Optimizing Practice Operations
5 Best Practices for the Fee for Service Model in Mental Health Care

Introduction
Navigating the fee-for-service model presents significant challenges for mental health practitioners, particularly in balancing revenue generation with quality care. This model can lead to challenges in maintaining high-quality patient care.
How can mental health providers strike a balance between maximizing operational efficiency and ensuring that patient outcomes remain at the forefront of their practice?
This article explores five best practices that can help mental health facilities thrive within this model, ultimately enhancing both service delivery and patient satisfaction.
Understand the Fee-for-Service Model in Mental Health Care
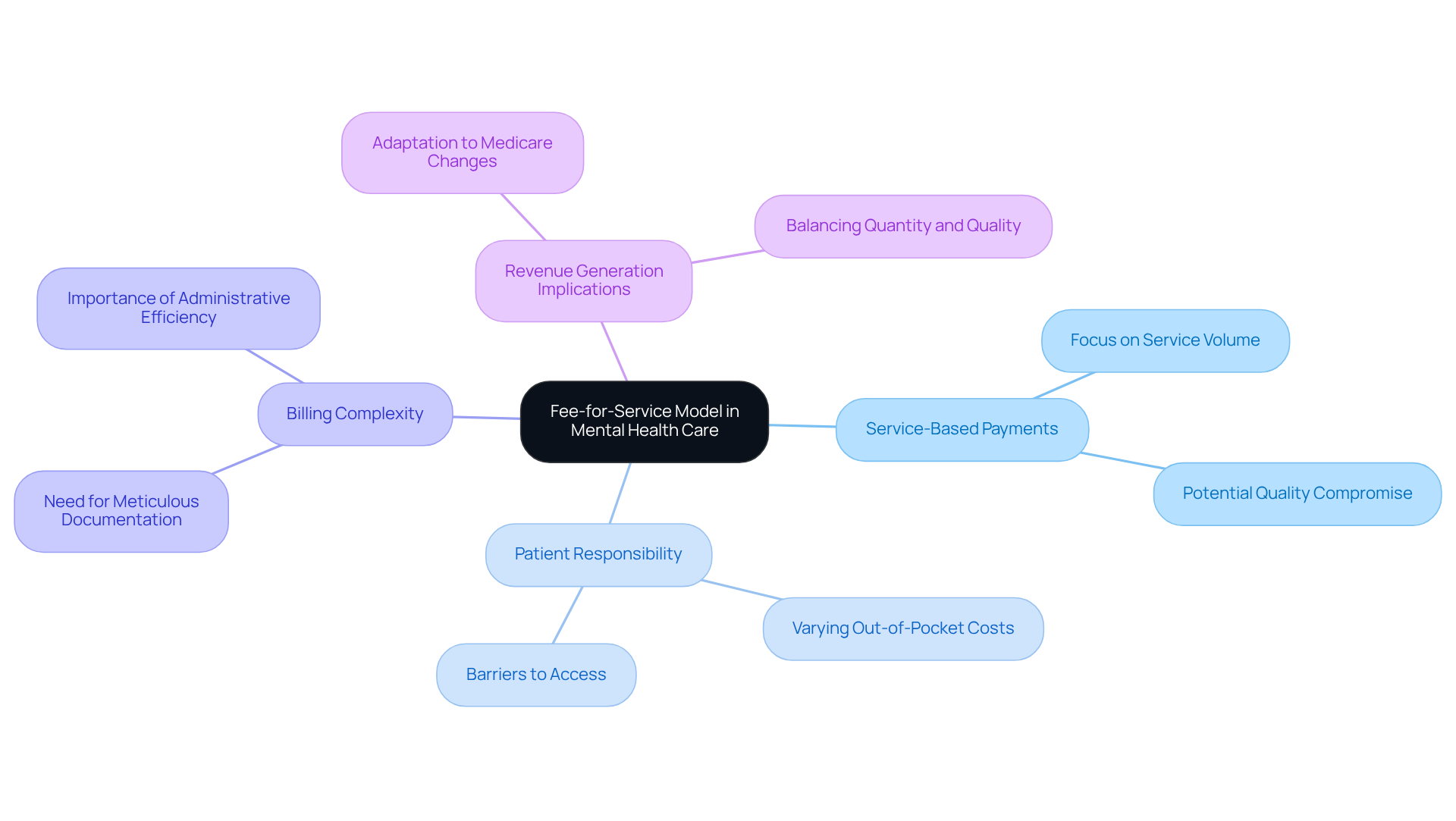
Understanding the fee for service model is essential for mental health practitioners navigating the complexities of healthcare reimbursement. The fee for service model is a common payment structure in healthcare. Providers receive reimbursement for each service they render to patients. In the context of mental wellness support, this translates to therapists and clinics charging for individual sessions, evaluations, and various services offered. A thorough understanding of the fee for service model is crucial for mental health practitioners, significantly influencing both revenue generation and operational efficiency.
Key characteristics of the FFS model include:
- Service-Based Payments: Providers are compensated for each service delivered. This can lead to a focus on service volume over quality of care.
- Patient Responsibility: Patients often face varying out-of-pocket costs based on their insurance coverage. This variability in costs can create barriers to accessing essential mental health services.
- Billing Complexity: The FFS model necessitates meticulous documentation and coding to secure proper reimbursement, highlighting the importance of administrative efficiency.
The effect of the fee for service model on revenue generation in mental wellness settings is substantial. As practices adapt to the evolving landscape of healthcare reimbursement, understanding the nuances of the fee for service model becomes essential. For example, mental wellness providers must be aware of the implications of the 2026 Medicare Physician Fee Schedule. These changes may necessitate adjustments in practice management to ensure financial viability.
Mental health professionals often share differing views on the FFS payment structure. Some emphasize that while the fee for service model allows for immediate revenue generation, it may inadvertently prioritize service quantity over patient outcomes. As one clinician remarked, ‘The fee for service model can sometimes lead to an emphasis on the number of sessions rather than the quality of service provided.’ This feeling emphasizes the necessity for mental wellness providers to balance service delivery with patient-focused support.
By mastering the fee for service model, mental wellness providers can effectively navigate its complexities and optimize billing methods, resulting in improved operational success and patient care outcomes.
Evaluate Current Operations and Identify Improvement Areas
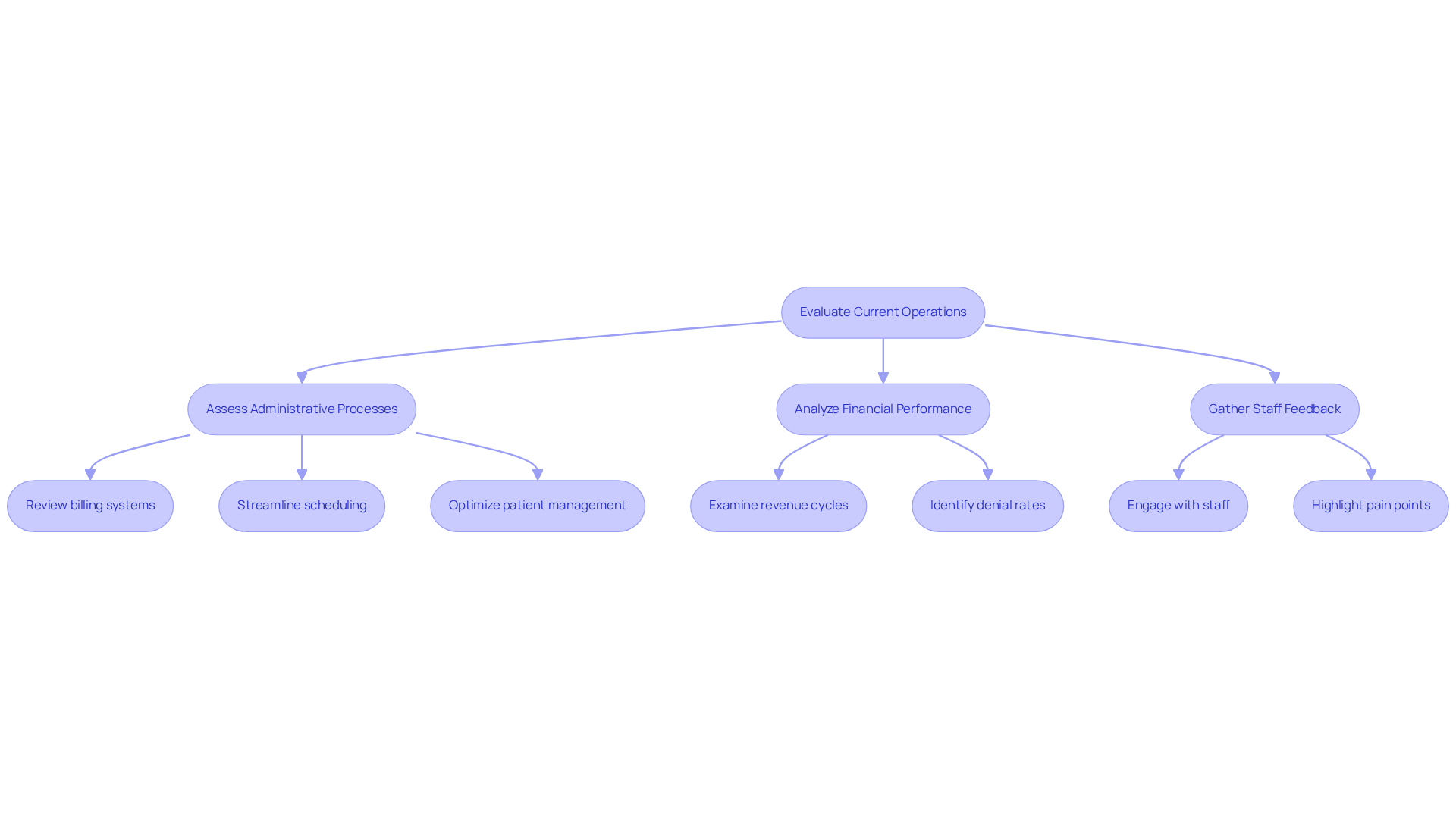
To thrive in a fee for service model, mental health facilities must rigorously assess their operational effectiveness. This process includes several key components:
- Assessing Administrative Processes: A detailed review of billing, scheduling, and patient management systems is essential to identify bottlenecks and inefficiencies. Practices should focus on streamlining these processes to enhance operational flow, leveraging tailored consulting and support from Healthcare Partners Consulting to optimize their administrative tasks.
- Analyzing Financial Performance: It is crucial to examine revenue cycles, including claim submission timelines and denial rates, which can range from 15 to 25 percent due to various operational challenges such as authorization errors and eligibility verification failures. Utilizing Healthcare Partners Consulting’s denial management services allows organizations to pinpoint these issues and develop strategies that enhance revenue and cash flow.
- Gathering Staff Feedback: Engaging with staff members provides valuable insights into their challenges and suggestions for improving workflows. This feedback can highlight specific pain points that may not be apparent through data analysis alone and can be enhanced through the structured support offered by Healthcare Partners Consulting.
By systematically evaluating these areas, facilities can identify significant opportunities for improvement, streamline operations, and enhance overall service delivery. In 2026, as behavioral wellness facilities encounter obstacles like staff shortages and the necessity for enhanced workflows, those that emphasize these assessments and contemplate the thorough medical billing and practice management solutions from Healthcare Partners Consulting will be better equipped to manage the intricacies of billing and reimbursement while ensuring high-quality service. Ultimately, those who prioritize these evaluations will not only enhance their operational efficiency but also secure their position in a competitive landscape.
Implement Strategic Changes for Successful Transition
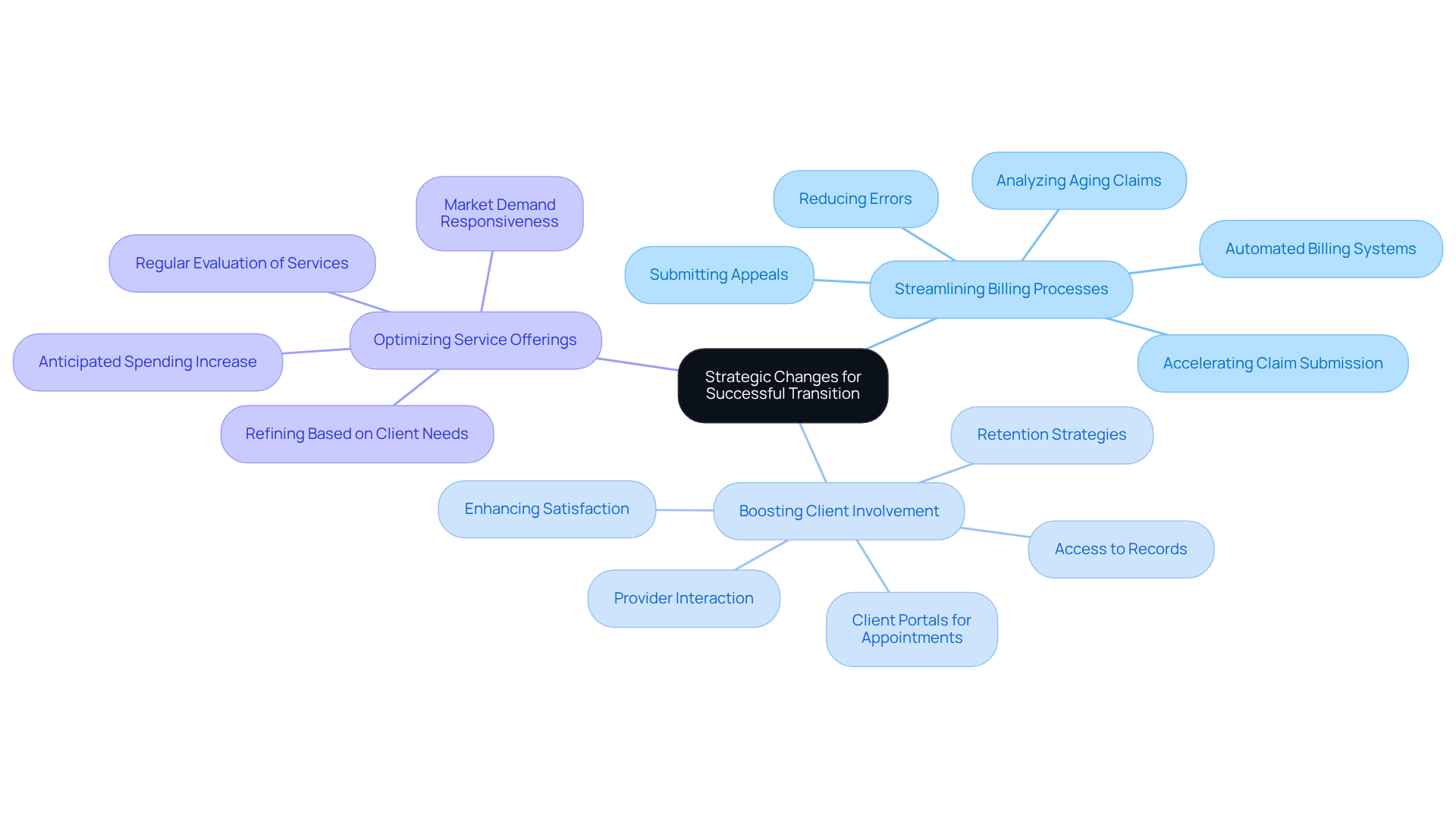
Transitioning to a more effective fee for service model necessitates strategic adjustments that enhance both operational efficiency and patient support. Key strategies include:
- Streamlining Billing Processes: Implementing automated billing systems, such as those offered by Healthcare Partners Consulting, can significantly reduce errors and accelerate claim submission. This efficiency mitigates operational inefficiencies in billing that can jeopardize the financial health of mental wellness organizations. HPC’s comprehensive medical billing solutions streamline follow-up tasks, such as analyzing aging claims and submitting appeals. As Ben Ray observes, “Value-based care models stress treatment involvement and social factors influencing well-being,” emphasizing the significance of efficient billing processes in supporting these models.
- Boosting Client Involvement: Using client portals enables users to arrange appointments, view their records, and interact with providers, which can enhance satisfaction and retention. Given that nearly one in four adult Americans experiences a mental wellness issue annually, enhancing client involvement is critical for sustaining robust operations. Moreover, behavioral wellness appointments among commercially insured individuals have exceeded primary care visits, indicating a rising demand for mental wellness services and the necessity for effective engagement strategies.
- Optimizing Service Offerings: Regularly evaluating and refining service offerings based on client needs and market demand ensures that practices remain competitive and responsive. This flexibility is crucial as expenditure on behavioral wellness is anticipated to rise by 10-20% in 2026 due to growing usage and specialty pharmacy trends.
By prioritizing these strategic changes, organizations can enhance operational efficiency and significantly improve the overall experience for individuals, which is a critical factor in a fee for service model. Additionally, organizations must remain vigilant regarding ongoing scrutiny related to MHPAEA compliance and provider directory accuracy, as these factors can significantly impact billing processes and operational risk management.
Train Staff and Ensure Regulatory Compliance
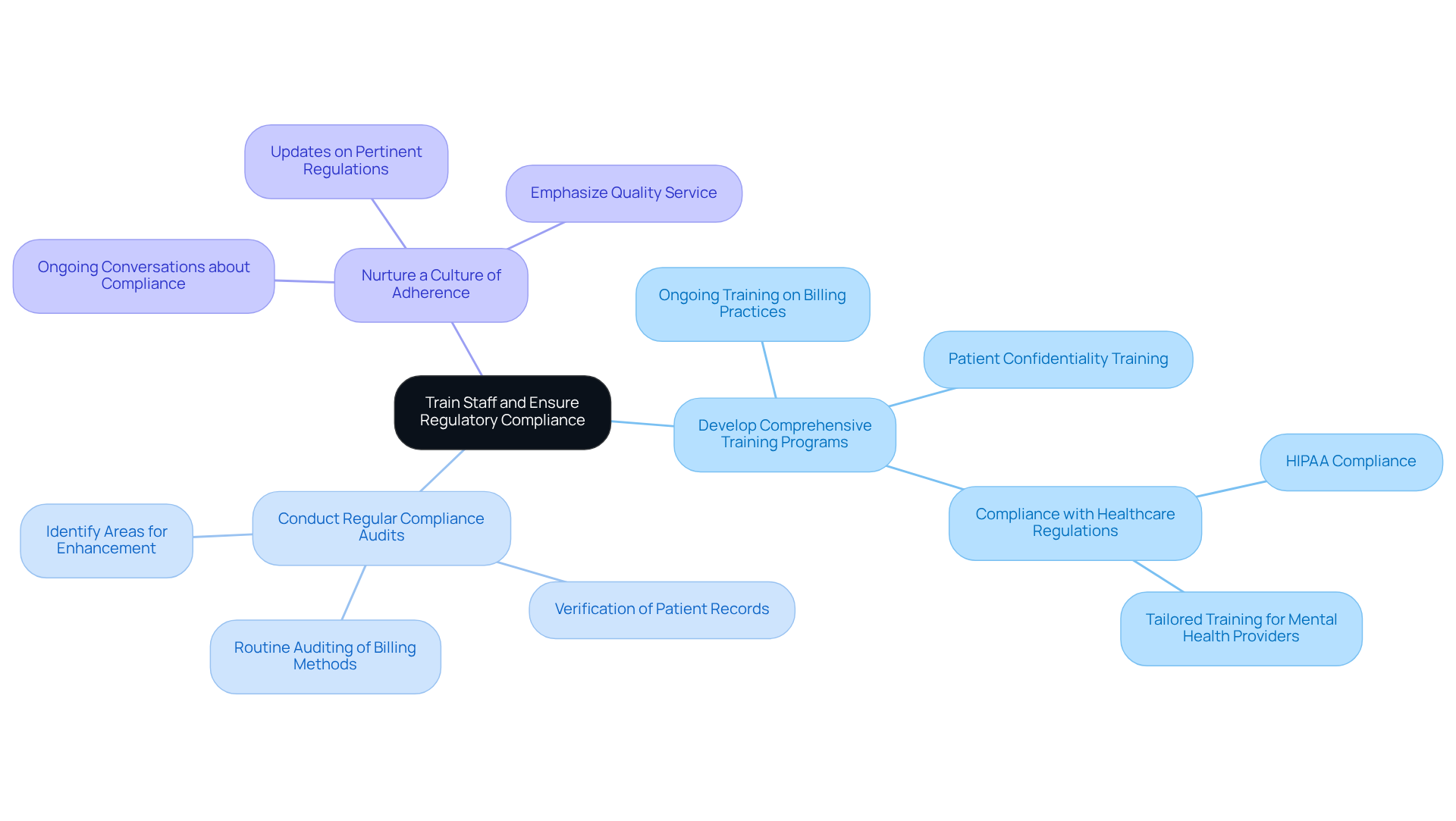
A well-trained team is essential for the success of mental wellness services that operate under a fee for service model, where compliance and quality care are paramount. To achieve this, practices should implement the following strategies:
- Develop Comprehensive Training Programs: Implement ongoing training that encompasses billing practices, patient confidentiality, and compliance with healthcare regulations, including HIPAA. Tailor training to the specific needs of mental health providers, ensuring staff are well-versed in current regulatory requirements.
- Conduct Regular Compliance Audits: Establish a routine for auditing billing methods and patient records to verify adherence to regulations and identify areas for enhancement. Regular audits not only assist in ensuring compliance but also improve the overall operational efficiency of the organization.
- Nurture a Culture of Adherence: Motivate personnel to emphasize compliance and quality service through ongoing conversations and updates on pertinent regulations and optimal methods. Establishing a setting where compliance is appreciated can significantly lower the risk of billing mistakes and improve trust among individuals.
Investing in employee development and compliance initiatives not only reduces risks but also enhances the quality of care offered to individuals. Ultimately, prioritizing employee development and compliance not only mitigates risks but also fosters a sustainable model for delivering high-quality mental health care.
Monitor Outcomes and Adjust Strategies for Continuous Improvement
In a competitive healthcare landscape, mental health services must prioritize continuous improvement to thrive under the fee for service model. To achieve this, practices should:
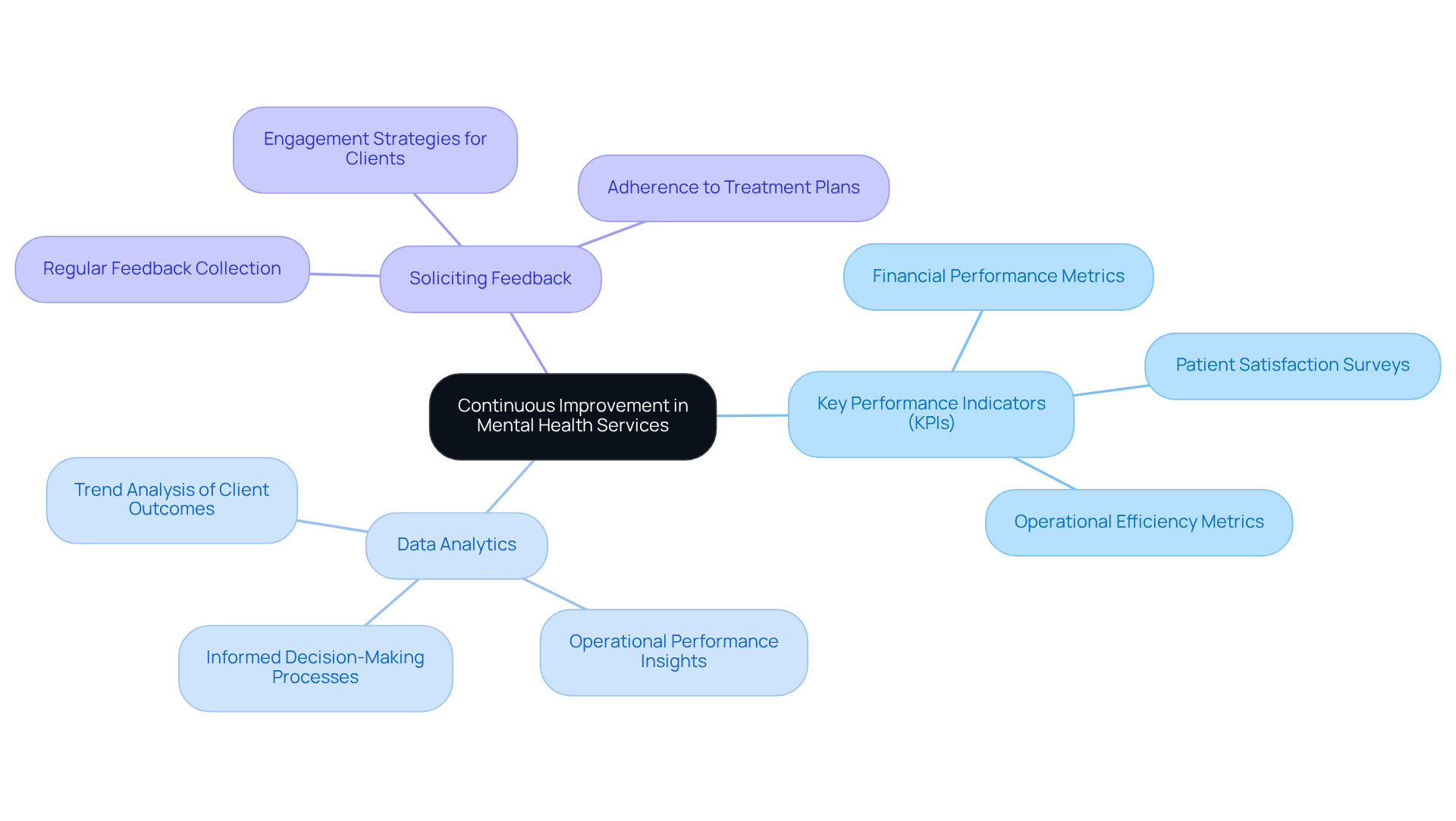
- Establish Key Performance Indicators (KPIs): Identifying and tracking KPIs related to financial performance, patient satisfaction, and operational efficiency is crucial for measuring success. Monitoring these indicators assists organizations in comprehending their performance and identifying areas requiring attention.
- Utilize Data Analytics: Leveraging data analytics tools allows organizations to analyze trends in client outcomes and operational performance. This informed decision-making process is essential for improving service quality and ensuring that methods adjust to changing individual requirements.
- Solicit Feedback from Individuals: Regularly gathering feedback from individuals about their experiences and outcomes is key to identifying areas for improvement. Engaged clients are more likely to adhere to treatment plans, which boosts overall satisfaction and treatment effectiveness.
By actively monitoring these outcomes and adjusting strategies, practices can respond effectively to patient needs and operational challenges. This responsiveness ultimately enhances both care quality and financial performance.
Conclusion
Effectively implementing the fee-for-service model is crucial for mental health practitioners seeking to optimize operational efficiency and enhance patient care. While this model generates immediate revenue, it also poses challenges that must be navigated to ensure quality service delivery.
Key practices discussed include:
- Evaluating current operations
- Implementing strategic changes
- Ensuring staff training and regulatory compliance
By assessing administrative processes, analyzing financial performance, and gathering staff feedback, mental health facilities can identify areas for improvement. Furthermore, streamlining billing processes and boosting client involvement are essential strategies for adapting to the evolving healthcare landscape.
By focusing on continuous improvement and adaptability, mental health services can significantly impact the healthcare landscape and patient outcomes.
Frequently Asked Questions
What is the fee-for-service model in mental health care?
The fee-for-service model is a payment structure where providers receive reimbursement for each service they deliver to patients, including individual sessions and evaluations.
What are the key characteristics of the fee-for-service model?
Key characteristics include service-based payments, patient responsibility for varying out-of-pocket costs, and the necessity for meticulous billing and documentation.
How does the fee-for-service model impact revenue generation in mental wellness settings?
The fee-for-service model significantly influences revenue generation, as practices must adapt to changes in healthcare reimbursement, such as those outlined in the 2026 Medicare Physician Fee Schedule.
What concerns do mental health professionals have regarding the fee-for-service model?
Some professionals express concern that the model may prioritize service quantity over quality, potentially leading to a focus on the number of sessions rather than patient outcomes.
What steps should mental health facilities take to evaluate their operations in a fee-for-service model?
Facilities should assess administrative processes, analyze financial performance, and gather staff feedback to identify inefficiencies and improve workflows.
Why is it important to analyze financial performance in mental health facilities?
Analyzing financial performance helps identify issues such as claim denial rates and revenue cycle challenges, which can impact cash flow and overall financial health.
How can staff feedback contribute to operational improvement in mental health facilities?
Staff feedback provides insights into challenges and suggestions for workflow improvements that may not be evident through data analysis alone.
What role does Healthcare Partners Consulting play in optimizing operations for mental health facilities?
Healthcare Partners Consulting offers tailored support to streamline administrative tasks, enhance denial management, and improve overall operational effectiveness in billing and practice management.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting