Mastering Medical Coding
What Do CPT Category II and III Codes Consist Of for Mental Health?

Introduction
Navigating the complexities of modern healthcare requires a deep understanding of CPT Category II and III codes for mental health practitioners. These codes serve as critical tools for performance measurement and facilitate the accurate documentation of emerging therapies and technologies. Yet, as psychological care evolves, providers face the challenge of leveraging these codes to improve care quality and maintain financial viability. By exploring the definitions, purposes, and implications of these coding systems, practitioners can uncover pathways to improved patient outcomes and operational success.
Define CPT Category II and Category III Codes
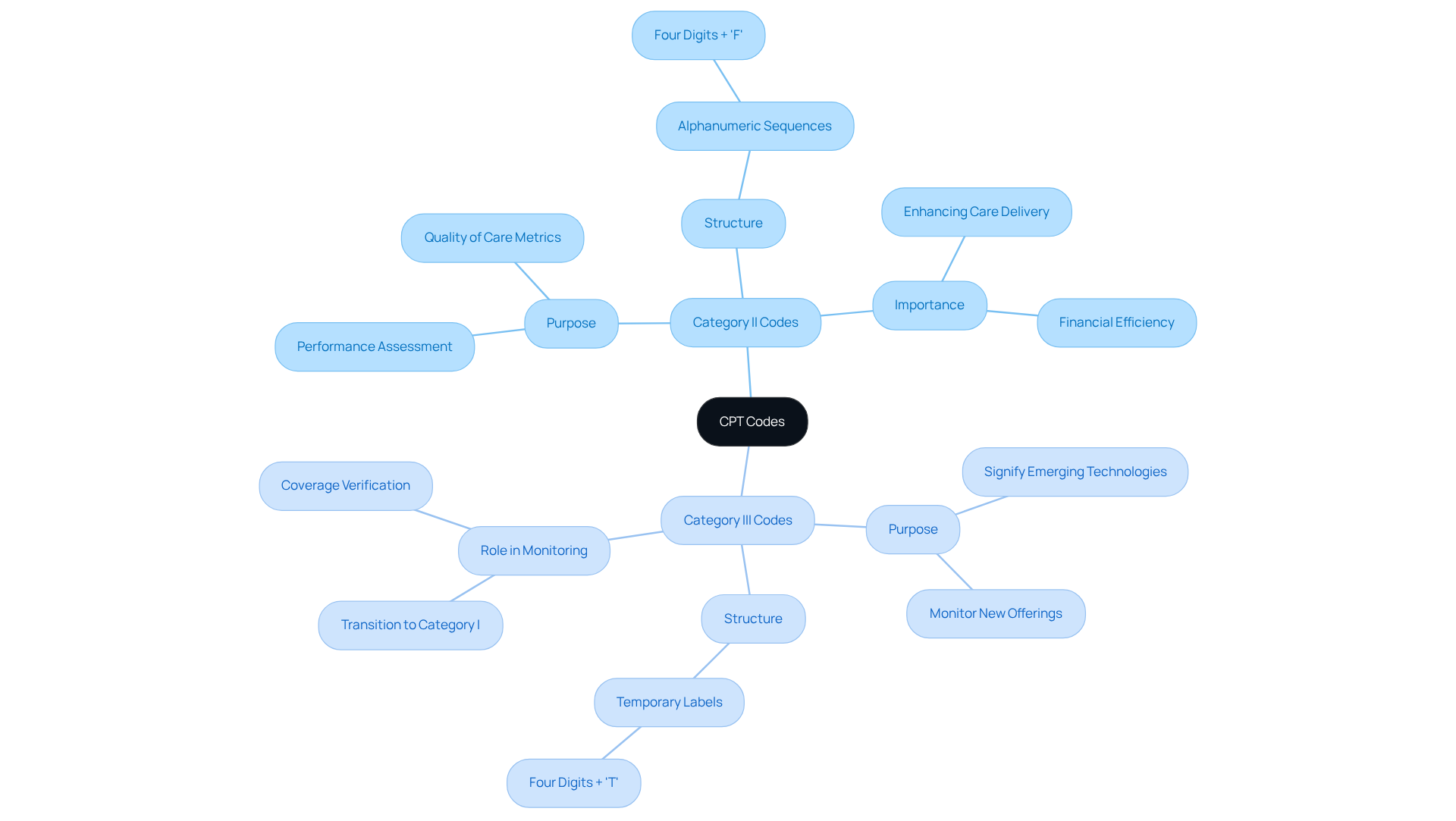
CPT Category II designations serve as vital tools for performance assessment in healthcare, raising the question of what do CPT Category II and Category III codes consist of? These alphanumeric sequences, comprising four digits and the letter ‘F’ (e.g., 3040F), are optional and not required for accurate encoding. However, they play a crucial role in reporting quality of care metrics, enabling practices to evaluate and enhance their delivery of care.
In contrast, when we ask what do CPT Category II and Category III codes consist of, we find that CPT Category III classifications are temporary labels that signify emerging technologies, offerings, and procedures. These identifiers, consisting of four numerical digits followed by the letter ‘T’ (e.g., 1234T), assist in monitoring new offerings that may ultimately evolve into permanent Category I identifiers.
The unveiling of these regulations showcases progress in medical practices and technology, ensuring that psychological care providers can accurately record and charge for innovative offerings. Without accurate documentation, practices risk significant financial losses. This oversight can lead to delayed reimbursements and hindered operational efficiency.
Precise coding is essential for prompt reimbursement and compliance, and Healthcare Partners Consulting focuses on helping psychological practices manage these complexities effectively. Their expertise in medical billing helps practices avoid claim denials and maximize revenue, ultimately supporting better patient outcomes and operational efficiency.
In mental health settings, understanding what do CPT Category II and Category III codes consist of is essential for improving care quality and ensuring precise billing practices.
Context and Importance of CPT Category II and Category III Codes
Understanding what do CPT Category II and Category III codes consist of is crucial, as these designations play a pivotal role in performance measurement initiatives, directly impacting the quality of patient care. These systems enable healthcare providers to report on quality metrics and enhance patient care by monitoring compliance with clinical guidelines, ultimately improving the overall quality of services provided.
Conversely, it is important to understand what do CPT Category II and Category III codes consist of, as they are essential for monitoring new and innovative procedures that are still undergoing evaluation. Adapting to new therapies and technologies poses challenges for psychological care providers, where new therapies and technologies can greatly affect treatment results.
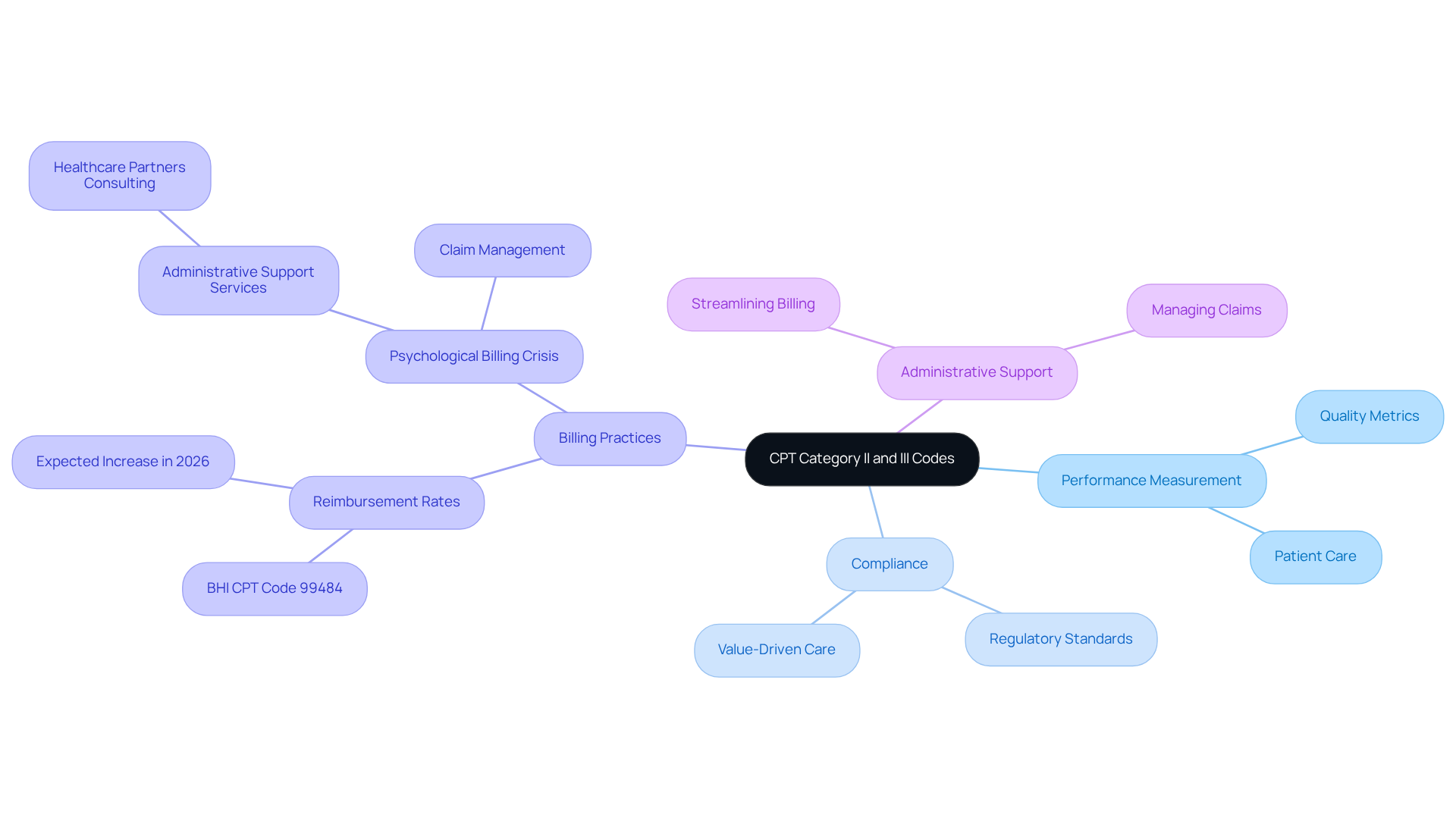
By applying these systems effectively, wellness practitioners ensure compliance with regulatory standards and engage in value-driven care models that prioritize quality. The BHI CPT identifier 99484, covering 20 minutes of non-face-to-face BHI time, is significant with a national average reimbursement of about $57. As reimbursement rates for BHI offerings are expected to rise in 2026, psychological care providers are urged to adopt these codes to enhance delivery and improve patient outcomes.
Moreover, tackling the ongoing psychological billing crisis necessitates extensive administrative support services, like those provided by Healthcare Partners Consulting. This includes streamlining billing and managing claims, which are vital for navigating the complexities of psychological billing. Tracking claims and denials after the update is essential for practices adjusting to these new standards, ensuring that they can resolve any problems quickly and sustain financial viability.
Furthermore, Healthcare Partners Consulting provides a performance-aligned medical billing pricing model, beginning at a minimum of $500 for practices with a gross income of $6,500 or below, which can further assist providers in managing their billing processes efficiently. Ultimately, embracing these billing practices is not just about compliance; it’s about fostering a sustainable future for psychological care.
Origins and Evolution of CPT Codes
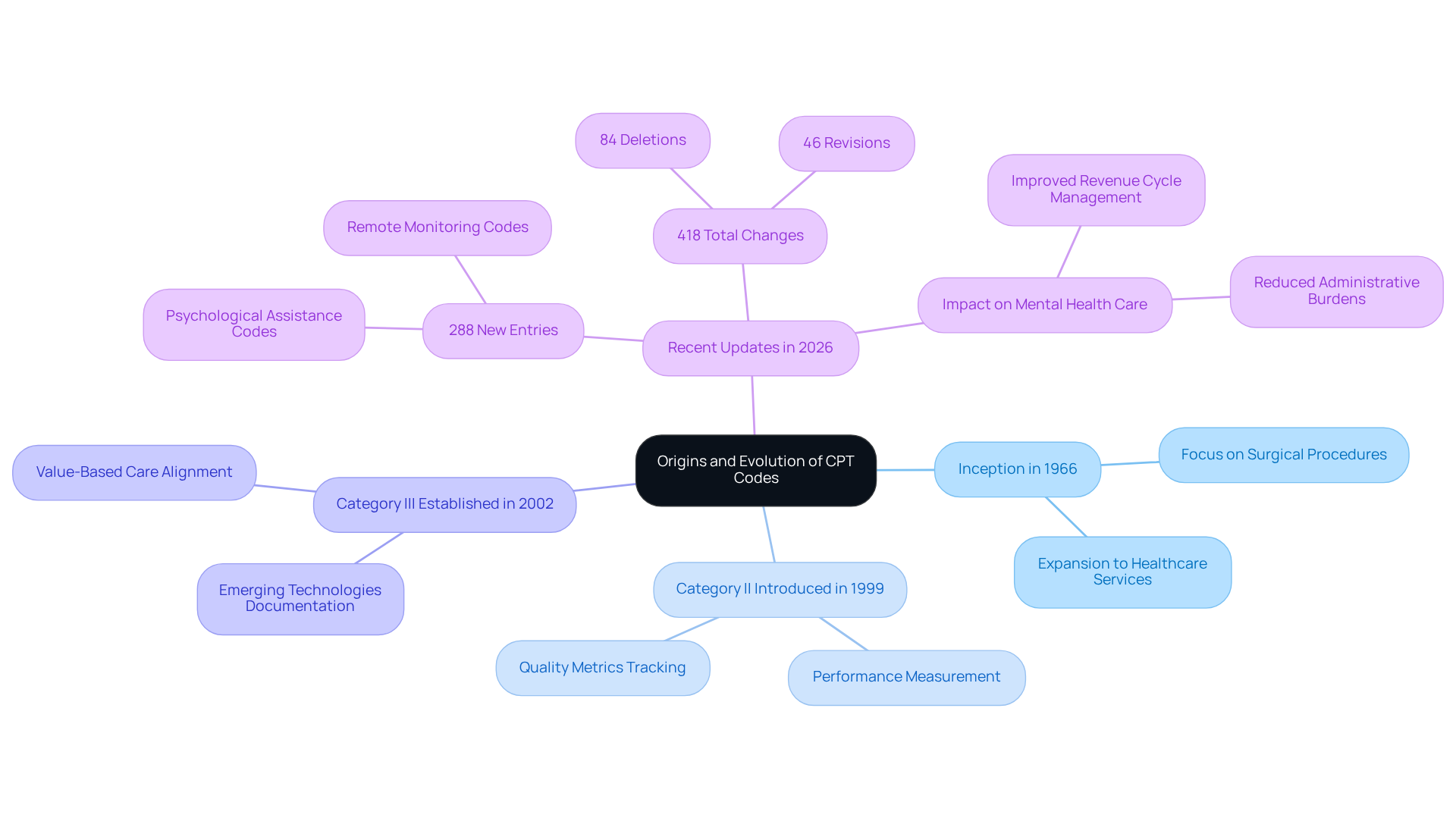
Since their inception in 1966, the Current Procedural Terminology (CPT) classifications have evolved significantly, reflecting the complexities of modern healthcare delivery. Originally focused on surgical procedures, the CPT classification has expanded to encompass a wide range of healthcare services, particularly in mental health.
In 1999, Category II classifications were introduced to enhance performance measurement, enabling providers to track quality metrics and improve patient care. Subsequently, Category III classifications were established in 2002 to document emerging technologies and procedures, aligning with the healthcare sector’s shift towards value-based care. This evolution underscores the importance of quality enhancement initiatives, making these standards crucial for providers navigating the complexities of billing and compliance.
Recent updates, including the 2026 CPT classification set, further illustrate this trend, with 288 new entries introduced to capture advancements in psychological assistance and technology. Incorporating these systems into billing practices allows psychological care providers to improve revenue cycle management and cash flow while reducing administrative burdens.
Comprehensive administrative support from Healthcare Partners Consulting, including services like Patient Medical Billing Support and Monthly AR Reports, enables practices to concentrate on delivering quality care while HPC manages the intricacies of billing and compliance.
Case studies highlight how the integration of billing practices can demonstrate what do CPT Category II and Category III codes consist of, facilitating more precise reporting and reimbursement for innovative mental health treatments. Ultimately, these advancements in CPT classifications are pivotal in shaping the future of mental health care accessibility and quality.
Key Characteristics of CPT Category II and Category III Codes
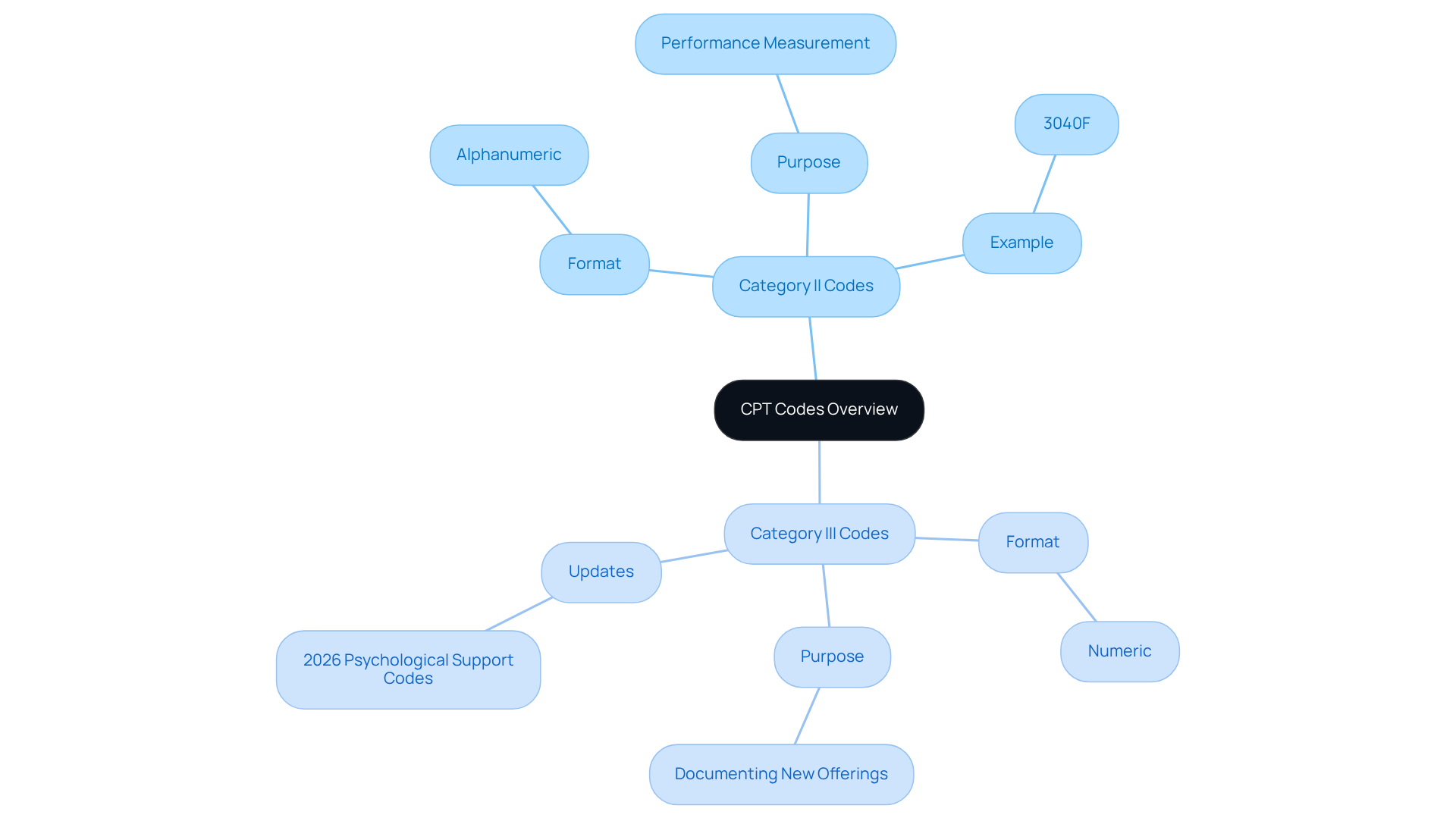
Accurate coding is essential, yet many providers face challenges that can hinder their financial success. CPT Category II identifiers illustrate what CPT Category II and Category III codes consist of, being recognized by an alphanumeric format, comprising four digits followed by the letter ‘F.’ These identifiers do not serve billing purposes. Instead, they function as performance measurement tools that monitor the quality of care delivered. For example, a sequence such as 3040F may indicate a particular preventive measure provided to patients.
In contrast, to understand what CPT Category II and Category III codes consist of, it is important to note that Category III classifications are temporary and denoted by four numeric digits followed by the letter ‘T.’ These protocols are essential for documenting new and emerging offerings, including telehealth interventions and innovative treatment approaches. As of the 2026 update, several new Category III codes have been introduced specifically for psychological support, reflecting advancements in care delivery.
Both categories are vital for precise reporting and adherence. They enable care providers to demonstrate the quality of their services and facilitate reimbursement processes. We at Healthcare Partners Consulting know that accurate coding is crucial for timely and correct reimbursement. Our expert team provides tailored coding support, ensuring that every claim submitted reflects the services provided, medical necessity, and relevant modifiers. This approach ultimately enhances revenue cycle management for mental health clinics, leading to fewer denials and faster payments. Ultimately, the precision of coding not only reflects the quality of care but also safeguards the financial viability of mental health services.
Conclusion
The effective use of CPT Category II and III codes is crucial for advancing mental health care quality. These coding systems facilitate performance measurement and enable accurate documentation of emerging technologies and treatments. The careful application of these codes supports compliance and operational efficiency, ultimately benefiting both providers and patients.
The article highlights the critical roles that CPT Category II and III codes play in mental health settings. Category II codes serve as performance measures, while Category III codes document innovative procedures that may transition into permanent identifiers. This dual functionality underscores the importance of precise coding for timely reimbursements and effective care delivery. Furthermore, the evolution of these codes reflects the healthcare sector’s commitment to addressing new challenges.
In light of the complexities surrounding mental health billing, navigating these challenges can be difficult for providers. By embracing these coding practices actively, mental health practices can improve their financial viability and enhance patient outcomes. This proactive approach can significantly enhance both financial stability and patient care outcomes. Expert support from Healthcare Partners Consulting can streamline billing and ensure compliance with evolving standards. Without the integration of these coding systems, the potential for enhanced patient care and accessibility may remain unfulfilled.
Frequently Asked Questions
What are CPT Category II codes?
CPT Category II codes are optional alphanumeric sequences consisting of four digits followed by the letter ‘F’ (e.g., 3040F) that serve as tools for performance assessment in healthcare. They are used for reporting quality of care metrics, enabling practices to evaluate and enhance their delivery of care.
What are CPT Category III codes?
CPT Category III codes are temporary identifiers consisting of four numerical digits followed by the letter ‘T’ (e.g., 1234T) that signify emerging technologies, offerings, and procedures. They assist in monitoring new offerings that may eventually evolve into permanent Category I identifiers.
Why are CPT Category II and Category III codes important for healthcare practices?
These codes are important because they help ensure accurate documentation and billing. Proper coding is essential for prompt reimbursement, compliance, and avoiding financial losses due to claim denials, which ultimately supports better patient outcomes and operational efficiency.
How can healthcare practices benefit from understanding CPT Category II and Category III codes?
Understanding these codes is crucial for improving care quality and ensuring precise billing practices, which can lead to enhanced delivery of care and better financial performance for healthcare practices.
What role does Healthcare Partners Consulting play in relation to CPT codes?
Healthcare Partners Consulting specializes in helping psychological practices manage the complexities of medical billing related to CPT codes, aiming to avoid claim denials and maximize revenue, thus supporting improved patient outcomes and operational efficiency.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting