Telehealth Billing Insights
Master Medical Revenue Cycle Management for Financial Success

Introduction
The medical revenue cycle management (RCM) process is critical to the financial health of healthcare organizations, as it directly connects patient care with fiscal sustainability. Mastering the essential steps of RCM enables healthcare providers to significantly enhance cash flow and operational efficiency. Navigating the intricate landscape of billing, coding, and compliance presents significant challenges for healthcare providers, often leading to costly errors and inefficiencies. This article presents best practices and innovative strategies that enhance financial performance and elevate the quality of patient care. Ultimately, effective RCM practices are essential not only for financial stability but also for ensuring high-quality patient care in an increasingly complex healthcare environment.
Outline the Essential Steps of Revenue Cycle Management
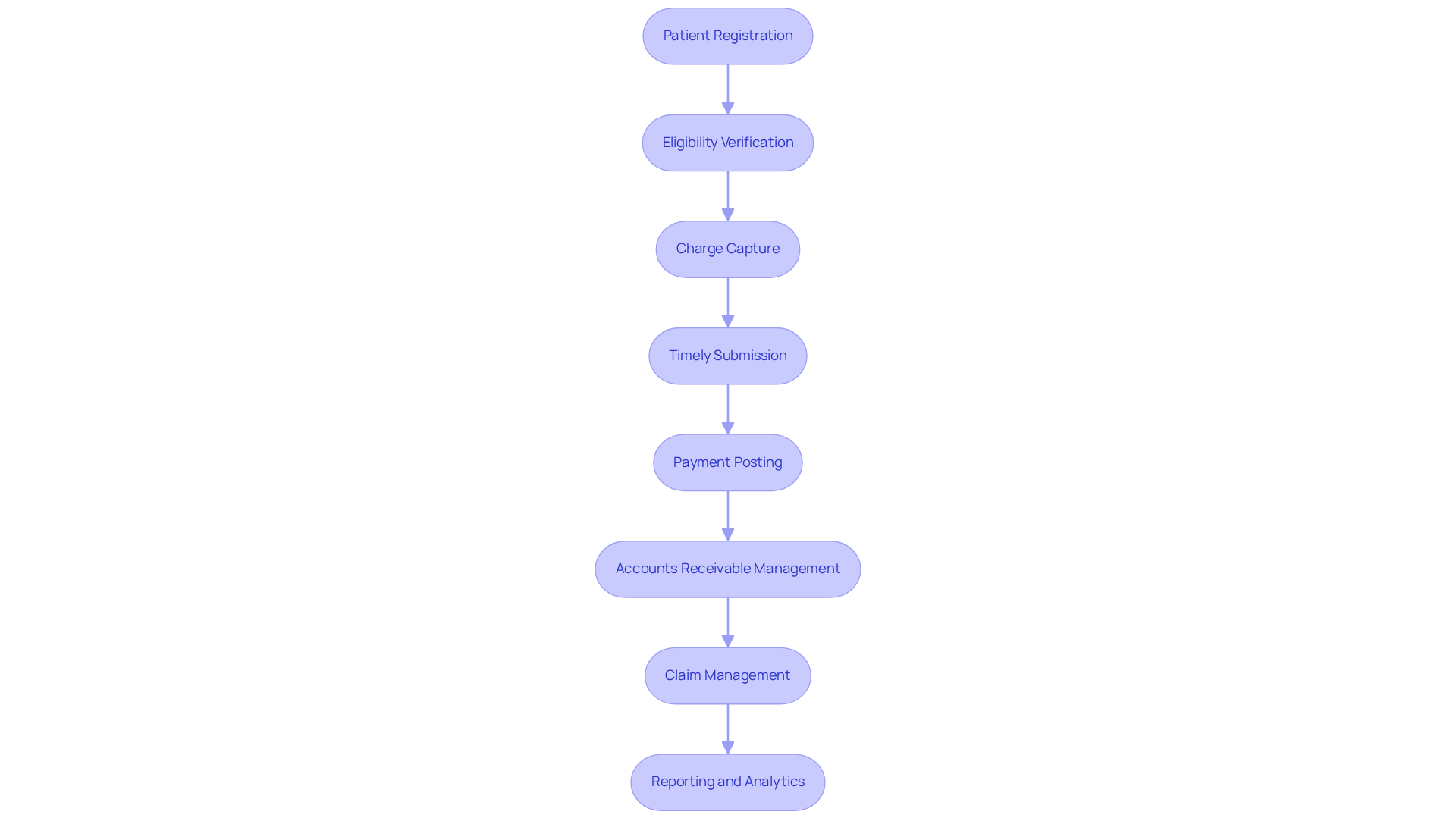
The medical revenue cycle management (RCM) is a critical process that directly impacts the financial viability of healthcare practices. The following steps outline the RCM process:
- Patient Registration: Accurate patient information collection at the first point of contact is vital. This includes verifying insurance details and demographic information to prevent billing errors later.
- Eligibility Verification: Confirming patient eligibility for services before treatment helps avoid claim denials. This step guarantees that the services offered are included by the patient’s insurance, which is essential for sustaining cash flow.
- Charge Capture: Accurately documenting all services rendered during patient visits is essential for billing. This involves coding procedures and diagnoses accurately to secure proper reimbursement, since errors can result in substantial revenue loss. Healthcare Partners Consulting emphasizes the importance of precise coding to prevent claim denials and enhance compliance.
- Timely Submission: Timely submission of requests to insurance companies is essential. Delays can lead to cash flow issues, so practices should aim for submissions within 30 to 40 days, significantly improving efficiency compared to the previous standard of three to six months.
- Payment Posting: Once payments are received, they must be posted accurately to patient accounts. This step helps maintain precise financial records and ensures that any discrepancies can be addressed quickly.
- Accounts Receivable Management: Monitoring outstanding demands and following up on unpaid invoices is crucial for maintaining cash flow. A systematic approach to managing accounts receivable can enhance financial stability. Healthcare Partners Consulting’s proactive workflows minimize rejections and enhance documentation, ensuring that no income slips away.
- Claim Management: Analyzing and addressing claim rejections swiftly can significantly influence income. Comprehending the causes for refusals enables establishments to modify their procedures and lessen future instances. Healthcare Partners Consulting provides comprehensive denial management services, handling coding, timely filing, prior authorization, and medical necessity denials to improve revenue cycle efficiency.
- Reporting and Analytics: Regularly reviewing financial reports and key performance indicators (KPIs) helps organizations identify trends and areas for improvement, ensuring ongoing financial health. Transparent reporting and regular audits are essential to this process, enabling organizations to remain informed and proactive.
As Andrew, a leader in financial cycle management, states, “Effective denial management practices are essential for maintaining income flow and ensuring financial sustainability in healthcare.” Ultimately, a robust strategy for managing the medical revenue cycle not only secures financial health but also enhances the quality of patient care delivered.
Optimize Each Step for Financial Sustainability
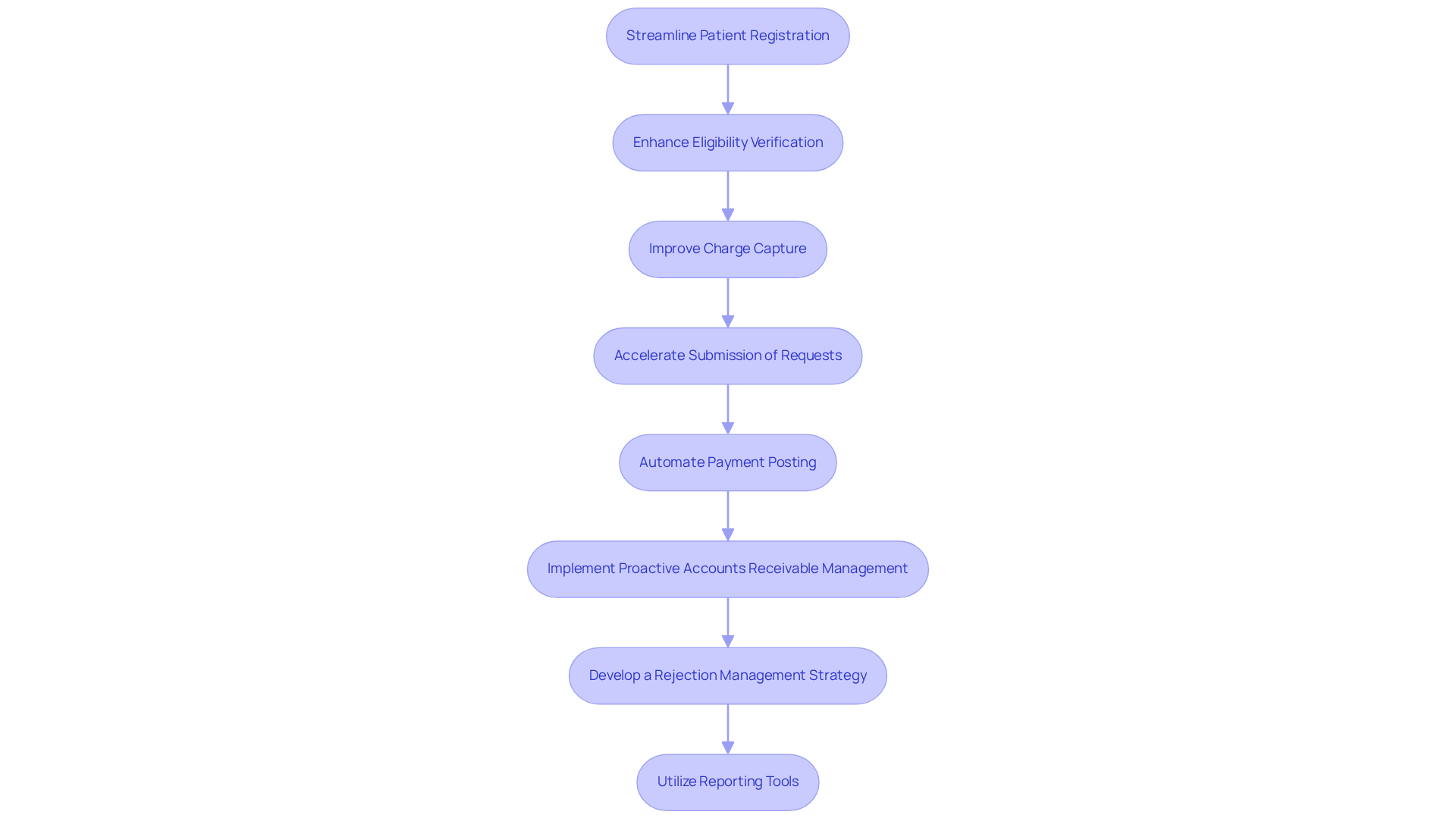
To achieve financial sustainability, healthcare providers must refine their revenue cycle management processes. Here are strategies for enhancing each phase:
- Streamline Patient Registration: Implement online registration forms to reduce wait times and improve data accuracy. Mistakes in data collection can lead to delays in processing and payments. Preparing personnel to gather comprehensive information can mitigate these issues, ensuring seamless processing and prompt payments.
- Enhance Eligibility Verification: Utilize automated tools to verify insurance eligibility in real-time. Automation can increase the frequency of eligibility checks by 11 times, significantly reducing the administrative burden. This leads to a more informed patient experience and reduces workload, ensuring that patients are aware of their coverage before services are rendered. AI-powered solutions can perform these checks 95% faster than human teams, enhancing operational efficiency.
- Improve Charge Capture: Invest in training for clinical staff on accurate documentation and coding practices. Regular audits help identify areas for improvement. They also ensure compliance with coding regulations, which is crucial for optimizing medical billing and speeding up reimbursements.
- Accelerate Submission of Requests: Adopt electronic submission to expedite the process. It’s beneficial to set a schedule for submitting requests within 24-48 hours after the visit to boost cash flow, as prompt submissions can result in increased revenue due to fewer rejections. Regular audits of the medical revenue cycle, ideally conducted quarterly, can help identify billing errors and ensure compliance with HIPAA and payer rules.
- Automate Payment Posting: Use software that integrates with billing systems to automate payment posting. This minimizes manual mistakes and allows staff to focus on more essential tasks, ensuring that accounts are updated quickly after requests are processed and compensated.
- Implement Proactive Accounts Receivable Management: Set up reminders for follow-ups on unpaid claims. Establish a clear protocol for addressing overdue accounts to maintain cash flow, as effective management of accounts receivable is crucial for financial stability. Healthcare Partners Consulting‘s approach to accounts receivable management can lead to a 20-40% reduction in days in accounts receivable, significantly enhancing cash flow and reducing administrative burdens.
- Develop a Rejection Management Strategy: Create a dedicated team to analyze rejection trends and implement corrective actions. Regular training on typical rejection reasons can empower staff to prevent future issues, which is essential for maintaining revenue integrity. The automation of eligibility verification has resulted in unparalleled precision and speed, decreasing rejections by 20%. By managing rejection workflows efficiently, organizations can retrieve previously refused submissions and improve overall billing precision.
- Utilize Reporting Tools: Leverage analytics software to track KPIs such as days in accounts receivable and claim denial rates. Consistently assessing these metrics enables organizations to recognize trends and modify strategies accordingly, promoting a data-informed approach to financial cycle enhancement. Organizations that implement these strategies can experience substantial income increases and enhanced growth in volume and profit margins.
By focusing on these strategies, healthcare practices can not only enhance their financial performance but also improve patient care outcomes.
Leverage Technology and Automation for Efficiency
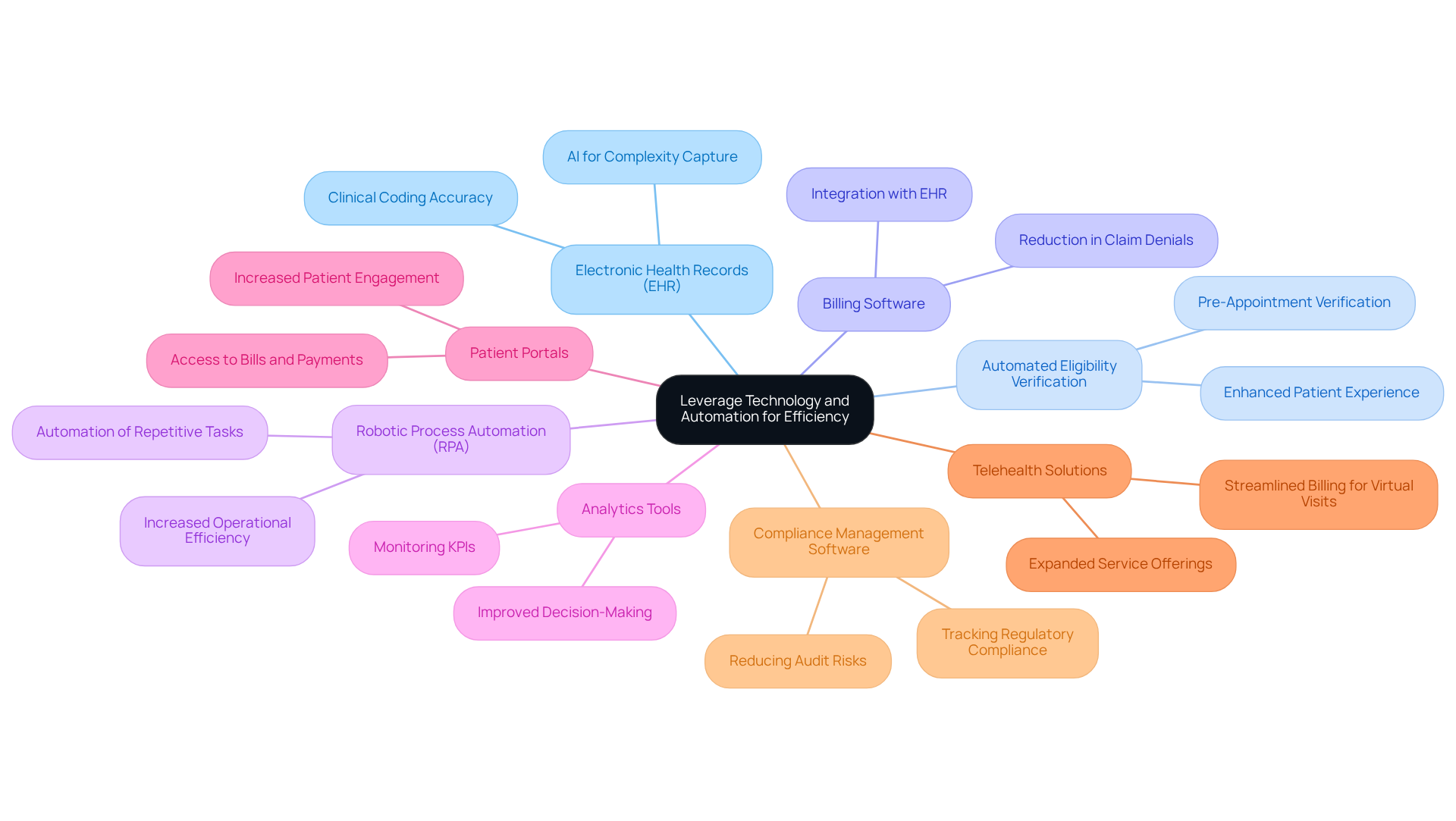
In the complex landscape of the medical revenue cycle, technology emerges as a critical factor in driving efficiency and accuracy. Healthcare Partners Consulting (HPC) offers comprehensive services that leverage technology in several key areas:
- Electronic Health Records (EHR): Advanced EHR systems have enabled organizations to achieve clinical coding accuracy rates of 90% or higher, as highlighted in the Oliver Wyman survey. This survey indicates that targeted uses of AI improve clinical complexity capture with similar accuracy rates, allowing for seamless documentation and coding while reducing the risk of errors.
- Automated Eligibility Verification: HPC highlights the need for verifying patient insurance eligibility before appointments, ensuring that patients are informed of their coverage prior to receiving services. This proactive approach minimizes delays and enhances the overall patient experience.
- Billing Software: Investing in comprehensive billing software that integrates with EHR systems is crucial. HPC ensures that the medical revenue cycle is streamlined, allowing for accurate and prompt claims submission, which contributes to a 20-30% reduction in claim denials.
- Robotic Process Automation (RPA): Utilizing RPA to automate repetitive tasks such as data entry and payment posting reduces manual errors and frees up staff to focus on more complex issues, ultimately enhancing operational efficiency.
- Analytics Tools: Implementing analytics tools to monitor key performance indicators (KPIs) and generate reports is essential. Organizations utilizing advanced analytics attain 5-10% greater returns on assets compared to industry counterparts, enabling informed decision-making and recognition of areas for enhancement, resulting in 15-25% quicker reimbursement timelines.
- Patient Portals: Providing patient portals allows individuals to access their bills, make payments, and interact with the clinic, boosting patient involvement and decreasing administrative burden.
- Telehealth Solutions: Incorporating telehealth platforms expands service offerings and streamlines billing for virtual visits, ensuring that all services are captured and billed appropriately.
- Compliance Management Software: Using software that helps track compliance with healthcare regulations ensures that billing practices adhere to legal standards, reducing the risk of audits.
Furthermore, tackling the obstacles presented by rejected claims is essential. HPC’s denial management services monitor, assess, and contest denied claims, significantly improving the income cycle efficiency. By adopting these technologies, healthcare providers can not only streamline their processes but also significantly enhance their medical revenue cycle performance. Ultimately, embracing these technological advancements can transform the financial health of healthcare organizations, paving the way for improved patient care and satisfaction.
Engage and Train Staff for Compliance and Success
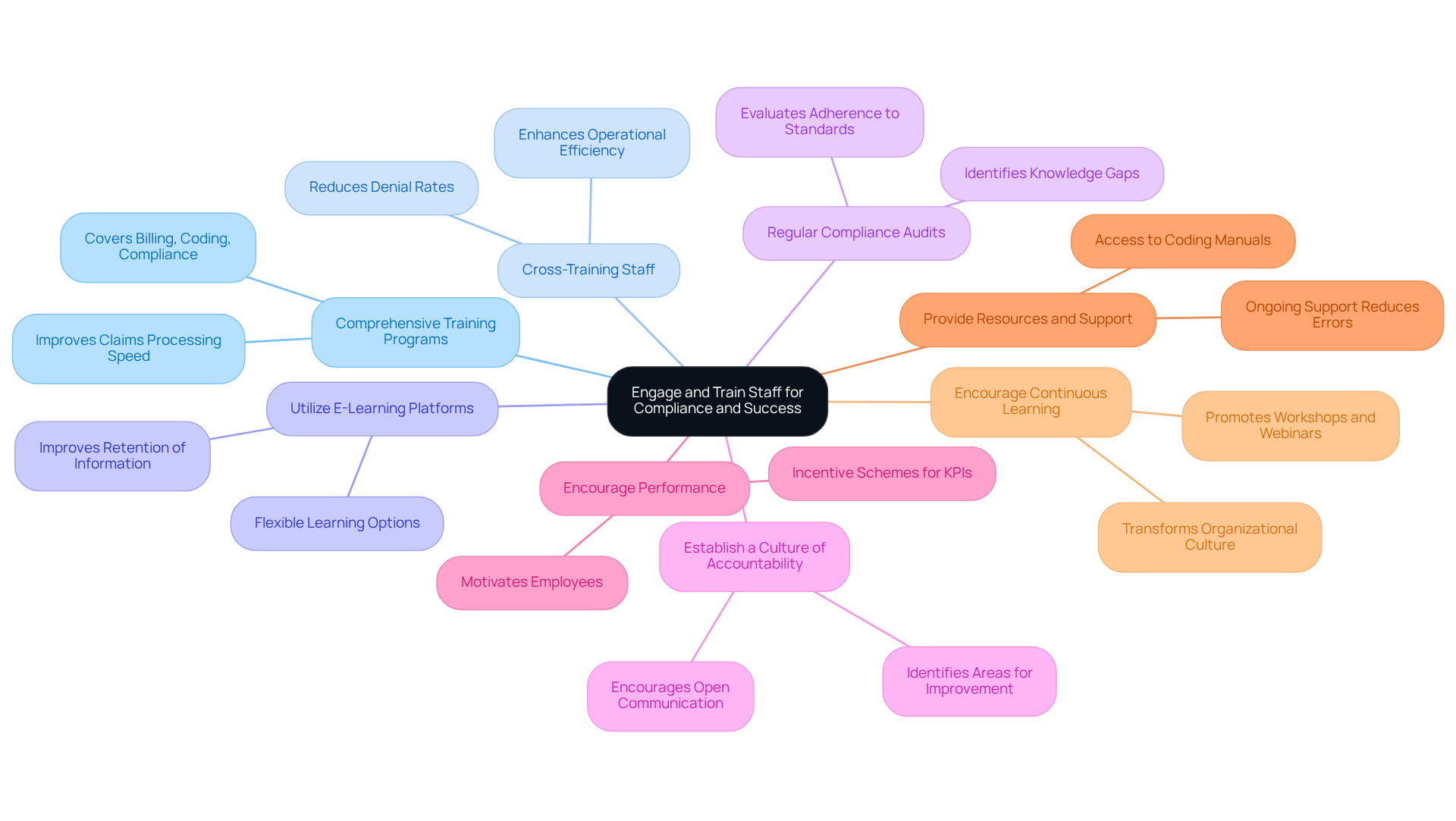
Engaging and training staff is crucial for optimizing the medical revenue cycle management and ensuring operational success. Here are effective strategies to ensure your team is well-prepared:
- Comprehensive Training Programs: Develop training initiatives that encompass all facets of the medical revenue cycle management, including billing, coding, compliance, and patient engagement. Regular training sessions keep staff informed about industry changes, which is essential for maintaining accuracy and compliance. Practices that invest in comprehensive training programs typically see 20-30% improvements in claims processing speed, which is essential for maximizing the medical revenue cycle and income.
- Cross-Training Staff: Encourage cross-training among team members to ensure a holistic understanding of the medical revenue cycle process. This approach fosters teamwork and ensures smoother operations during staff absences, ultimately enhancing operational efficiency. Understanding the nuances of different insurance requirements in the medical revenue cycle can significantly reduce denial rates, as effective denial management strategies can lead to a 30-50% reduction in recurring denial types.
- Utilize E-Learning Platforms: Implement e-learning platforms that offer flexible training options, allowing employees to learn at their own pace and revisit materials as needed. This adaptability can lead to better retention of information and improved performance, which is essential for enhancing billing accuracy.
- Regular compliance audits are essential to evaluate adherence to billing and coding standards within the medical revenue cycle. Use the findings to provide targeted training, addressing any knowledge gaps and reinforcing best practices. Without regular training, staff may struggle to keep up with industry standards in the medical revenue cycle, which can lead to significant financial repercussions.
- Establish a culture of accountability by nurturing a setting where team members feel accountable for their roles in the medical revenue cycle. Encourage open communication and feedback to identify areas for improvement, which can lead to enhanced performance and compliance. Creating this culture is vital for achieving our goals in denial management and financial recovery.
- Encourage Performance: Consider introducing incentive schemes that reward employees for meeting key performance indicators (KPIs) associated with the medical revenue cycle. This can motivate employees to strive for excellence and improve overall outcomes, particularly in recovering previously denied claims.
- Provide Resources and Support: Ensure that staff have access to essential resources, such as coding manuals and compliance guidelines. Ongoing support helps staff feel confident in their roles, reducing the likelihood of errors. With staff turnover in medical billing averaging around 25% annually, investing in training can help retain talent and reduce recruitment costs.
- Encourage Continuous Learning: Promote a culture of continuous learning by encouraging staff to attend workshops, webinars, and industry conferences. Remaining knowledgeable about optimal methods and new developments in revenue cycle management is essential for sustained success and corresponds with the flexible assistance offered by Healthcare Partners Consulting.
Ultimately, a well-trained team is not just an asset; it is a cornerstone of financial stability and growth in the medical revenue cycle for healthcare practices.
Conclusion
Effective revenue cycle management is critical for healthcare practices striving for financial stability and optimal patient care. By implementing the outlined strategies, providers can streamline their processes and enhance their overall financial performance. This comprehensive approach to revenue cycle management ensures that each step – from patient registration to claim management – is optimized for efficiency and accuracy.
Key insights from the article emphasize the importance of:
- Thorough patient registration
- Timely eligibility verification
- Effective charge capture to prevent revenue loss
Additionally, leveraging technology and automation plays a pivotal role in enhancing operational efficiency, while engaging and training staff ensures compliance and fosters a culture of accountability. Regular audits and performance tracking further support ongoing improvements in the revenue cycle.
By prioritizing revenue cycle management, healthcare providers not only secure their financial future but also elevate the standard of care they provide to patients. By adopting these best practices and embracing technological advancements, healthcare providers can transform their financial health and enhance patient outcomes.
Frequently Asked Questions
What is revenue cycle management (RCM) in healthcare?
Revenue cycle management (RCM) is a critical process that impacts the financial viability of healthcare practices by managing the financial transactions involved in patient care.
What is the first step in the RCM process?
The first step is Patient Registration, which involves collecting accurate patient information, including verifying insurance details and demographic information to prevent billing errors.
Why is eligibility verification important in RCM?
Eligibility verification is important because it confirms a patient’s eligibility for services before treatment, helping to avoid claim denials and ensuring that the services provided are covered by the patient’s insurance.
What does charge capture involve?
Charge capture involves accurately documenting all services rendered during patient visits, including coding procedures and diagnoses correctly to secure proper reimbursement and prevent revenue loss.
How does timely submission affect the RCM process?
Timely submission of requests to insurance companies is essential to avoid cash flow issues, with practices aiming for submissions within 30 to 40 days to improve efficiency.
What is payment posting in the RCM process?
Payment posting is the step where received payments are accurately recorded in patient accounts, helping to maintain precise financial records and quickly address any discrepancies.
Why is accounts receivable management crucial?
Accounts receivable management is crucial for monitoring outstanding demands and following up on unpaid invoices, which enhances cash flow and financial stability.
What role does claim management play in RCM?
Claim management involves analyzing and addressing claim rejections swiftly to influence income positively. Understanding the causes of refusals helps organizations improve their processes and reduce future denials.
How do reporting and analytics contribute to RCM?
Reporting and analytics involve regularly reviewing financial reports and key performance indicators (KPIs) to identify trends and areas for improvement, ensuring ongoing financial health.
What are the benefits of effective denial management in healthcare?
Effective denial management practices are essential for maintaining income flow and ensuring financial sustainability in healthcare, ultimately enhancing the quality of patient care delivered.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting