Mastering Medical Coding
Navigate Radiology Code Changes: Essential Updates for 2026

Introduction
As the healthcare landscape evolves, the impending changes to radiology codes in 2026 introduce significant complexities that demand attention from medical professionals. With the introduction of 288 new CPT codes and substantial revisions to existing regulations, grasping these updates is vital for accurate billing and optimizing reimbursement. Adapting to these changes is fraught with complexities that can hinder effective implementation. This raises a critical question: how can healthcare providers navigate the new coding standards while minimizing claim denials and ensuring compliance?
Clarify the Role of CPT Codes in Radiology
CPT numbers are essential for ensuring accurate communication in the radiology billing process amid the upcoming radiology code changes. These standardized codes describe medical, surgical, and diagnostic services, playing a crucial role in facilitating appropriate compensation for healthcare practitioners. Each CPT designation corresponds to a specific procedure, enabling clear communication between providers and payers.
Accurate coding, especially in light of the radiology code changes, is not merely a compliance issue; it significantly influences reimbursement rates and the overall management of patient statements. For instance, the 2026 CPT update introduces 288 new entries, including:
- Entries 92X01 and 92X02 for coronary therapeutic services
- Entries 37XX1-37X46 for Lower Extremity Revascularization
These updates directly improve billing accuracy and minimize claim denials. A case study involving an MRI scan of the pelvis illustrates this point: the patient exhibited fullness after a hysterectomy and right-side oophorectomy, leading to the final CPT designation assigned of 72195, which directly influenced the reimbursement process.
Understanding and applying these guidelines is crucial for medical professionals to minimize claim rejections and navigate medical regulations effectively. Additionally, effective management of patient statements, including addressing underpayments and aging claims, is vital for optimizing revenue cycle processes. Consultations tailored to specific needs can help identify the best administrative solutions for healthcare practices, ensuring that providers are well-equipped to handle the intricacies of billing and compliance.
Reviewing the 2026 CPT Coding Manual is essential for compliance with the latest radiology code changes.
Explore Key CPT Code Changes for 2026
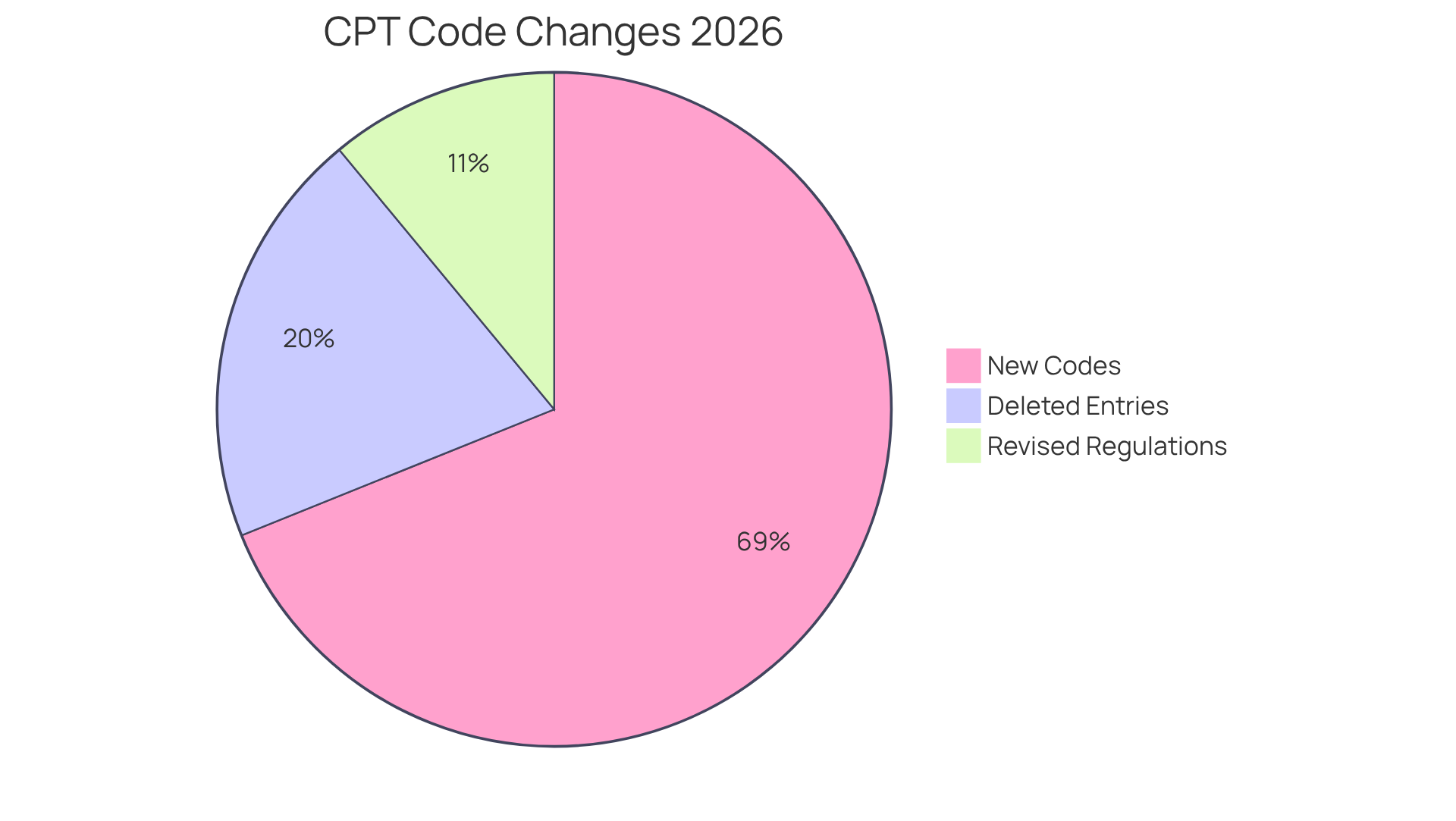
The 2026 radiology code changes introduce significant modifications to billing practices, requiring immediate attention from healthcare providers. These updates encompass a total of 418 modifications, which include:
- 288 New Codes: These codes encompass a range of imaging procedures, reflecting advancements in technology and methodologies.
- 46 Revised Regulations: Updates to existing regulations ensure alignment with current medical practices, enhancing accuracy in billing.
- 84 Deleted Entries: The removal of specific entries poses challenges for healthcare providers, necessitating adjustments to their billing practices to avoid errors and ensure compliance.
Significantly, the revisions to protocols for lower extremity vascular procedures improve specificity, enabling more accurate reporting. For example, the revascularization classifications now categorize interventions by vascular regions, enhancing clarity in billing. Healthcare providers need to stay informed about radiology code changes to refine their billing procedures and maintain compliance, as the precision of classification directly influences reimbursement rates and operational efficiency.
Case studies highlight the positive effects of these updates. For instance, the introduction of new codes for remote monitoring services has simplified billing for healthcare practitioners, enabling them to report monitoring over shorter durations of 2-15 days within a 30-day period. This shift not only improves billing accuracy but also reflects the industry’s move towards integrating technology in patient care.
Healthcare Partners Consulting offers flexible service plans tailored to the size of your practice and claim volume, ensuring that mental health clinics can effectively navigate these updates. Their specialty-focused, relationship-driven service aims to enhance revenue and decrease denials, facilitating adaptation to the changing coding landscape.
As the American Medical Association highlights, staying ahead of CPT changes is vital for operational efficiency in managing practitioner data and claims processing. Ultimately, these updates are crucial for ensuring that medical professionals can deliver high-quality care while effectively managing the complexities of billing.
Implement Strategies for Adapting to New Coding Standards
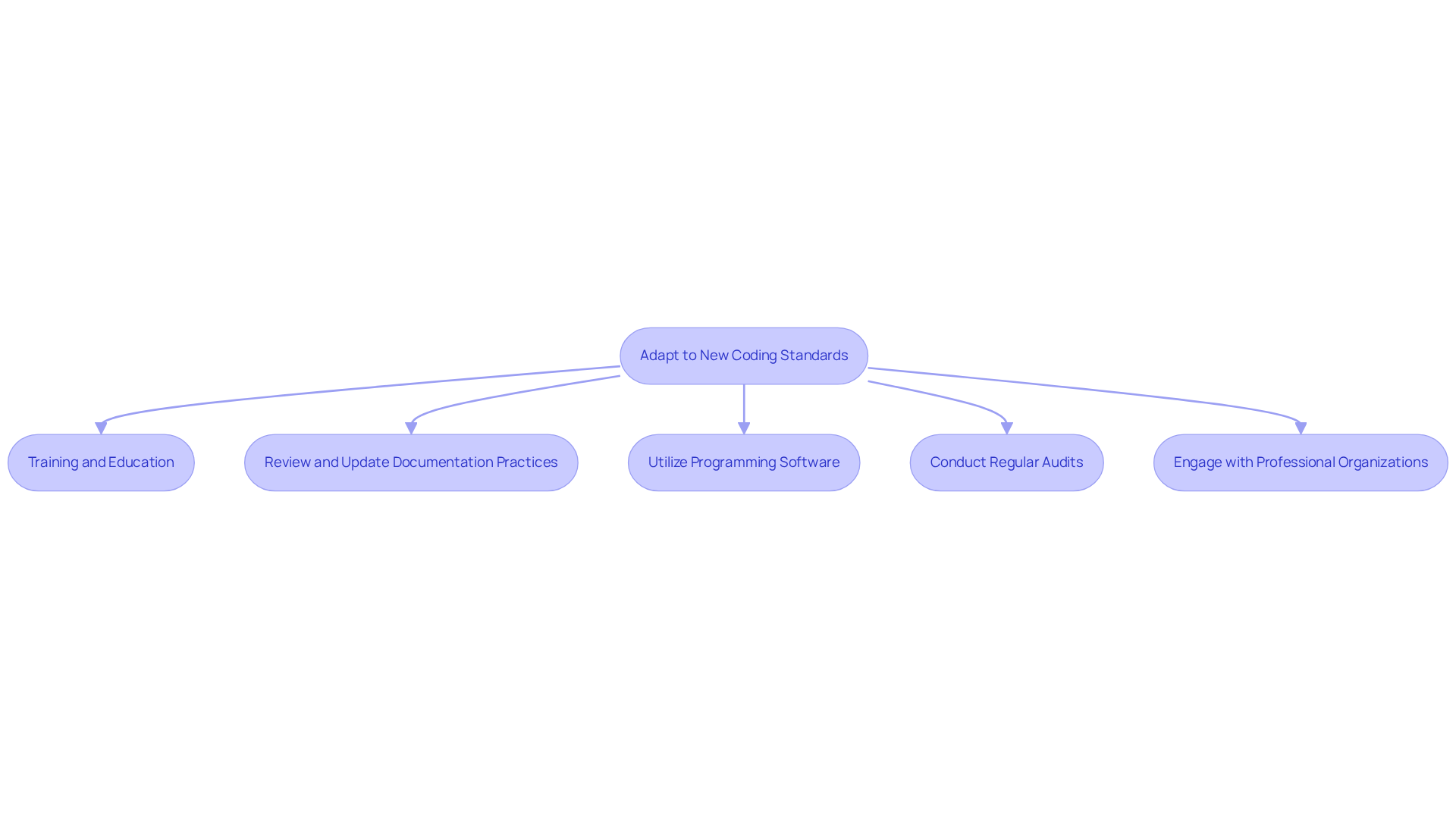
As healthcare coding evolves, the risk of non-compliance increases without proactive measures. To effectively adapt to the new coding standards for 2026, healthcare providers should implement the following strategies:
- Training and Education: Regular training for programming staff on new standards is crucial for compliance. This approach mitigates the risk of denials from outdated knowledge.
- Review and Update Documentation Practices: It is essential to ensure that clinical documentation aligns with the new standards. Accurate documentation supports compliance and enhances reimbursement, reducing claim denials.
- Utilize Programming Software: Investing in updated programming software that integrates the latest CPT codes can significantly streamline the programming process. This software includes real-time error checks to prevent denials before submission.
- Conduct Regular Audits: Implementing periodic assessments of programming practices allows suppliers to identify and correct discrepancies. Ongoing evaluation is vital for billing accuracy and compliance.
- Engage with Professional Organizations: Engagement with organizations like the American College of Radiology (ACR) provides valuable resources and updates on billing changes, keeping practices informed.
Ultimately, neglecting these strategies could jeopardize financial stability and compliance in an increasingly complex healthcare landscape.
Ensure Compliance with Updated Coding Regulations
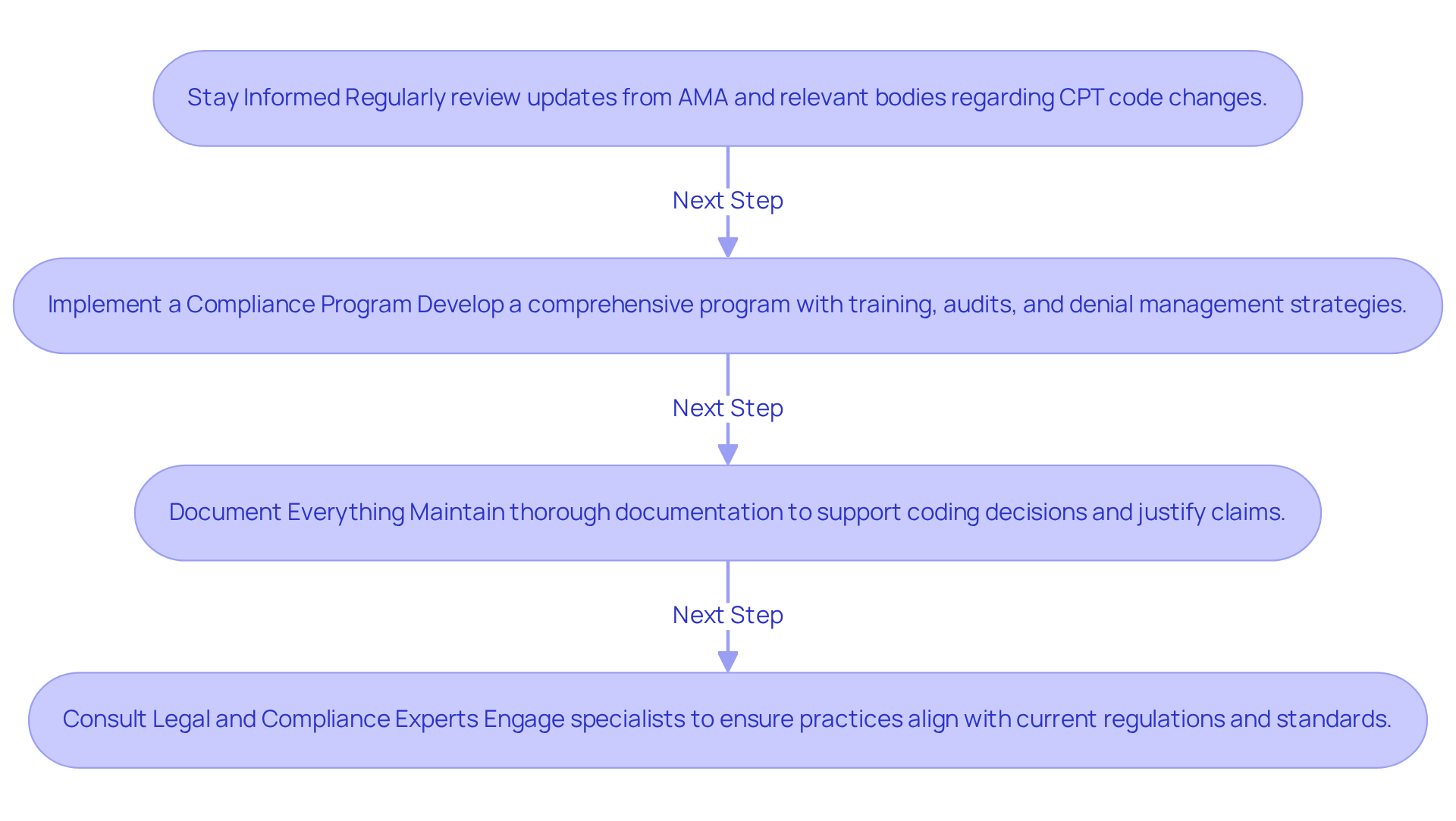
Adhering to updated programming regulations is essential for healthcare providers to avoid financial penalties and ensure proper reimbursement. Here are key steps to ensure compliance:
- Stay Informed: Regularly review updates from the American Medical Association (AMA) and other relevant bodies regarding CPT code changes.
- Implement a Compliance Program: Develop a comprehensive compliance program that includes regular training, audits, and updates to programming practices. This program must include denial management strategies to optimize revenue recovery.
- Document Everything: Maintain thorough documentation that supports the coding decisions made, as this is crucial during audits and for justifying claims.
- Consult Legal and Compliance Experts: Consult with specialists in compliance within the medical field to ensure that all practices align with current regulations and standards. Personalized consultations can help identify optimal administrative solutions tailored to your practice’s needs.
By embracing compliance and expert guidance, healthcare providers can safeguard their financial health and operational integrity.
Conclusion
Navigating the upcoming radiology code changes in 2026 presents significant challenges for healthcare providers, necessitating a strategic approach to maintain billing accuracy and compliance. CPT codes play a crucial role in facilitating communication between providers and payers, ensuring accurate billing and reimbursement of medical services. With 288 new codes and numerous revisions set to take effect, understanding these updates is crucial for optimizing revenue cycles and minimizing claim denials.
The article highlights the necessity of proactive adaptation strategies for healthcare providers. From ongoing staff training and documentation reviews to the integration of updated programming software, providers must implement robust measures to align with the new coding standards. Additionally, staying informed through professional organizations and conducting regular audits will further enhance compliance and operational efficiency. The case studies presented illustrate how these changes can positively impact billing accuracy and overall financial health.
In conclusion, embracing the 2026 radiology coding updates is not merely a compliance necessity but a pathway to improved operational success. Healthcare providers must prioritize education and proactive strategies to navigate these changes effectively. By doing so, they can ensure high-quality patient care while safeguarding their financial stability in an increasingly complex healthcare landscape. Proactive engagement with these updates will not only enhance compliance but also fortify financial health in an evolving healthcare environment.
Frequently Asked Questions
What are CPT codes and why are they important in radiology?
CPT codes are standardized codes that describe medical, surgical, and diagnostic services. They are essential for accurate communication in the radiology billing process and play a crucial role in ensuring appropriate compensation for healthcare practitioners.
How do CPT codes influence reimbursement rates?
Accurate coding significantly influences reimbursement rates and the overall management of patient statements. Properly assigned CPT codes help minimize claim denials, which directly affects the reimbursement process.
What changes are introduced in the 2026 CPT update?
The 2026 CPT update introduces 288 new entries, including codes 92X01 and 92X02 for coronary therapeutic services, and entries 37XX1-37X46 for Lower Extremity Revascularization.
Can you provide an example of how CPT codes affect billing accuracy?
A case study involving an MRI scan of the pelvis shows that the final CPT designation assigned (72195) influenced the reimbursement process after the patient exhibited fullness following a hysterectomy and right-side oophorectomy.
Why is it important for medical professionals to understand CPT guidelines?
Understanding and applying CPT guidelines is crucial for minimizing claim rejections and effectively navigating medical regulations, which helps optimize revenue cycle processes.
What should healthcare providers do to manage patient statements effectively?
Effective management of patient statements includes addressing underpayments and aging claims, which is vital for optimizing revenue cycle processes.
How can healthcare practices ensure they are compliant with the latest radiology code changes?
Reviewing the 2026 CPT Coding Manual is essential for compliance with the latest radiology code changes. Tailored consultations can also help identify the best administrative solutions for healthcare practices.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting