Mastering Medical Coding
Master Durable Medical Equipment Codes for Optimal Revenue Management

Introduction
Understanding the complexities of Durable Medical Equipment (DME) coding is essential for healthcare providers who seek to optimize their revenue management. The demand for DME is increasing, largely due to an aging population and a rise in chronic health conditions. This escalation underscores the necessity for accurate coding and billing practices. However, many providers encounter common pitfalls that can result in claim denials and financial setbacks. Therefore, how can healthcare practices effectively navigate the intricacies of DME coding to enhance their financial sustainability?
Define Durable Medical Equipment and Its Importance in Billing
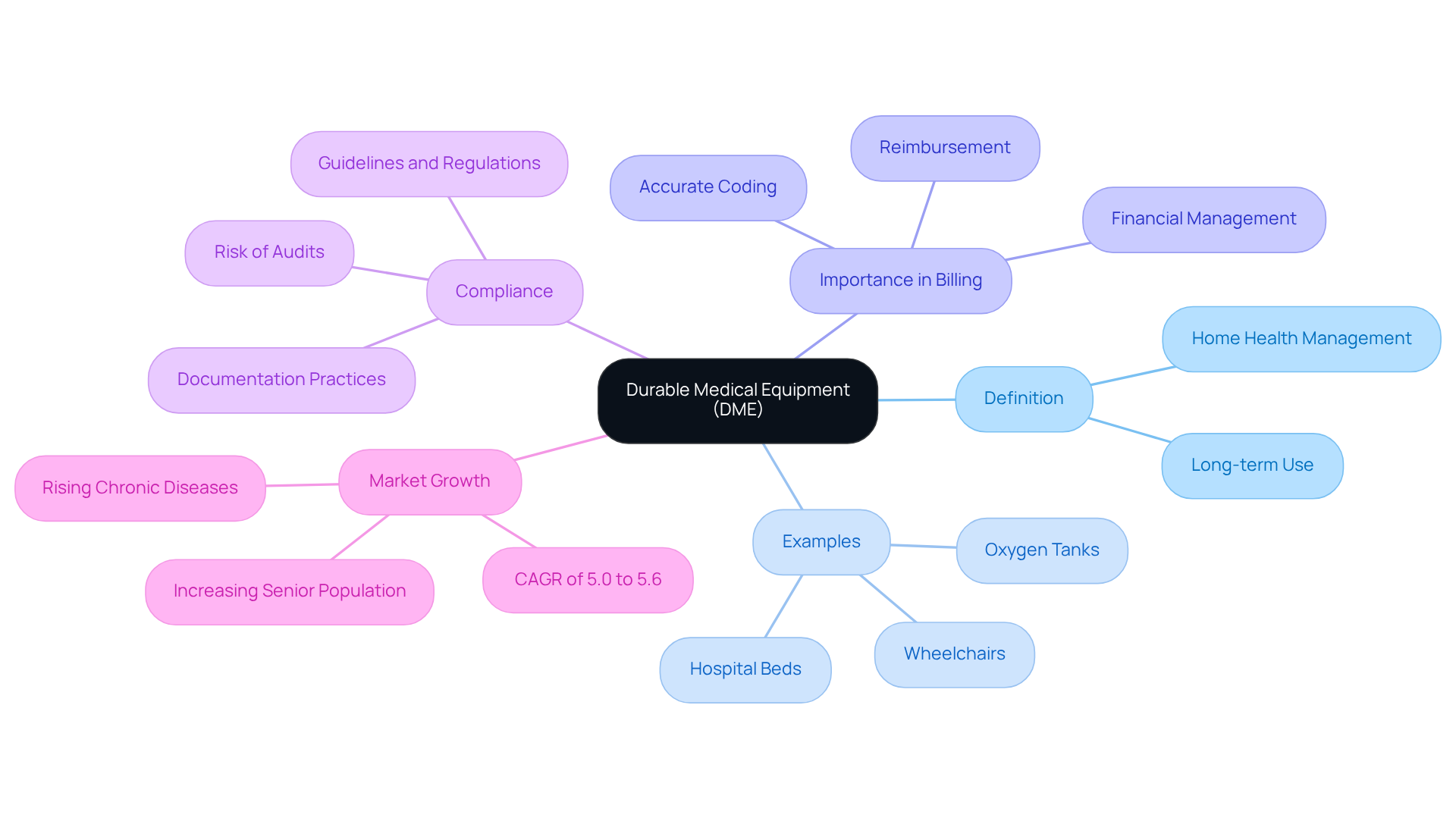
Durable Medical Equipment (DME) includes medical devices designed for long-term use, assisting patients in managing health conditions within their homes. Common examples of DME are wheelchairs, oxygen tanks, and hospital beds. For healthcare providers, a thorough understanding of DME is essential, as it significantly influences both patient care and the financial management of their practices.
Accurate identification and classification of durable medical equipment codes are vital to ensure that providers receive appropriate reimbursement for the services rendered, thereby enhancing revenue management. Inaccurate programming can lead to claim denials, increased administrative burdens, and financial losses, underscoring the necessity for providers to stay informed about guidelines and compliance requirements.
Furthermore, effective DME billing practices are crucial for maintaining compliance with healthcare regulations, thereby reducing the risk of audits and penalties. Healthcare Partners Consulting offers comprehensive accounts receivable management solutions that improve revenue cycle efficiency, enhance cash flow, and reduce denials through meticulous documentation practices. Their dedicated team actively follows up on unpaid or underpaid claims and coordinates structured payment plans, ensuring accuracy and compliance, which are essential for timely reimbursement.
As the U.S. DME market is projected to grow at a compound annual growth rate (CAGR) of 5.0% to 5.6% in the coming years-driven by an increasing senior population and the rising prevalence of chronic diseases-the significance of DME in healthcare delivery will only grow. Providers that prioritize accurate coding and invoicing processes will not only improve their revenue management but also enhance patient outcomes by ensuring timely access to durable medical equipment codes.
Understand HCPCS Codes for Durable Medical Equipment
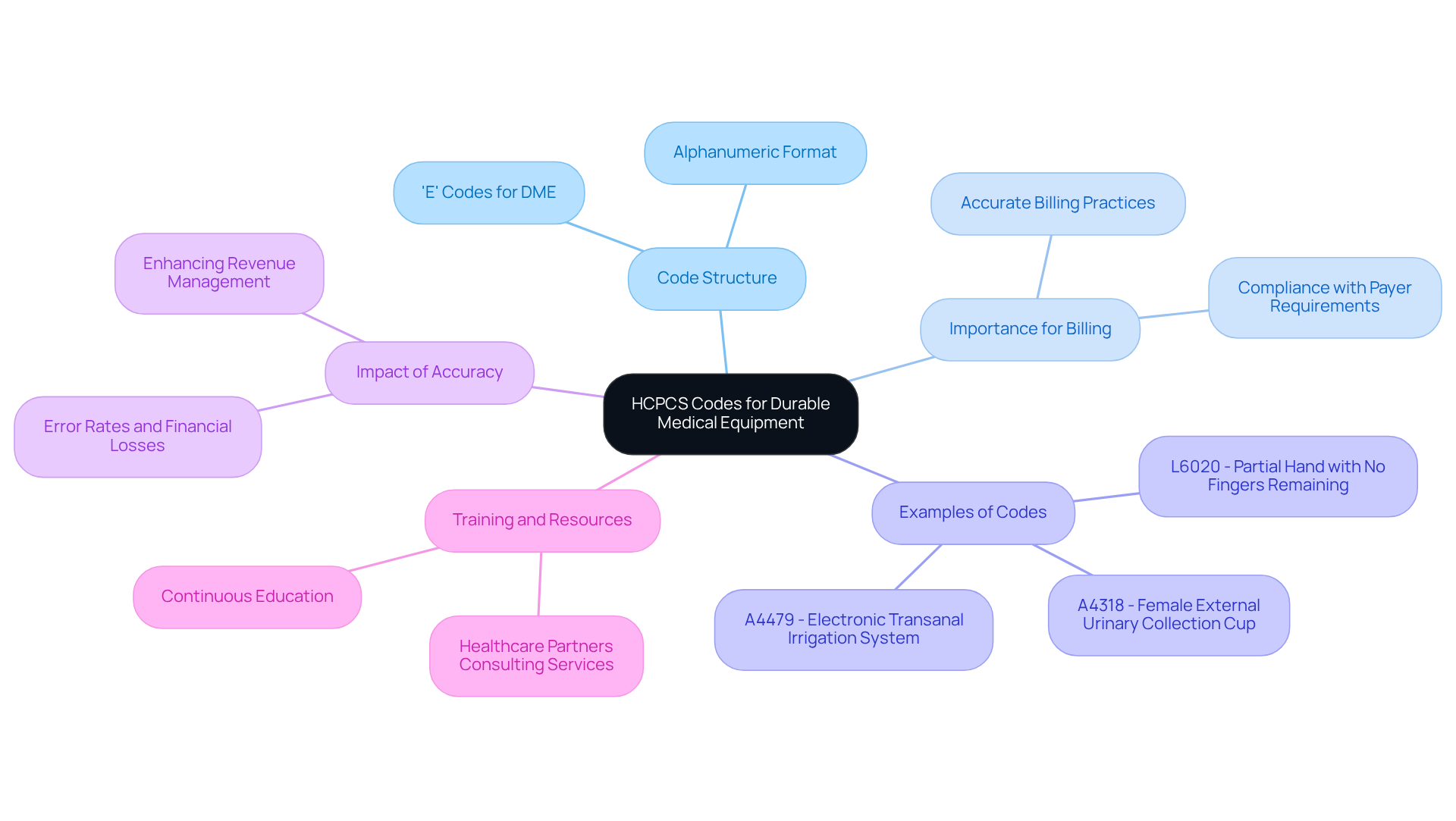
The Healthcare Common Procedure Coding System (HCPCS) is essential for identifying products, supplies, and services that are not covered by the Current Procedural Terminology (CPT). Within this framework, durable medical equipment codes are particularly important for HCPCS Level II invoicing. These alphanumeric codes, starting with a letter followed by four digits, categorize various types of equipment, with ‘E’ codes specifically assigned to durable medical equipment codes.
A precise understanding and application of these codes are crucial for healthcare providers to ensure accurate billing and compliance with payer requirements. For example, the introduction of new codes, such as A4318 for a female external urinary collection cup, highlights the ongoing evolution of DME classifications. Regular training and updates on HCPCS codes can significantly reduce error rates, which negatively impact revenue cycles. Studies have shown that high error rates in DME classification can result in substantial financial losses for healthcare providers, underscoring the importance of meticulous classification practices.
Healthcare coding specialists assert that accuracy in HCPCS Level II coding is not just a compliance issue; it is a critical factor in enhancing revenue management. By investing in continuous education and resources related to these codes, providers can improve their invoicing accuracy, ultimately fostering better financial sustainability and operational efficiency. Additionally, Healthcare Partners Consulting provides comprehensive services, including denial management and appeals, to recover underpaid or denied claims, ensuring that providers maximize their revenue potential.
Identify Common Errors in DME Coding and Billing
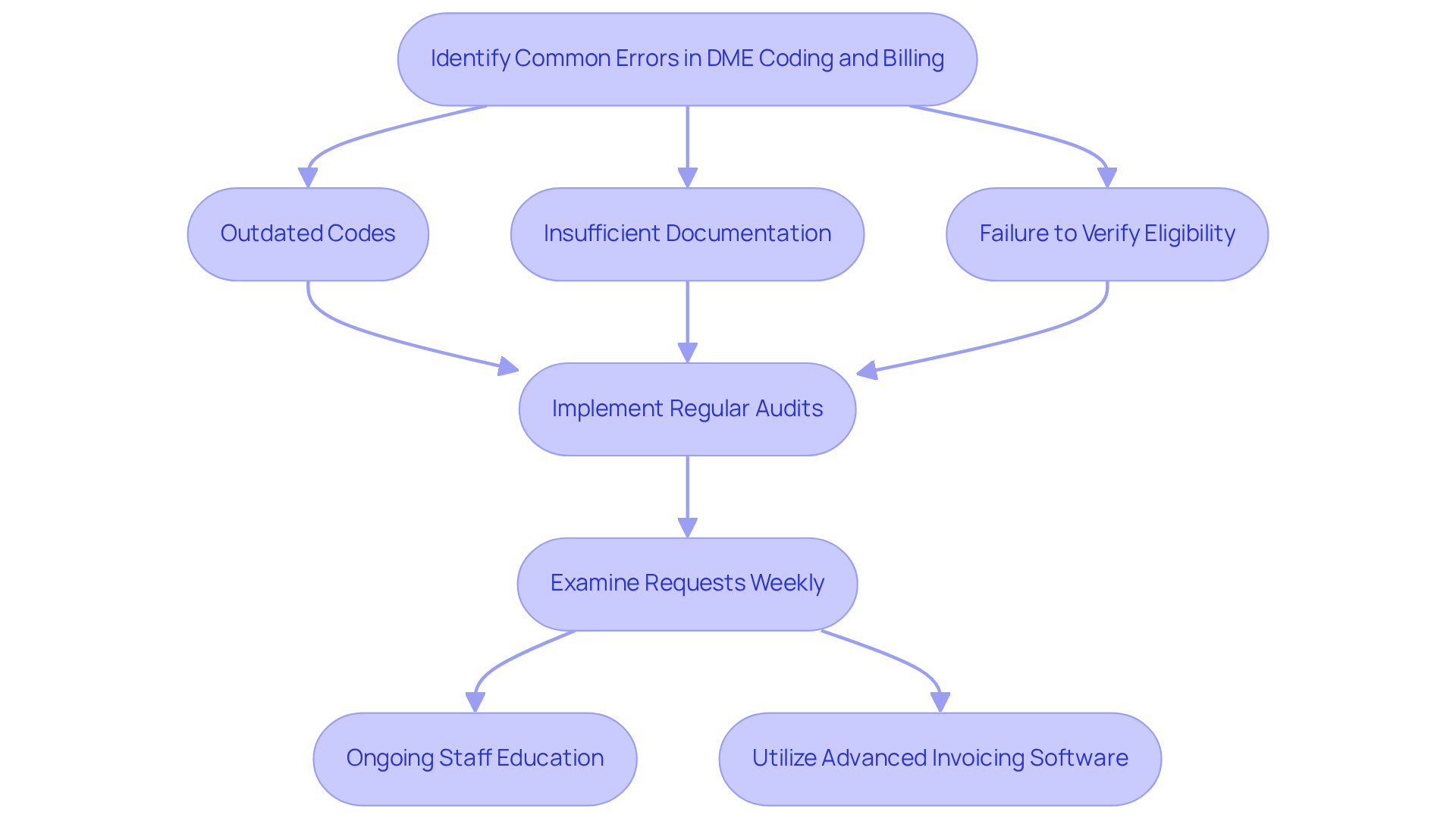
Common mistakes in durable medical equipment codes and invoicing can lead to significant revenue loss and compliance challenges. Errors often include:
- The use of outdated or incorrect durable medical equipment codes
- Insufficient documentation
- Failure to verify patient eligibility before invoicing
Notably, approximately 10-12% of medical requests are initially rejected due to avoidable invoicing mistakes, which adversely affects cash flow and operational effectiveness. Claim denials not only delay payments but also escalate administrative costs, diverting valuable resources away from patient care.
To mitigate these issues, healthcare providers should adopt a proactive approach by implementing regular audits of their billing processes. This entails examining a selection of requests weekly to identify trends in mistakes, such as missing modifiers or inaccurate labeling. Additionally, it is crucial to ensure that staff receive ongoing education on current classification practices, including the complexities of behavioral health and payer-specific guidelines, to maintain accuracy.
Utilizing advanced invoicing software that detects potential errors prior to submission can further enhance the accuracy of entries, ultimately leading to quicker payments and improved revenue cycle management. By concentrating on these strategies, healthcare practices can significantly diminish the financial repercussions of coding errors and bolster their overall operational efficiency.
Establish Documentation Requirements for DME Claims
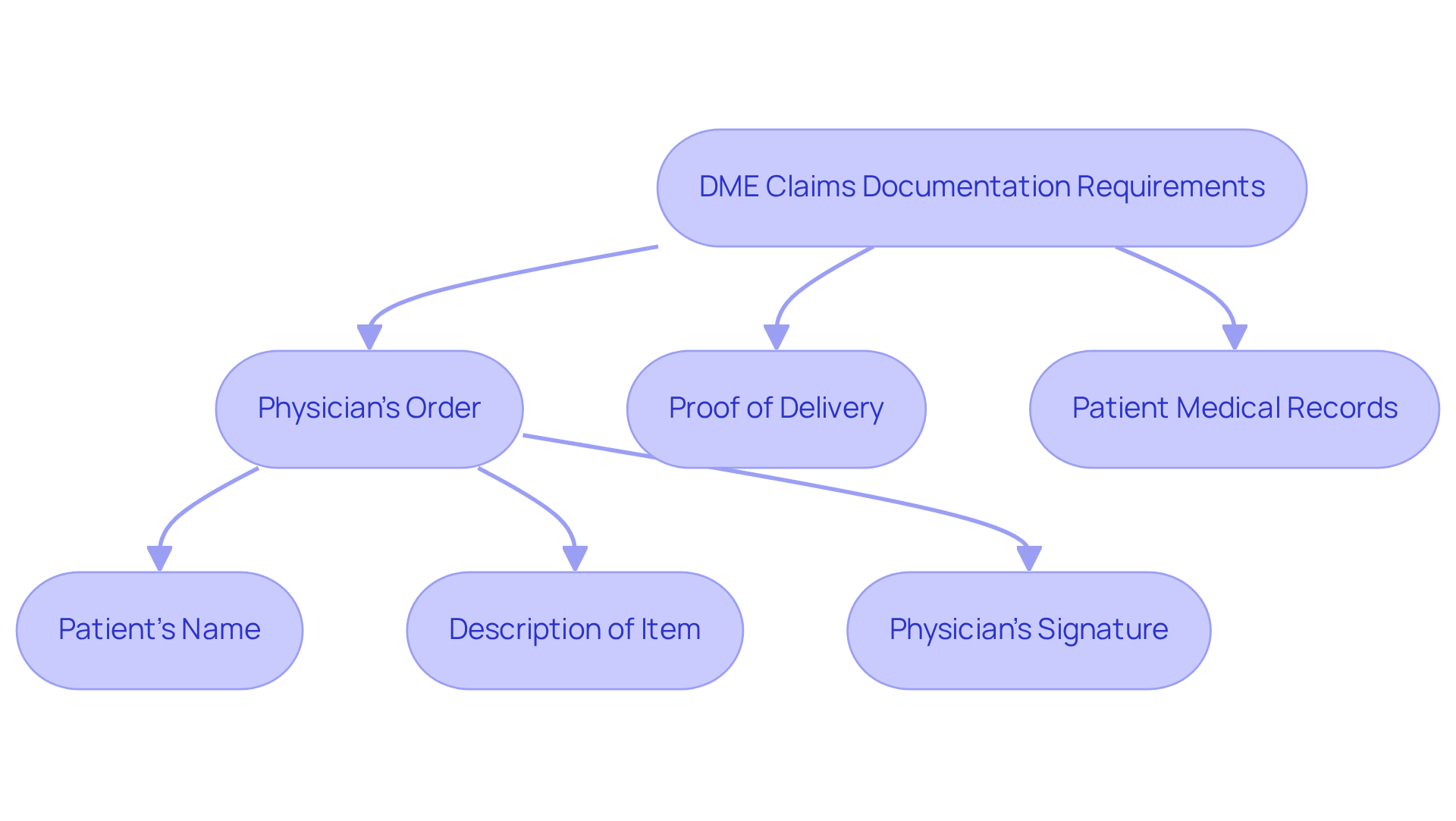
Documentation plays a pivotal role in the durable medical equipment codes billing process, significantly impacting the success of processing requests. Providers are required to maintain comprehensive records, which must include:
- A physician’s order
- Proof of delivery
- Detailed patient medical records that substantiate the necessity for the equipment
For example, Medicare mandates a Standard Written Order (SWO) for all DME requests. This order must encompass:
- The patient’s name
- A description of the item
- The physician’s signature
Accurate and current documentation not only facilitates smoother processing of requests but also serves a critical function during audits and appeals, allowing providers to effectively substantiate their submissions with durable medical equipment codes.
Entities that implement robust documentation practices can substantially reduce audit risks and improve the accuracy of their submissions. This, in turn, enhances revenue outcomes, underscoring the importance of meticulous record-keeping in the DME billing landscape.
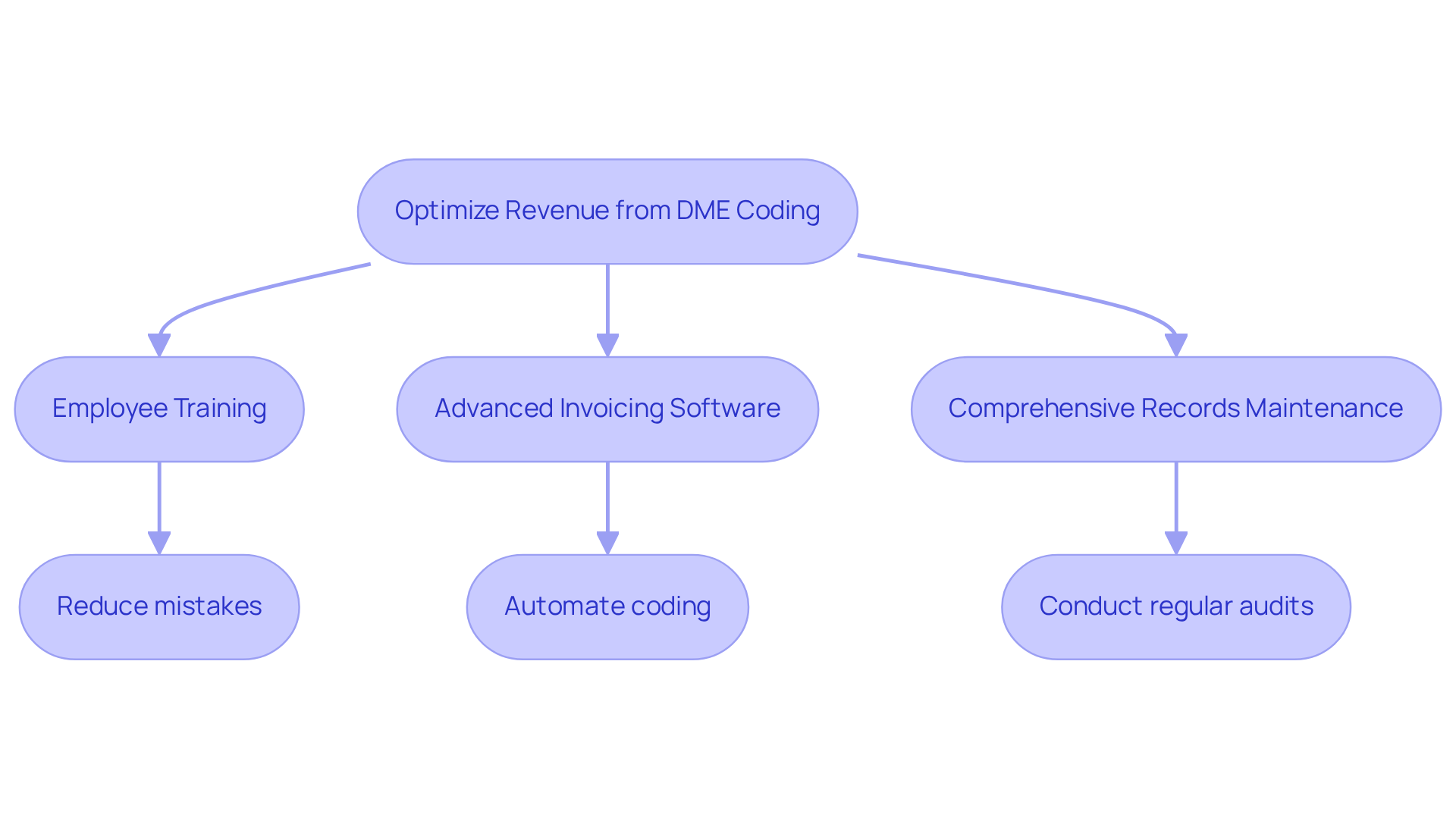
Implement Strategies to Optimize Revenue from DME Coding
To maximize revenue from durable medical equipment codes, healthcare providers must implement several essential strategies.
- Investing in thorough employee training on the latest programming techniques and payer requirements is crucial. This investment can significantly reduce mistakes and improve acceptance rates. Research indicates that 90% of rejections are avoidable with enhanced front-end procedures, which include precise classification and eligibility verification. Healthcare Partners Consulting underscores the importance of verifying insurance eligibility prior to providing DME, as this practice can minimize outstanding balances and enhance cash flow.
- Employing advanced invoicing software that automates coding and monitors claims can streamline the payment process, thereby enhancing accuracy and efficiency. Automation technologies can decrease invoicing mistakes by up to 60% compared to manual processes, resulting in quicker reimbursements and a 20% reduction in denials due to eligibility errors. HPC’s organized payment plans and dedicated accounts receivable specialists further facilitate this automation, ensuring that invoicing processes are both efficient and effective.
- Maintaining comprehensive records is vital for reducing denials, as inaccuracies can lead to significant financial repercussions. Regular audits of invoicing practices are necessary to identify errors and ensure compliance with evolving HCPCS codes and payer policies. Additionally, proactive follow-up with payers on unpaid or underpaid claims can further optimize revenue. For example, organizations that adopt proactive denial management strategies, such as those provided by HPC, can reduce denial rates by up to 75%, thereby optimizing revenue. By focusing on these best practices and leveraging HPC’s comprehensive medical billing solutions, healthcare providers can significantly enhance their overall financial performance and billing accuracy using durable medical equipment codes.
Conclusion
Mastering durable medical equipment (DME) coding is essential for healthcare providers who seek to optimize revenue management and enhance patient care. Accurate coding and billing practices not only ensure appropriate reimbursement but also play a critical role in compliance with healthcare regulations. As the demand for DME continues to grow, understanding the intricacies of coding and documentation becomes increasingly vital for maintaining financial health within healthcare practices.
This article has shared key insights regarding:
- The importance of accurate HCPCS coding
- Common errors that can lead to claim denials
- Essential documentation requirements that support successful billing
Implementing strategies such as:
- Ongoing staff training
- Utilizing advanced invoicing software
- Conducting regular audits
can significantly mitigate the risks associated with coding inaccuracies. By prioritizing these best practices, healthcare providers can enhance their revenue cycle management and improve overall operational efficiency.
In conclusion, the significance of mastering DME coding extends beyond financial implications; it directly impacts patient outcomes and access to necessary medical equipment. By investing in proper coding practices and staying informed about the latest updates in HCPCS codes, healthcare providers can ensure they are maximizing their revenue potential while delivering high-quality care to their patients. Embracing these strategies is essential for any provider aiming to thrive in the evolving landscape of durable medical equipment billing.
Frequently Asked Questions
What is Durable Medical Equipment (DME)?
Durable Medical Equipment (DME) refers to medical devices designed for long-term use to assist patients in managing health conditions at home. Common examples include wheelchairs, oxygen tanks, and hospital beds.
Why is understanding DME important for healthcare providers?
A thorough understanding of DME is essential for healthcare providers as it influences patient care and financial management. Accurate identification and classification of DME codes are vital for ensuring appropriate reimbursement and enhancing revenue management.
What are the consequences of inaccurate DME coding?
Inaccurate DME coding can lead to claim denials, increased administrative burdens, and financial losses for healthcare providers, highlighting the need to stay informed about guidelines and compliance requirements.
How can effective DME billing practices benefit healthcare providers?
Effective DME billing practices help maintain compliance with healthcare regulations, reducing the risk of audits and penalties. This can improve revenue cycle efficiency, enhance cash flow, and minimize claim denials.
What role does Healthcare Partners Consulting play in DME billing?
Healthcare Partners Consulting offers accounts receivable management solutions that improve revenue cycle efficiency, enhance cash flow, and reduce denials through meticulous documentation practices and follow-up on unpaid claims.
What is the projected growth of the U.S. DME market?
The U.S. DME market is projected to grow at a compound annual growth rate (CAGR) of 5.0% to 5.6% in the coming years, driven by an increasing senior population and the rising prevalence of chronic diseases.
What are HCPCS codes and their significance in DME billing?
The Healthcare Common Procedure Coding System (HCPCS) includes alphanumeric codes used to identify products, supplies, and services not covered by the Current Procedural Terminology (CPT). HCPCS Level II codes, particularly ‘E’ codes, are crucial for accurate DME invoicing.
How can healthcare providers ensure accurate HCPCS coding?
Healthcare providers can ensure accurate HCPCS coding by regularly training and updating their knowledge of these codes, which significantly reduces error rates that can negatively impact revenue cycles.
What services does Healthcare Partners Consulting provide related to HCPCS coding?
Healthcare Partners Consulting provides services including denial management and appeals to help recover underpaid or denied claims, ensuring that providers maximize their revenue potential through accurate HCPCS coding.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting