General
Master the Prescription Prior Authorization Process in 4 Steps

Introduction
Navigating the prescription prior authorization process presents significant challenges that can adversely affect patient care. Understanding this critical mechanism not only helps healthcare providers ensure appropriate treatment but also enhances operational efficiency and patient satisfaction. The ongoing challenge is for providers to effectively manage this complex process to minimize delays and improve outcomes. This article presents a structured approach to streamline prior authorization requests, address common challenges, and utilize technology for improved management, thereby enhancing patient care and operational efficiency.
Understand Prior Authorization: Definition and Importance
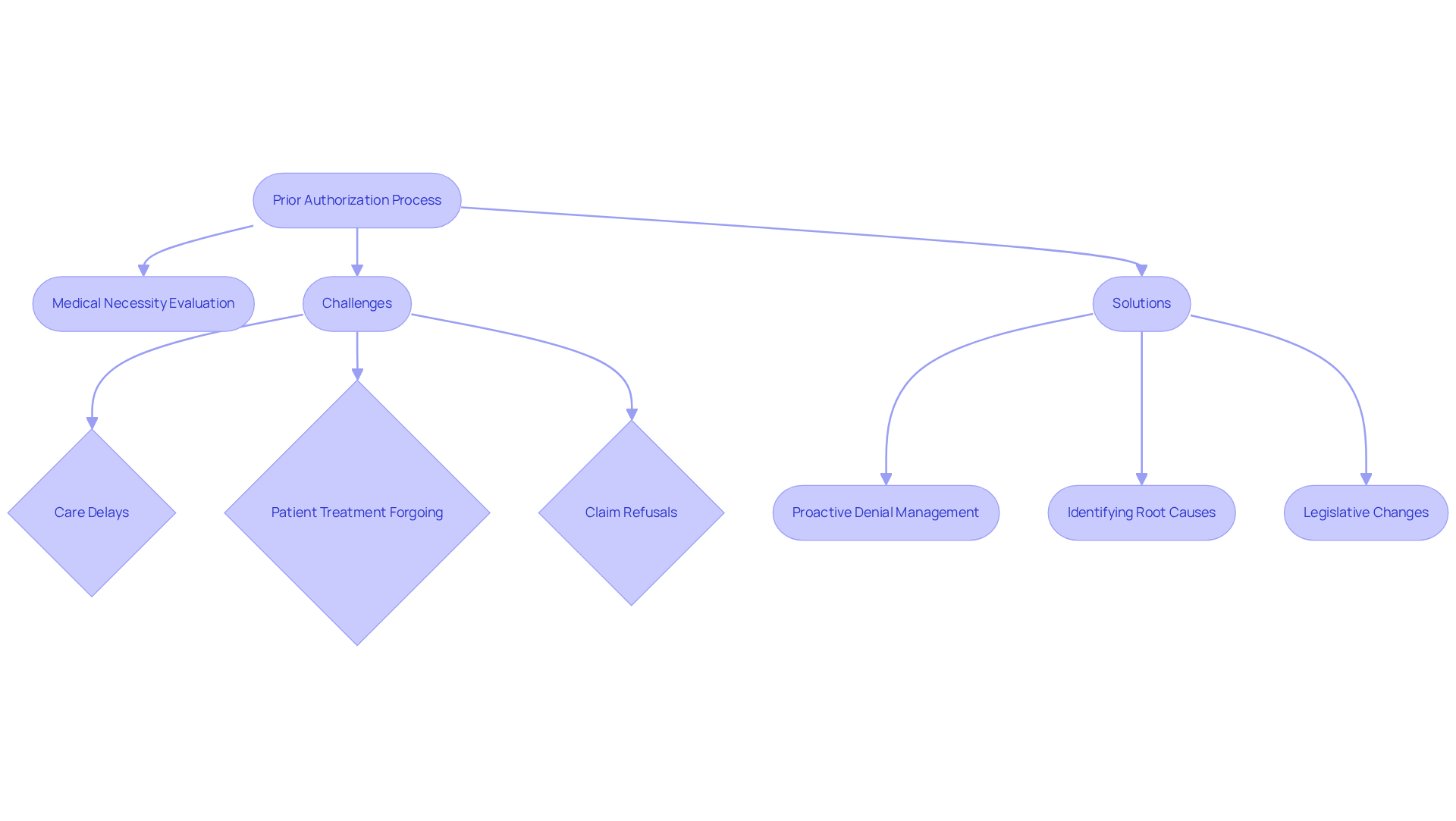
The prescription prior authorization process is a critical mechanism that health insurance firms use to evaluate the medical necessity of treatments before they are administered. This step is essential for controlling healthcare costs and ensuring that patients receive appropriate care. A recent survey indicated a significant challenge in timely patient care, revealing that 93% of doctors faced care delays due to previous approvals, with 82% noting that patients occasionally forgo suggested treatments. Consequently, these delays can compromise patient health and satisfaction, highlighting the need for healthcare providers to grasp the intricacies of the PA process.
Healthcare Partners Consulting specializes in addressing various claim refusals, including:
- Pre-approval refusals
- Coding issues
- Timely filing problems
- Medical necessity refusals
These are particularly relevant in this context. Their proactive denial management solutions focus on identifying the root causes of these denials and implementing strategies to reduce future occurrences.
The significance of the prescription prior authorization process extends beyond cost control; it plays a vital role in preventing unnecessary procedures and ensuring that prescribed treatments adhere to evidence-based guidelines. Recent legislative changes, such as the Improving Seniors’ Timely Access to Care Act, aim to simplify and accelerate the PA procedures, potentially enhancing patient outcomes by reducing administrative burdens. By mastering the PA procedure and leveraging the comprehensive denial management services provided by Healthcare Partners, healthcare providers can improve operational efficiency and ultimately enhance patient satisfaction. Ultimately, a thorough understanding of the PA process is essential for healthcare providers aiming to optimize patient care and operational efficiency.
Implement a Step-by-Step Process for Managing Requests
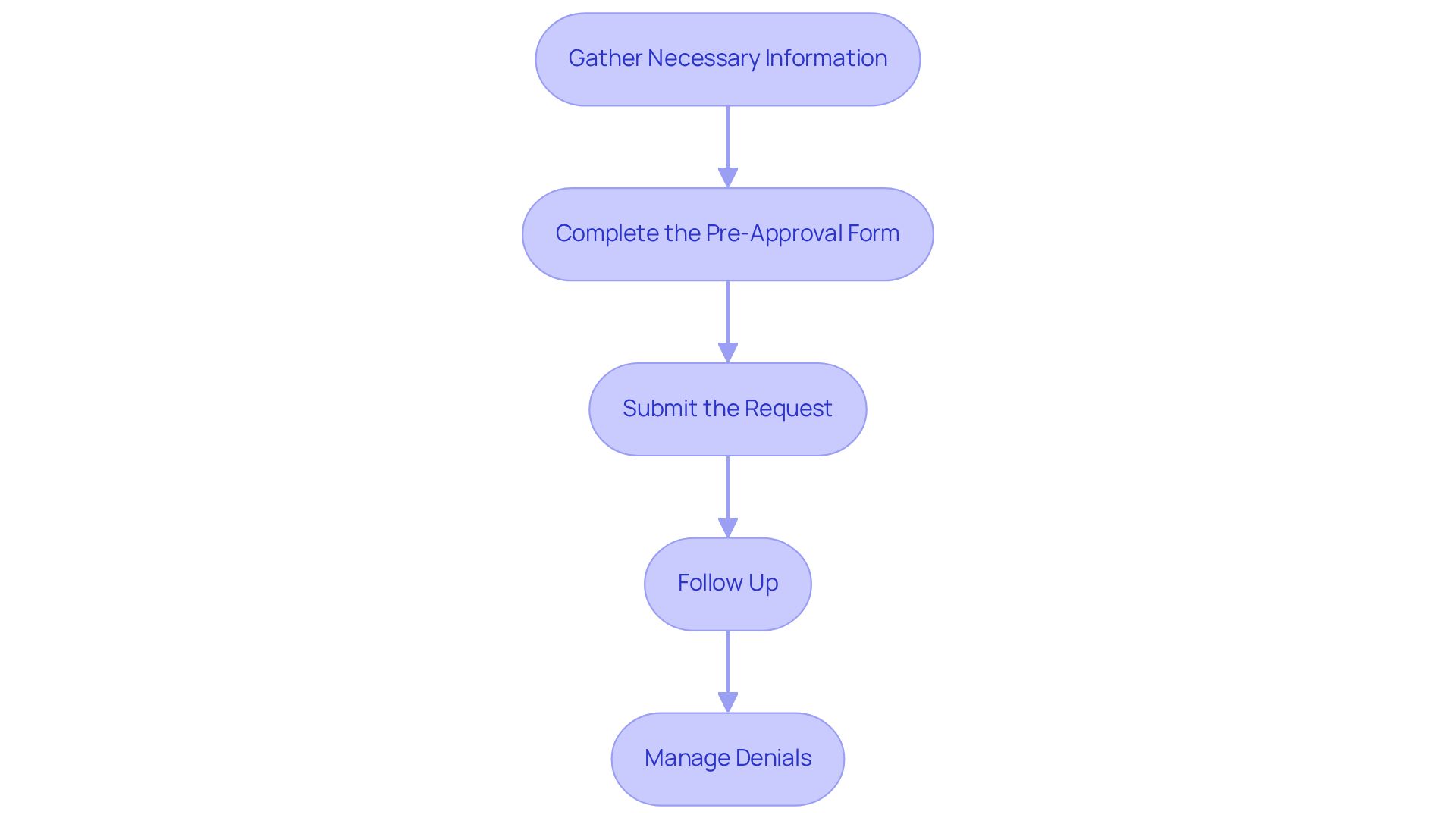
Navigating the prior approval process requires meticulous attention to detail to ensure timely access to necessary treatments.
- Gather Necessary Information: Begin by collecting all pertinent patient information, including insurance details, medical history, and the specific treatment or medication being requested. Accurate coding is crucial to prevent approval delays.
- Complete the Pre-Approval Form: Accurately fill out the pre-approval form, ensuring that all necessary documentation is included. This should encompass clinical notes and previous treatment records that substantiate the necessity of the requested service, as thorough documentation can significantly impact approval rates.
- Submit the Request: Send the completed prior approval request to the insurance company through the designated channel, whether electronically or via fax. Retain a copy of the submission for your records, as this can be crucial for follow-up and tracking.
- Follow Up: After submission, proactively follow up with the insurance company to confirm receipt of the request and to inquire about the expected timeline for a decision. Timely follow-ups expedite the process and reduce potential issues. Additionally, if approval is not granted, we assist with appeals and next steps to manage denials effectively.
Ultimately, a proactive approach in managing the approval process can significantly influence patient care outcomes.
Identify and Overcome Common Challenges in Prior Authorization
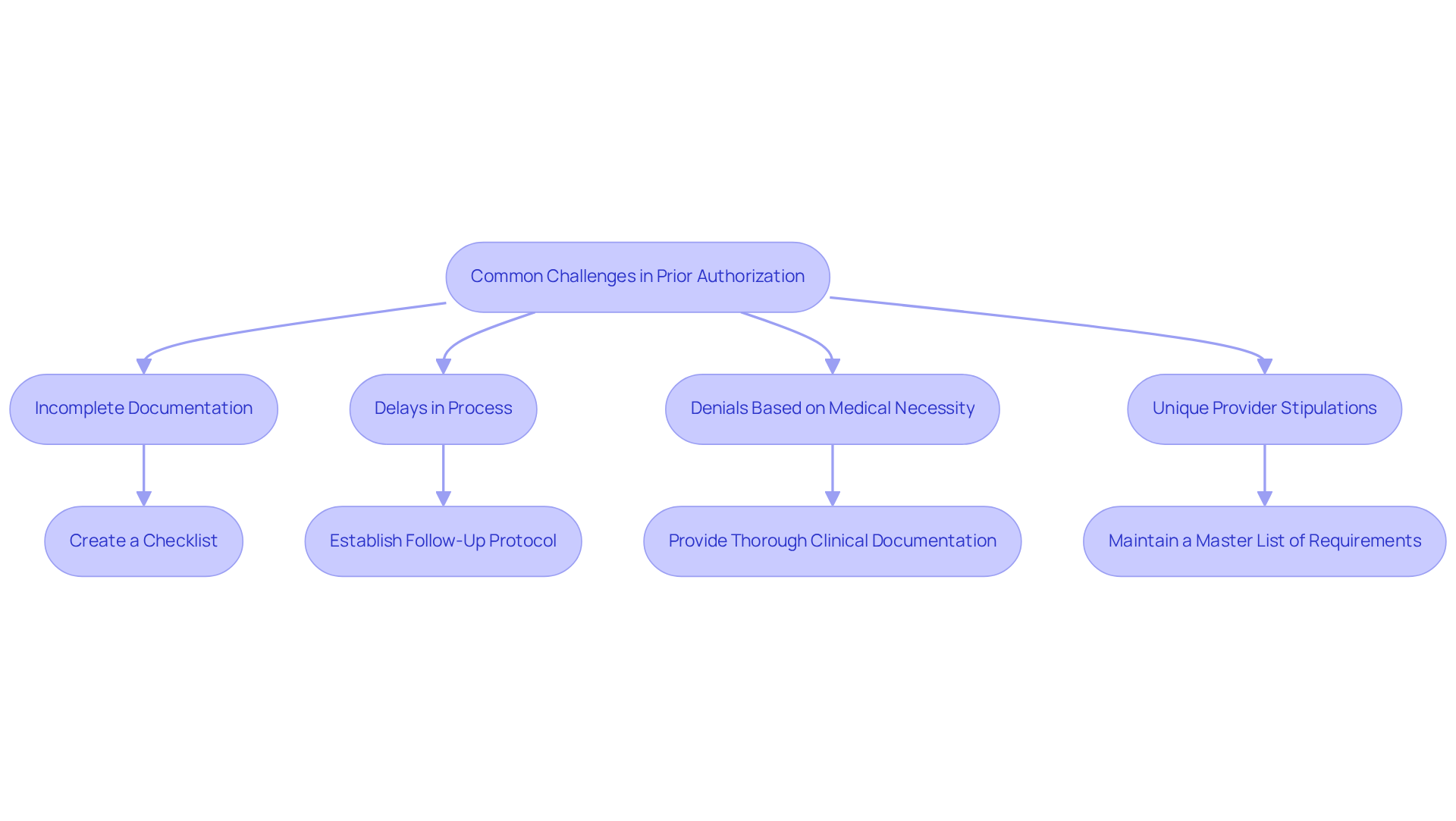
Incomplete documentation can significantly delay the prescription prior authorization process, which impacts patient care. To address this, create a comprehensive checklist of necessary information to ensure nothing is overlooked before submission. Healthcare Partners Consulting assists clinics in developing effective documentation practices to minimize errors.
Delays in the prescription prior authorization process can hinder timely patient care. To lessen these delays, establish a follow-up protocol that includes frequent status checks on requests and maintains open communication with insurance representatives. Utilizing Healthcare Partners Consulting’s virtual scheduling services can streamline communication and improve response times.
Insurers often deny requests based on perceived medical necessity. To counteract this, it is crucial to provide thorough clinical documentation that clearly articulates the patient’s condition and justifies the requested treatment, thereby strengthening the case for approval. Healthcare Partners Consulting assists in preparing clinical documentation that meets insurer requirements.
Each provider has unique stipulations for advance approval, complicating the prescription prior authorization process. To streamline operations, maintain a master list of payer-specific requirements to ensure compliance and facilitate smoother submissions across different insurers. Healthcare Partners Consulting helps clinics stay updated on these requirements and implement best practices for compliance. Addressing these issues is essential for enhancing patient care and operational efficiency.
Leverage Technology to Streamline Prior Authorization Workflows
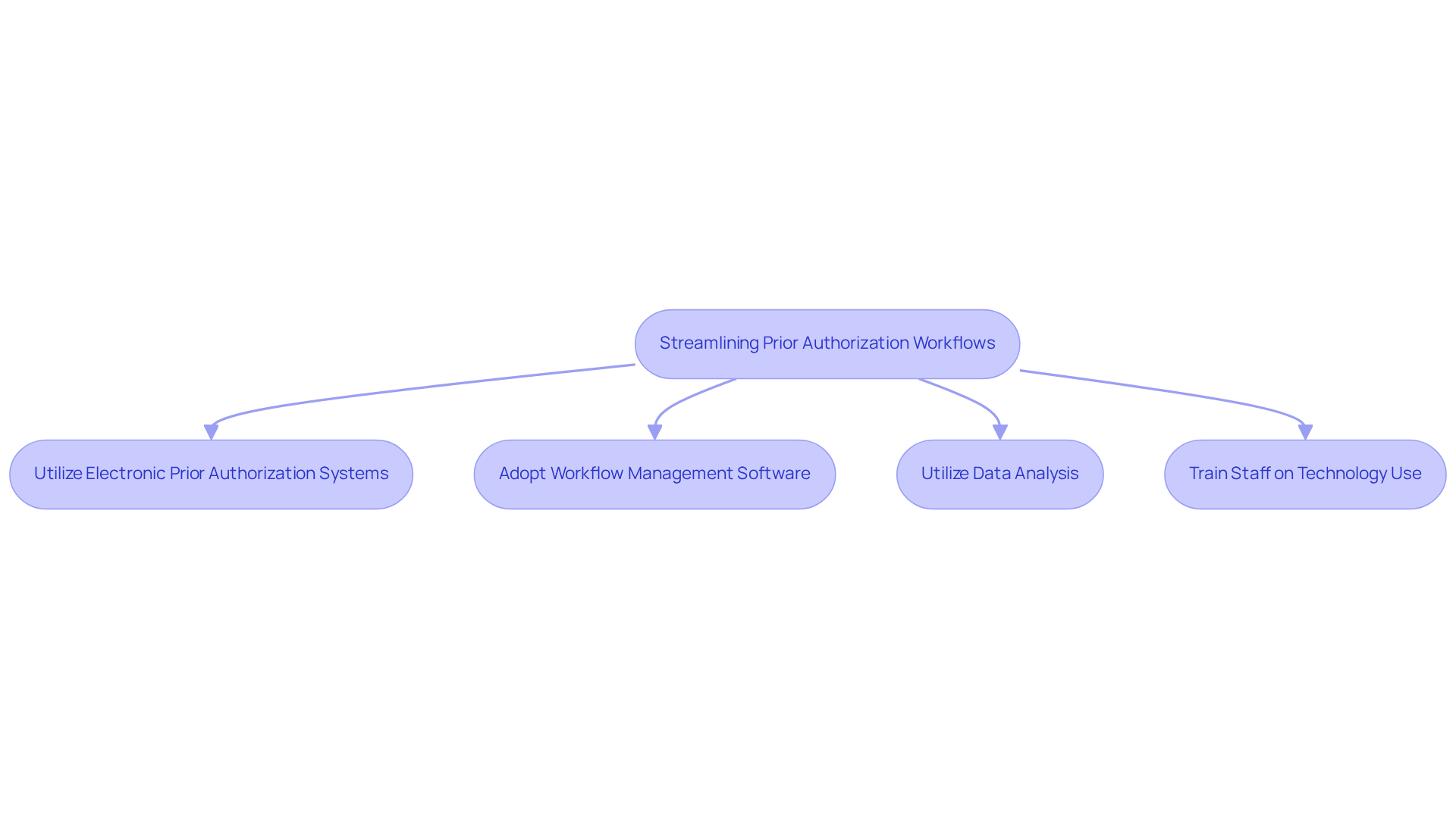
The complexities of the prescription prior authorization process often hinder efficient patient care, necessitating innovative solutions.
- Utilize Electronic Prior Authorization (ePA) Systems: Implement ePA systems that seamlessly integrate with your electronic health records (EHR). These systems automate submission and tracking of approval requests, reducing manual errors and accelerating the process. By 2027, all payers will be required to connect with providers through electronic systems, moving away from outdated fax-based workflows.
- Adopt Workflow Management Software: Invest in comprehensive software solutions designed to manage the entire initial approval workflow, from submission to follow-up. These tools provide reminders and track request statuses, preventing any oversight. The integration of such systems can enhance communication and reduce delays, ultimately improving patient care.
- Utilize Data Analysis: Leverage data analysis to identify trends in previous approval requests and refusals. This information can help refine your approach, allowing you to proactively address common issues that lead to denials. A survey indicated that 82% of physicians report patients discontinuing recommended treatment due to approval obstacles, highlighting the significance of data-driven strategies in enhancing approval rates.
- Train Staff on Technology Use: Ensure that all staff members involved in the preceding approval process receive thorough training on the technology being utilized. This training should encompass effective system usage and troubleshooting common issues. Given that 95% of administrators view the prescription prior authorization process as a burden, equipping your team with the necessary skills can streamline operations and boost efficiency.
Without embracing these advancements, healthcare providers risk perpetuating inefficiencies that compromise patient outcomes.
Conclusion
Mastering the prescription prior authorization process is crucial for healthcare providers seeking to enhance both patient care and operational efficiency. Navigating the complexities of insurance requirements can be challenging for healthcare professionals. Mastering this process leads to improved patient outcomes and satisfaction.
Throughout the article, key strategies have been outlined, including:
- The importance of gathering accurate information
- Completing thorough documentation
- Maintaining proactive communication with insurance companies
Emphasizing the role of technology, such as electronic prior authorization systems and workflow management software, can significantly streamline operations and mitigate common challenges faced during the approval process. Additionally, leveraging data analysis to identify trends in approval requests can further enhance efficiency and effectiveness.
Mastering prior authorization is essential, as it directly impacts the ability to provide timely and necessary care to patients. Healthcare providers are encouraged to adopt these best practices and innovative technologies to overcome obstacles, reduce delays, and ultimately prioritize patient health. Implementing these strategies will empower healthcare providers to deliver timely care, ultimately transforming patient experiences.
Frequently Asked Questions
What is prior authorization in healthcare?
Prior authorization is a process used by health insurance firms to evaluate the medical necessity of treatments before they are administered, ensuring appropriate care and controlling healthcare costs.
Why is prior authorization important?
It is important because it helps prevent unnecessary procedures, ensures adherence to evidence-based guidelines, and controls healthcare costs, ultimately impacting patient health and satisfaction.
What challenges do healthcare providers face with prior authorization?
Healthcare providers face significant challenges, including care delays, with 93% of doctors reporting delays due to prior approvals and 82% noting that patients sometimes forgo suggested treatments.
What services does Healthcare Partners Consulting offer related to prior authorization?
Healthcare Partners Consulting specializes in addressing claim refusals related to pre-approval, coding issues, timely filing problems, and medical necessity refusals, focusing on proactive denial management solutions.
How can legislative changes impact the prior authorization process?
Legislative changes, such as the Improving Seniors’ Timely Access to Care Act, aim to simplify and accelerate prior authorization procedures, potentially enhancing patient outcomes by reducing administrative burdens.
How can healthcare providers improve their understanding of the prior authorization process?
Healthcare providers can improve their understanding by mastering the PA procedure and utilizing comprehensive denial management services to enhance operational efficiency and patient satisfaction.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting