Telehealth Billing Insights
10 Essential Telehealth CPT Codes Every Mental Health Clinic Needs

Introduction
Navigating the complexities of telehealth billing presents significant challenges for mental health clinics in today’s healthcare landscape. As telemedicine becomes integral to patient care, clinics must use CPT codes effectively to optimize reimbursement and comply with regulations. Continuous updates and complexities surrounding these codes require clinics to adapt swiftly; failure to do so could jeopardize financial stability and quality of care.
This article will detail ten essential telehealth CPT codes that every mental health clinic should understand, offering insights into their applications and best practices for successful billing.
99201: New Patient Office or Other Outpatient Visit
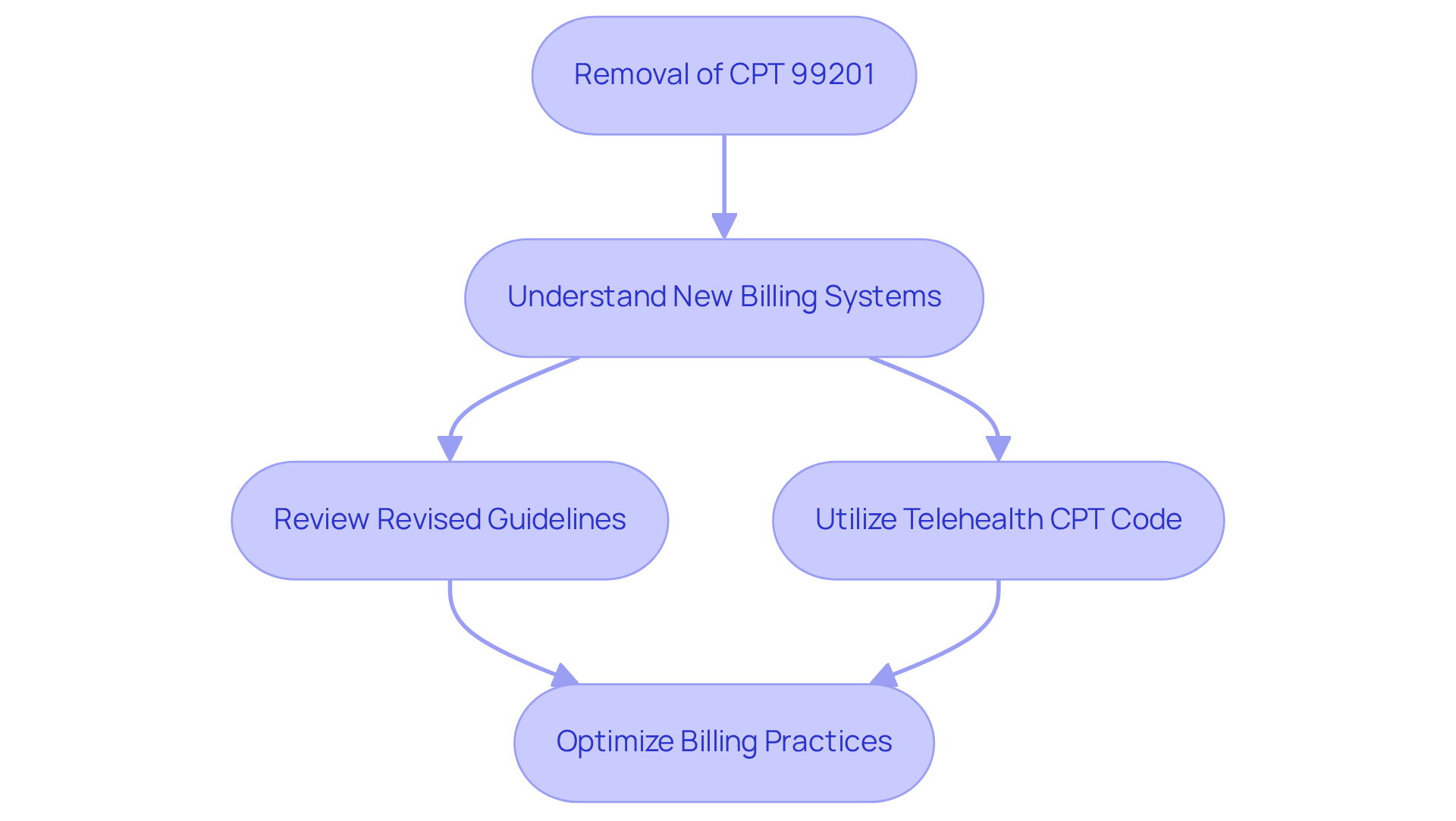
The CPT designation 99201 played a crucial role in new patient office visits requiring straightforward medical decision-making. This system has been removed as of January 1, 2021. Clinics may face challenges in adapting to new billing systems without a clear understanding of the previous CPT designation. Typically, it involved a brief history and examination, lasting about 10 minutes. Current practices must adhere to the revised guidelines that align with similar services, ensuring compliance with billing regulations and optimizing reimbursement opportunities for new patient visits by utilizing the telehealth CPT code. Understanding the evolution of these guidelines is vital for optimizing billing practices and ensuring financial sustainability.
99202: Established Patient Office or Other Outpatient Visit
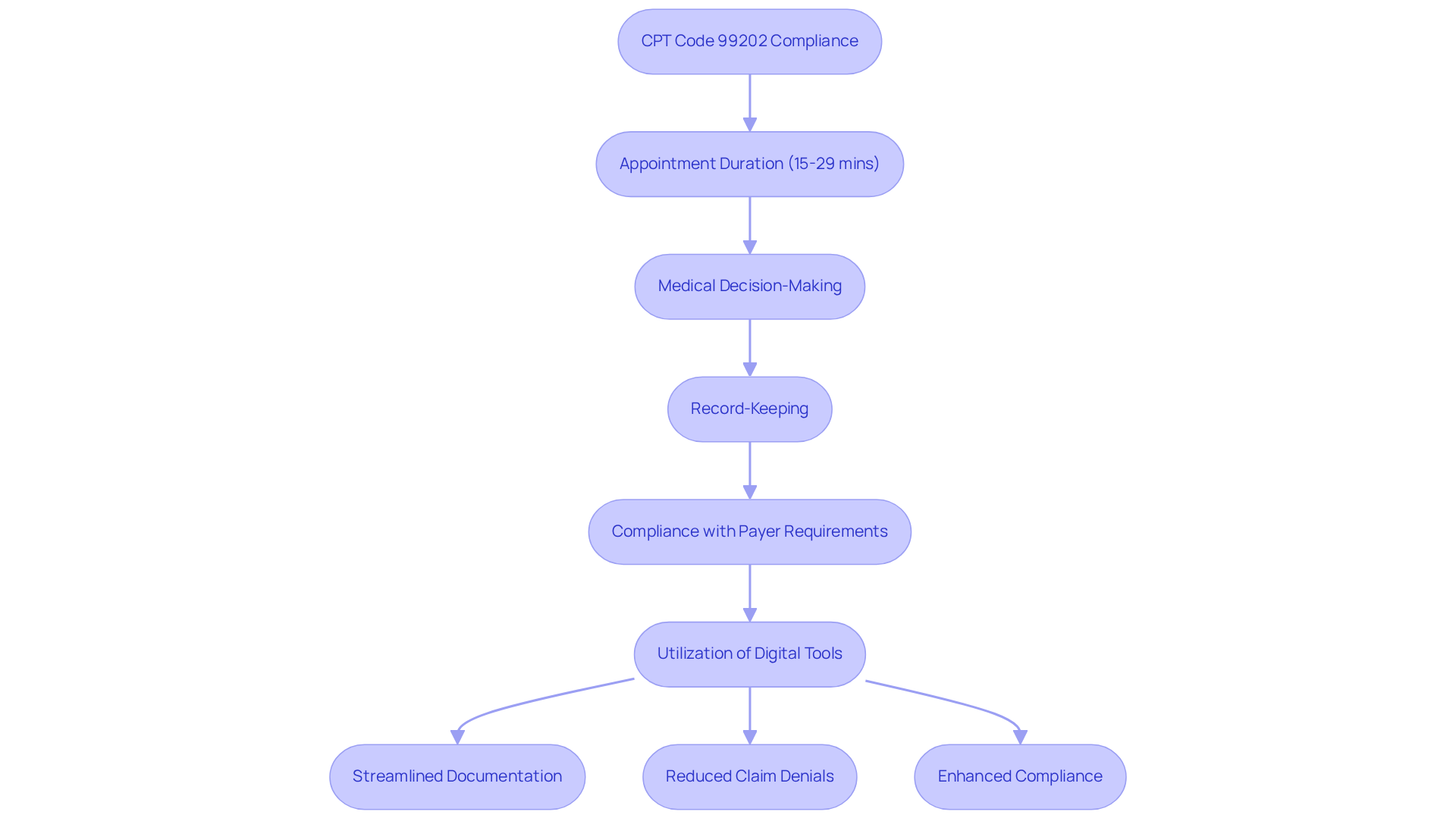
CPT designation 99202 plays a critical role in defining the parameters for established patient office visits that require a medically appropriate history and/or examination. This regulation pertains to visits lasting between 15 and 29 minutes and involves straightforward medical decision-making.
For psychological facilities, careful record-keeping of every appointment is crucial to validate billing for this classification. Accurate records ensure compliance with payer requirements. They also optimize reimbursement for ongoing patient care. Without effective documentation, wellness clinics may struggle to maintain healthy revenue streams, particularly due to the new CPT codes introduced in 2026 that create billing opportunities for practices utilizing digital tools.
Healthcare Partners Consulting emphasizes the importance of precise coding and adherence in their tailored revenue cycle management services, which are customized to address the distinct requirements of wellness providers. Neglecting these standards could jeopardize financial health and reimbursement timelines, especially concerning the telehealth cpt code eligibility and the incorporation of AI-assisted services in mental wellness billing.
By utilizing expert coding assistance and proactive revenue cycle strategies, healthcare facilities can enhance their financial health and guarantee timely reimbursements. Key benefits of these services include:
- Streamlined documentation processes
- Reduced claim denials
- Enhanced compliance with payer guidelines
Ultimately, adherence to these evolving standards is vital for sustaining financial viability in healthcare practices.
99441: Telephone Evaluation and Management Service
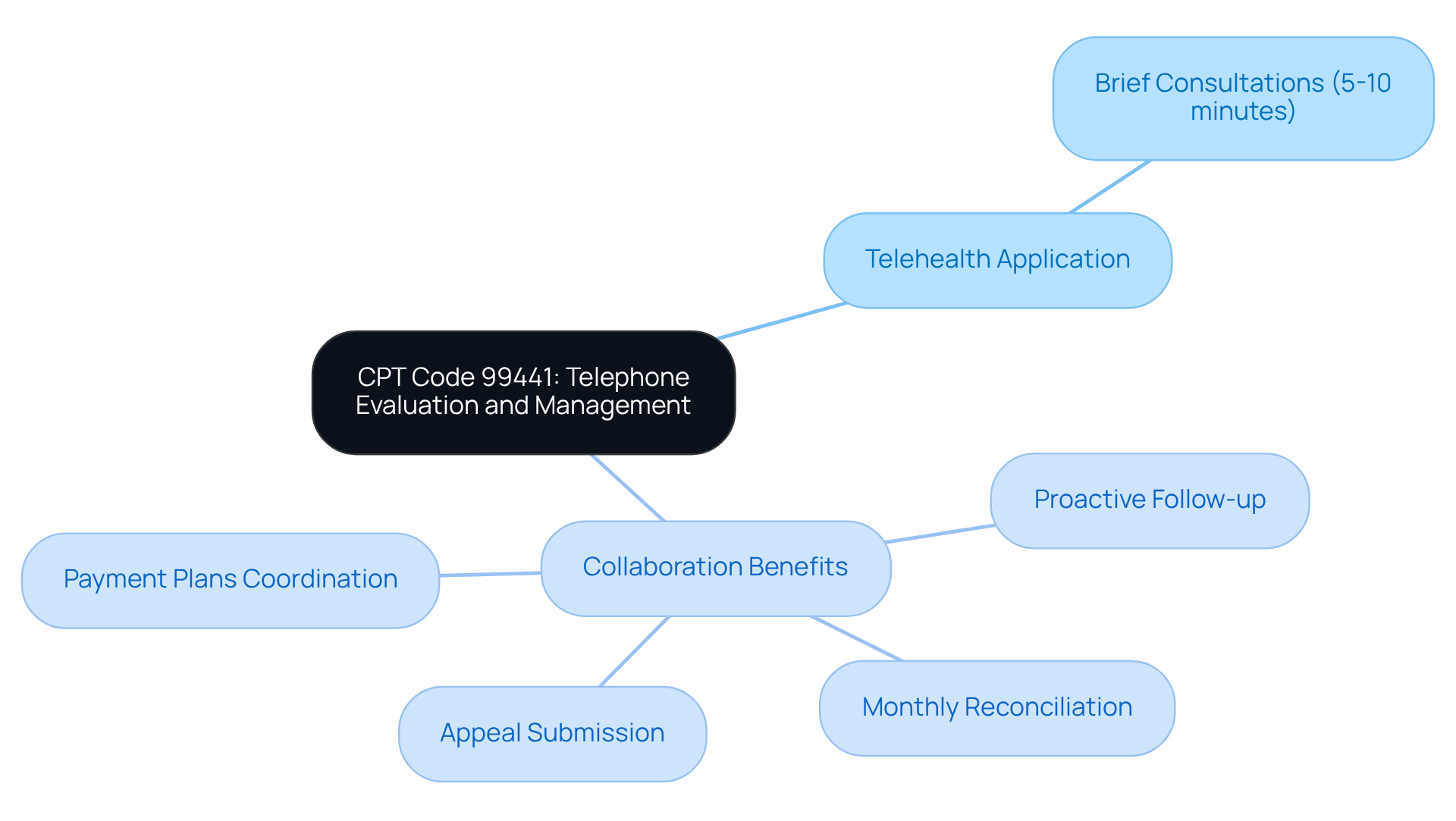
CPT designation 99441 serves as a critical tool for telephone evaluation and management services provided by healthcare professionals. This guideline applies to brief consultations of 5-10 minutes, allowing facilities to bill for essential follow-up discussions and patient inquiries. With the expansion of telehealth, effectively applying the telehealth CPT code is crucial for medical facilities to engage patients and secure reimbursement for their expertise.
By collaborating with Healthcare Partners Consulting, mental health facilities can optimize their operations and improve revenue cycle efficiency through comprehensive accounts receivable management solutions. Key benefits of this partnership include:
- Proactive follow-up with payers on unpaid or underpaid claims.
- Appeal submission for denied or incorrectly processed claims.
- Structured payment plans coordination to support patient financial needs.
- Monthly reconciliation and AR trending analysis for better financial oversight.
This collaboration not only supports the effective use of the telehealth CPT code 99441 but also reduces administrative burdens, ensuring that clinics can concentrate on delivering quality care while benefiting from enhanced cash flow and fewer denials. Ultimately, this partnership empowers clinics to enhance their financial health while prioritizing patient care.
99415: Prolonged Service in the Office or Other Outpatient Setting
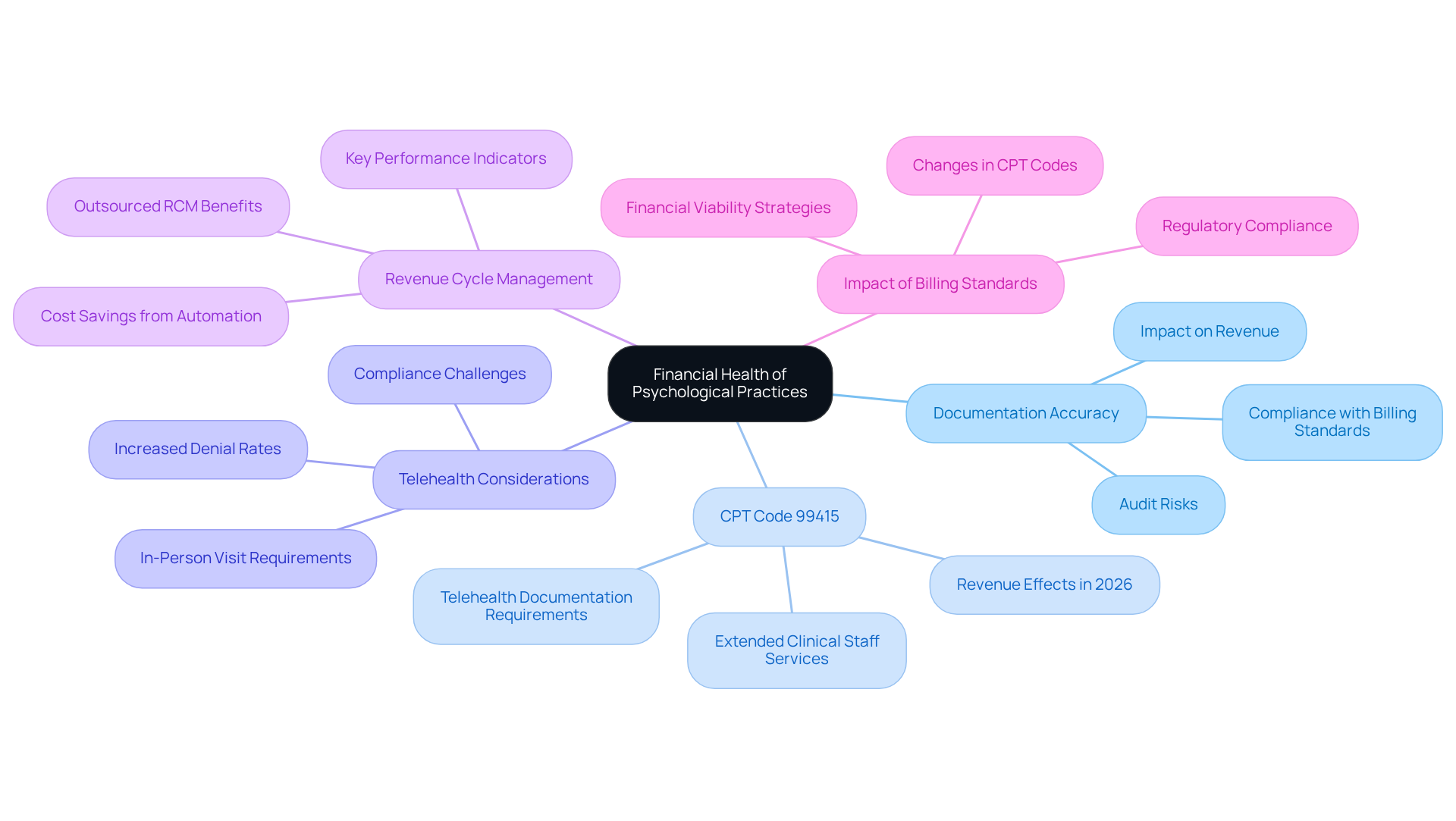
Inaccurate documentation can jeopardize the financial health of psychological practices. CPT designation 99415 is assigned for extended clinical staff services during evaluation and management in office or outpatient settings. This guideline applies when the total time spent exceeds the typical duration for the highest level of service billed.
For psychological care facilities, accurate records of the time spent on patient support are vital, as they directly affect income. Accurate recording is crucial for billing extended consultations. These consultations are often essential in therapeutic contexts.
In 2026, the revenue effect of using CPT code 99415 can be significant, especially as psychological practices adjust to changing billing standards and strive to enhance their financial outcomes. Considering that many psychological consultations now take place through telehealth, ensuring adherence to the telehealth CPT code documentation requirements is crucial for optimizing reimbursement and maintaining practice operations.
Wellness centers can enhance revenue by adopting comprehensive revenue cycle management strategies. Outsourced RCM from Healthcare Partners Consulting can deliver operational cost savings of 30-40% compared to in-house billing departments, while also providing tailored coding support and quality assurance processes.
Furthermore, with telehealth denials increasing by 84% in 2025, healthcare facilities must prioritize precise documentation to reduce potential revenue loss. By utilizing professional psychological and behavioral billing services, clinics can ensure compliance, accuracy, and ultimately, revenue optimization.
Ultimately, the financial viability of practices hinges on meticulous documentation and adherence to billing standards.
90791: Psychiatric Diagnostic Evaluation
CPT identifier 90791 plays a critical role in psychiatric diagnostic evaluations, necessitating a comprehensive understanding for effective reimbursement. This code is specifically for the initial intake appointment, excluding other medical services. Grasping the requirements for this code is vital for wellness facilities to ensure they are reimbursed for the crucial assessments that guide treatment choices and patient care approaches.
Collaborating with Healthcare Partners Consulting enables mental wellness clinics to streamline operations and reduce administrative burdens in billing and coding. Their comprehensive administrative support, including a credentialing toolkit that simplifies the credentialing process and ensures compliance, allows therapists and behavioral health groups to focus on providing quality care while optimizing revenue cycle management.
Ultimately, this partnership empowers clinics to prioritize patient care while ensuring financial sustainability.
90853: Group Psychotherapy
The CPT designation 90853 plays a pivotal role in the billing process for group psychotherapy sessions. This code is assigned when a therapist delivers treatment to multiple patients simultaneously. It is suitable for sessions lasting 46-60 minutes and is essential for facilities that incorporate group therapy into their treatment methods. Proper documentation of the session’s content and participant engagement is crucial for effective billing. This ensures compliance and maximizes reimbursement.
At Healthcare Partners Consulting, we emphasize accurate coding as the foundation of timely reimbursement. Our certified medical billing experts are trained in the nuances of behavioral care coding, ensuring that every claim submitted reflects the services provided and adheres to payer-specific guidelines. Our tailored coding support helps mental health clinics minimize claim denials and improve revenue cycle management. Ultimately, precise coding practices can significantly impact the financial health of mental health facilities.
90846: Family Therapy without the Patient Present
The CPT designation 90846 plays a critical role in family psychotherapy, particularly when the patient is not present. This guideline applies to sessions lasting a minimum of 50 minutes and is crucial for understanding family dynamics that influence the patient’s treatment.
Mental health facilities must ensure that documentation reflects the session’s focus and the involvement of family members to justify billing this classification and enhance treatment outcomes. Inadequate documentation can result in denied claims and delayed reimbursements.
Accurate coding is vital for ensuring timely reimbursement and compliance, which directly impacts the revenue cycle management of your practice. Partnering with Healthcare Partners Consulting enables clinics to achieve compliance and optimize revenue through expert medical billing solutions.
Ultimately, effective billing practices can transform the financial health of your practice.
99213: Established Patient Office Visit for Medication Management
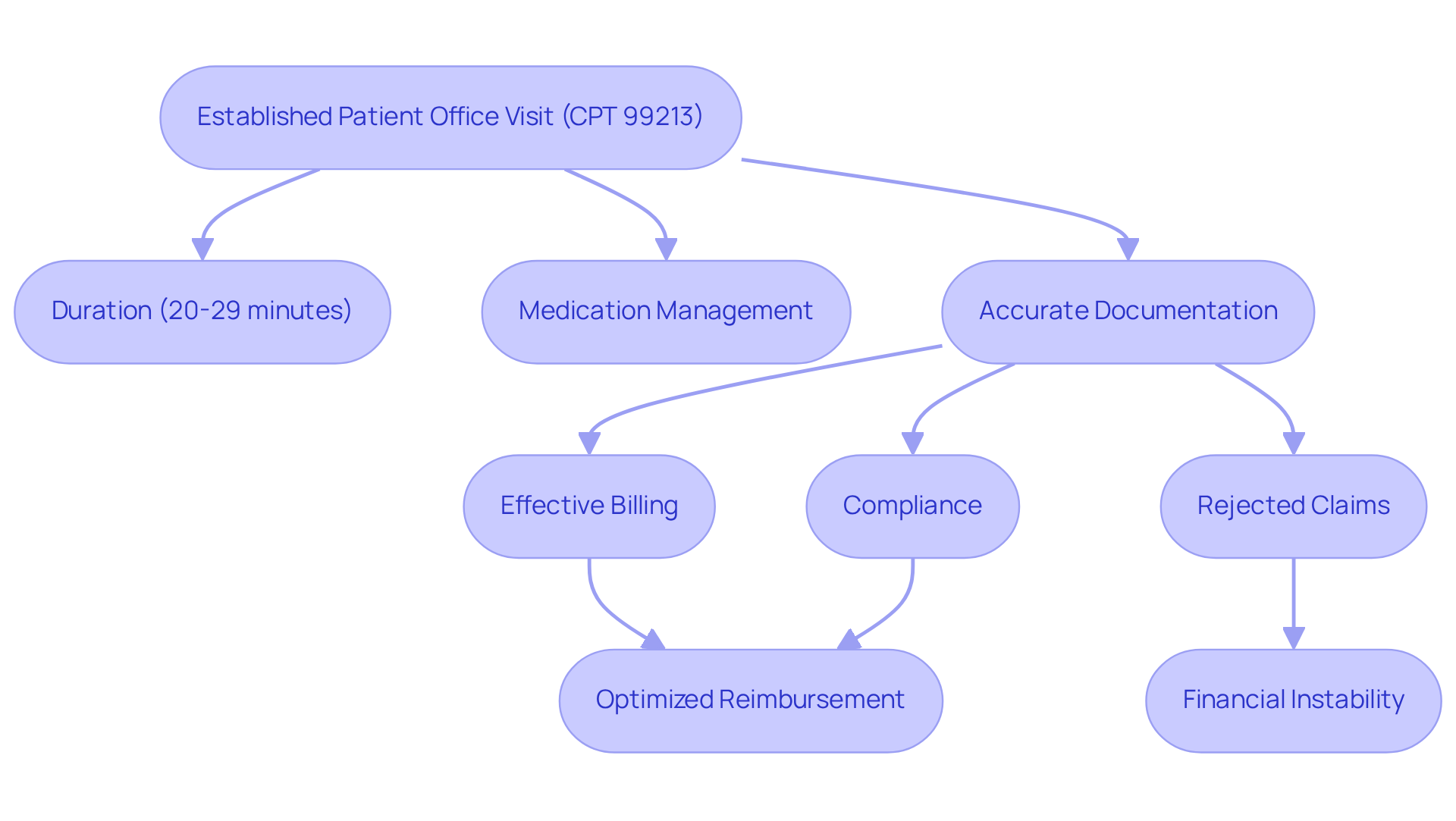
CPT designation 99213 is critical for established patient office visits, particularly those focused on evaluation and management, typically lasting between 20 to 29 minutes. This code is crucial for medication management visits, enabling clinicians to evaluate treatment responses and make necessary adjustments.
Accurate documentation of visit content and time spent is essential for effective billing, ensuring compliance with regulations and optimizing reimbursement for patient care. With a 45% rise in psychological support receipt among young adults from 2019 to 2022, the need for precise documentation in billing practices is more crucial than ever.
Incorrect documentation can lead to rejected claims, jeopardizing the financial stability of practices. Healthcare Partners Consulting highlights that 43% of insured adults with psychological concerns did not receive the treatment they believed they required in the past year, demonstrating the wider consequences of documentation errors on patient care and practice sustainability.
Thus, ensuring precise documentation is not merely a compliance issue; it is fundamental to sustaining both practice viability and patient care quality.
99442: Online Evaluation and Management Service
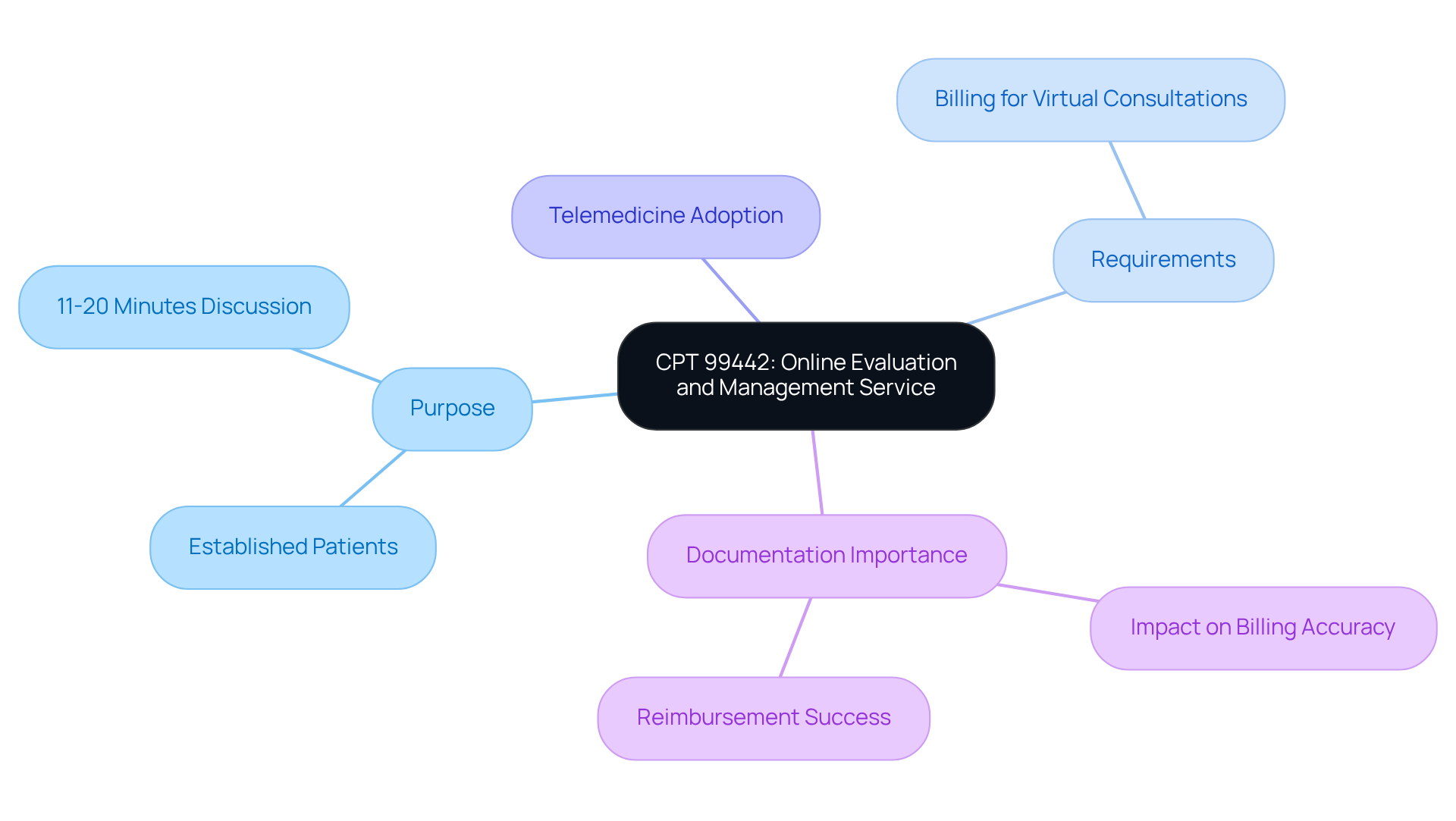
CPT 99442 serves as a pivotal code for online evaluation and management services, specifically designed for established patients and requiring 11-20 minutes of medical discussion. This telehealth CPT code reflects the increasing adoption of telemedicine in psychological services, enabling facilities to bill for virtual consultations that enhance patient access to care. Thorough documentation of online interactions is essential, as it directly impacts billing accuracy and reimbursement success.
Healthcare Partners Consulting: Streamlining Telehealth Billing Processes
Navigating the complexities of billing and reimbursement can be a daunting task for psychological practices. Healthcare Partners Consulting (HPC) helps clinics navigate the intricate landscape of coding and reimbursement, ensuring adherence to regulations while maximizing revenue potential. Their specialized knowledge in medical billing, combined with a commitment to a people-first approach, allows healthcare providers to concentrate on patient care rather than administrative tasks.
HPC offers comprehensive accounts receivable management solutions. These include:
- Proactive follow-up on unpaid claims
- Appeal submissions for denied claims
- Coordination of structured payment plans
All of which enhance revenue cycle efficiency. As a result, clinics utilizing HPC’s services have reported significant improvements in operational efficiency, with many experiencing revenue increases of up to 30%.
Furthermore, behavioral wellness providers lose up to 20% of potential revenue due to preventable billing mistakes, highlighting the essential role HPC plays in avoiding such losses. By mitigating billing errors, HPC not only safeguards revenue but also empowers mental health providers to prioritize patient care, effectively addressing the ongoing mental health billing crisis.
Conclusion
For mental health clinics, mastering telehealth CPT codes is essential to ensure effective billing and financial stability. Understanding the essential telehealth CPT codes is crucial for mental health clinics aiming to optimize their billing practices and ensure financial sustainability. As mental health services change, coding requirements for reimbursement also evolve. This article has outlined ten vital CPT codes that every mental health clinic should be familiar with, highlighting the importance of accurate documentation, adherence to updated guidelines, and the importance of specialized billing services in managing these coding challenges.
Key insights discussed include the specifics of each CPT code, from initial patient visits to ongoing therapy sessions, and the implications of these codes for billing and compliance. Accurate record-keeping is crucial, as billing errors can significantly impact finances. Clinics that focus on these areas are more likely to get timely reimbursements and stay financially healthy.
In light of the increasing reliance on telehealth services, mental health providers are encouraged to adopt comprehensive revenue cycle management strategies. Collaborating with experts can significantly enhance billing efficiency, reduce claim denials, and ultimately allow providers to focus on delivering quality care. By implementing these strategies, clinics can not only enhance their financial health but also improve patient care outcomes.
Frequently Asked Questions
What is the significance of CPT designation 99201?
CPT designation 99201 was important for new patient office visits requiring straightforward medical decision-making, but it was removed as of January 1, 2021. This change poses challenges for clinics adapting to new billing systems.
What was the typical duration and process for a visit classified under CPT 99201?
A visit under CPT 99201 typically involved a brief history and examination lasting about 10 minutes.
What are the key aspects of CPT designation 99202?
CPT designation 99202 defines parameters for established patient office visits requiring a medically appropriate history and/or examination, lasting between 15 and 29 minutes, and involving straightforward medical decision-making.
Why is accurate record-keeping important for psychological facilities under CPT 99202?
Accurate record-keeping is crucial for validating billing for CPT 99202, ensuring compliance with payer requirements, and optimizing reimbursement for ongoing patient care.
What challenges may wellness clinics face regarding new CPT codes introduced in 2026?
Wellness clinics may struggle to maintain healthy revenue streams without effective documentation and adherence to new CPT codes, especially those that create billing opportunities for practices utilizing digital tools.
How can Healthcare Partners Consulting assist healthcare facilities?
Healthcare Partners Consulting provides tailored revenue cycle management services to enhance financial health, streamline documentation processes, reduce claim denials, and ensure compliance with payer guidelines.
What is CPT designation 99441 used for?
CPT designation 99441 is used for telephone evaluation and management services, allowing healthcare professionals to bill for brief consultations of 5-10 minutes.
How does the expansion of telehealth impact billing practices?
The expansion of telehealth necessitates the effective application of telehealth CPT codes, which is crucial for medical facilities to engage patients and secure reimbursement.
What are the benefits of collaborating with Healthcare Partners Consulting for mental health facilities?
Benefits include proactive follow-up on unpaid claims, appeal submissions for denied claims, structured payment plan coordination, and monthly reconciliation for better financial oversight.
What overall benefits do healthcare facilities gain from enhanced coding assistance and revenue cycle strategies?
Facilities can enhance their financial health, ensure timely reimbursements, reduce administrative burdens, and focus more on delivering quality patient care.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting