Optimizing Practice Operations
Master RCM World Trends to Boost Your Mental Health Practice
Introduction
Mental health practices often grapple with financial sustainability as they adapt to rapid changes in the healthcare landscape. The industry is adapting to trends such as telehealth, automation, and value-based care. Mental health providers encounter both challenges and opportunities to enhance their operations. Effective navigation of RCM is essential for these practices to thrive amidst ongoing changes.
Understand the Fundamentals of Revenue Cycle Management
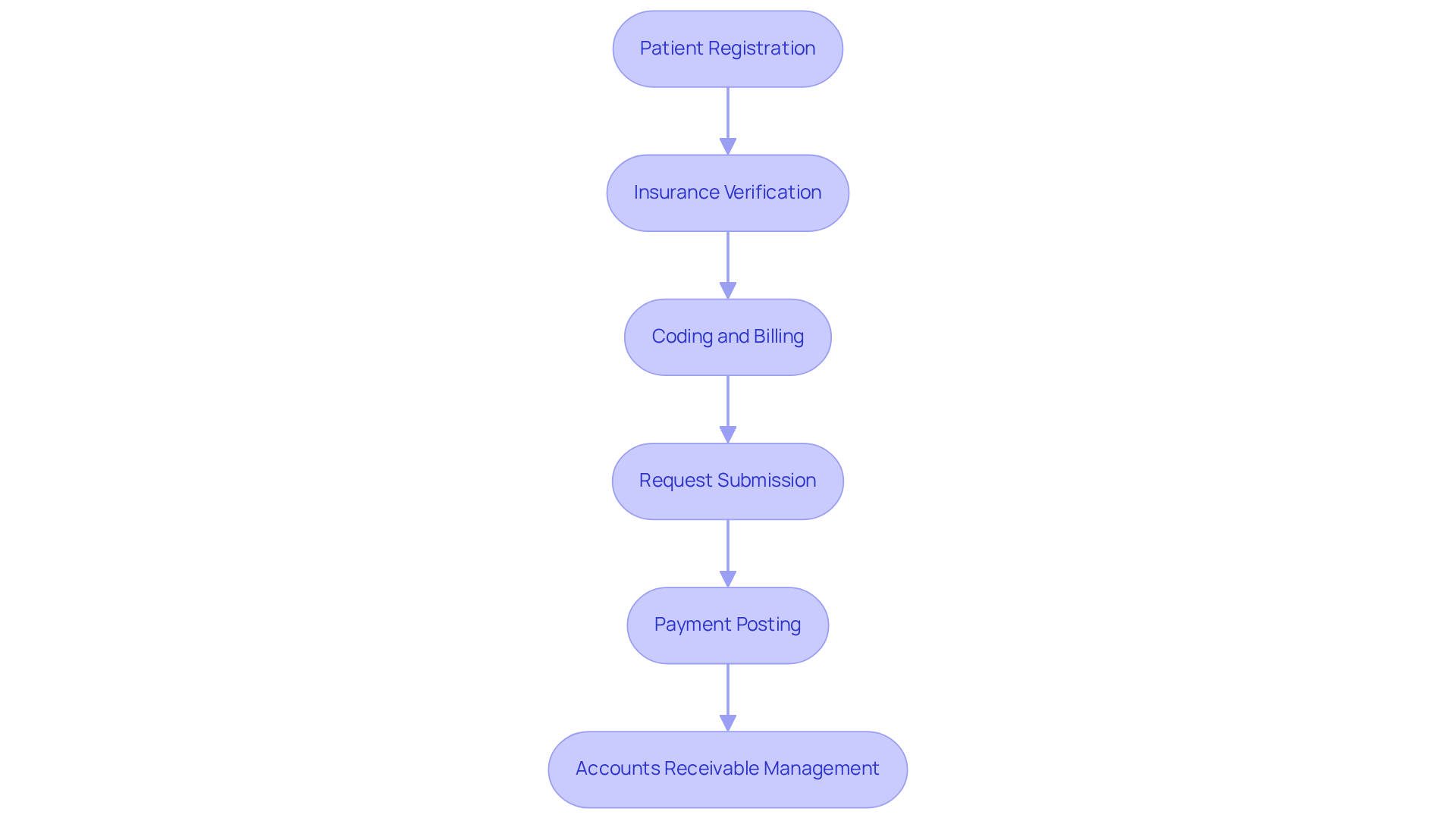
In the complex landscape of healthcare finance, effective Revenue Cycle Management (RCM) is essential for ensuring the sustainability of mental health practices. RCM encompasses the complete financial process of a healthcare facility, from client registration to the final payment for services provided. For mental health practices, understanding RCM involves several key components:
- Patient Registration: Accurate data collection at the outset is crucial for smooth billing processes. This involves confirming insurance details and comprehending the demographics of individuals receiving care. Almost 40% of denial occurrences stem from front-end mistakes, highlighting the necessity for careful registration methods.
- Insurance Verification: Verifying patient insurance coverage prior to services being delivered assists in avoiding denial of payments and guarantees that the facility is compensated for services rendered. Practices that verify eligibility before every session can collect 94 to 97 percent of their earned revenue, underscoring the financial benefits of proactive verification.
- Coding and Billing: Proper coding of services is essential for accurate billing. Mental health practices must be familiar with specific codes related to mental health services to avoid errors that can lead to delayed payments. Systematic coding inaccuracies can result in revenue impacts exceeding $60,000 per clinician annually, emphasizing the importance of precise documentation.
- Request Submission: Submitting requests swiftly and precisely is essential for sustaining cash flow. Practices should have a streamlined process for submitting requests to insurance companies. Delays in submission can stall cash flow significantly, with practices potentially facing $5,000 to $8,000 in stalled revenue monthly due to unsubmitted requests.
- Payment Posting: Once payments are received, they must be accurately posted to patient accounts to maintain financial records and ensure transparency. This step is vital for tracking revenue and managing accounts receivable effectively.
- Accounts Receivable Management: Monitoring outstanding requests and following up on unpaid invoices is vital for maintaining a healthy revenue stream. Healthcare Partners Consulting offers comprehensive accounts receivable management solutions, including structured payment plans coordination and dedicated AR specialists assigned to your account. Practices that actively manage denials within 72 hours can collect 94 to 97 percent of their earned revenue, underscoring the critical role of accounts receivable management. HPC’s proactive follow-up with payers on unpaid claims and appeal submissions for denied claims significantly enhances cash flow and reduces staffing burdens.
By prioritizing these RCM fundamentals, mental health practices can secure their financial future and enhance the quality of care they provide to their patients in alignment with RCM world trends.
Identify Key Trends Shaping RCM in Healthcare
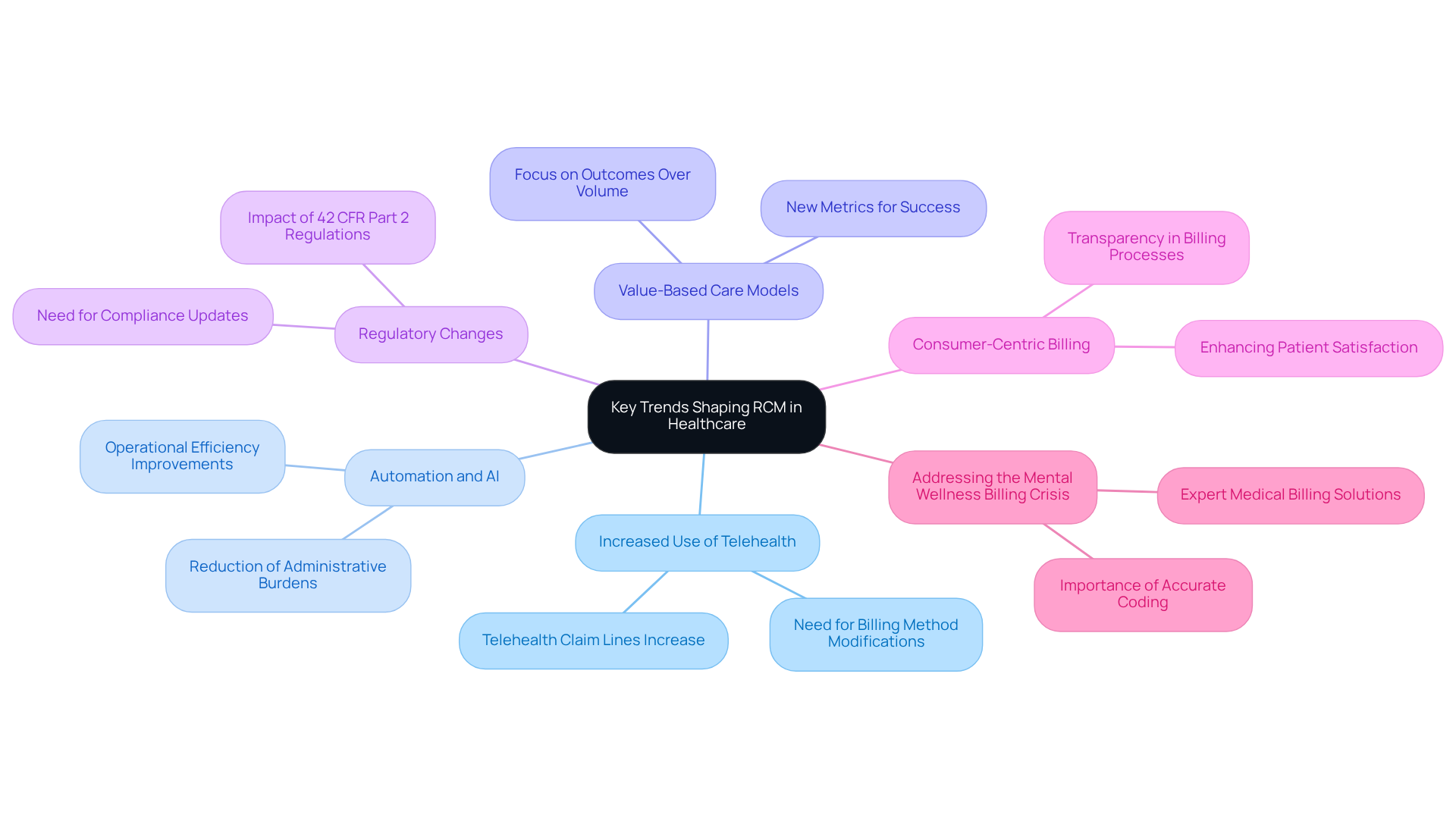
The landscape of Revenue Cycle Management in healthcare is evolving, driven by several key trends that demand attention from mental health practices:
- Increased Use of Telehealth: The adoption of telehealth services has transformed the delivery of mental health care. Providers must modify their billing methods to accommodate virtual visits, requiring a thorough understanding of telehealth reimbursement policies. Recent data shows a rise in telehealth claim lines from 4.73 percent in March to 4.86 percent in April, indicating a 2.7 percent increase in utilization.
- Automation and AI: The integration of automation and artificial intelligence into RCM processes is revolutionizing operational efficiency, minimizing errors, and accelerating payment cycles. Practices that implement these technologies can significantly enhance efficiency according to RCM world trends. For example, AI tools are now converting narrative documentation into structured, payer-ready formats, improving billing accuracy and reducing administrative burdens.
- Value-Based Care Models: As healthcare transitions to value-focused care, mental health providers must adjust their RCM strategies in line with RCM world trends, emphasizing outcomes over service volume to align with evolving reimbursement models. This transition necessitates developing new metrics for measuring success and reimbursement, aligning financial incentives with quality care delivery.
- Regulatory Changes: Ongoing changes in healthcare regulations significantly impact billing and compliance requirements. Staying informed about the RCM world trends is essential for avoiding penalties and ensuring smooth operations. For example, the complete implementation of revised 42 CFR Part 2 regulations is scheduled to commence on February 16, 2026, requiring modifications in compliance methods.
- Consumer-Centric Billing: There is an increasing emphasis on transparency and consumer engagement in billing processes. Adopting patient-friendly billing methods not only enhances satisfaction but also fosters trust and supports prompt payments, ultimately benefiting financial wellbeing.
- Addressing the Mental Wellness Billing Crisis: Insights from industry experts, including Davia Ward, emphasize the critical need for accurate coding and compliance to navigate the ongoing challenges in mental wellness billing effectively. Healthcare Partners Consulting specializes in delivering expert medical billing solutions customized for mental and behavioral wellness providers, ensuring compliance and enhancing revenue through accurate coding and strategic management of the revenue cycle.
By proactively adapting to RCM world trends, mental health practices can not only survive but also thrive in a challenging healthcare landscape.
Leverage Technology and Automation for Enhanced Efficiency
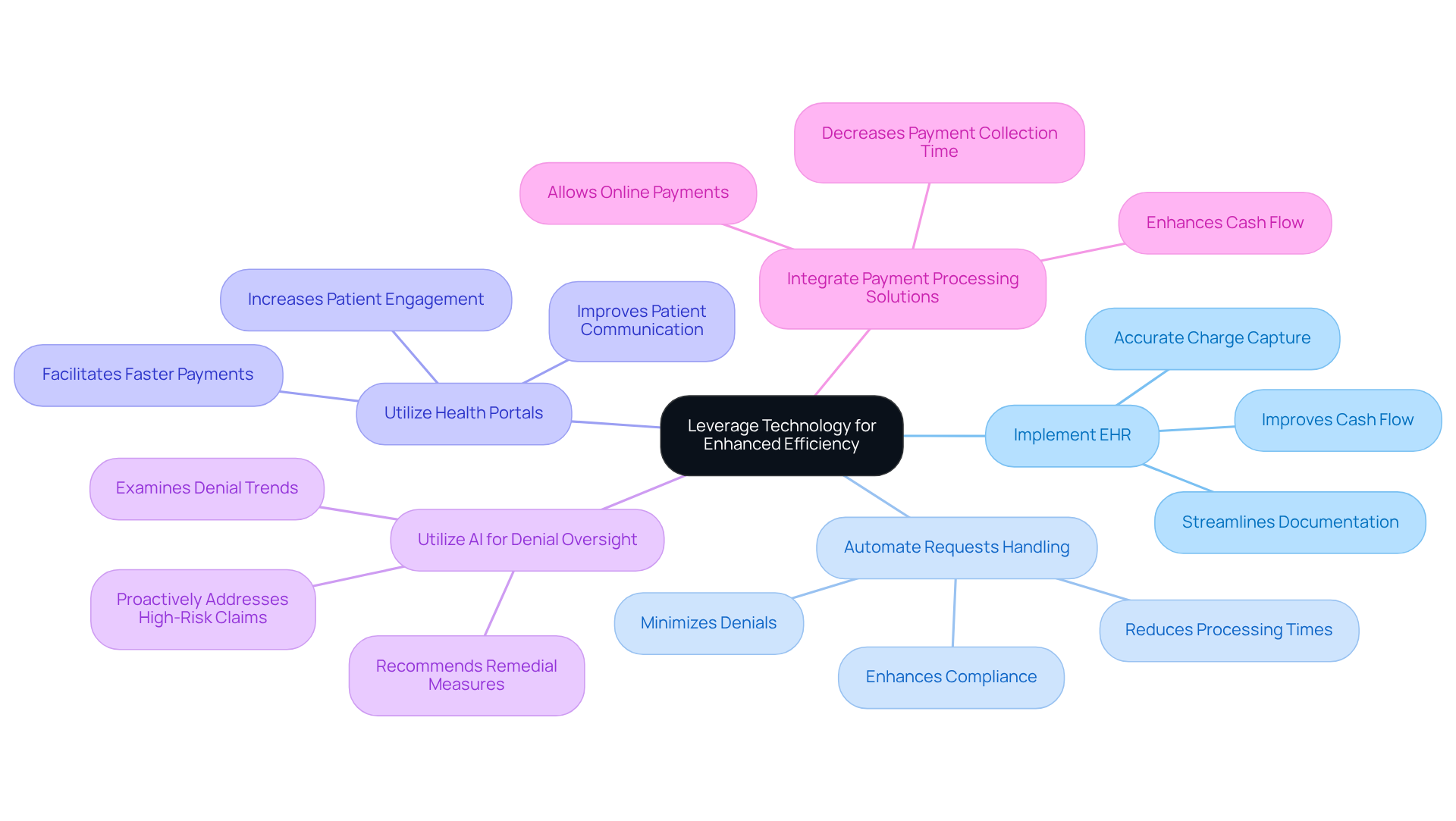
Incorporating technology into Revenue Cycle Management (RCM) presents a pivotal opportunity for mental health practices to enhance operational efficiency. Here are some strategies to consider:
- Implement Electronic Health Records (EHR): EHR systems streamline documentation and billing processes by integrating clinical and financial data. This captures all chargeable services accurately for reimbursement, which improves cash flow.
- Automate Requests Handling: Utilizing software that streamlines submission and tracking can reduce processing times from days to mere hours. Automated systems can flag potential issues before claims are submitted, minimizing denials and enhancing compliance. Claims often face denials due to overlooked issues, leading to delays and lost revenue.
- Utilize Health Portals: Health portals improve communication and enable individuals to view their billing details, make payments, and manage appointments. This transparency can lead to improved patient satisfaction and faster payments, as patients are more engaged in their financial responsibilities.
- Utilize AI for Denial Oversight: AI resources can examine trends in denial occurrences and recommend remedial measures, assisting organizations in lowering the frequency of rejected submissions. By leveraging predictive analytics, organizations can proactively address high-risk claims, enhancing overall revenue.
- Integrate Payment Processing Solutions: Streamlining payment processing through integrated solutions can enhance cash flow by allowing patients to pay their bills online. This decreases the time required to gather payments and enhances the overall financial condition of the business.
Ultimately, embracing these technological advancements not only improves financial outcomes but also allows practices to prioritize patient care more effectively.
Consider Outsourcing RCM Functions for Operational Relief
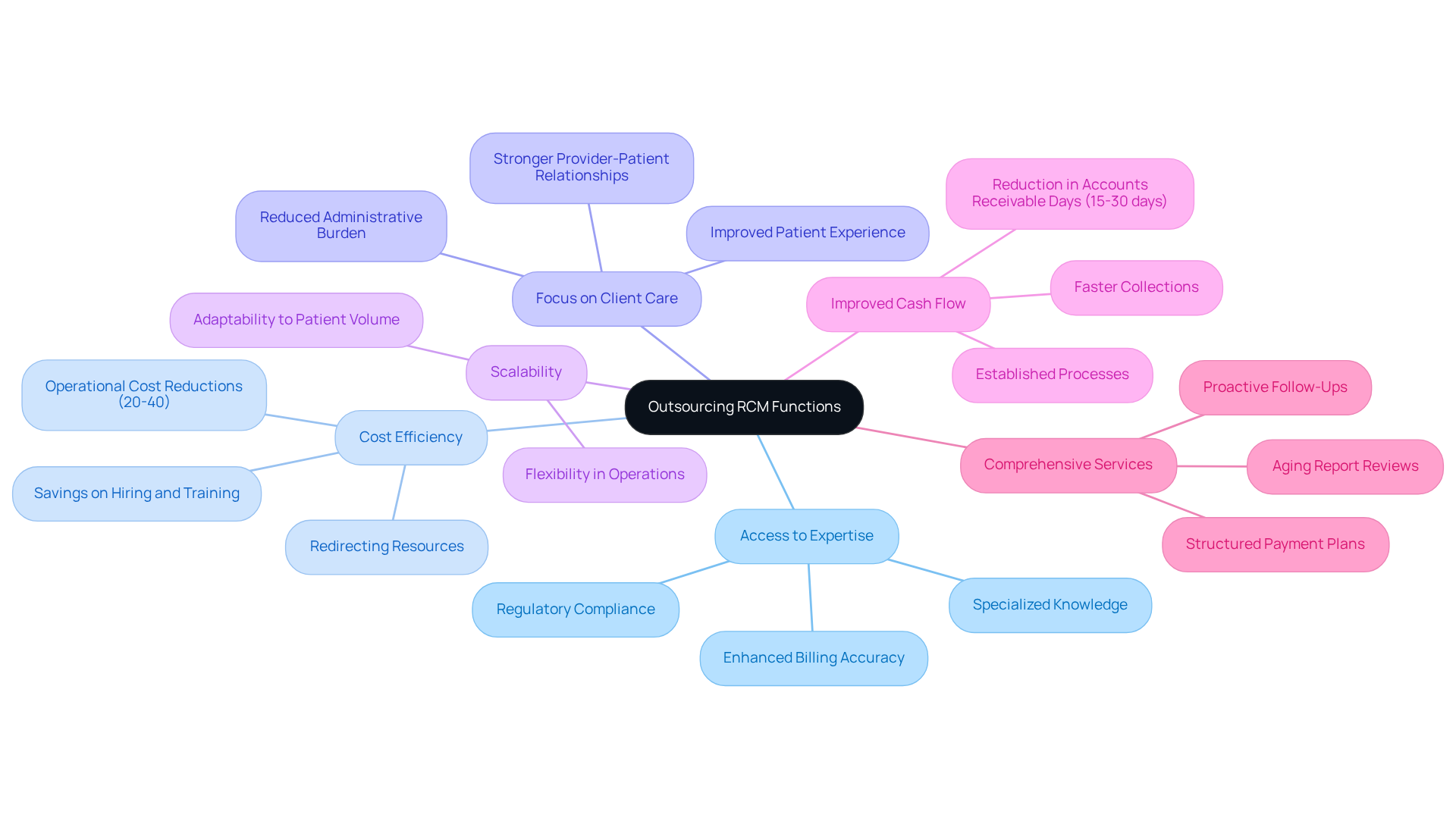
Outsourcing Revenue Cycle Management (RCM) functions presents a strategic opportunity for mental health providers to enhance operational efficiency, reflecting the current RCM world trends. Here are some key considerations and benefits:
- Access to Expertise: Outsourcing RCM to Healthcare Partners Consulting allows organizations to tap into specialized knowledge and skills that might not exist within their teams. This expertise can significantly enhance billing accuracy and ensure compliance with ever-evolving regulations.
- Cost Efficiency: Outsourcing can result in significant cost savings, with healthcare organizations reporting operational cost reductions of 20% to 40% compared to in-house RCM departments. This reduction comes from cutting costs associated with hiring, training, and software licensing, enabling practices to redirect resources to other essential areas. Industry experts emphasize that ‘While outsourcing seems like an added expense, it often saves money in the long run’ (Revantage Billing).
- Focus on Client Care: With administrative burdens alleviated, mental health providers can dedicate more time to client care rather than billing and collections. This shift not only improves the experience of individuals receiving care but also promotes stronger provider-individual relationships.
- Scalability: Outsourcing provides the adaptability to modify RCM operations according to the organization’s needs, accommodating fluctuations in patient volume without requiring substantial staffing changes. This adaptability is crucial for methods facing seasonal variations or unexpected surges in demand.
- Improved Cash Flow: Providers that outsource RCM to Healthcare Partners Consulting often benefit from established processes and advanced technologies that facilitate faster collections. For instance, practices can see a reduction in accounts receivable days by approximately 15 to 30 days, leading to improved cash flow and financial stability. A Texas-based psychiatry group, for instance, reduced denial rates by 42% after outsourcing their billing to HPC, illustrating the tangible benefits of this approach.
- Comprehensive Services: Healthcare Partners Consulting offers additional services such as aging report reviews, proactive follow-ups with payers on unpaid claims, and structured payment plans, which further enhance the efficiency of RCM processes.
By carefully evaluating these potential benefits, mental health practices can make informed decisions about outsourcing RCM functions that align with RCM world trends. Ultimately, this strategic choice can profoundly impact the financial health and operational success of mental health practices.
Conclusion
Navigating the complexities of Revenue Cycle Management (RCM) presents significant challenges for mental health practices striving for success in today’s healthcare landscape. By understanding the essentials of RCM, including patient registration, insurance verification, and coding, practices can improve their financial health while providing high-quality care to clients. Current trends, including telehealth and automation, highlight the need for practices to adapt their RCM strategies to ensure operational efficiency and compliance.
Key components and trends shaping RCM include:
- The necessity of accurate patient data
- Timely submissions
- Effective accounts receivable management
By leveraging technology and considering outsourcing options, mental health providers can streamline their processes, reduce costs, and focus more on patient care. The shift towards value-based care and consumer-centric billing models also calls for practices to rethink their RCM strategies to align with evolving industry standards.
Embracing effective Revenue Cycle Management principles secures financial viability while enhancing the overall patient experience. Prioritizing RCM is essential not only for financial stability but also for fostering a superior patient experience in a dynamic healthcare environment.
Frequently Asked Questions
What is Revenue Cycle Management (RCM) in healthcare?
Revenue Cycle Management (RCM) is the complete financial process of a healthcare facility, encompassing everything from client registration to the final payment for services provided.
Why is accurate patient registration important in RCM?
Accurate patient registration is crucial because it helps to ensure smooth billing processes and minimizes errors. Approximately 40% of denial occurrences stem from mistakes made during registration.
How does insurance verification contribute to RCM?
Verifying patient insurance coverage before services are delivered helps avoid payment denials and ensures that the facility is compensated for services rendered. Practices that verify eligibility before every session can collect 94 to 97 percent of their earned revenue.
What role does coding and billing play in RCM?
Proper coding of services is essential for accurate billing. Mental health practices must use specific codes related to mental health services to avoid errors that can lead to delayed payments. Inaccurate coding can result in significant revenue losses.
Why is timely request submission important?
Submitting requests quickly and accurately is vital for maintaining cash flow. Delays in submission can stall cash flow significantly, potentially leading to $5,000 to $8,000 in stalled revenue monthly.
What is the significance of payment posting in RCM?
Accurate posting of payments to patient accounts is essential for maintaining financial records and ensuring transparency, which is vital for tracking revenue and managing accounts receivable effectively.
How can accounts receivable management impact a mental health practice’s revenue?
Monitoring outstanding requests and following up on unpaid invoices is crucial for maintaining a healthy revenue stream. Active management of denials within 72 hours can help practices collect 94 to 97 percent of their earned revenue.
What services does Healthcare Partners Consulting offer for accounts receivable management?
Healthcare Partners Consulting provides comprehensive accounts receivable management solutions, including coordination of structured payment plans and dedicated AR specialists to enhance cash flow and reduce staffing burdens.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting