Mastering Medical Coding
Understanding the CPT Code for MAC Anesthesia: Key Insights for Clinics

Introduction
In the intricate realm of healthcare billing, accurate coding stands as a fundamental pillar, especially for Monitored Anesthesia Care (MAC). The CPT codes associated with MAC not only facilitate proper communication between healthcare providers and insurers but also play a pivotal role in securing timely reimbursements and maintaining compliance with ever-evolving regulations. This high denial rate underscores the critical need for precise coding practices, as around 30% of sedation claims face denials due to coding errors. Clinics must adopt strategic approaches to navigate this complex landscape, ensuring both financial stability and the delivery of safe, responsive patient care.
Define CPT Code for Monitored Anesthesia Care (MAC)
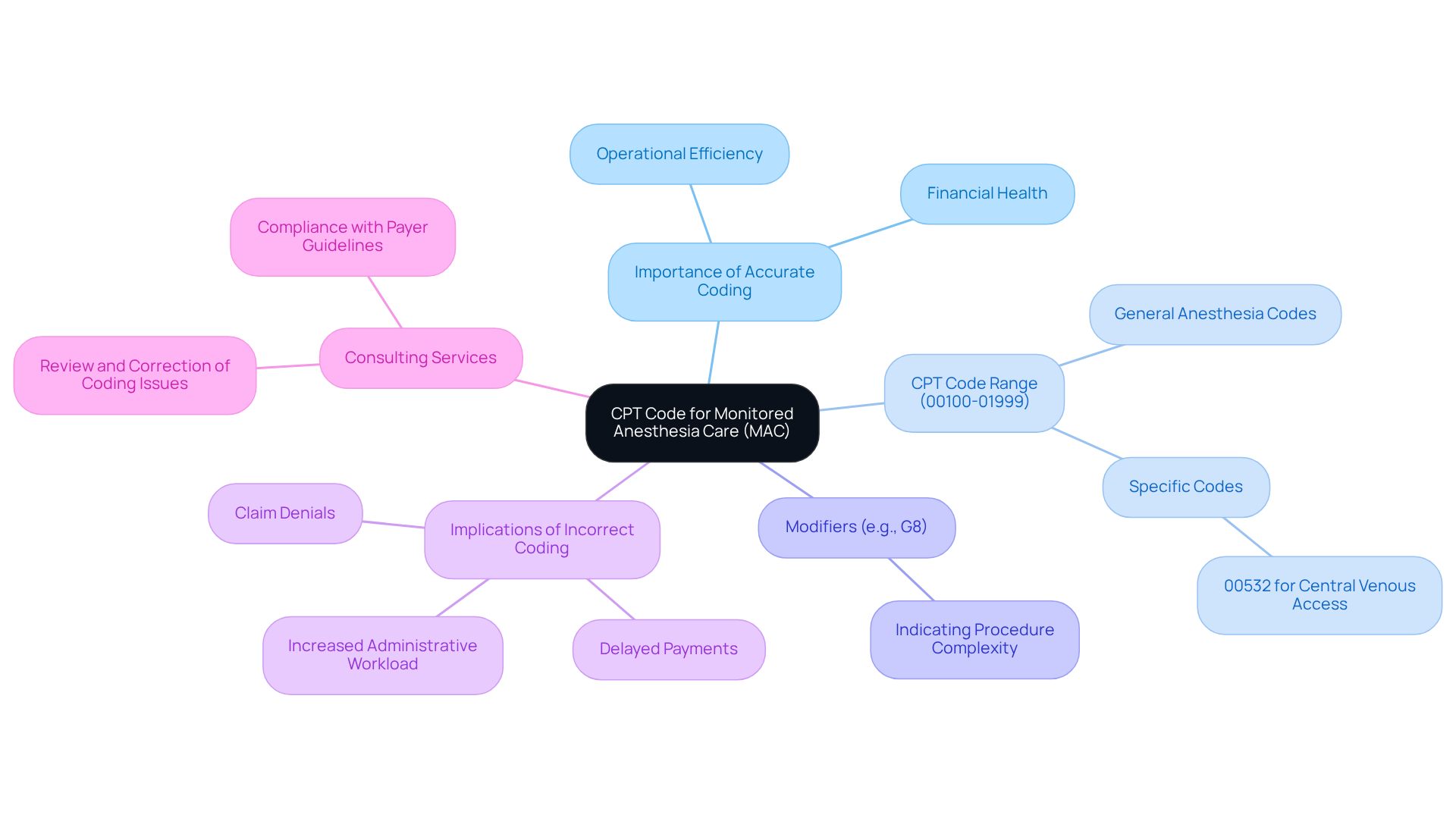
Accurate CPT code for MAC anesthesia designations are critical for effective billing of sedation services that monitor vital signs and sedation levels during procedures. Unlike general sedation, MAC allows patients to remain aware and responsive while receiving tranquilization. The pertinent CPT code for MAC anesthesia lies between 00100 and 01999, encompassing a range of sedation services. For instance, number 00532 is specifically assigned for sedation services related to central venous access. Additionally, modifiers such as G8 can be appended to indicate the complexity of the procedure, which is essential for accurate billing and reimbursement.
Incorrect or incomplete coding can lead to significant operational challenges, including claim denials, delayed payments, and increased administrative workload. Healthcare Partners Consulting addresses these challenges by reviewing and correcting coding issues before claims are submitted, ensuring compliance with payer-specific guidelines and staying current on CPT, ICD-10, and HCPCS updates. By mastering these codes, practices can enhance their financial health and operational effectiveness, making it a vital aspect of effective practice management in healthcare settings. Recent updates highlight ongoing discussions around sedation coding, emphasizing the need for healthcare providers to stay informed about changes in billing practices and payer policies. As noted by MedBill Geeks, “Anesthesia medical billing represents one of the most complex specialties in healthcare revenue cycle management.” Moreover, UnitedHealthcare’s payment policy permits distinct reimbursement for moderate sedation services, emphasizing the changing environment of billing practices for sedation.
Contextualize the Importance of CPT Code in Anesthesia Billing
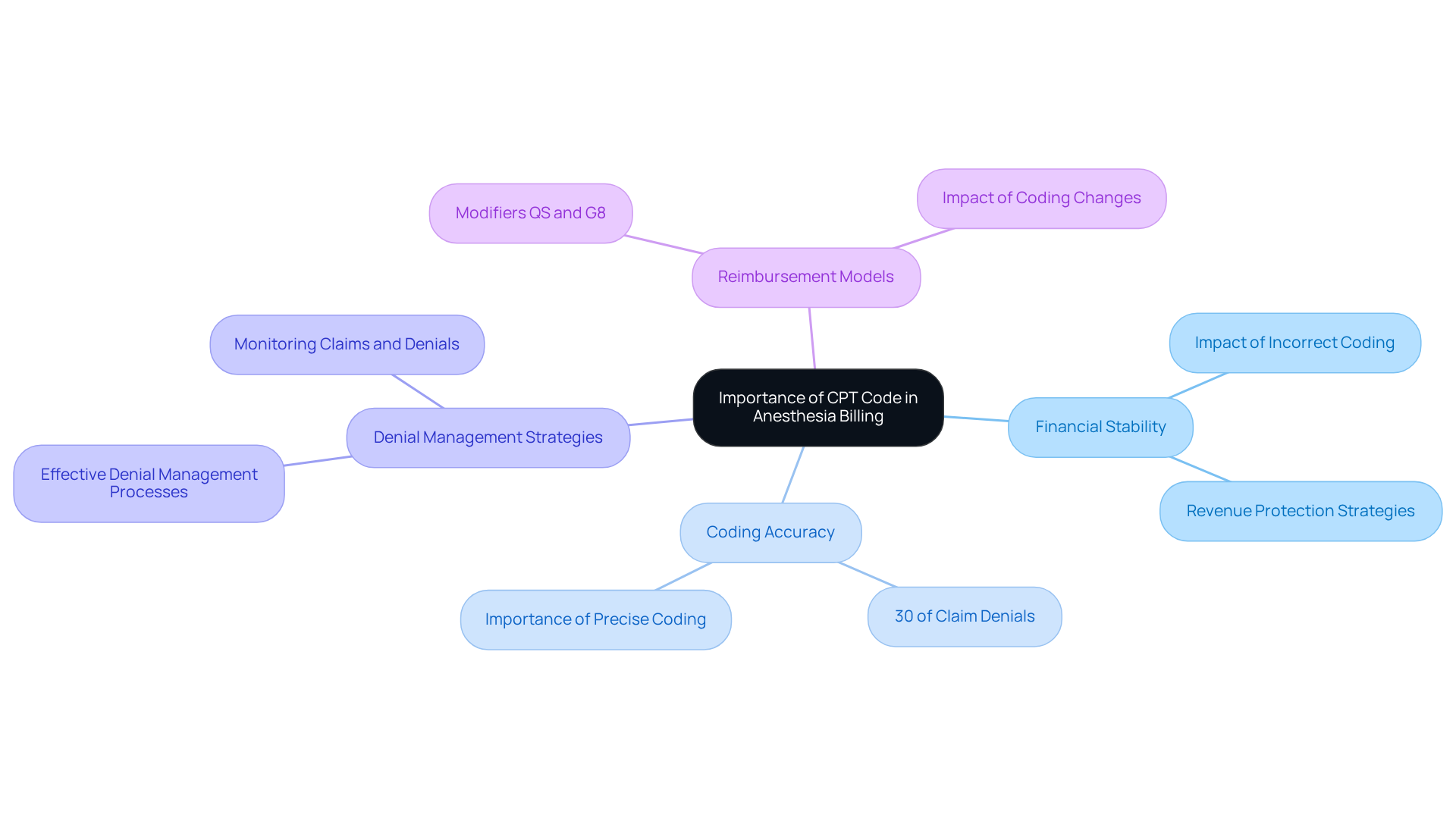
Inaccurate CPT coding can significantly jeopardize the financial stability of healthcare practices, particularly in sedation billing. CPT codes, such as the cpt code for mac anesthesia, are critical in sedation billing, providing a standardized method for healthcare providers to communicate services to insurers. Accurate coding is essential not only for securing reimbursement but also for ensuring compliance with healthcare regulations.
In the realm of Monitored Anesthesia Care, the precise application of the cpt code for mac anesthesia is crucial for justifying the medical necessity of services, thereby minimizing the risk of claim denials. With around 30% of sedation claim denials attributed to incorrect CPT coding, meticulous attention to detail is vital to avoid financial repercussions.
As reimbursement models continue to evolve, understanding the intricacies of sedation coding becomes increasingly important for maintaining the financial health of practices. Implementing effective denial management strategies is essential for safeguarding practice revenue, as they facilitate the recovery of denied claims and alleviate administrative burdens.
For instance, the strategic use of modifiers such as QS and G8 can substantially influence reimbursement rates, with studies showing that their correct application can increase reimbursement by up to 15%. Additionally, implementing robust denial management processes can lead to a 30-50% reduction in recurring denial types. Thus, providers must stay abreast of coding changes and payer requirements to optimize billing practices and ensure compliance.
Explore Key Characteristics and Requirements of MAC CPT Code
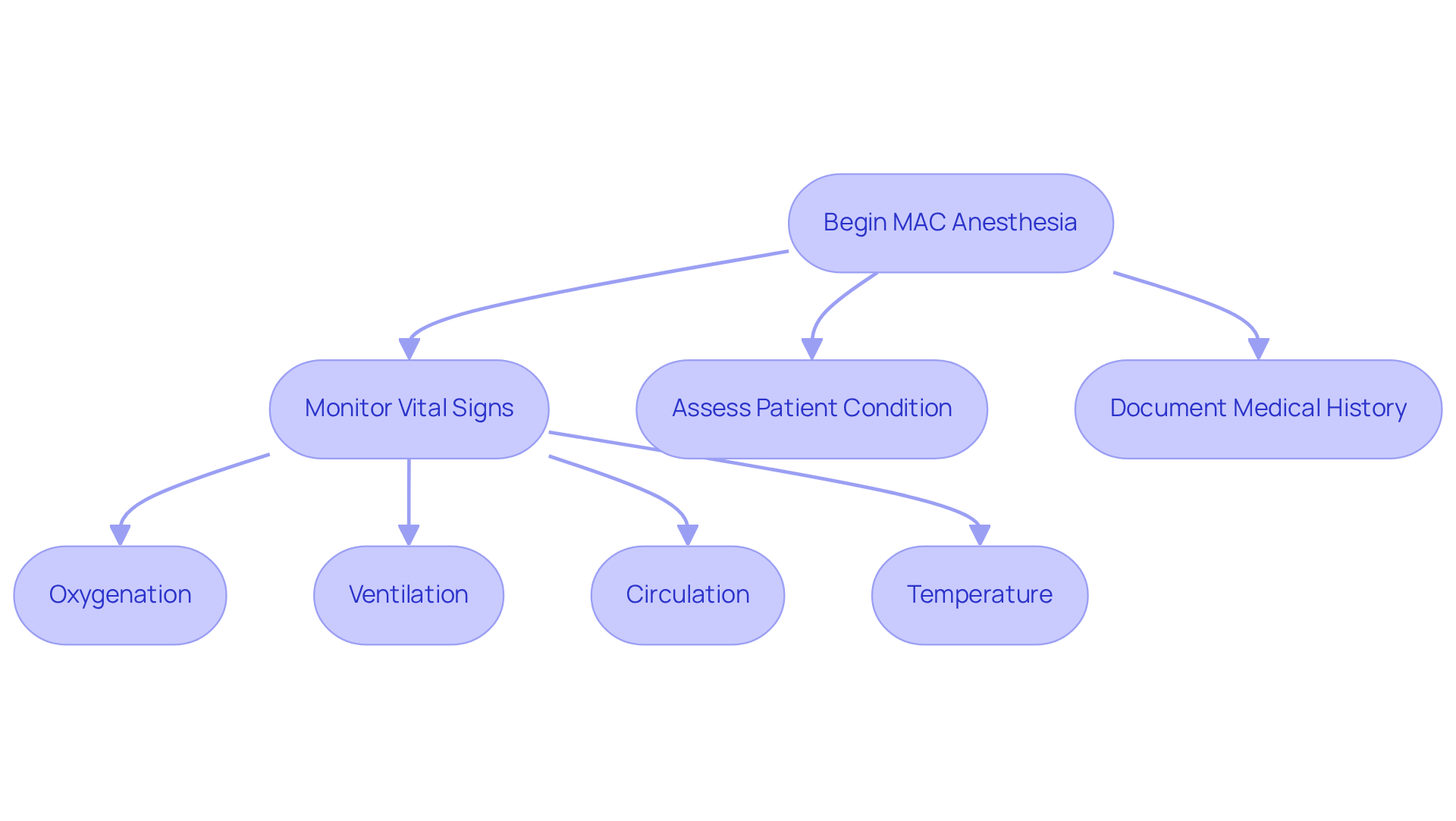
The cpt code for mac anesthesia requires rigorous monitoring of vital signs to ensure patient safety and compliance with established guidelines. Continuous monitoring of vital signs – such as oxygenation, ventilation, circulation, and temperature – is paramount. It is imperative that anesthesia staff continuously assess the individual’s condition to determine the necessity of general anesthesia. Furthermore, documentation is essential; providers must keep precise records that validate the use of MAC, including the individual’s medical history and the details of the procedure. Strict adherence to these requirements ensures accurate billing and enhances the overall safety and quality of care provided to individuals. For instance, the American Society of Anesthesiologists (ASA) guidelines state that MAC should only be billed when the provider is actively engaged in overseeing the individual throughout the procedure. Non-compliance with these standards can have serious repercussions for both patient outcomes and billing integrity.
Provide Examples and Variations of CPT Code for MAC Anesthesia
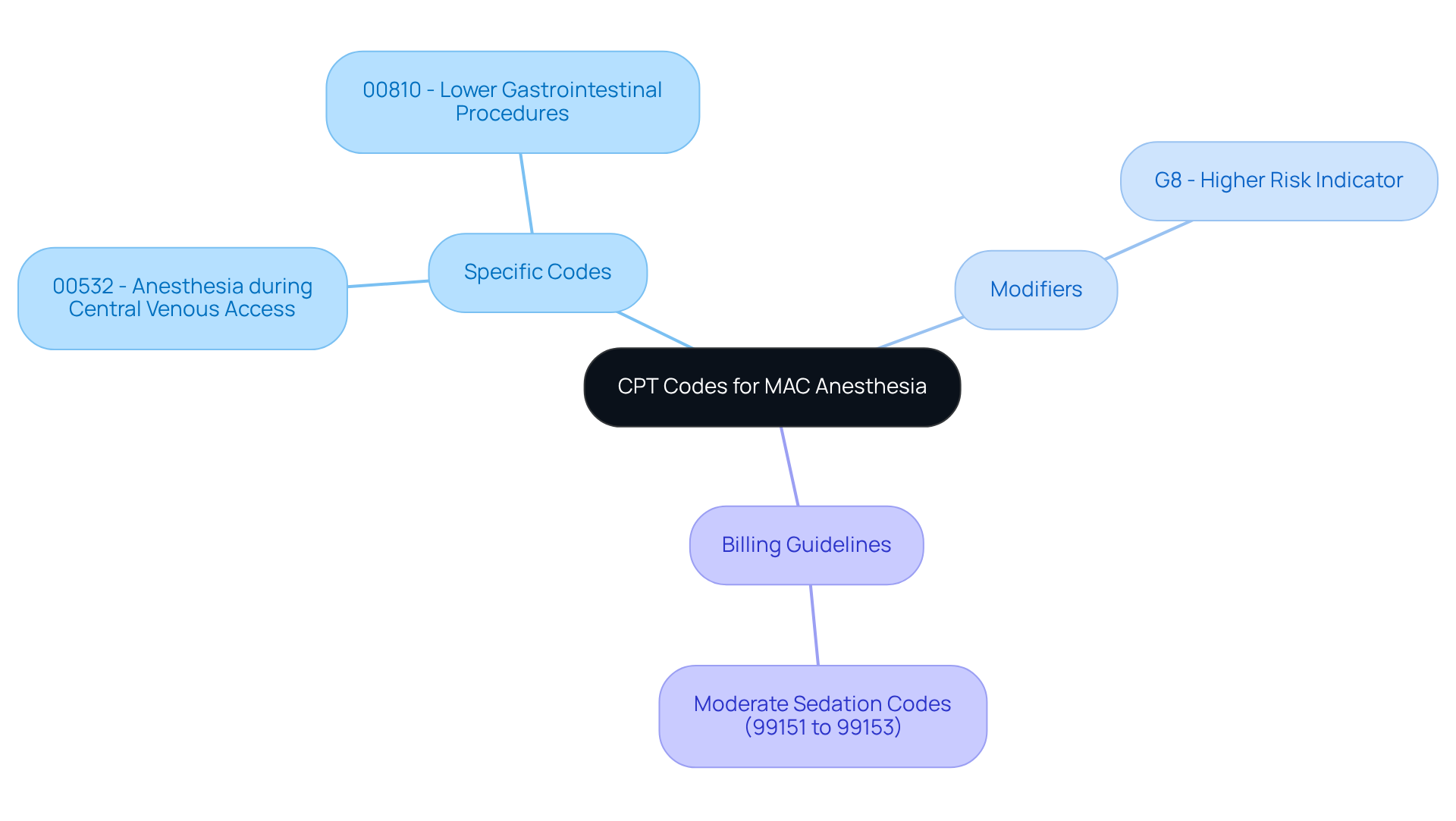
Understanding the nuances of the CPT code for MAC anesthesia is crucial for accurate billing and compliance. The CPT code for MAC anesthesia includes:
- 00532 for anesthesia during central venous access
- 00810 for lower gastrointestinal procedures
These guidelines can vary significantly based on the complexity of the surgical procedure and the patient’s overall health. For instance, when billing for MAC in complex surgeries, modifiers like G8 are often used to indicate that the patient has a higher risk due to pre-existing health conditions. Additionally, CPT numbers 99151 to 99153 cover moderate sedation administered by the same physician providing the diagnostic or therapeutic service, showcasing the range of services that can be billed under the MAC framework.
Healthcare providers must thoroughly understand these codes and their variations to ensure accurate billing and compliance with payer requirements. Inaccurate billing can lead to significant financial repercussions and compliance issues for healthcare providers.
Conclusion
Accurate application of CPT codes for Monitored Anesthesia Care (MAC) is crucial for effective anesthesia billing. This coding ensures clear communication with insurers and is essential for compliance and maximizing reimbursement. Incorrect coding can result in claim denials and financial instability for practices.
Throughout the article, key insights have been provided regarding the importance of precise CPT coding for MAC anesthesia. The discussion highlighted the critical nature of specific codes, such as 00532 for central venous access, and emphasized the necessity of employing modifiers like G8 to reflect the complexity of procedures accurately. Moreover, the article underscored the significance of ongoing education and adherence to evolving guidelines to mitigate the risks associated with billing errors.
As healthcare billing practices evolve, providers must stay informed about changes in CPT codes and payer policies. Implementing robust denial management strategies and maintaining accurate documentation not only safeguards financial health but also enhances the quality of care delivered to patients. By embracing these strategies, healthcare providers can not only enhance their operational efficiency but also significantly improve patient outcomes.
Frequently Asked Questions
What is the CPT code range for Monitored Anesthesia Care (MAC)?
The CPT code for MAC anesthesia lies between 00100 and 01999, which encompasses a range of sedation services.
What is the significance of the CPT code 00532?
The CPT code 00532 is specifically assigned for sedation services related to central venous access.
How do modifiers like G8 affect billing for MAC anesthesia?
Modifiers such as G8 can be appended to indicate the complexity of the procedure, which is essential for accurate billing and reimbursement.
What challenges can arise from incorrect or incomplete coding in anesthesia services?
Incorrect or incomplete coding can lead to claim denials, delayed payments, and increased administrative workload.
How does Healthcare Partners Consulting help with coding issues?
Healthcare Partners Consulting reviews and corrects coding issues before claims are submitted, ensuring compliance with payer-specific guidelines and staying current on CPT, ICD-10, and HCPCS updates.
Why is mastering CPT codes important for healthcare practices?
Mastering these codes can enhance financial health and operational effectiveness, making it a vital aspect of effective practice management in healthcare settings.
What recent updates are relevant to sedation coding practices?
Recent updates highlight ongoing discussions around sedation coding, emphasizing the need for healthcare providers to stay informed about changes in billing practices and payer policies.
What does UnitedHealthcare’s payment policy indicate about moderate sedation services?
UnitedHealthcare’s payment policy permits distinct reimbursement for moderate sedation services, indicating changes in billing practices for sedation.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting