Telehealth Billing Insights
4 Essential Features of Clearinghouse Billing Software for Clinics

Introduction
Many clinics struggle to manage the complexities of healthcare billing effectively, often leading to financial challenges. Clearinghouse billing software emerges as a critical asset, providing essential features that streamline operations, enhance financial performance, and improve patient interactions. Clinics must identify the functionalities that are essential for their success amidst numerous options. This article examines four essential features of clearinghouse billing software that clinics should consider to navigate billing complexities and enhance revenue potential.
Healthcare Partners Consulting: Comprehensive Support for Mental Health Billing
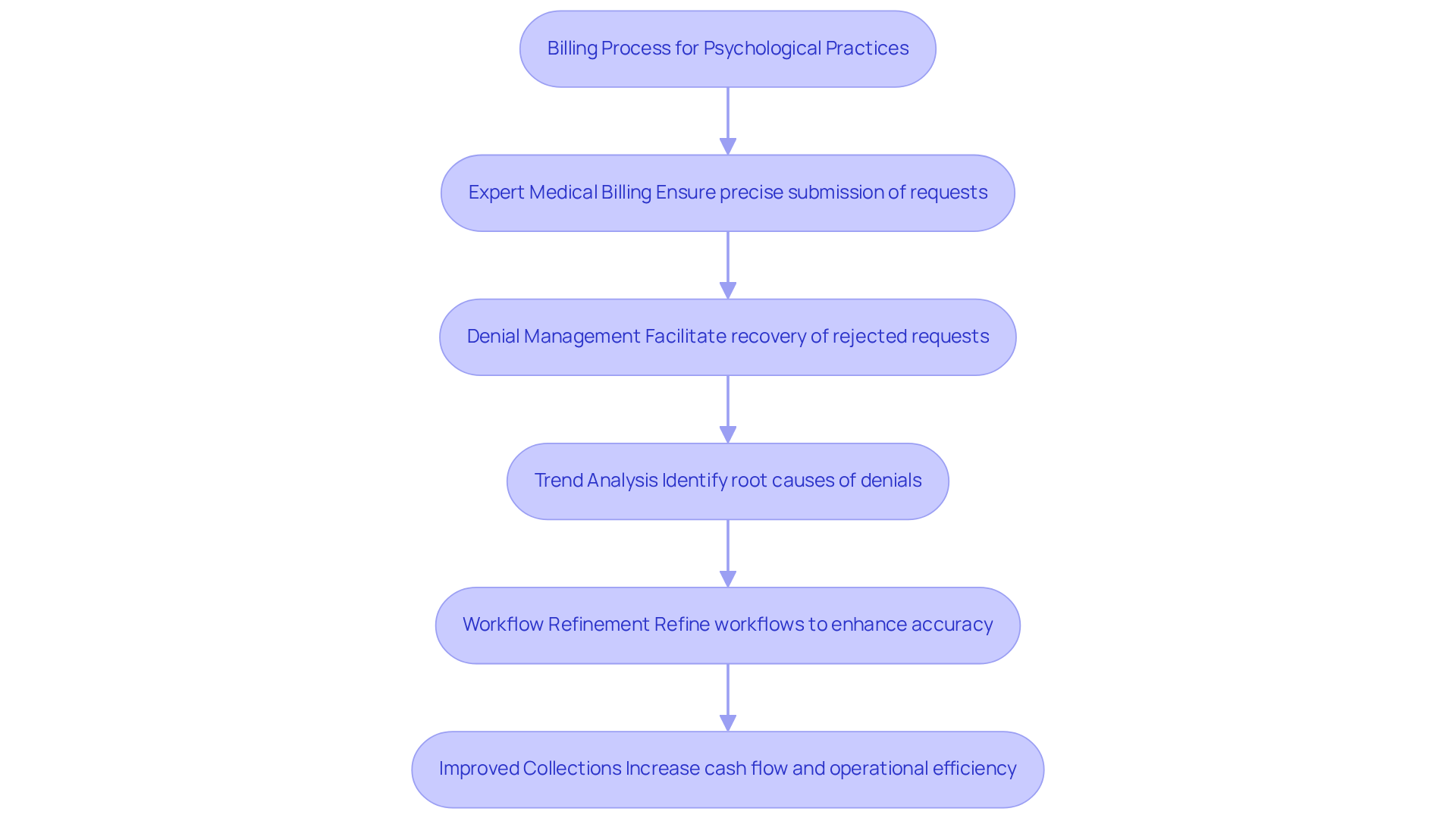
As psychological practices navigate an increasingly complex billing landscape, specialized administrative support becomes essential. Healthcare Partners Consulting (HPC) offers expert medical billing and denial management services tailored for psychological practices. These services ensure precise submission of requests and maximize revenue.
As the landscape of psychological billing evolves in 2026, practices are increasingly reliant on expert advice to navigate complex insurance requirements and compliance challenges. HPC’s denial management strategies facilitate the recovery of rejected requests, leading to improved collections and increased cash flow.
By analyzing trends to identify root causes and refining workflows, HPC achieves a 30-50% reduction in recurring denial types, significantly alleviating administrative burdens and enhancing billing accuracy. This comprehensive support is crucial for clinics seeking to enhance operational efficiency and prioritize the delivery of high-quality mental health services.
Claims Scrubbing: Ensuring Accuracy and Reducing Denials
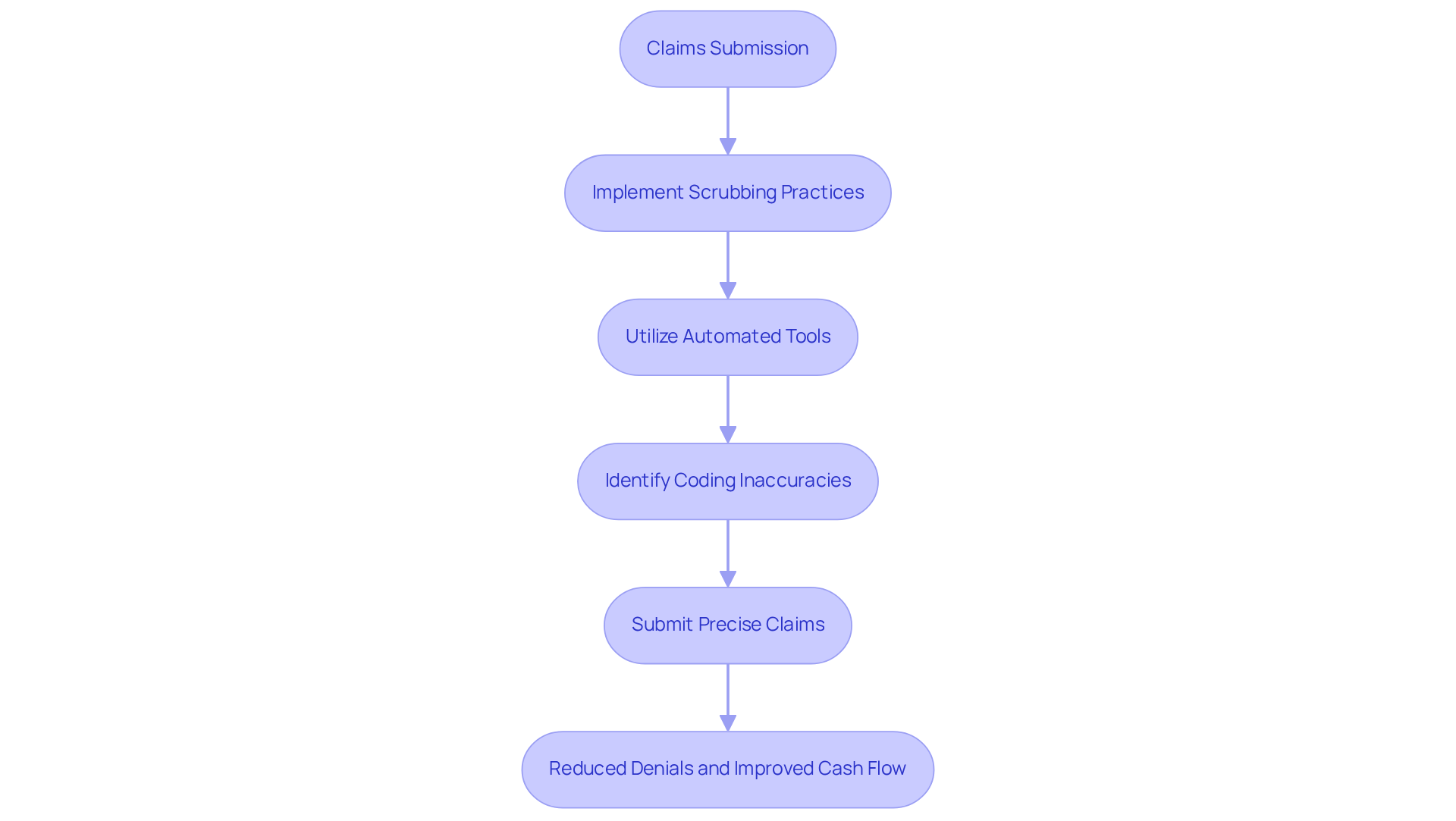
Claims cleaning is essential for effective billing in healthcare, as it directly impacts revenue cycle management. This proactive approach ensures compliance with payer requirements and reduces the risk of denials. Clinics often struggle with claim denials, but implementing strong scrubbing practices can lead to significant advancements in their revenue cycle management. Precise submissions enable faster reimbursements and improve cash flow.
Industry experts highlight that effective scrubbing practices reduce errors and streamline the billing process, allowing mental health providers to focus more on patient care instead of dealing with administrative obstacles. Recent advancements in billing scrubbing technology, such as automated tools that identify coding inaccuracies, enable clinics to recover lost revenue and enhance operational efficiency.
For instance, practices utilizing claims scrubbing tools have reported a 50% reduction in claim denials, underscoring the importance of this feature in optimizing financial performance. Furthermore, resources such as the crucial toolkit for wellness providers streamline credentialing and administrative duties, additionally aiding clinics in managing the intricacies of billing.
Insights from industry experts, including Davia Ward, underscore the ongoing mental health billing crisis, stressing the need for effective solutions that improve healthcare efficiency and client satisfaction. Addressing these challenges through effective claims scrubbing can transform the financial landscape for mental health providers.
Insurance Eligibility Verification: Streamlining Patient Coverage Checks
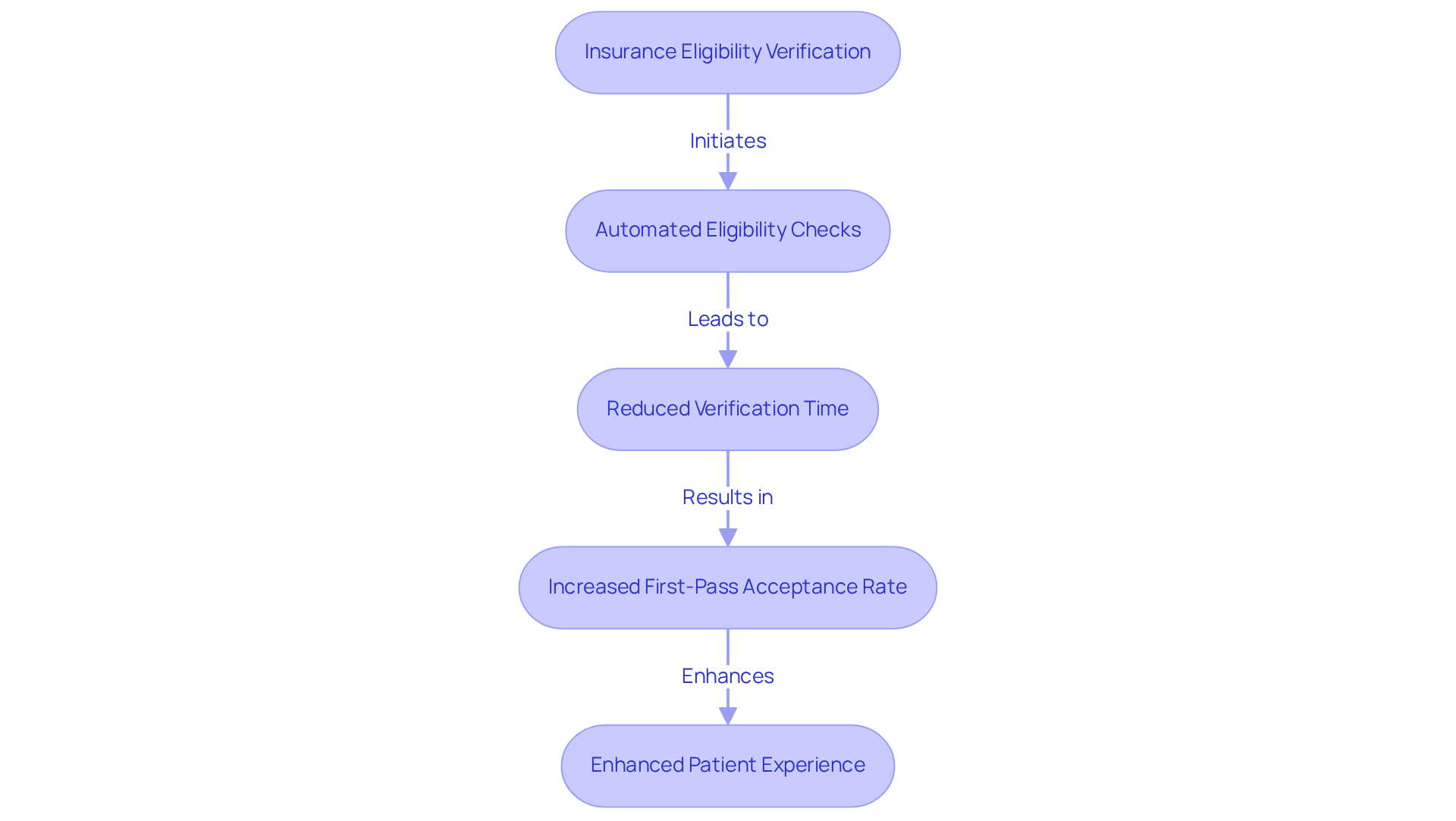
Verifying insurance eligibility is crucial for ensuring seamless billing and service delivery in healthcare. This process is enhanced by clearinghouse billing software, which automates eligibility checks, simplifies intake, and reduces the risk of denial issues related to coverage. In 2026, nearly 1 in 5 in-network claims are denied initially, primarily due to eligibility and registration errors, underscoring the necessity for effective verification systems.
Automated eligibility checks not only ensure that clinics deliver services to individuals with active insurance but also enhance satisfaction and financial stability. For instance, practices utilizing automated verification tools can reduce verification time to under five seconds, leading to a first-pass acceptance rate of 94% to 96%. This efficiency enables staff to concentrate more on interactions with clients instead of administrative tasks, ultimately enhancing the overall experience for patients.
Clinics using these technologies have seen real improvements in how they handle client intake. For instance, one clinic introduced real-time eligibility checks and observed a significant reduction in check-in delays and manual tasks for staff, resulting in a more efficient and satisfactory experience for patients. Healthcare professionals emphasize that efficient eligibility verification not only saves time but also reduces unexpected out-of-pocket expenses for individuals, fostering trust and satisfaction.
Additionally, denial management and appeals processes are crucial for recovering underpaid or denied claims, further enhancing the financial health of clinics. As individuals increasingly expect clear and accurate pricing information, automated systems that provide upfront estimates based on verified coverage are becoming essential. This proactive approach not only improves communication with clients but also aligns with the No Surprises Act, which mandates good-faith estimates for scheduled services. By adopting automated verification and denial management strategies, clinics can not only enhance their financial health but also build lasting trust with their patients.
Electronic Remittance Advice (ERA) Processing: Enhancing Payment Reconciliation
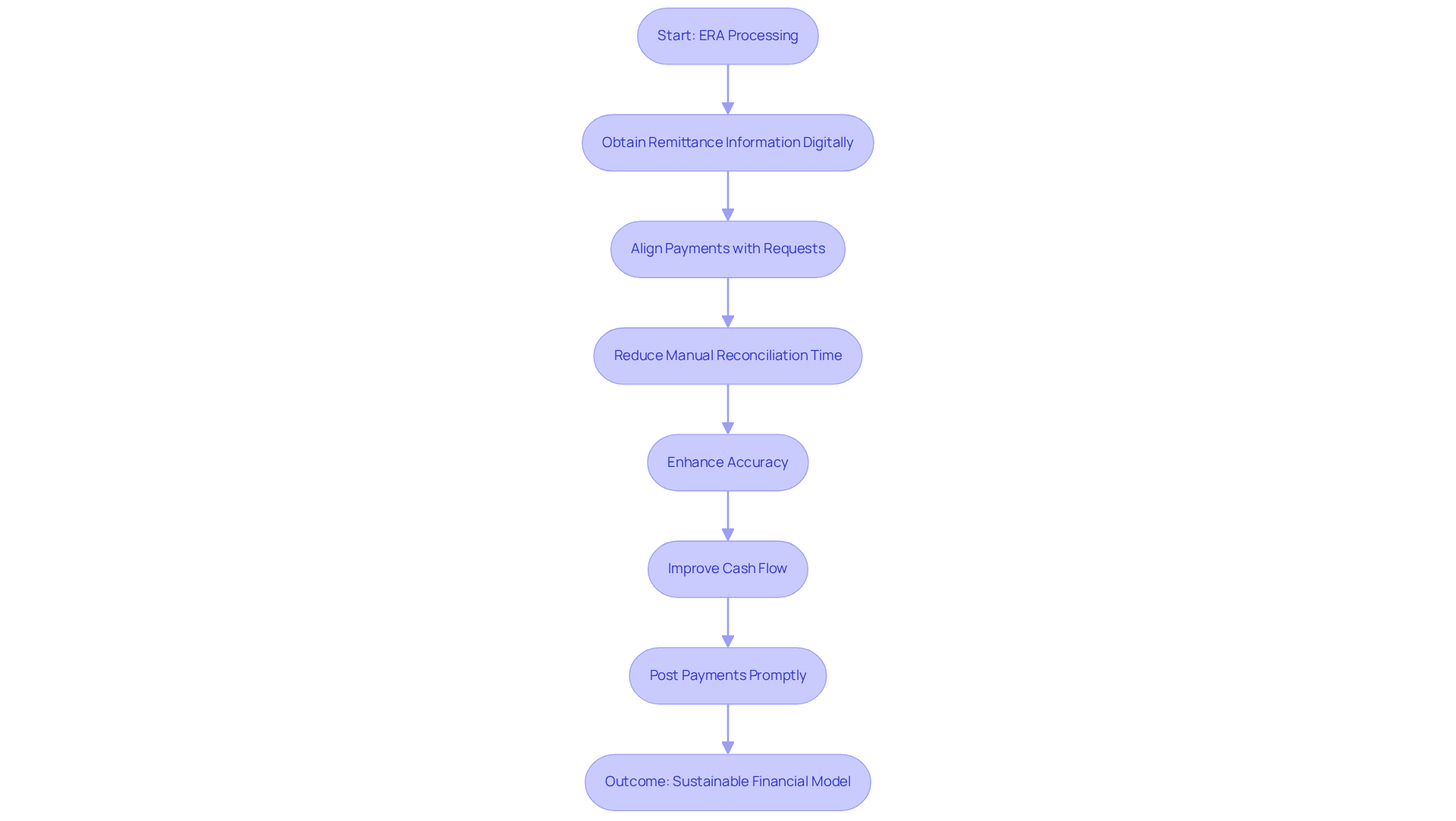
Electronic Remittance Advice (ERA) processing significantly enhances the efficiency of clearinghouse billing software, streamlining the payment reconciliation process. By obtaining remittance information digitally, clinics can efficiently align payments with requests, reducing the time dedicated to manual reconciliation. This automation not only enhances accuracy but also improves cash flow by ensuring that payments are posted promptly.
With Healthcare Partners Consulting’s comprehensive revenue cycle management services, including structured payment plans and monthly AR reports, practices can take advantage of proactive follow-up on unpaid or underpaid claims, which translates to faster payments and reduced staffing burdens.
The toolkit designed for mental health providers further simplifies credentialing and administrative tasks, allowing practices to focus on patient care rather than administrative burdens. Ultimately, this focus on automation and efficiency fosters a more sustainable financial model for healthcare practices.
Conclusion
Optimizing administrative processes in healthcare clinics, particularly in mental health practices, hinges on effective billing software solutions. Clearinghouse billing software plays a pivotal role in this optimization. By leveraging advanced features such as claims scrubbing, insurance eligibility verification, and electronic remittance advice processing, clinics can significantly enhance their billing accuracy, streamline operations, and ultimately improve patient satisfaction.
This discussion highlights four essential features crucial for effective billing management:
- Claims scrubbing drastically reduces denial rates.
- Verifying insurance eligibility helps avoid unnecessary delays.
- Electronic remittance advice processing facilitates quicker payment reconciliations.
- These elements streamline the revenue cycle, enabling healthcare providers to concentrate on delivering quality care instead of being overwhelmed by administrative tasks.
In a complex billing landscape, clinics must adopt these features to ensure their operational success. Embracing automated systems and expert support can transform the financial health of practices, ensuring they remain viable while providing high-quality mental health services. By prioritizing these technologies, clinics can not only enhance their operational efficiency but also foster stronger relationships with their patients.
Frequently Asked Questions
What services does Healthcare Partners Consulting (HPC) provide for psychological practices?
HPC offers expert medical billing and denial management services tailored specifically for psychological practices, ensuring precise submission of requests and maximizing revenue.
Why is specialized administrative support important for psychological practices?
As the billing landscape becomes more complex, specialized administrative support is essential for navigating insurance requirements and compliance challenges effectively.
How does HPC help with denial management?
HPC employs denial management strategies that facilitate the recovery of rejected requests, which leads to improved collections and increased cash flow for practices.
What impact does HPC’s analysis of trends have on billing?
By analyzing trends to identify root causes and refining workflows, HPC achieves a 30-50% reduction in recurring denial types, which alleviates administrative burdens and enhances billing accuracy.
How does HPC’s support benefit clinics?
HPC’s comprehensive support is crucial for clinics aiming to enhance operational efficiency while prioritizing the delivery of high-quality mental health services.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting