General
Why Benefit Verification is Important for Mental Health Clinics

Introduction
The landscape of mental health care is often complicated by the nuances of insurance coverage, making benefit verification an essential component for ensuring financial stability and patient satisfaction. This process not only confirms the details of a patient’s insurance plan but also significantly impacts the revenue cycle management of mental health clinics. The stakes are considerable; inaccuracies in benefit verification can result in claim denials, unexpected patient charges, and a deterioration of trust.
How can mental health facilities effectively address these challenges to improve operational efficiency and strengthen patient relationships?
Define Benefit Verification and Its Role in Revenue Cycle Management
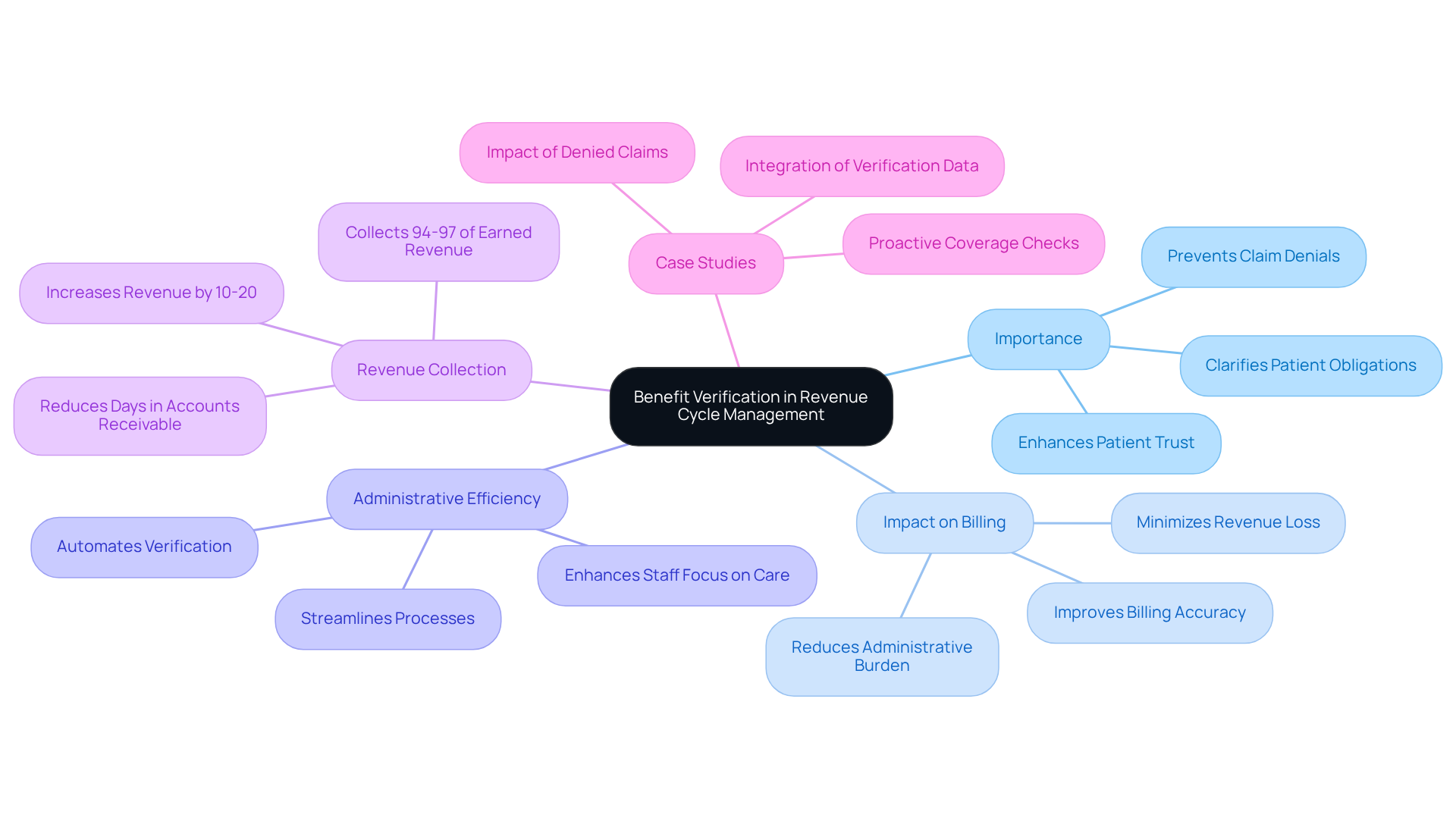
Coverage confirmation is a critical process that highlights why benefit verification is important, as it validates an individual’s insurance protection and the specific benefits available under their plan prior to treatment. This step is essential in revenue cycle management, illustrating why benefit verification is important, as it allows healthcare providers to accurately bill for services rendered and avoid costly claim denials. In mental health facilities, where services can be diverse and complex, knowing why benefit verification is important helps clarify which treatments are included, the extent of that coverage, and any patient obligations, such as co-pays or deductibles. Establishing this information upfront highlights why benefit verification is important, as it not only streamlines billing processes but also significantly reduces administrative burdens and enhances overall financial health.
Healthcare Partners Consulting brings over 37 years of experience in optimizing revenue cycle management (RCM) for mental health practices. Their proactive workflows minimize denials and simplify documentation, highlighting why benefit verification is important for clinics to effectively manage benefit confirmation. The revenue impact of systematic coding inaccuracies can exceed $60,000 per clinician annually, highlighting the financial stakes involved. Furthermore, it is essential to understand why benefit verification is important, as efficient eligibility assessment can reduce claim denials due to incorrect or absent insurance details, which is particularly crucial given that the typical denial rate for behavioral health practices hovers around 11.8 percent. Over three-quarters of healthcare practitioners identify claims denials as a significant issue, with each rejected claim costing between $25 and $45 to resubmit, thereby straining finances and limiting resources for care.
Case studies illustrate the benefits of proactive validation. For instance, clinics that identify potential coverage concerns during checks and address them with patients before providing services can prevent unexpected charges, thereby enhancing patient confidence and satisfaction. Additionally, practices that recognize why benefit verification is important and consistently verify eligibility before each session collect between 94 and 97 percent of earned revenue, in contrast to those that do not, which often experience lower collection rates. Behavioral health practices typically achieve 10 to 20 percent more revenue with optimized revenue cycle management compared to general medical billing.
Expert opinions emphasize why benefit verification is important, noting that implementing real-time eligibility checks before each appointment can significantly improve revenue cycle metrics. As payer requirements become increasingly stringent, it is critical to understand why benefit verification is important for comprehensive entitlement assessment. By investing in robust validation methods that comply with HIPAA and payer-specific regulations, mental health facilities can ensure financial stability, reduce administrative burdens, and ultimately focus more on delivering high-quality care.
Examine the Consequences of Poor Benefit Verification on Financial Health
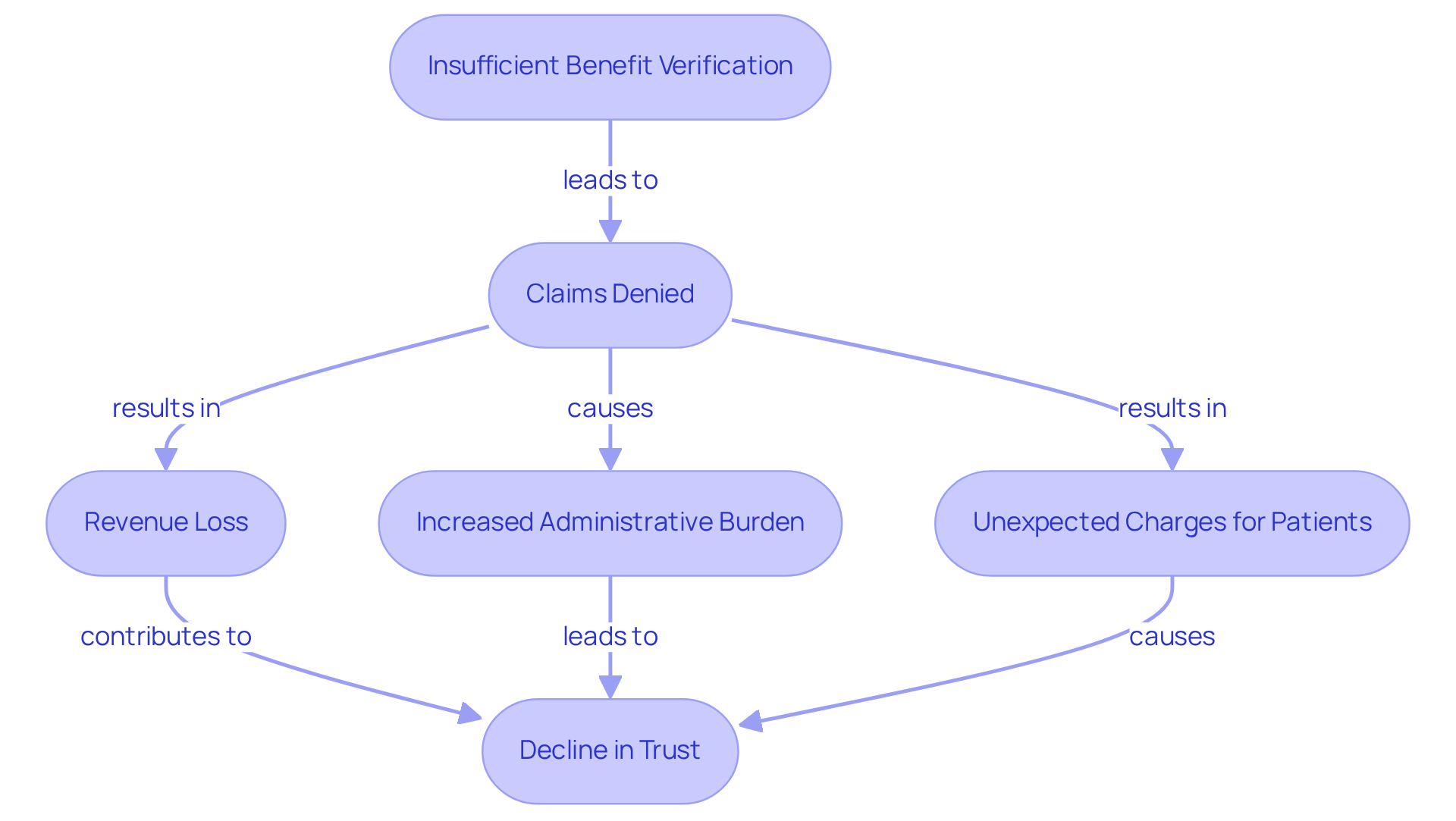
Insufficient verification of advantages highlights why benefit verification is important, as it can lead to significant financial challenges for mental health facilities. When healthcare providers fail to accurately confirm a patient’s benefits, they risk submitting claims that may be denied, which illustrates why benefit verification is important to prevent issues related to inadequate coverage or incorrect billing codes. This not only results in substantial revenue loss but also increases the administrative burden, as staff must allocate additional time to address denied claims. Patients may encounter unexpected charges, leading to dissatisfaction and a decline in trust towards the facility. The financial stability of a practice can be severely compromised; studies indicate that approximately 24% of all claim denials arise from eligibility errors, with as many as 60% of denied claims never being resubmitted. This underscores why benefit verification is important to ensure the financial health of mental health facilities through robust support assessment procedures.
Analyze the Impact of Benefit Verification on Patient Trust and Practice Success
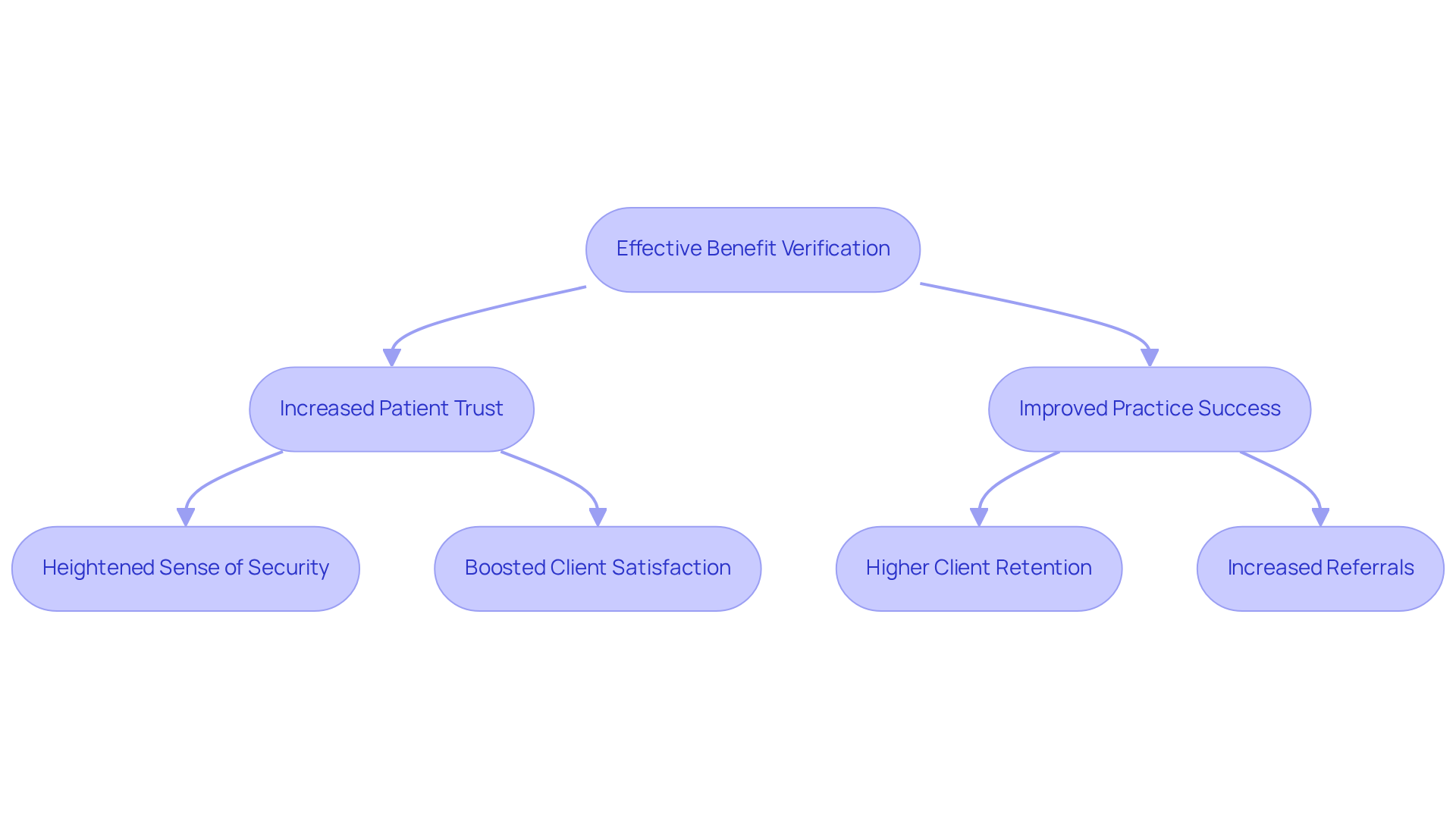
Effective benefit verification is important for building trust between individuals and mental health clinics. When individuals are informed about their coverage and potential out-of-pocket expenses prior to treatment, they experience a heightened sense of security regarding their financial obligations and the care they receive. This transparency significantly boosts client satisfaction, which is essential for the success of any practice.
Clinics that prioritize benefit confirmation frequently report improved client retention and increased referrals; satisfied individuals are more likely to recommend services to others. For instance, Healthcare Partners Consulting implements organized validation procedures that have shown to enhance transparency and trust, leading to notable increases in client loyalty and collections.
Conversely, clinics that struggle with confirmation may suffer reputational damage, as individuals confronted with unexpected expenses tend to share negative experiences, adversely affecting the clinic’s ability to attract new clients. Research indicates that 40% of individuals may cancel or postpone care if they do not receive a clear cost estimate beforehand.
Thus, recognizing why benefit verification is important not only mitigates financial surprises but also plays a vital role in fostering enduring relationships with individuals, ultimately contributing to the overall success of mental health practices.
Explore Strategies for Effective Benefit Verification to Enhance Practice Efficiency
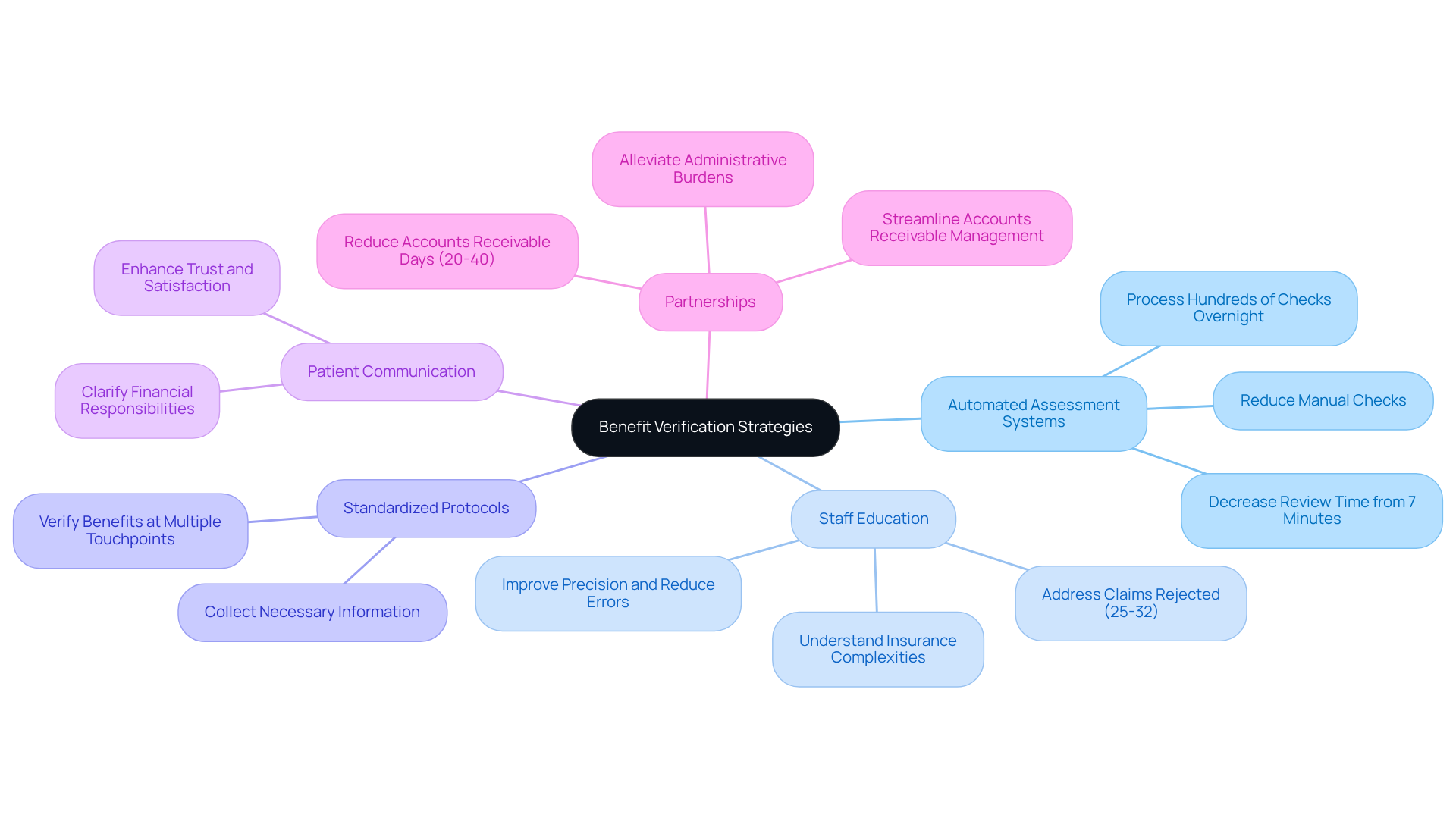
To enhance practice efficiency, mental health clinics can implement several strategies that illustrate why benefit verification is important. Automated assessment systems can drastically reduce the time and effort associated with manual checks, allowing staff to concentrate more on patient care. For instance, these systems can handle hundreds of checks overnight, significantly decreasing the average manual review time of seven minutes per check.
Additionally, educating personnel on the complexities of insurance plans and validation procedures can lead to improved precision and a reduction in errors, addressing the 25-32% of claims rejected due to eligibility concerns. Establishing a standardized protocol for verifying benefits at multiple touchpoints, such as during client intake and prior to appointments, highlights why benefit verification is important, as it ensures that all necessary information is collected and validated. This is crucial in illustrating why benefit verification is important, as the U.S. healthcare industry spends $43 billion annually on eligibility verification.
Moreover, fostering transparent dialogue with patients regarding their insurance coverage and potential expenses can enhance trust and satisfaction, ultimately benefiting the clinic’s reputation and financial stability. By integrating these strategies, mental health clinics can optimize their operations and minimize revenue leakage, positioning themselves for greater success in a competitive landscape.
Furthermore, partnering with Healthcare Partners Consulting can streamline accounts receivable management through features like the Monthly AR Report and proactive follow-up with payers. This partnership can lead to a 20-40% reduction in accounts receivable days and improved cash flow, while also alleviating the administrative burdens that often hinder practice efficiency.
Conclusion
The importance of benefit verification in mental health clinics is paramount. This critical process not only ensures accurate billing for services but also protects against the financial risks associated with claim denials. By confirming insurance coverage and understanding the specifics of patient benefits, clinics can optimize their revenue cycle management and improve operational efficiency.
Key insights throughout this article have underscored the repercussions of inadequate benefit verification, including increased claim denials and a decline in patient trust. The financial implications are significant, with potential revenue losses and administrative burdens that threaten a clinic’s stability. In contrast, effective benefit verification promotes transparency, enhances patient satisfaction, and ultimately contributes to the success of the practice by improving client retention and referrals.
Given these insights, mental health clinics must prioritize benefit verification as a fundamental aspect of their operations. By investing in robust verification strategies, clinics can not only reduce financial risks but also cultivate enduring relationships with patients. Adopting these practices is essential for achieving both financial stability and high-quality care in an increasingly competitive environment.
Frequently Asked Questions
What is benefit verification and why is it important in revenue cycle management?
Benefit verification is the process of confirming an individual’s insurance coverage and the specific benefits available under their plan before treatment. It is important in revenue cycle management as it helps healthcare providers accurately bill for services and avoid costly claim denials.
How does benefit verification affect mental health facilities specifically?
In mental health facilities, benefit verification clarifies which treatments are covered, the extent of that coverage, and any patient obligations like co-pays or deductibles. This upfront information streamlines billing processes, reduces administrative burdens, and enhances overall financial health.
What are the financial implications of not performing benefit verification?
Systematic coding inaccuracies can lead to significant revenue loss, exceeding $60,000 per clinician annually. Additionally, the typical denial rate for behavioral health practices is around 11.8 percent, and each rejected claim can cost between $25 and $45 to resubmit.
How can proactive benefit verification improve revenue collection?
Clinics that verify eligibility before each session can collect between 94 and 97 percent of earned revenue, compared to those that do not, which often experience lower collection rates. Optimized revenue cycle management can yield 10 to 20 percent more revenue for behavioral health practices compared to general medical billing.
What role does real-time eligibility checking play in benefit verification?
Implementing real-time eligibility checks before appointments can significantly improve revenue cycle metrics and help ensure compliance with payer requirements, enhancing financial stability for mental health facilities.
What are the benefits of addressing coverage concerns early in the process?
Identifying potential coverage issues during checks and discussing them with patients before services are provided can prevent unexpected charges, thereby enhancing patient confidence and satisfaction.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting