Telehealth Billing Insights
Which of the Following Is a HIPAA Rule? 10 Essential Guidelines for Clinics

Introduction
Healthcare data breaches highlight the critical role of the Health Insurance Portability and Accountability Act (HIPAA) in safeguarding patient privacy. This legislation establishes crucial standards for protecting sensitive medical information and serves as a lifeline for healthcare providers striving to maintain trust and avoid severe penalties. Clinics face significant challenges in understanding and implementing HIPAA regulations, leading to the question: what essential guidelines must they follow to navigate the labyrinth of HIPAA regulations effectively? This article outlines ten essential HIPAA rules that every clinic must comprehend to ensure compliance and protect sensitive patient information.
Understand the Health Insurance Portability and Accountability Act (HIPAA)
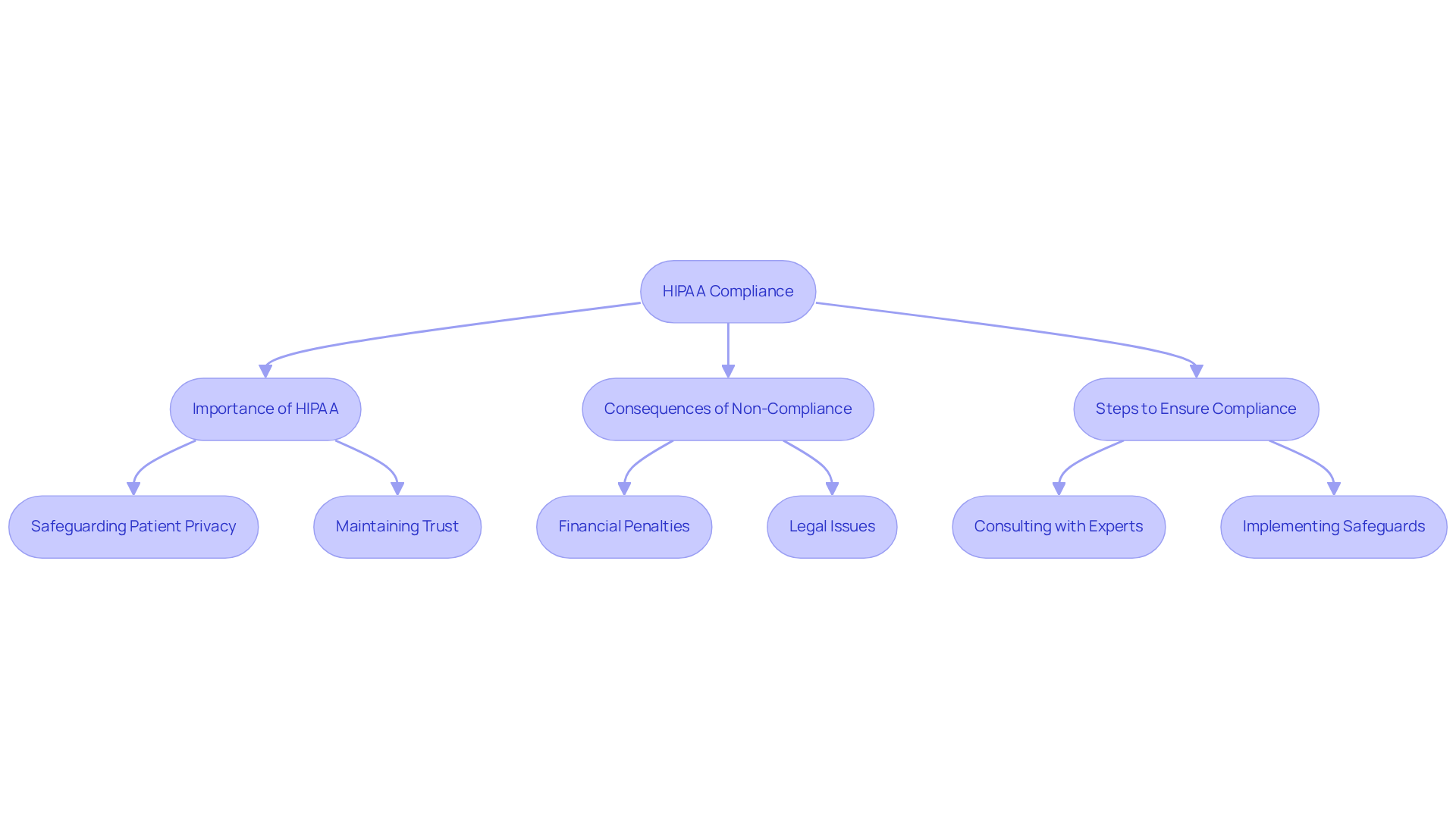
The increasing frequency of healthcare data breaches highlights the critical importance of the Health Insurance Portability and Accountability Act (HIPAA) in safeguarding patient privacy. By establishing national standards for the protection of health information, the act mandates that healthcare providers implement robust safeguards to protect sensitive medical data. Complying with health privacy regulations is essential for healthcare facilities to maintain trust and avoid serious legal issues.
However, many healthcare facilities struggle to maintain compliance amidst increasing data breaches. For instance, the HHS Office for Civil Rights reported a staggering increase in healthcare data breaches, with 63 breaches affecting 500 or more individuals reported in February 2026. These incidents highlight the urgent need for medical facilities to adhere to privacy regulations to protect patient data from unauthorized access and identity theft.
Consider the real-world implications of privacy regulations in clinics. A New York law firm faced a $200,000 fine for privacy regulation violations after a ransomware attack, illustrating the financial dangers linked to non-compliance. Furthermore, New York Presbyterian Hospital consented to a $300,000 settlement for privacy law violations associated with website pixel use, underscoring the financial consequences of failing to adhere to regulations. The HHS emphasizes the need for timely breach notifications to protect individuals from potential harm, reinforcing the importance of strict regulatory compliance.
Specialists in healthcare regulations emphasize that understanding privacy laws is essential for medical facilities. As noted by compliance professionals, “HIPAA not only protects patient privacy but also enhances the overall quality of care by ensuring that sensitive information is handled appropriately.” To further assist healthcare facilities in navigating these complexities, Healthcare Partners Consulting offers personalized consultations. By discussing your practice in a 30-minute call, we can map your current workflow and identify the services that will move the needle fastest. Schedule a meeting with us to ensure that your clinic remains compliant and efficient. Ultimately, neglecting compliance can lead to devastating consequences for both patients and healthcare providers.
Identify When HIPAA Applies to Your Practice
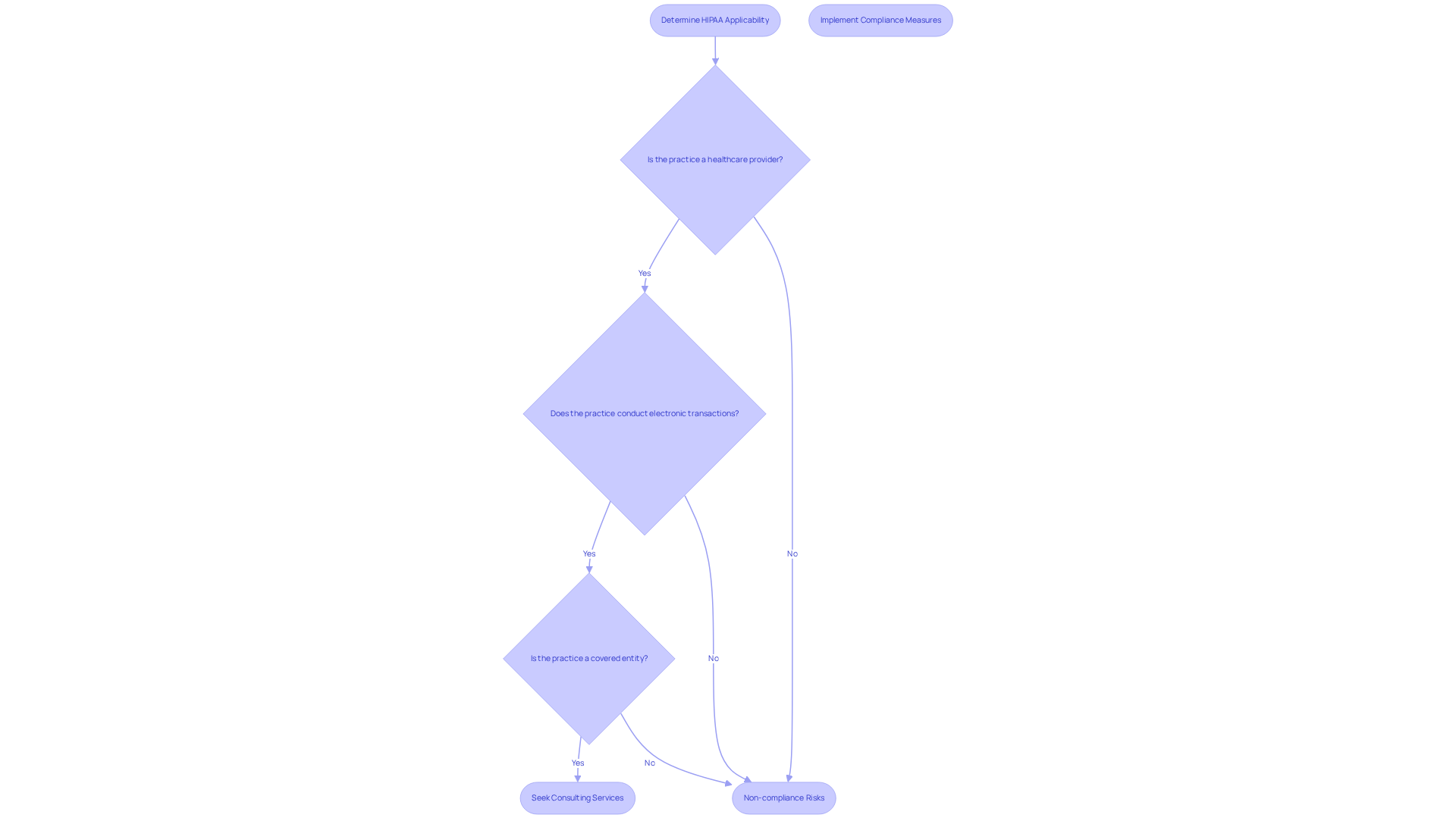
Understanding the implications of the Health Insurance Portability and Accountability Act is crucial for healthcare providers. Clinics must clearly understand when they qualify as ‘covered entities’ under HIPAA to ensure compliance. This understanding helps practices identify their regulatory obligations, as it includes any healthcare provider conducting certain transactions electronically, such as billing and claims processing.
Many clinics face challenges in determining their status as covered entities under HIPAA. This lack of clarity can lead to significant compliance risks and operational inefficiencies.
Healthcare Partners Consulting provides tailored solutions to enhance compliance and streamline operations, ensuring accurate claims processing and fast reimbursement solutions. Their customized consultations help identify the most effective administrative solutions for your practice, improving overall efficiency in managing regulations.
Without a clear grasp of these regulations, clinics risk non-compliance and potential financial setbacks.
Recognize What Constitutes Protected Health Information (PHI)
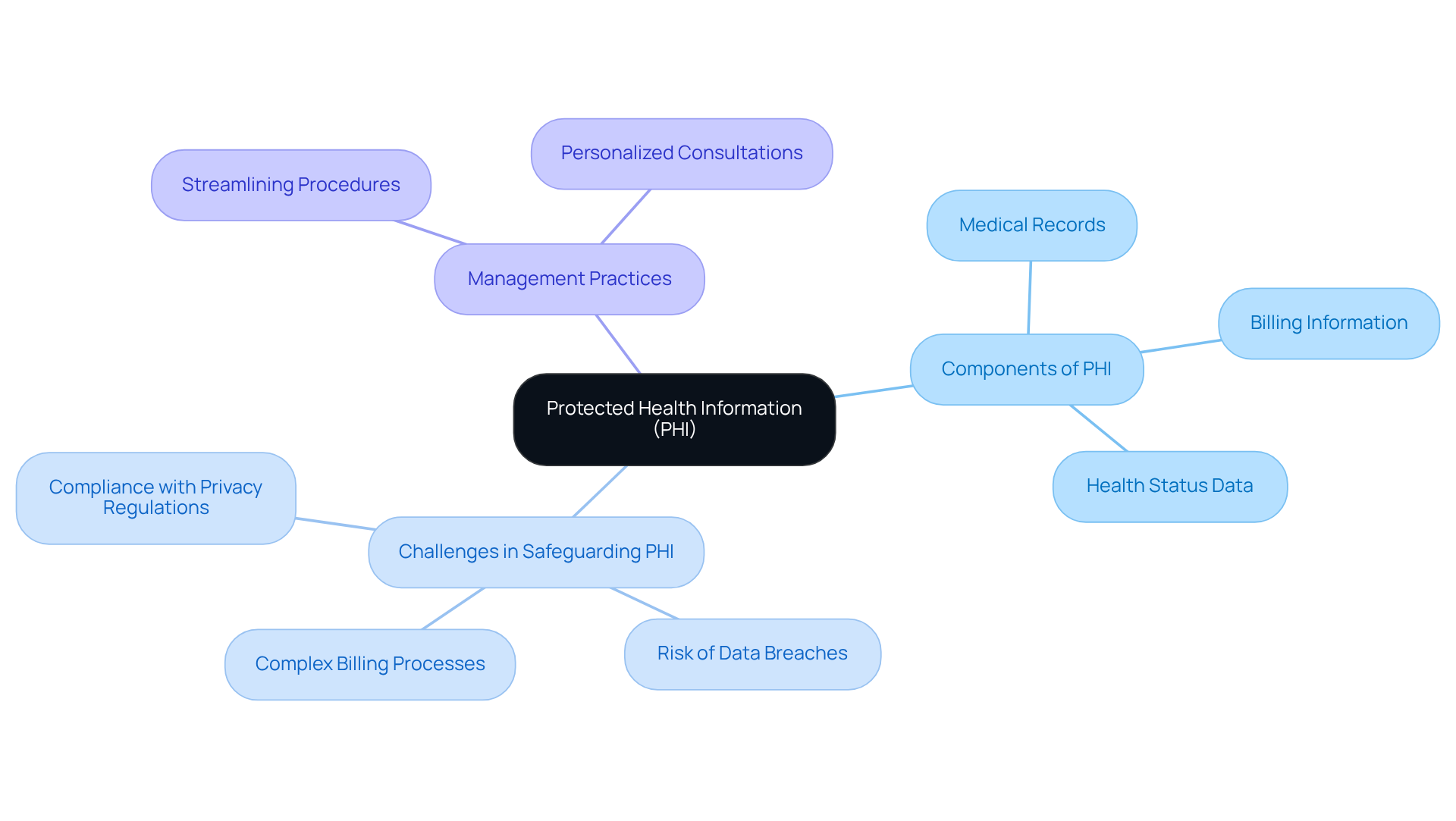
Clinics face significant challenges in safeguarding Protected Health Information (PHI) while managing complex billing processes. PHI encompasses medical records, billing information, and any data that pertains to an individual’s health status. Clinics must ensure that all PHI is adequately safeguarded to comply with privacy regulations, which raises the question of which of the following is a HIPAA rule.
Effective management of patient statements is essential for addressing issues such as underpayments, unprocessed claims, and aging claims in healthcare billing. By streamlining these procedures, facilities can enhance their financial stability and ensure compliance with regulations, which of the following is a HIPAA rule.
Personalized consultations can identify optimal administrative solutions tailored to healthcare practices‘ specific needs. This ensures effective navigation of these complexities.
Learn HIPAA’s 18 Identifiers for Patient Information
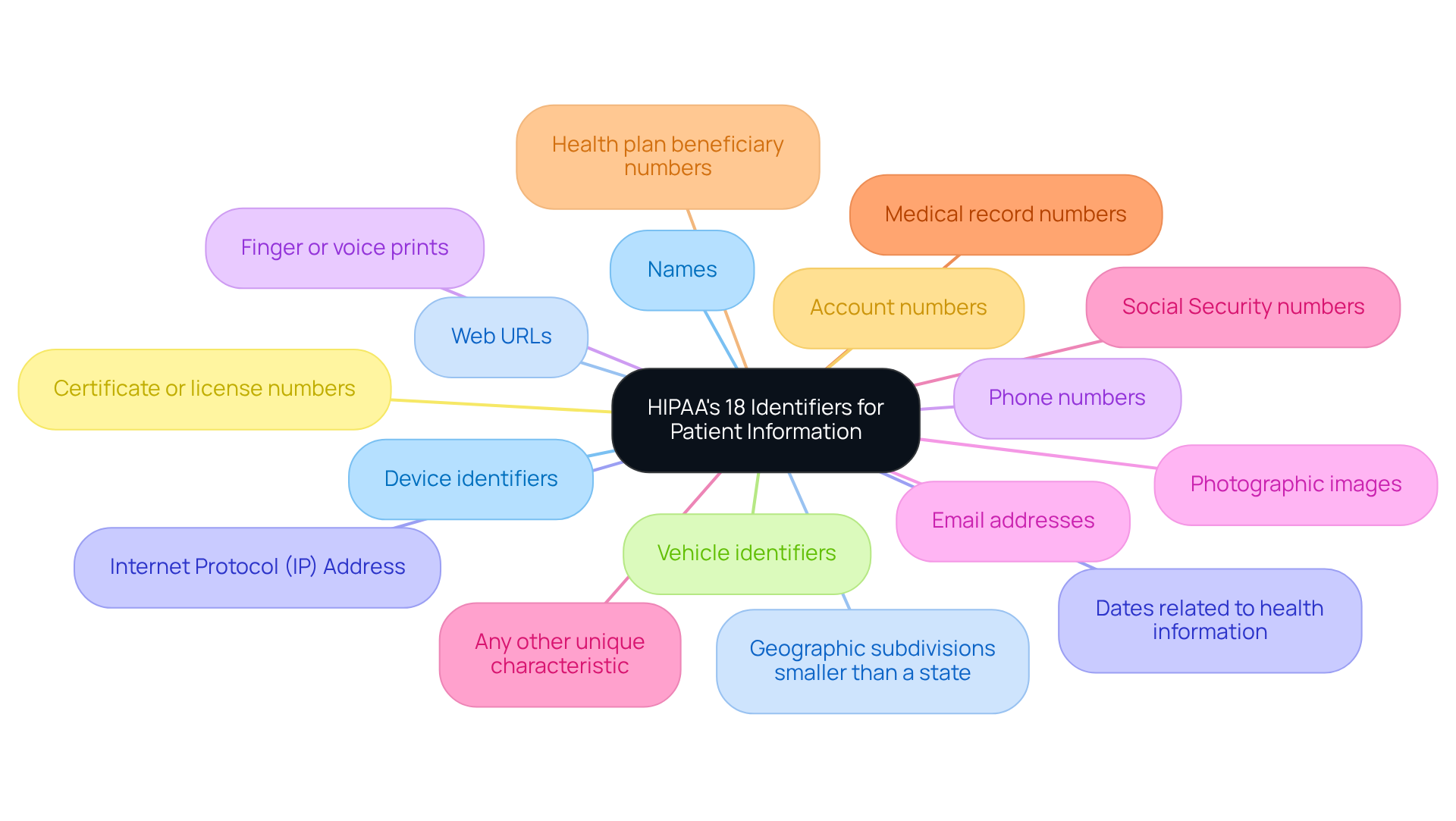
The Health Insurance Portability and Accountability Act outlines 18 specific identifiers that qualify as Protected Health Information (PHI), necessitating stringent compliance measures. These identifiers include:
- Names
- Geographic subdivisions smaller than a state
- Dates related to health information
- Phone numbers
- Email addresses
- Social Security numbers
Healthcare facilities must implement robust measures to safeguard these identifiers in compliance with HIPAA.
Healthcare facilities should consider utilizing automated risk management systems like EPICompliance to enhance regulatory compliance and bolster PHI security. Regular training for staff on handling sensitive information and understanding the implications of data breaches is essential.
As of 2026, clinics must be aware that the deadline for updating the Notice of Privacy Practices (NPP) is February 16, 2026. Effective adherence involves not only documentation but also the demonstrable implementation of security measures. As Gil Vidals, CEO of Vault, emphasizes, “Without implementation, documentation will inevitably fail audits.” Ultimately, the integrity of patient information hinges on the proactive implementation of security protocols.
Understand Personally Identifiable Information (PII) in Healthcare
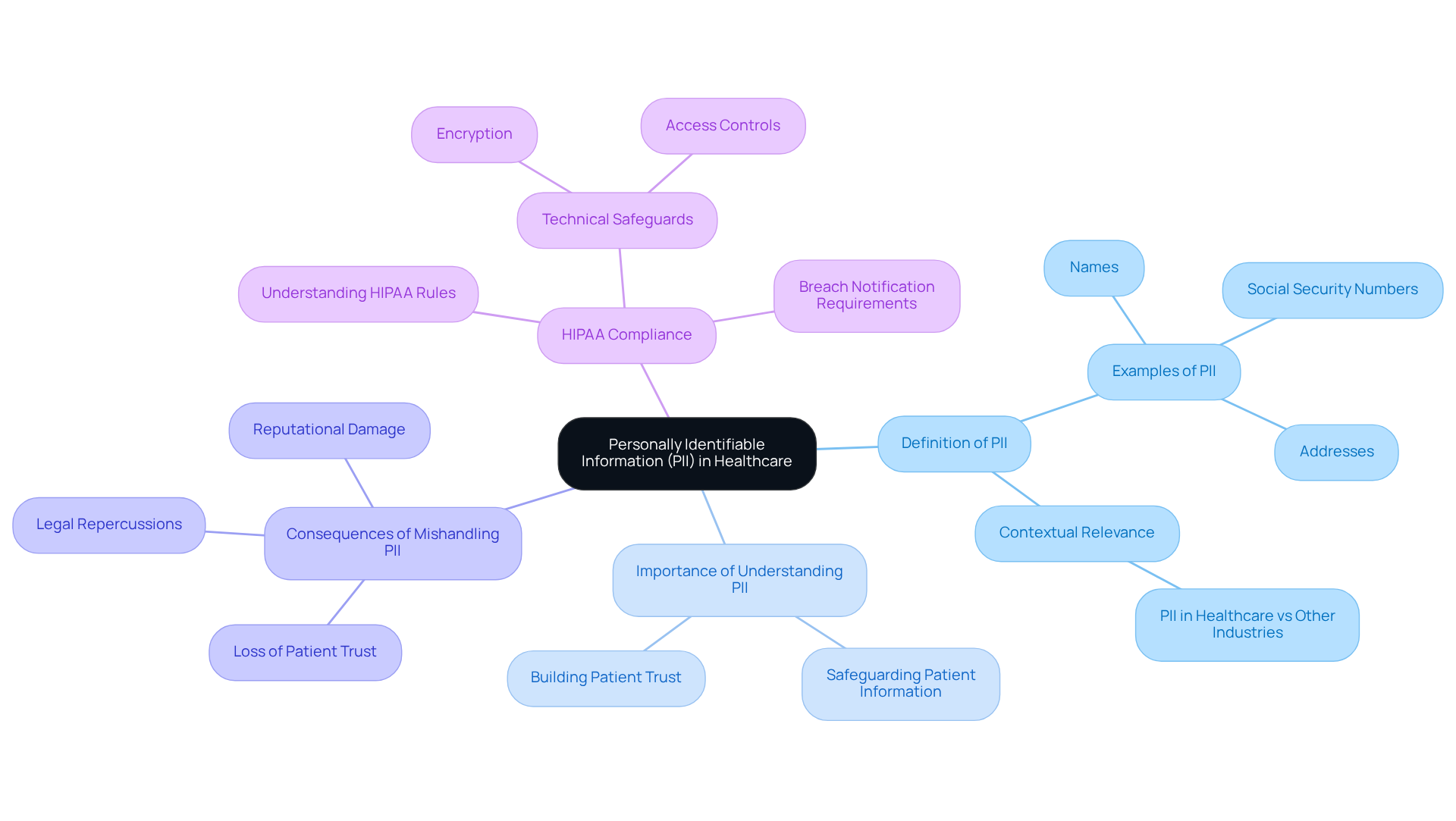
Understanding the nuances of Personally Identifiable Information (PII) is essential for healthcare facilities to navigate the complexities of data protection. PII refers to any data that can be used to identify an individual, such as names, addresses, and Social Security numbers. In the healthcare sector, the intersection of PII and PHI highlights the necessity for facilities to understand which of the following is a HIPAA rule to effectively protect patient data.
Mishandling PII can lead to severe legal repercussions and loss of patient trust. Therefore, comprehending these concepts is essential for safeguarding patient information and ensuring compliance with regulations. Failure to adequately protect PII can result in significant legal and reputational consequences for healthcare organizations.
Identify Examples of Personally Identifiable Information (PII)
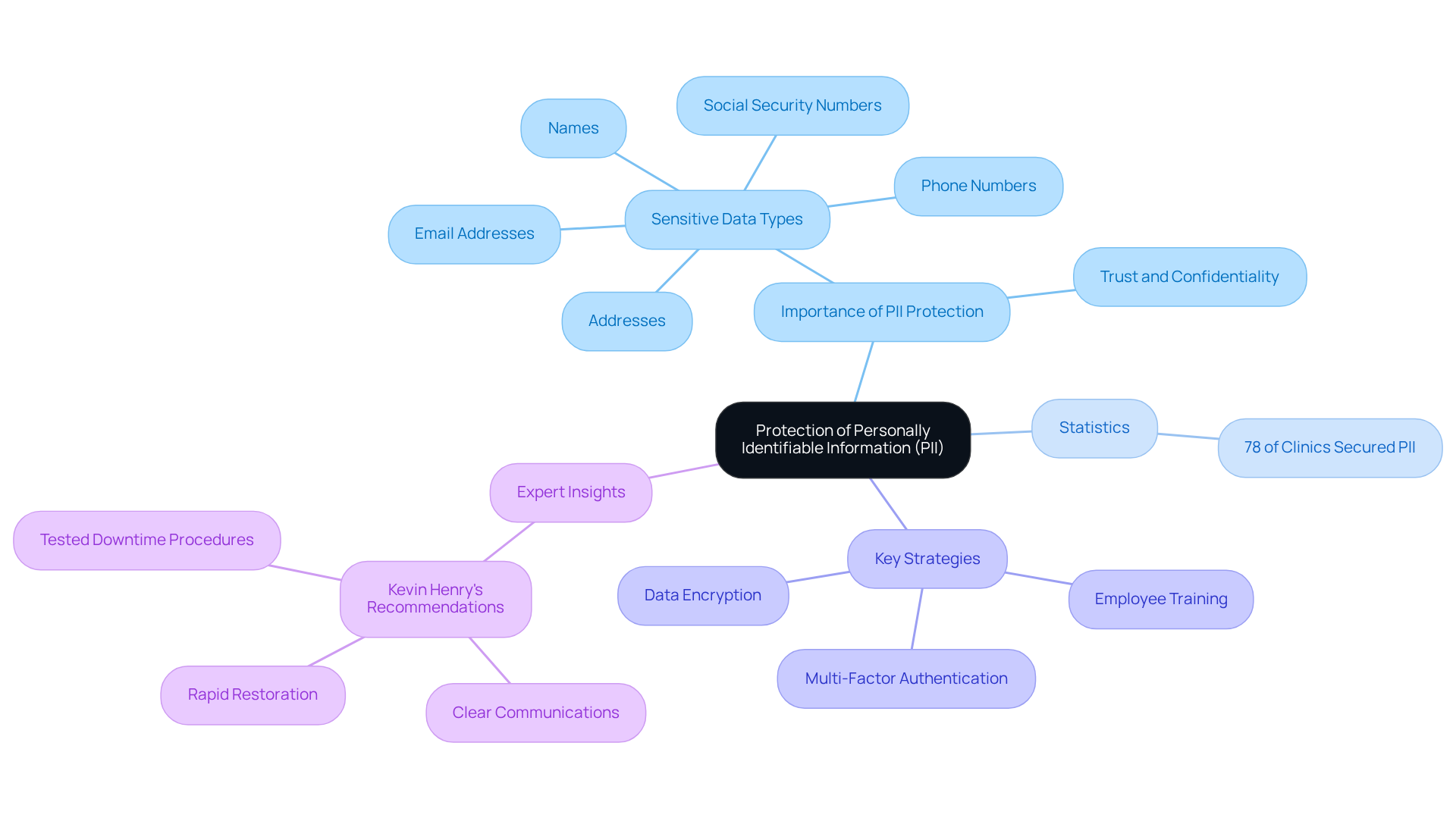
The protection of Personally Identifiable Information (PII) in healthcare is critical, as it includes sensitive data such as names, addresses, phone numbers, email addresses, and Social Security numbers. About 78% of healthcare clinics have implemented measures to secure PII, reflecting a growing awareness of the need for robust data protection.
Key strategies for securing PII involve:
- Encrypting sensitive data
- Training employees on privacy policies
- Implementing multi-factor authentication for medical record access
For instance, a notable healthcare practice recently adopted a comprehensive data protection protocol that emphasizes data classification, encryption, and role-based access controls, along with regular audits of data access logs.
Compliance officers emphasize that securing PII is essential for maintaining trust and confidentiality, beyond just regulatory compliance. As Kevin Henry, an expert in healthcare data security, states, “Clear communications with individuals, rapid restoration, and tested downtime procedures are pivotal to minimize harm.”
Without robust data handling procedures and staff training, clinics risk not only data breaches but also the erosion of patient trust.
Obtain Necessary HIPAA Authorization from Patients
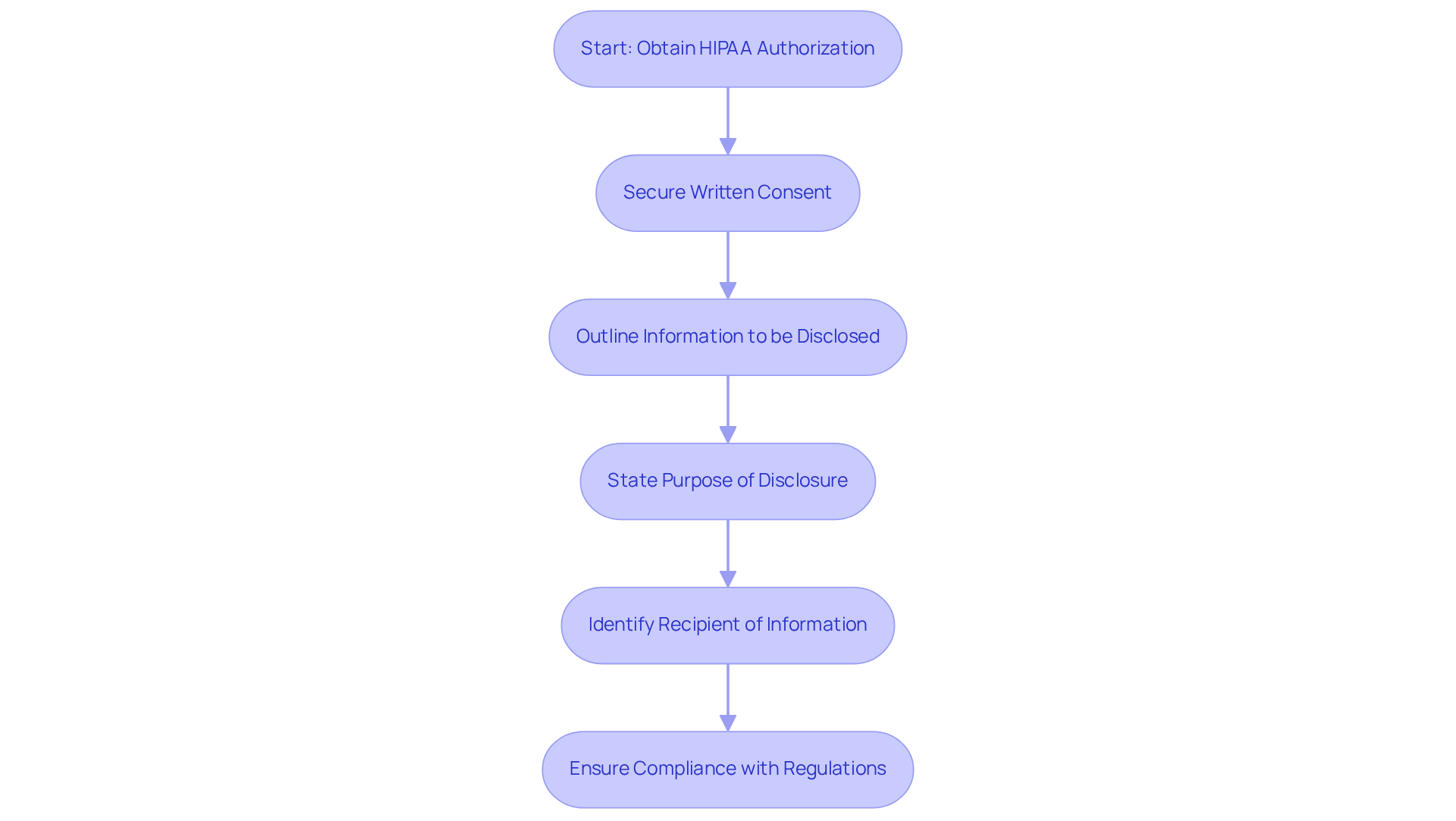
Under privacy regulations, healthcare providers face stringent requirements regarding the use of PHI. They must secure written consent from individuals before utilizing or revealing their PHI for reasons other than treatment, payment, or healthcare operations. This authorization must clearly outline the information to be disclosed, the purpose of the disclosure, and the recipient of the information.
Recent updates to healthcare regulations have increased the focus on consent from individuals, making it essential for providers to ensure they are acquiring authorization correctly. Legal specialists emphasize the significance of explicit client consent, underscoring the critical need for thorough documentation and compliance with current standards. For instance, healthcare attorney Gil Vidals emphasizes that ‘a signed BAA alone is not enough,’ highlighting the necessity for comprehensive documentation and adherence to updated standards.
Clinics that manage their HIPAA authorization processes effectively demonstrate the benefits of robust compliance strategies. For instance, a mental health facility in California established a streamlined authorization process that enhanced client engagement and decreased processing times considerably. This strategic approach ensured compliance while enhancing trust and satisfaction among patients.
As the landscape of healthcare continues to evolve, understanding and implementing the latest authorization requirements, including mandatory encryption at rest and the enforcement of Multi-Factor Authentication (MFA), will be essential for medical facilities aiming to maintain compliance and safeguard individual privacy.
Navigate the Process of Obtaining HIPAA Authorization
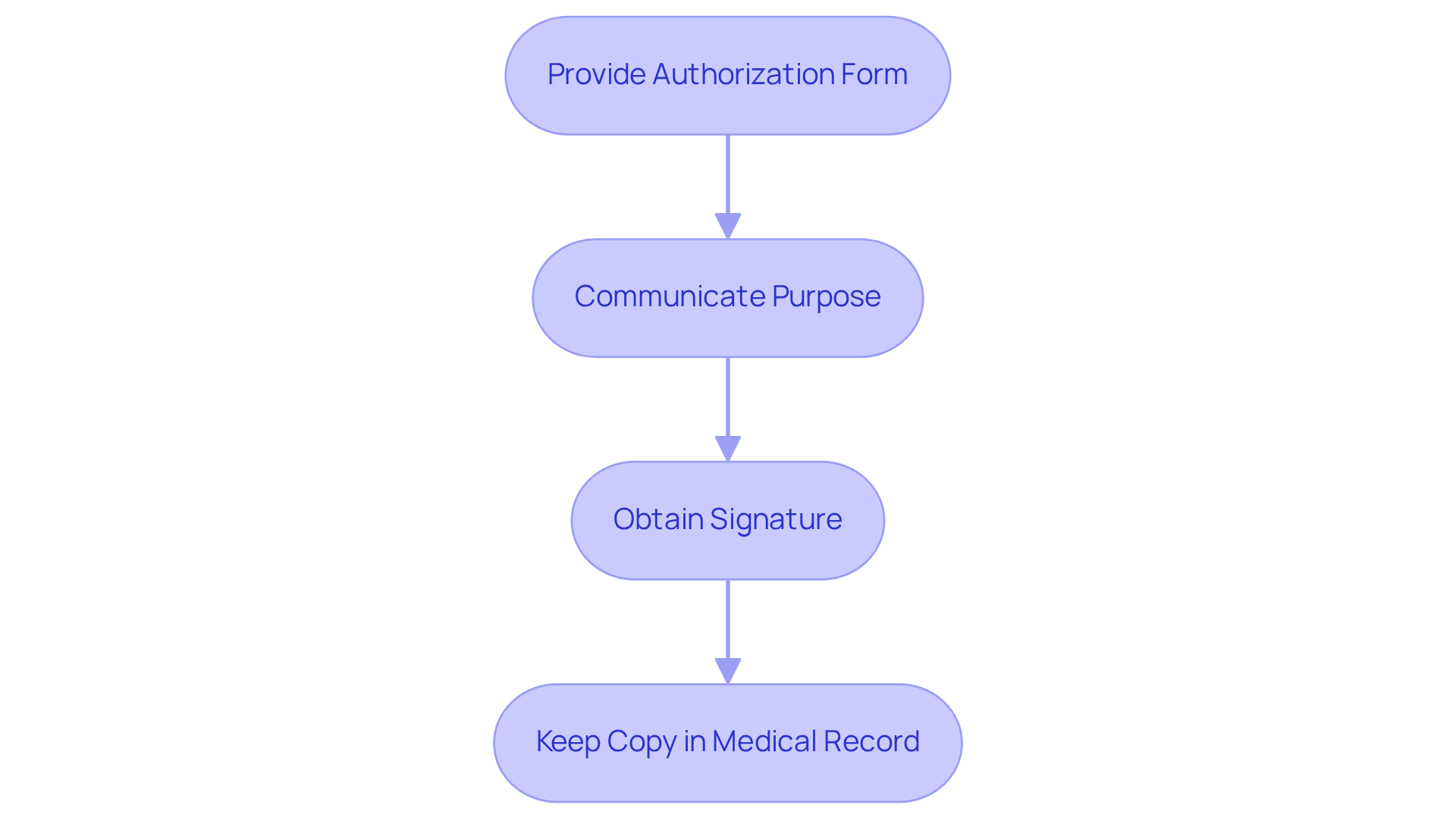
Clinics must implement best practices to ensure effective HIPAA authorization:
- Provide a clear and concise authorization form that specifies the information to be disclosed, ensuring it is written in plain language to enhance understanding.
- Clearly communicate the purpose of the disclosure to the individual, reinforcing how it relates to their care and treatment.
- Obtain the individual’s signature on the authorization form, confirming their consent for the specified disclosures.
- Keep a copy of the signed authorization in the individual’s medical record to ensure compliance and facilitate audits.
As of 2026, only 40% of individuals understand HIPAA authorization forms, highlighting the need for healthcare facilities to enhance communication strategies. Compliance specialists emphasize that simplifying the authorization process and providing ongoing education can significantly improve understanding and engagement among individuals. Implementing these practices will enhance compliance and strengthen patient trust.
Manage Revocation of HIPAA Authorization Effectively
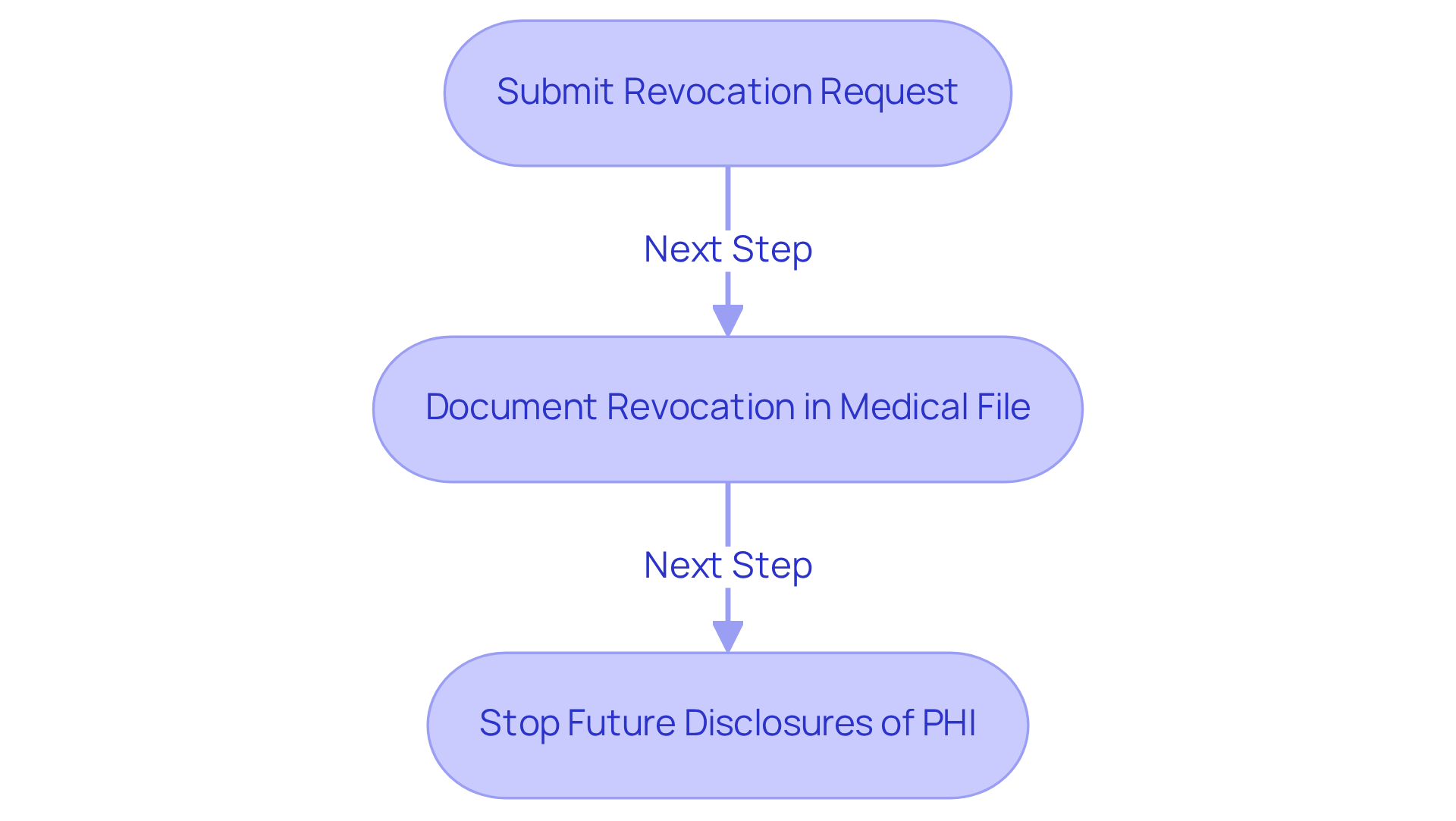
The ability to withdraw HIPAA authorization is a fundamental right that supports individual autonomy and privacy. Clinics must take specific steps to manage this process effectively:
- Offer individuals a straightforward and easy way to submit revocation requests, preferably in writing, to guarantee clarity and adherence.
- Record the revocation thoroughly in the individual’s medical file, as proper documentation is crucial for maintaining precise health records and ensuring adherence to HIPAA regulations.
- Stop any future disclosures of protected health information (PHI) immediately upon receiving a revocation request, ensuring privacy and adhering to legal obligations.
Many clinics struggle with proper documentation of revocation requests, which can lead to compliance issues. As healthcare regulation expert David Senter notes, “Proper documentation of revocation requests is essential for upholding standards and safeguarding individual rights.”
To enhance your compliance strategies, we recommend a 30-minute consultation with Healthcare Partners Consulting. We’ll map your current workflow and identify the services that will move the needle fastest for your practice. By addressing these documentation challenges, clinics can significantly enhance their compliance with HIPAA regulations. Enhancing documentation practices not only ensures compliance but also reinforces the trust between clinics and their clients.
Understand Waivers and Alterations of HIPAA Authorization
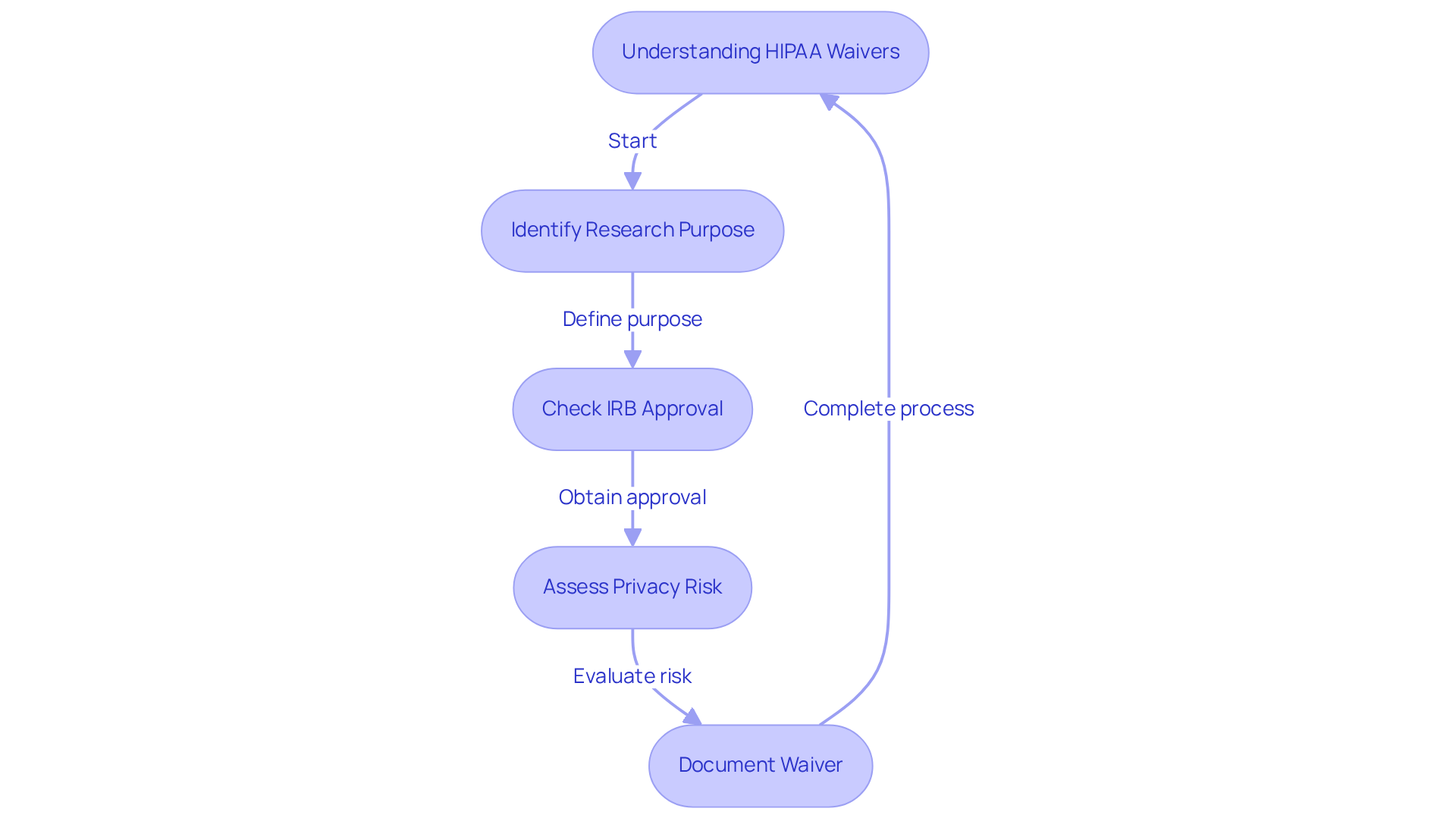
Understanding the conditions under which waivers or changes of authorization are permissible is crucial for healthcare facilities engaged in research. The law allows for such waivers, particularly in research settings, where an Institutional Review Board (IRB) can grant these waivers for specific uses of Protected Health Information (PHI) without requiring patient authorization, as long as the research meets certain criteria. For instance, research that poses minimal privacy risk and cannot be conducted without access to PHI may qualify for a waiver. Adherence to these regulations is essential, and clinics must thoroughly document any waivers issued to ensure compliance with privacy standards.
Recent insights from research compliance specialists highlight the critical need for medical facilities to grasp the precise conditions that allow for waivers related to healthcare privacy regulations. As noted, “Authorization is not necessary if your activity aligns with one of these research exemptions.” This underscores the importance of understanding the specific circumstances under which waivers are permissible. Moreover, a notable portion of healthcare facilities, around 65% in 2026, reported being aware of waivers for research purposes, indicating a growing recognition of these essential compliance aspects.
Examples of healthcare facilities effectively utilizing HIPAA waivers demonstrate the practical implications of these regulations. For example, a mental health facility conducting a study on treatment outcomes was able to utilize existing patient records without individual authorizations, thanks to an IRB-approved waiver. This streamlined their research process while ensuring compliance with privacy regulations.
Ultimately, a thorough understanding of HIPAA waivers is not just beneficial; it is essential for maintaining compliance and protecting patient privacy.
Conclusion
The Health Insurance Portability and Accountability Act (HIPAA) is crucial for safeguarding patient privacy in healthcare, yet many clinics face challenges in compliance. These comprehensive guidelines are critical for clinics to effectively manage sensitive medical information while ensuring compliance with federal regulations. Throughout this article, we have highlighted key aspects of HIPAA compliance, including:
- The identification of protected health information (PHI)
- The necessity of obtaining patient authorization
- The importance of managing personally identifiable information (PII)
Each section underscored the need for clinics to adopt effective strategies and best practices to navigate these complexities, ensuring that patient data remains secure and that regulatory requirements are met.
Given the rising incidence of healthcare data breaches, healthcare providers must prioritize HIPAA compliance to mitigate risks. By investing in training and streamlined processes, clinics can protect patients while improving operational efficiency. Ultimately, prioritizing HIPAA compliance is not just a regulatory obligation; it is a fundamental step toward fostering patient trust and ensuring the integrity of healthcare operations.
Frequently Asked Questions
What is the Health Insurance Portability and Accountability Act (HIPAA)?
HIPAA is a federal law that establishes national standards for the protection of health information, mandating healthcare providers to implement safeguards to protect sensitive medical data and ensure patient privacy.
Why is HIPAA compliance important for healthcare facilities?
Compliance with HIPAA is essential for maintaining patient trust and avoiding serious legal issues, as it protects against unauthorized access to patient data and identity theft.
What recent trends have been observed regarding healthcare data breaches?
There has been a significant increase in healthcare data breaches, with reports indicating 63 breaches affecting 500 or more individuals in February 2026, highlighting the urgent need for compliance with privacy regulations.
Can you provide examples of financial consequences due to HIPAA violations?
Yes, a New York law firm faced a $200,000 fine for privacy regulation violations after a ransomware attack, and New York Presbyterian Hospital agreed to a $300,000 settlement for violations related to website pixel usage.
What are the implications of timely breach notifications under HIPAA?
Timely breach notifications are crucial to protect individuals from potential harm and reinforce the importance of strict regulatory compliance as emphasized by the HHS.
How does HIPAA enhance the quality of care in healthcare facilities?
HIPAA not only protects patient privacy but also ensures that sensitive information is handled appropriately, which can enhance the overall quality of care.
When does HIPAA apply to healthcare practices?
HIPAA applies to healthcare providers that qualify as ‘covered entities,’ which includes those conducting certain electronic transactions like billing and claims processing.
What challenges do clinics face in determining their status as covered entities?
Many clinics struggle with clarity regarding their status as covered entities under HIPAA, which can lead to compliance risks and operational inefficiencies.
How can Healthcare Partners Consulting assist healthcare facilities with HIPAA compliance?
Healthcare Partners Consulting offers tailored solutions and personalized consultations to help clinics enhance compliance, streamline operations, and improve claims processing and reimbursement solutions.
What constitutes Protected Health Information (PHI)?
PHI includes medical records, billing information, and any data related to an individual’s health status, which clinics must safeguard to comply with HIPAA regulations.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting