Telehealth Billing Insights
What’s an EOB? Understanding Its Role in Healthcare Billing

Introduction
Navigating the complexities of healthcare billing requires a thorough understanding of documents such as the Explanation of Benefits (EOB). This essential tool clarifies the services received, the costs incurred, and the role of insurance coverage in managing healthcare expenses. Despite its importance, many individuals lack clarity regarding the details and significance of their EOBs, which can lead to confusion and unexpected costs.
Patients frequently encounter discrepancies in their EOBs, which can lead to confusion and unexpected costs. By mastering the details of their EOBs, patients can mitigate financial risks and enhance their healthcare decision-making.
Define Explanation of Benefits (EOB)
A Summary of Benefits (EOB) is a crucial document provided by health coverage firms that details the medical treatments received by an individual, so you might be wondering, what’s an EOB? It outlines how a claim was processed, specifying the expenses associated with the services rendered, the amount covered by the insurance provider, and the individual’s financial responsibility.
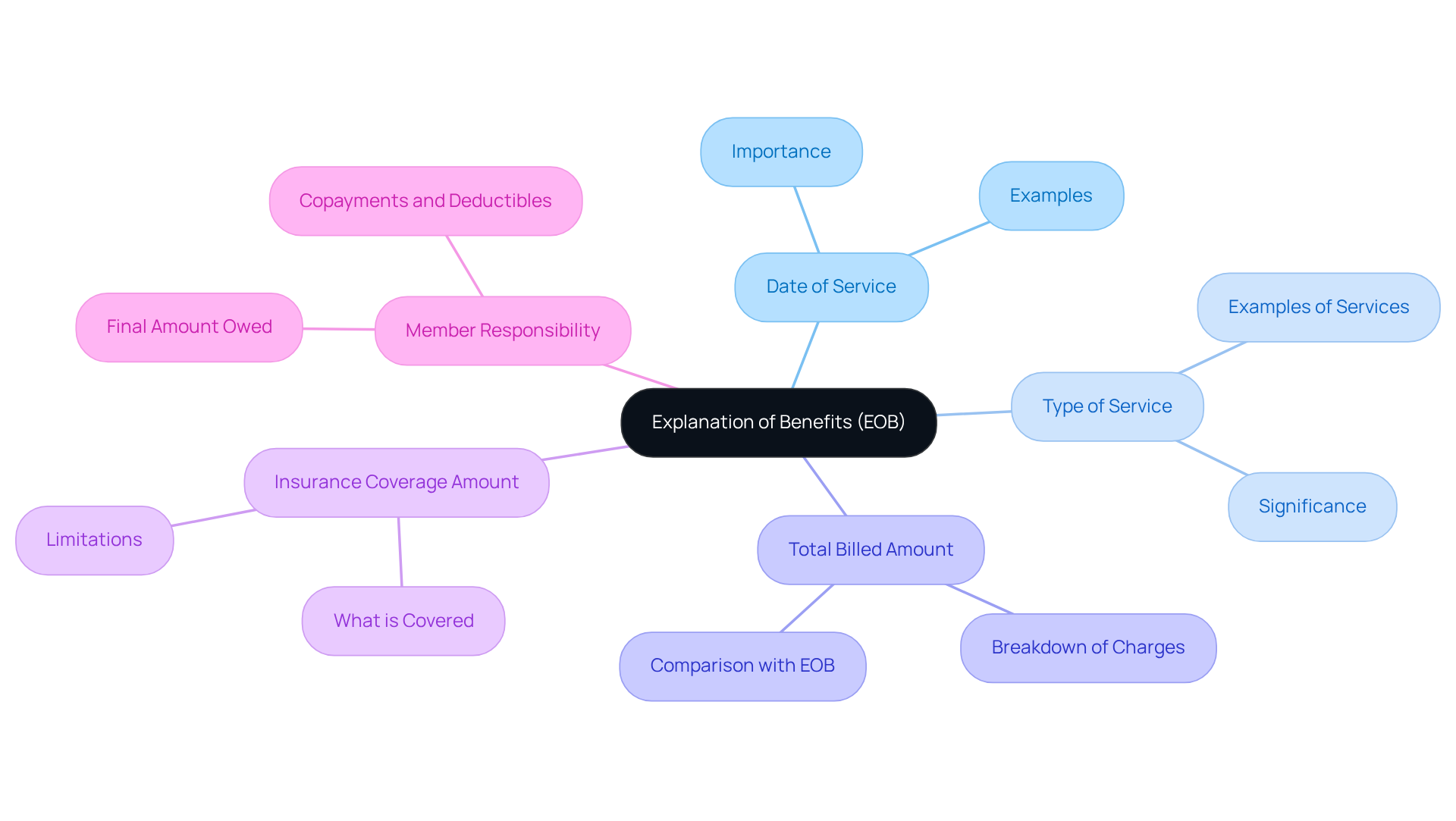
When asking ‘what’s an EOB’, it’s important to note that an EOB is not an invoice or payment request; it helps individuals understand their healthcare costs and coverage. Typically, an EOB contains essential information such as:
- The date of service
- The type of service provided
- The total billed amount
- The insurance coverage amount
- Any responsibility of the individual, including copayments or deductibles
The EOB also includes a Member Responsibility section, showing what you owe after deductibles, copays, or coinsurance are taken into account. It is crucial for individuals to compare the EOB with the provider’s bill to ensure accuracy before making any payments, as discrepancies can arise, such as unexpected claim denials or differences between the EOB and the provider’s bill.
Inaccurate coding can complicate the claims process, resulting in delays and increased workload for medical practices. Healthcare Partners Consulting addresses these challenges by reviewing and correcting coding issues before claims are submitted, thereby enhancing compliance and streamlining operations. Understanding what’s an EOB is crucial for patients to evaluate their financial obligations and manage healthcare costs efficiently.
Understand the Importance of EOBs in Healthcare
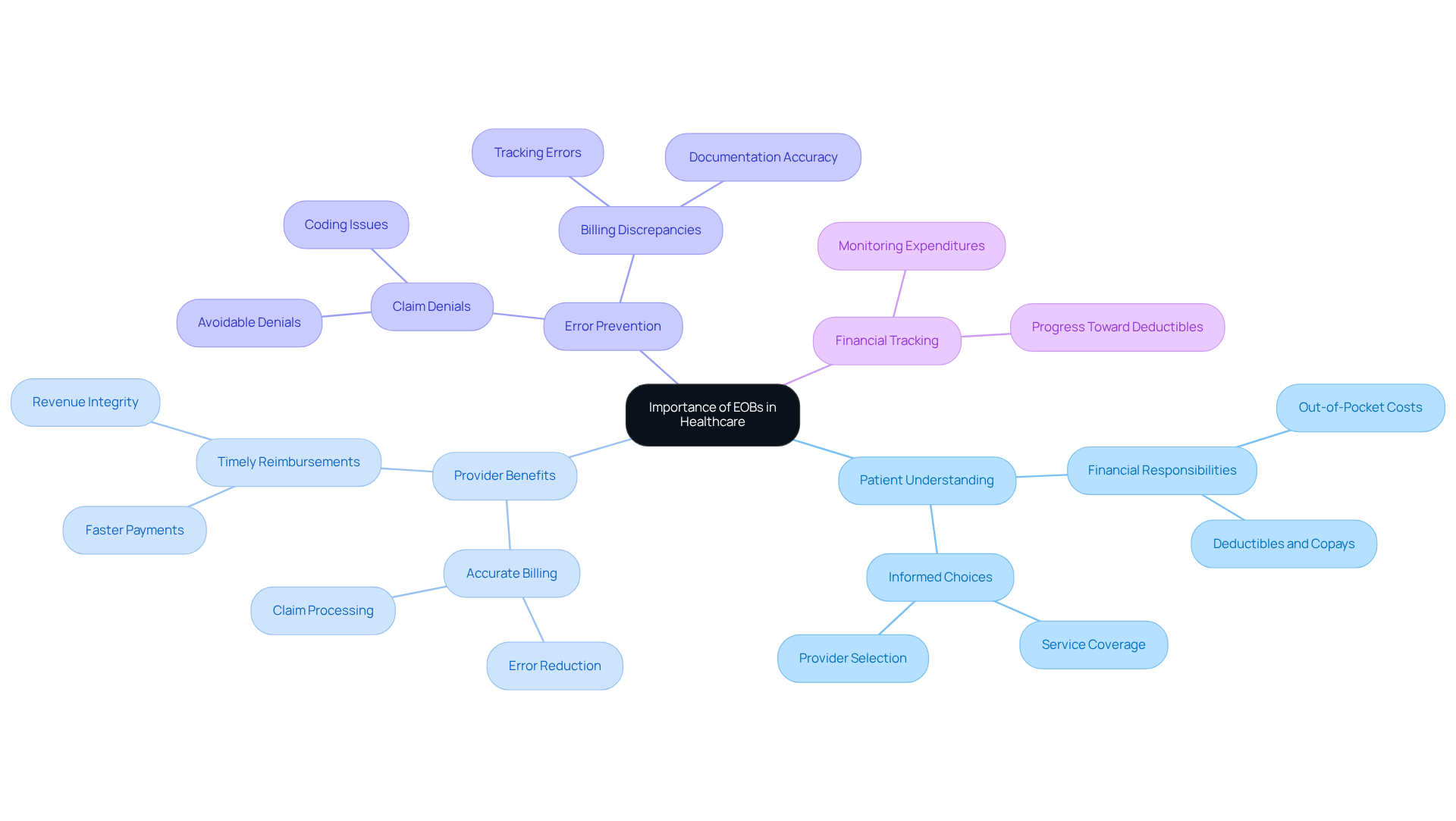
In the complex landscape of medical billing, understanding what’s an EOB is a critical tool for clarity and understanding. They provide essential insights into how insurance benefits are applied, significantly reducing confusion and potential disputes over billing. EOBs empower patients to understand their financial responsibilities and answer the question, ‘what’s an EOB,’ by outlining covered services and the patient’s financial responsibility, facilitating informed choices regarding their healthcare options. Furthermore, they serve as a valuable resource for tracking medical expenditures and monitoring progress toward meeting deductibles or out-of-pocket maximums.
For medical service providers, EOBs are indispensable for maintaining accurate billing and ensuring timely reimbursements. They offer a comprehensive overview of how claims are processed, highlighting necessary adjustments and minimizing the likelihood of errors. Errors in medical billing can lead to significant financial discrepancies for both patients and providers, highlighting why understanding what’s an EOB is essential for maintaining revenue integrity and operational efficiency. Additionally, about 30% of claims are denied on first submission, emphasizing how knowing what’s an EOB is vital in preventing billing errors and fostering smoother interactions between patients and providers.
Healthcare Partners Consulting enhances this process through comprehensive accounts receivable management solutions, including proactive follow-up with payers on unpaid or underpaid claims and appeal submissions for denied claims. By utilizing EOBs effectively, or what’s an EOB, alongside these offerings, both individuals and providers can navigate the complexities of medical billing with greater confidence and understanding, ultimately leading to improved cash flow and reduced denials. Ultimately, knowing what’s an EOB and leveraging them effectively can transform the billing experience, fostering transparency and trust between patients and providers.
Identify Key Components of an EOB
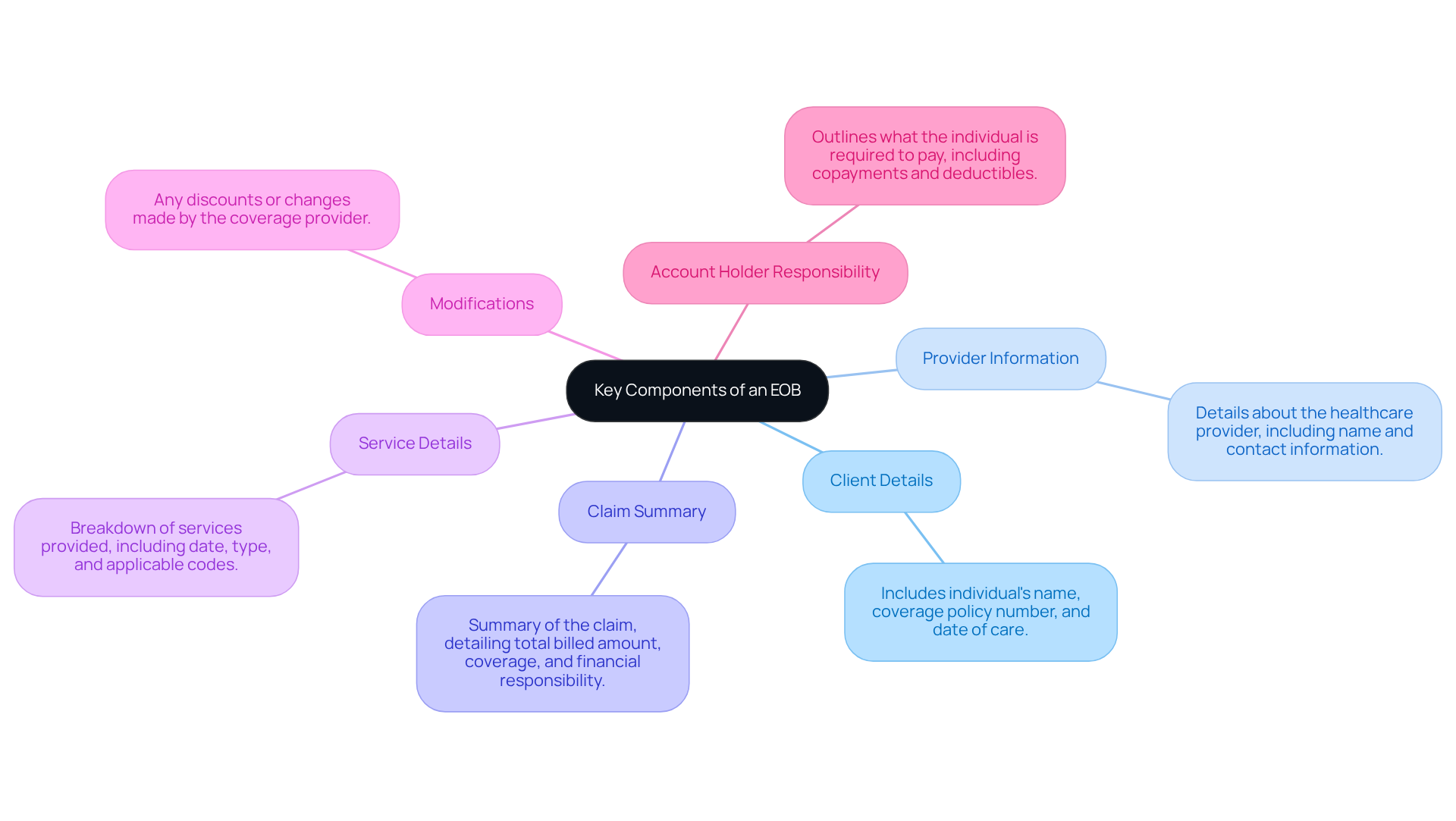
For patients, understanding what’s an EOB can often be challenging, leading to confusion about their healthcare expenses. An EOB typically includes several essential components that are crucial for understanding the billing process:
- Client Details: This section includes the individual’s name, coverage policy number, and the date of care.
- Provider Information: Details about the healthcare provider who delivered the care, including their name and contact information.
- Claim Summary: A summary of the claim, detailing the total billed amount, the amount covered by the policy, and the individual’s financial responsibility.
- Service Details: A breakdown of the services provided, including the date of service, type of service, and any applicable codes.
- Modifications: Any discounts or changes made by the coverage provider that can influence the total sum due by the individual.
- Account Holder Responsibility: This section outlines what the individual is required to pay, including copayments, deductibles, and any remaining balance after coverage.
Keep in mind that EOBs aren’t payment requests and don’t show a final balance due. Grasping these components is crucial for patients to interpret their healthcare costs effectively and understand what’s an EOB. For example, the ‘patient responsibility‘ amount indicates the part of a claim not covered by a plan, which may include deductibles and coinsurance. Patients should keep EOBs for their records and follow up on any discrepancies with their provider or insurance company. By understanding what’s an EOB and mastering the details of their EOBs, patients can avoid unexpected financial burdens and make informed decisions about their healthcare.
Navigate Common EOB Scenarios and Questions
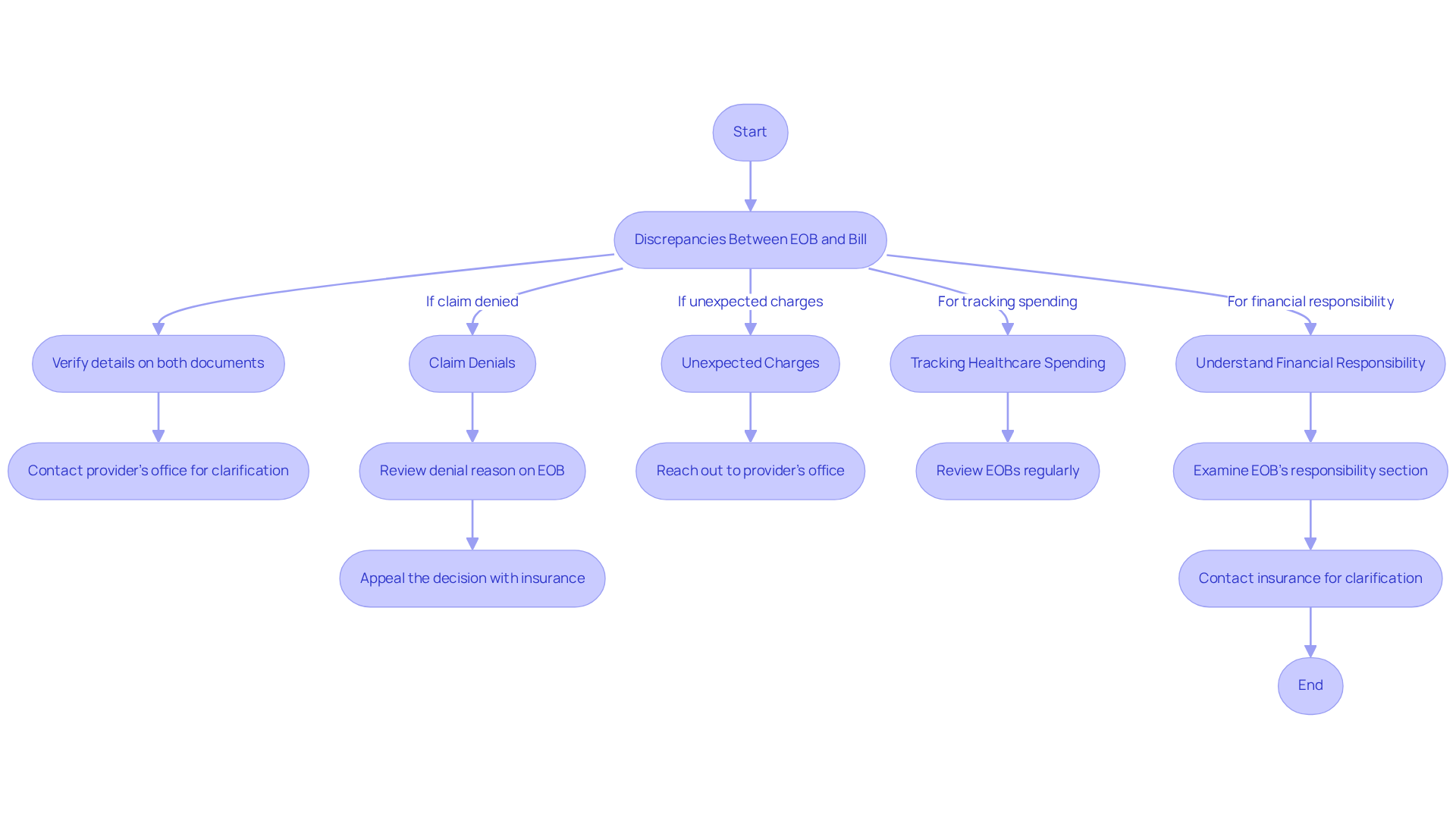
Understanding what’s an EOB can help navigate the complexities that often lead to confusion for patients. Here are some common situations and how to navigate them:
- Discrepancies Between EOB and Bill: If the amount owed on the EOB differs from the bill received from the provider, patients should first verify the details on both documents. Contacting the provider’s office for clarification can help resolve misunderstandings. Many patients unknowingly overpay due to billing errors, which can be as high as 80%. This step is crucial to avoid overpayment.
- Claim Denials: If a claim is denied, the EOB will indicate the reason for the denial. Patients should review this information carefully, as approximately 86% of denials are potentially avoidable. They may need to appeal the decision with their insurance company, which can be a complex process but is essential for recovering lost payments. Understanding modifier requirements and ensuring accurate coding, as emphasized by Healthcare Partners Consulting, can clarify what’s an EOB and significantly reduce the likelihood of denials.
- Unexpected Charges: Patients may find charges on their EOB that they did not anticipate. In such cases, it is advisable to reach out to the provider’s office to understand the nature of these charges and whether they were properly communicated prior to service. Taking this proactive step can clear up misunderstandings and help avoid unexpected costs.
- Tracking Healthcare Spending: EOBs can help individuals monitor their healthcare expenses over time. By reviewing EOBs regularly, individuals can track their progress toward meeting deductibles and out-of-pocket maximums, which is crucial for financial planning. This practice can also highlight any discrepancies that may arise in billing. Accurate coding, supported by Healthcare Partners Consulting, drives better billing outcomes and can lead to faster payment turnaround.
- Understanding Financial Responsibility: When unsure about their financial obligations, individuals should closely examine the EOB’s responsibility section. Contacting their insurance company for further clarification can provide additional insights. Being proactive and informed enables patients to effectively manage their healthcare costs and avoid unexpected financial burdens. Additionally, utilizing comprehensive denial management services from Healthcare Partners Consulting can help clinics handle coding, timely filing, prior authorization, and medical necessity denials, further enhancing their billing accuracy.
Conclusion
Understanding the intricacies of an Explanation of Benefits (EOB) is crucial for effective healthcare billing management for both patients and providers. This document serves as a vital communication tool, elucidating the services rendered, the insurance coverage applied, and the financial responsibilities of the patient. By understanding the intricacies of an EOB, individuals can manage their healthcare costs with enhanced clarity and confidence.
Throughout the article, key insights have been provided regarding the significance of EOBs. These documents not only help patients comprehend their healthcare expenses but also serve as a safeguard against billing errors and misunderstandings. By detailing the components of an EOB, including client information, claim summaries, and financial responsibilities, patients are empowered to make informed decisions. Additionally, examining common scenarios related to EOBs underscores the necessity for proactive engagement in managing healthcare costs, preventing unexpected charges or claim denials.
In conclusion, the importance of understanding EOBs cannot be overstated. They play a crucial role in fostering transparency between patients and providers, ultimately leading to improved financial management and trust in the healthcare system. By taking the time to review and comprehend EOBs, patients can better track their medical expenses, resolve discrepancies, and ensure they are receiving the full benefits of their health coverage. Interacting with EOBs not only bolsters individual financial accountability but also streamlines the healthcare billing process for all stakeholders.
Frequently Asked Questions
What is a Summary of Benefits (EOB)?
A Summary of Benefits (EOB) is a document provided by health coverage firms that details the medical treatments received by an individual, outlining how a claim was processed, the expenses associated with the services rendered, the amount covered by the insurance provider, and the individual’s financial responsibility.
Is an EOB an invoice or payment request?
No, an EOB is not an invoice or payment request. It helps individuals understand their healthcare costs and coverage.
What information is typically included in an EOB?
An EOB typically contains the following information: the date of service, the type of service provided, the total billed amount, the insurance coverage amount, and any responsibility of the individual, including copayments or deductibles.
What is the Member Responsibility section of an EOB?
The Member Responsibility section shows what an individual owes after deductibles, copays, or coinsurance are taken into account.
Why is it important to compare the EOB with the provider’s bill?
It is important to compare the EOB with the provider’s bill to ensure accuracy before making any payments, as discrepancies can arise, such as unexpected claim denials or differences between the EOB and the provider’s bill.
How can inaccurate coding affect the claims process?
Inaccurate coding can complicate the claims process, leading to delays and increased workload for medical practices.
How does Healthcare Partners Consulting help with coding issues?
Healthcare Partners Consulting addresses coding challenges by reviewing and correcting coding issues before claims are submitted, enhancing compliance and streamlining operations.
Why is understanding an EOB important for patients?
Understanding an EOB is crucial for patients to evaluate their financial obligations and manage healthcare costs efficiently.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting