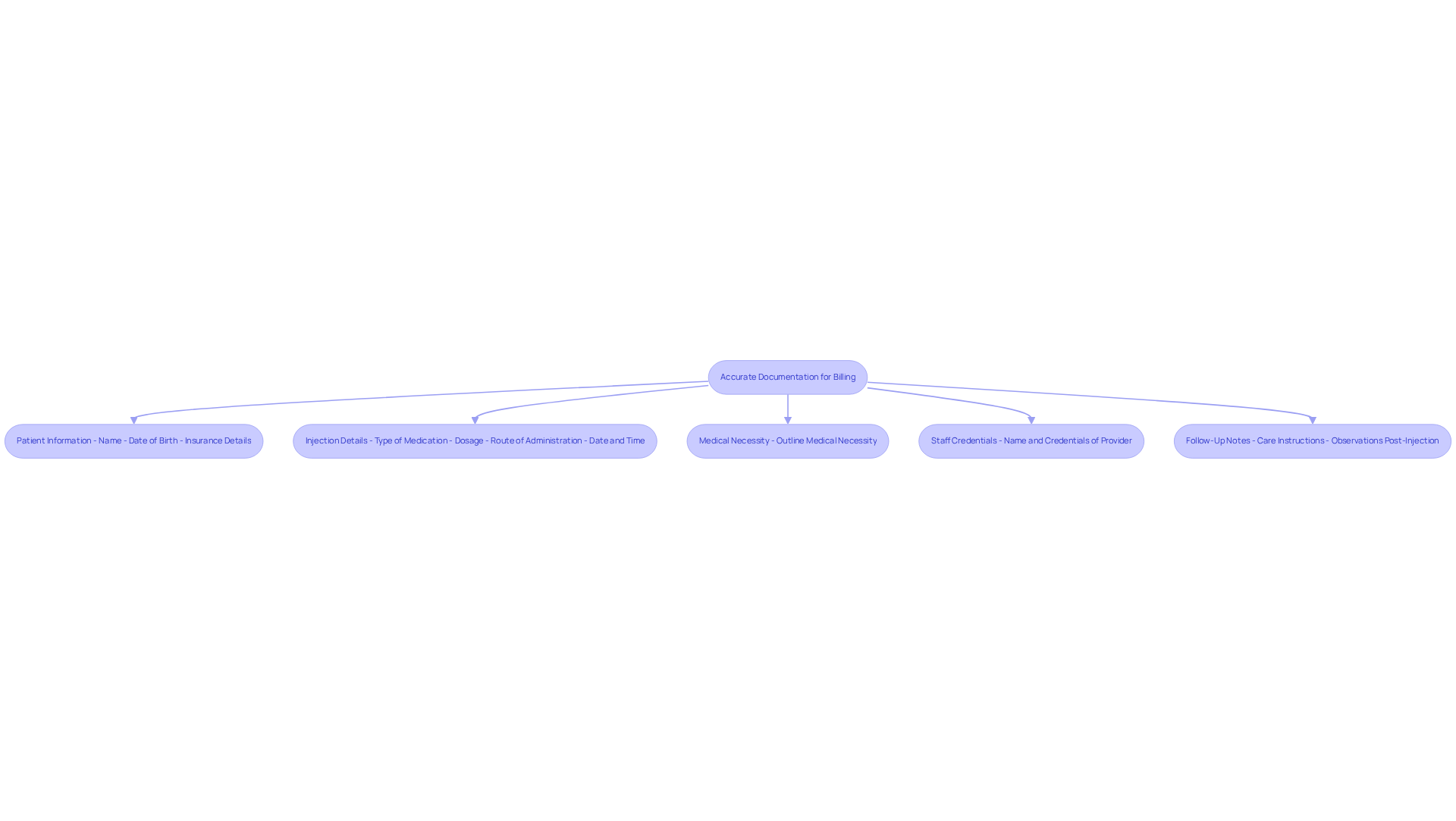
Accurate documentation is crucial for the successful billing of the medication injection CPT code 96372. Clinics must consistently document the following elements:
- Patient Information: This includes the patient’s name, date of birth, and insurance details.
- Injection Details: It is essential to document the type of medication administered, dosage, route of administration, and the date and time of the injection.
- Medical Necessity: Clearly outlining the medical necessity for the injection in the patient’s record is vital to support the request. Insufficient documentation is a primary reason for denials, making this step critical.
- Staff Credentials: The name and credentials of the healthcare provider administering the injection should be recorded.
- Follow-Up Notes: Any follow-up care instructions or observations post-injection must be included.
By maintaining thorough and precise records, healthcare facilities can significantly reduce the likelihood of denial and ensure adherence to payer requirements, particularly regarding the medication injection CPT code. Compliance officers emphasize that comprehensive documentation of medical necessity is essential for substantiating requests and safeguarding revenue, particularly amid heightened scrutiny and audit risks in the healthcare environment.
Additionally, Healthcare Partners Consulting (HPC) aids healthcare facilities in adhering to payer-specific guidelines for credentialing and re-credentialing, ensuring providers remain compliant with the latest regulations. HPC’s team also reviews and corrects coding issues prior to claims submission, which helps mitigate errors and enhances the precision of payment processes. This proactive approach not only facilitates timely reimbursements but also protects against compliance risks, allowing healthcare facilities to concentrate on delivering quality care.
Avoid Common Pitfalls in Medication Injection Billing
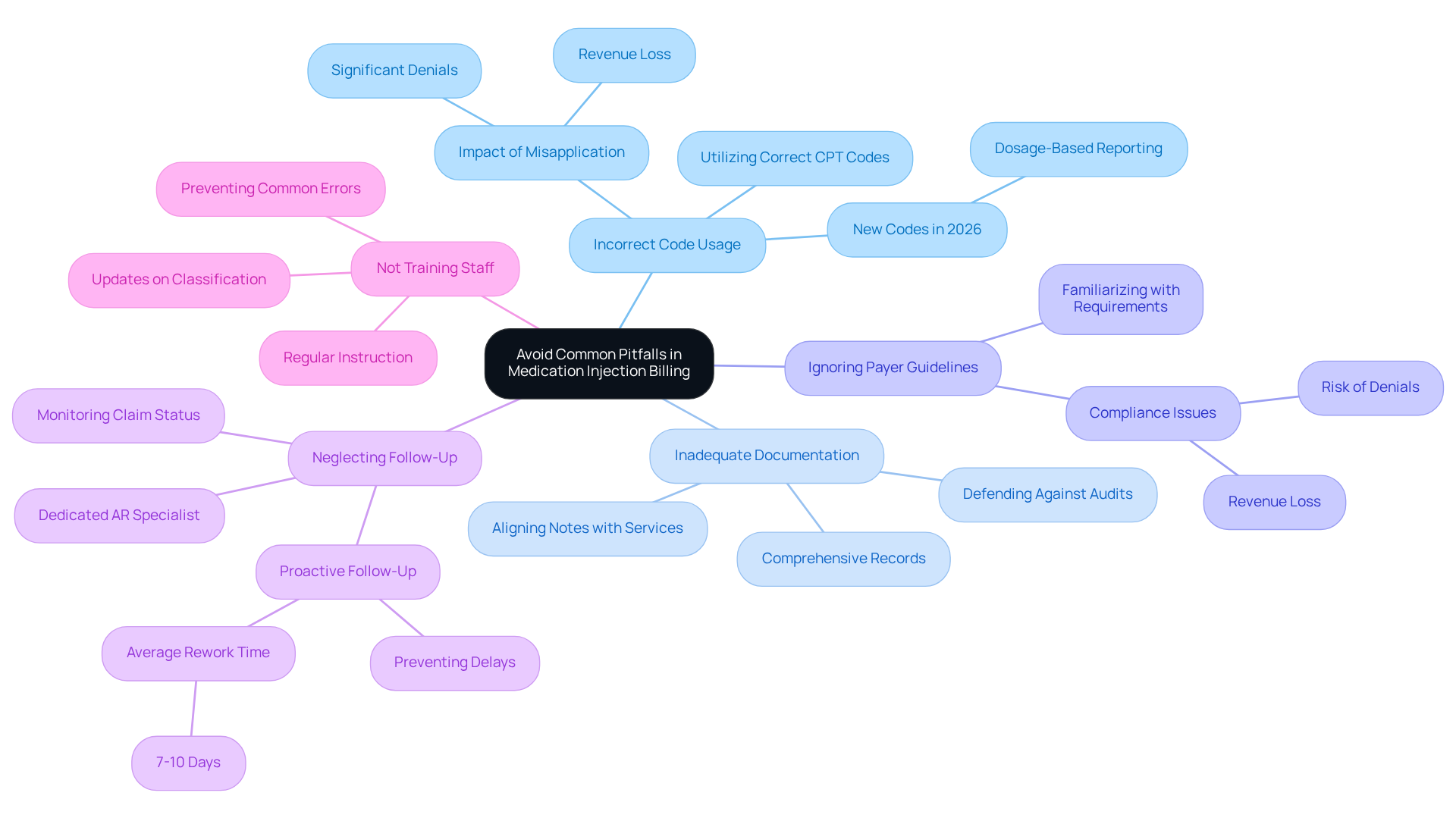
To avoid common pitfalls in billing for medication injections, clinics should focus on several critical issues:
- Incorrect code usage: Utilizing the correct medication injection CPT code for the specific injection administered is essential. Misapplication can lead to significant denials, adversely affecting revenue. The introduction of new medication injection CPT codes for injectable drugs in 2026, which are tied to strict dosage-based reporting, underscores the necessity of accurate coding.
- Inadequate Documentation: Comprehensive documentation is vital. Failing to record all essential details can result in rejections of requests. Clear notes that align with the services billed are crucial for defending against audits and ensuring compliance with payer requirements.
- Ignoring Payer Guidelines: Each payer may have specific requirements for billing injections. Familiarizing oneself with these guidelines is essential to avoid compliance issues that could lead to denials. Practices that neglect these guidelines risk losing substantial revenue due to incorrect submissions.
- Neglecting Follow-Up: After submitting requests, actively monitoring their status is important. Proactive follow-up with payers on unpaid or underpaid requests can prevent delays in reimbursement. The average time to rework a denied claim is 7-10 days, highlighting the importance of a proactive approach to denial management to enhance cash flow. Assigning a dedicated AR specialist to your account can ensure timely follow-up and resolution of issues.
- Not Training Staff: Regular instruction on invoicing methods and updates in classification is crucial. Ensuring that staff are well-informed about the latest coding changes and payer requirements can prevent many common errors. Clinics that prioritize compliance can safeguard their revenue and are better positioned to maintain compliance and optimize their revenue cycle.
By proactively addressing these pitfalls and leveraging comprehensive accounts receivable management solutions, including monthly reconciliation and structured payment plans, clinics can enhance their billing accuracy and improve their overall revenue cycle, ultimately leading to better financial health and patient care.
Conclusion
Mastering the complexities of CPT code billing for medication injections is crucial for clinics seeking to optimize their revenue cycle management. By implementing effective practices surrounding CPT code 96372, healthcare facilities can improve their billing efficiency and ensure timely reimbursements, thereby supporting their financial sustainability.
Key strategies encompass:
- Verifying patient eligibility
- Employing accurate modifiers
- Maintaining comprehensive documentation of all necessary details
Regular staff training and leveraging technology to streamline billing processes further aid in minimizing errors and enhancing compliance. Moreover, proactive follow-up on claims and awareness of common pitfalls-such as incorrect code usage and insufficient documentation-are essential for safeguarding revenue and preventing costly denials.
In summary, prioritizing effective billing practices transcends mere compliance; it is a fundamental aspect of delivering quality patient care. Clinics that invest in training, technology, and thorough documentation will not only bolster their financial health but also enhance patient satisfaction. By embracing these strategies, healthcare providers can concentrate on what truly matters: delivering exceptional care while sustaining a robust financial foundation.
Frequently Asked Questions
What is CPT coding and why is it important?
CPT (Current Procedural Terminology) coding serves as a standardized framework for detailing medical, surgical, and diagnostic services, which is essential for accurate invoicing and reimbursement in the healthcare sector.
What is the CPT code for medication injections?
The CPT code for therapeutic, prophylactic, or diagnostic injections administered subcutaneously or intramuscularly is 96372.
Why is understanding CPT coding important for clinics?
Understanding CPT coding is crucial for optimizing revenue cycle management, reducing errors, and enhancing reimbursement rates within clinics.
How can training financial personnel in CPT coding principles benefit healthcare practices?
Training financial personnel in CPT coding principles can significantly reduce errors and improve reimbursement rates, thereby supporting the financial sustainability of healthcare practices.
What role does proactive follow-up with payers play in revenue maximization?
Proactive follow-up with payers regarding unpaid or underpaid invoices is vital for maximizing revenue in healthcare facilities.
How can structured payment plans impact cash flow in healthcare facilities?
Implementing structured payment plans can enhance cash flow within healthcare facilities.
What are some effective techniques for improving revenue cycle management?
Effective techniques include robust CPT training, using internal checklists, and reviewing high-risk claims to prevent modifier errors.
What potential pitfalls should healthcare facilities be aware of in CPT coding practices?
Healthcare facilities should be aware of potential pitfalls such as unclear documentation and failure to meet new requirements, which can lead to common errors that adversely impact revenue.
Why is it important to stay current with coding practices?
Staying current with coding practices is essential to avoid errors and ensure compliance with evolving regulations, especially as the healthcare environment changes leading into 2026 and beyond.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting