Mastering Medical Coding
What’s a CPT Code? Understanding Its Role in Mental Health Billing

Introduction
CPT codes are essential for effective communication in mental health billing, ensuring accurate service identification and fair compensation. Understanding these codes allows mental health practitioners to effectively navigate billing complexities and secure fair compensation for their services. As new classifications emerge in healthcare, providers must adapt to avoid the pitfalls of inaccurate coding, which can jeopardize their financial stability.
Define CPT Codes: Understanding Their Role in Healthcare
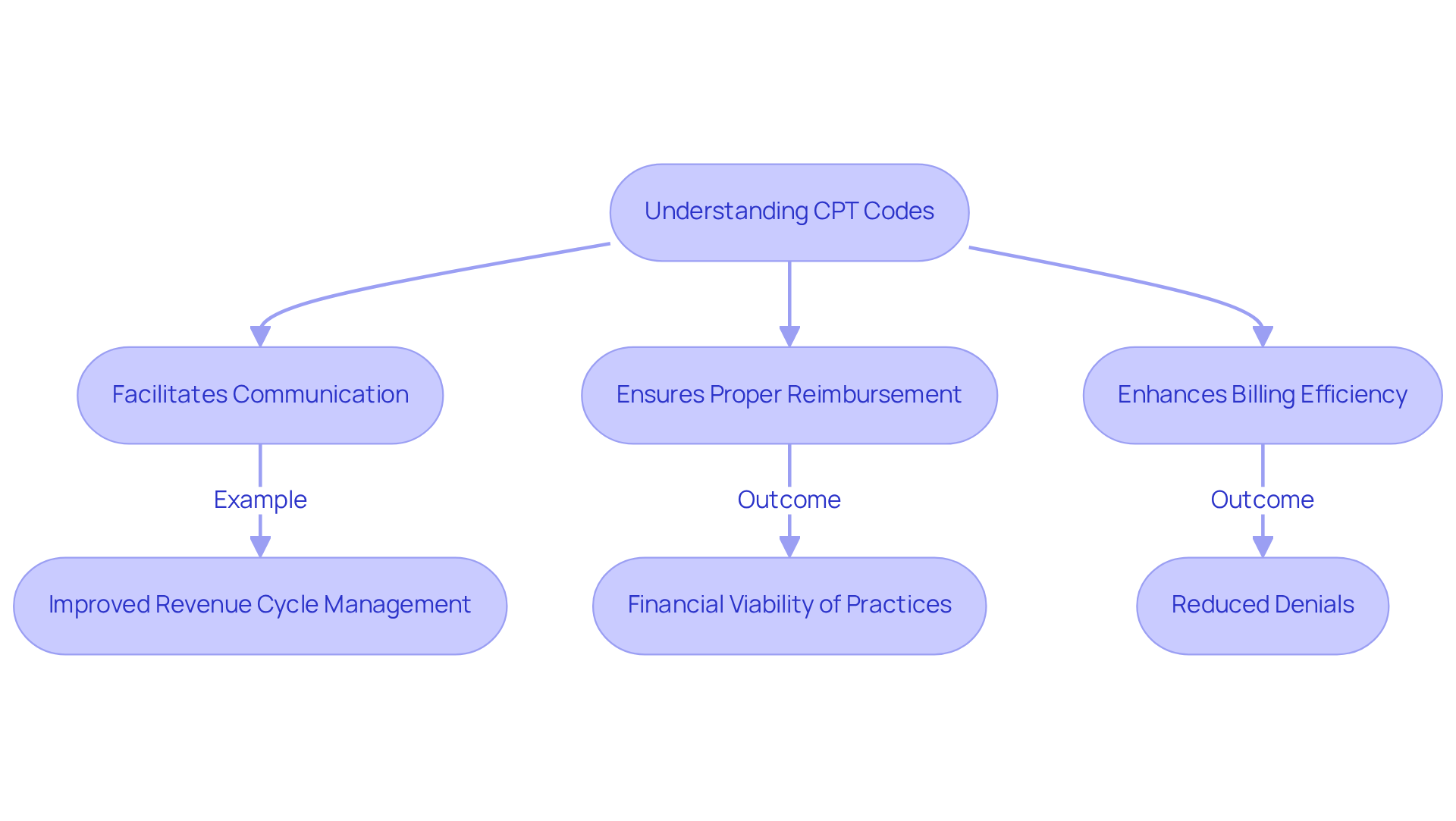
CPT numbers are critical identifiers in the healthcare system, serving as a bridge between providers and insurers. These identifiers create a universal language among healthcare providers, insurers, and patients. This facilitates clear communication about the services rendered. For instance, a particular CPT designation may signify a psychotherapy session, allowing mental health experts to bill precisely for their services.
The significance of CPT classifications extends beyond simple identification of services; they are essential for guaranteeing suitable reimbursement rates for healthcare providers. Practices that effectively utilize CPT numbers can significantly enhance their billing efficiency. For instance, a multi-specialty clinic improved its revenue cycle management by optimizing compliance and reducing denials, resulting in a savings of $500,000 in one year. This illustrates the direct impact that accurate coding has on financial outcomes for healthcare practices.
Furthermore, the growing intricacy of CPT classifications, especially with the addition of new entries in 2026, highlights the importance for psychological care providers to remain updated. Navigating the complexities of CPT classifications can pose significant challenges for healthcare providers. These updates not only reflect advancements in medical practices but also impact reimbursement rates and billing efficiency. Failure to adapt to these changes may result in decreased reimbursement rates and operational inefficiencies. As healthcare evolves, knowing what’s a CPT code becomes even more critical in navigating the complexities of insurance claims and ensuring that providers receive fair compensation for their services.
Healthcare Partners Consulting offers a vital credentialing toolkit designed for mental wellness providers. This toolkit simplifies administrative processes for therapists and behavioral care groups by providing features such as streamlined credentialing, compliance tracking, and billing support. By enabling practices to manage the intricacies of CPT classifications and billing, the toolkit ultimately improves their operational efficiency and financial stability.
Ultimately, the effective use of CPT numbers can determine the financial viability of psychological practices in an evolving healthcare landscape.
Trace the History: Evolution of CPT Codes Over Time
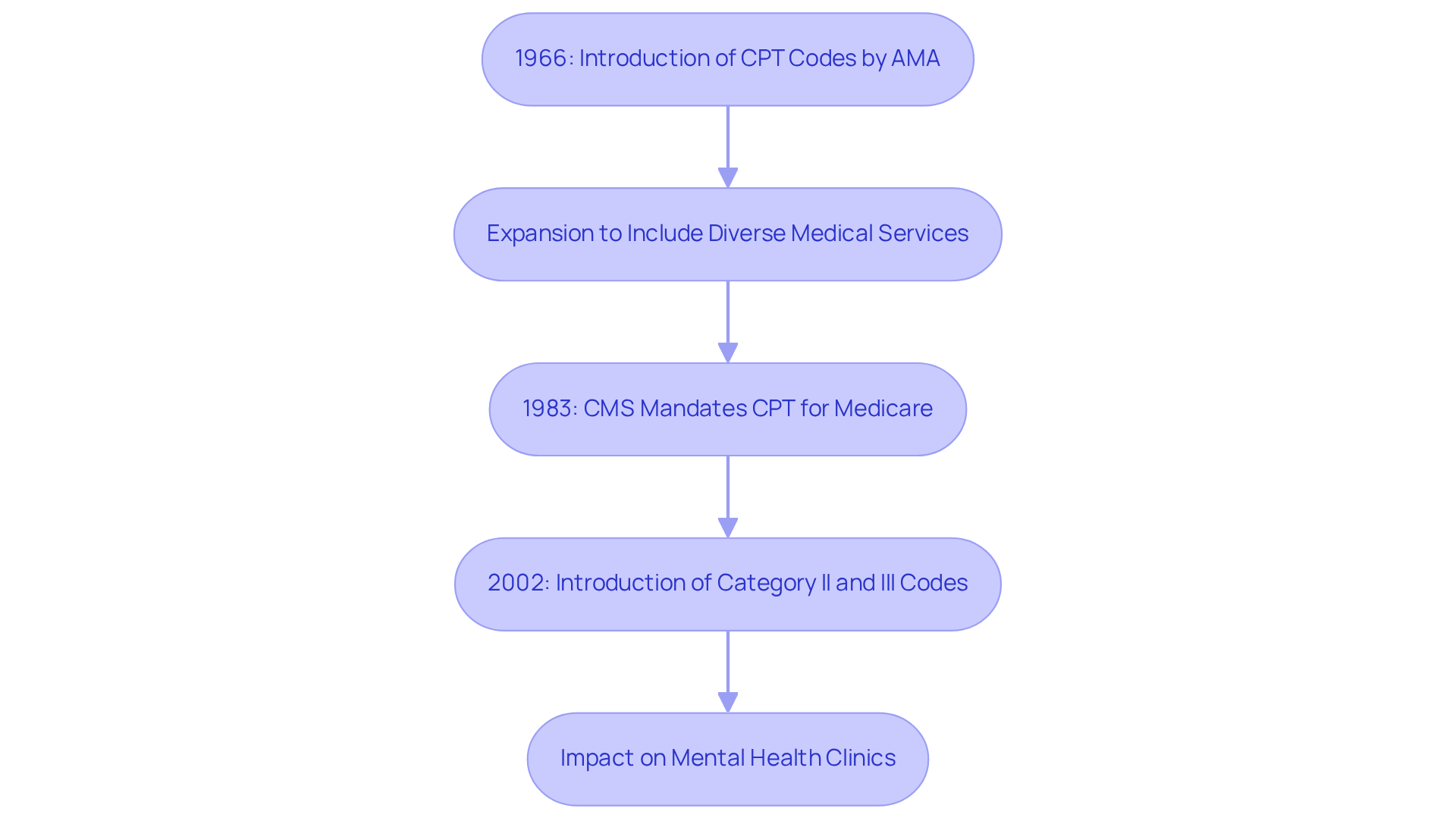
The evolution of Current Procedural Terminology (CPT) classifications reveals a complex interplay between standardization and the growing demands of diverse medical services. The history of CPT classifications began in 1966 when the American Medical Association (AMA) introduced them to standardize the reporting of medical services. Initially, the focus was primarily on surgical procedures; however, the CPT classification has significantly expanded over the decades to include a wide range of medical services, particularly in mental health treatments.
In 1983, a significant shift took place when the Centers for Medicare & Medicaid Services (CMS) required the use of CPT designations for Medicare service reporting. This mandate not only underscored the importance of CPT designations in healthcare billing but also fostered a more consistent labeling method across various medical fields. The ongoing updates to the CPT classification reflect advancements in medical technology and evolving healthcare practices, ensuring that the coding system remains relevant and effective in supporting accurate billing and reimbursement. Notably, the introduction of Category II and Category III CPT classifications in 2002 further enhanced the assessment of healthcare performance and the adoption of innovative medical practices, illustrating the continuous evolution of this essential system.
In the context of mental health clinics, effective administration of CPT classifications is crucial for enhancing revenue cycle management. Ensuring accurate coding and timely submission is essential for clinics to enhance cash flow, minimize write-offs, and achieve greater financial visibility. Specific strategies such as:
- Analyzing aging claims
- Contacting payers for clarification on payment status
- Submitting appeals for denials or underpayments
- Following up on patient balances
are vital. Regular follow-up on claims and detailed reporting can help identify trends and optimize collections, allowing clinic owners to focus more on patient care rather than administrative burdens. Ultimately, understanding what’s a CPT code not only enhances financial performance but also empowers clinics to prioritize patient care.
Explore CPT Code Categories: Types and Their Applications
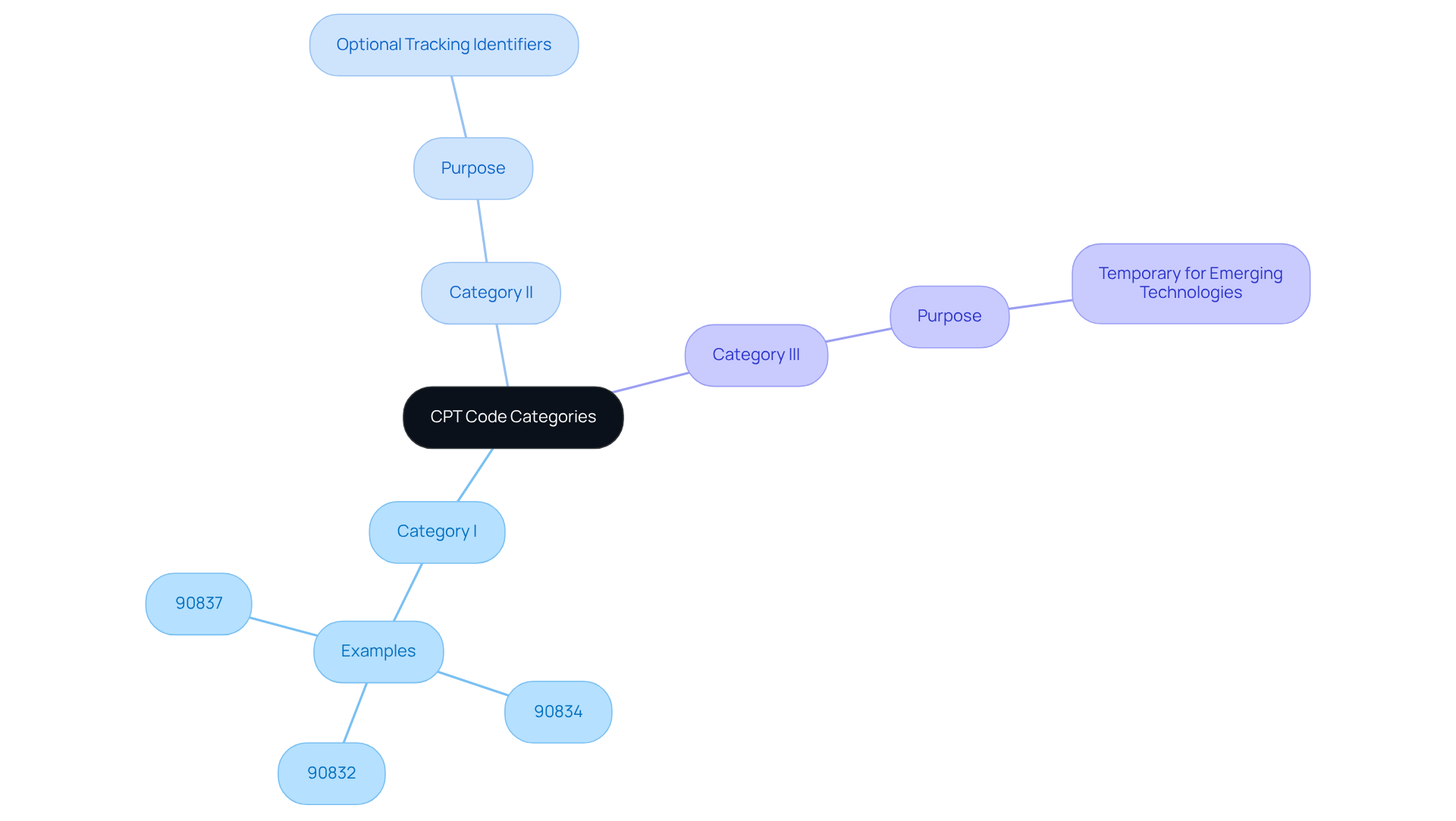
CPT designations play a pivotal role in the billing processes of psychological services, categorized into three main groups:
- Category I
- Category II
- Category III
Category I classifications are the most commonly used, depicting established medical procedures and services, including psychotherapy sessions. For example, numbers 90832, 90834, and 90837 are assigned for personal therapy, reflecting the standard practices in psychological care.
Category II designations function as optional tracking identifiers, mainly focused on performance evaluation, whereas Category III designations are temporary and relate to emerging technologies and procedures.
For psychological service providers, understanding these classifications is essential for selecting appropriate billing identifiers and ensuring compliance with regulations. The efficient use of Category I classifications in psychological practices not only enables precise billing but also aids in delivering effective care.
Healthcare Partners Consulting offers a toolkit designed for wellness providers to streamline credentialing and administrative tasks. This toolkit, along with our comprehensive FAQs, provides valuable insights into our services and enhances your practice’s operational efficiency.
Understand the Importance: CPT Codes in Medical Billing and Coding
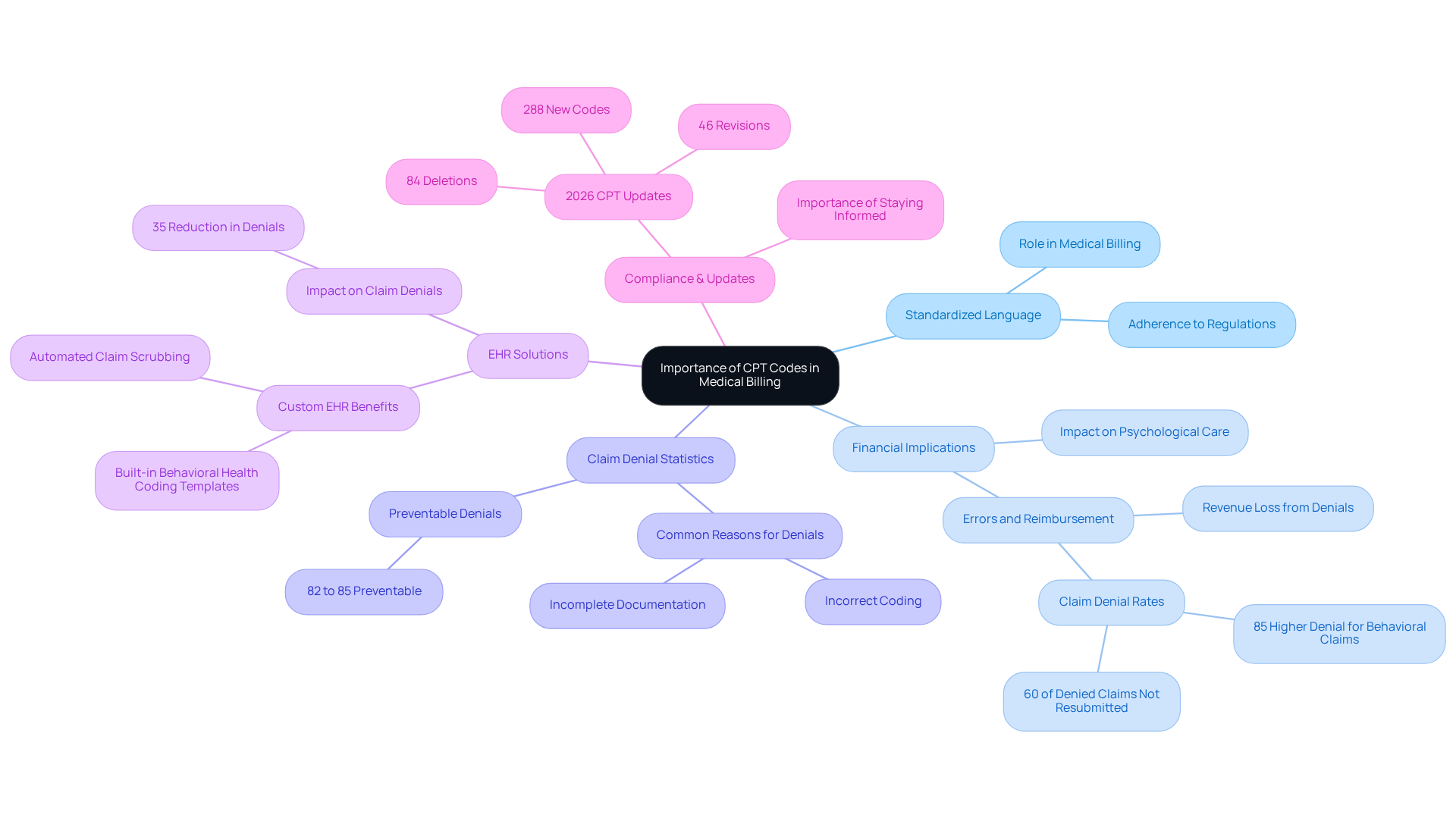
CPT designations serve as a standardized language in medical billing, yet their accurate application is often overlooked, leading to significant financial implications for healthcare providers. Accurate coding is essential for timely reimbursement; errors can result in claim denials or payment delays. In psychological care practices, the proper application of CPT numbers not only ensures adherence to regulations but also greatly influences financial viability.
For instance, behavioral wellness claims are denied 85% more frequently than general medical claims, underscoring the importance of precise coding. Studies indicate that 60% of denied claims are never resubmitted, resulting in substantial revenue loss. By accurately applying CPT classifications, mental wellness providers can streamline billing procedures and reduce administrative burdens, allowing for greater focus on patient care.
Clinics using customized EHR solutions with integrated behavioral coding templates report a 35% reduction in claim denials, illustrating the direct relationship between precise coding and improved financial outcomes. As the 2026 CPT update introduces 288 new codes, 84 deletions, and 46 revisions, staying informed about these changes is crucial for maintaining compliance and optimizing revenue.
At Healthcare Partners Consulting, our expert team specializes in psychological and behavioral billing, ensuring that your practice benefits from customized coding support and comprehensive revenue cycle management. Inaccurate coding can jeopardize the financial health of mental health practices, making it imperative to prioritize compliance and accuracy in billing processes.
Conclusion
Navigating the complexities of mental health billing hinges on a thorough understanding of CPT codes. These codes serve as a standardized language that facilitates communication between healthcare providers, insurers, and patients, ensuring that mental health services are accurately identified and billed. The effective use of CPT codes streamlines the billing process and significantly impacts the financial sustainability of psychological practices.
Throughout the article, key insights were discussed, including:
- The historical evolution of CPT codes
- Their categorization
- The critical role they play in ensuring timely reimbursements
The importance of accurately applying these codes cannot be overstated, as errors in coding can disrupt the billing process, leading to significant financial repercussions for practices. Staying informed about CPT updates and employing effective coding strategies enhances revenue cycle management, allowing healthcare providers to concentrate on patient care.
In conclusion, the significance of CPT codes in mental health billing extends beyond mere compliance; they are vital for the financial health of practices. As the healthcare landscape continues to evolve, mental health providers must prioritize understanding and effectively utilizing these codes to ensure fair compensation for their services. Mastering CPT coding is crucial for ensuring financial viability and delivering quality patient care in a competitive landscape.
Frequently Asked Questions
What are CPT codes and why are they important in healthcare?
CPT codes are critical identifiers in the healthcare system that serve as a universal language among providers, insurers, and patients. They facilitate clear communication about the services rendered and are essential for ensuring appropriate reimbursement rates for healthcare providers.
How do CPT codes impact billing efficiency for healthcare practices?
Practices that effectively utilize CPT codes can enhance their billing efficiency, leading to improved revenue cycle management. For example, a multi-specialty clinic optimized compliance and reduced denials, resulting in a savings of $500,000 in one year.
What challenges do healthcare providers face regarding CPT classifications?
Healthcare providers face challenges in navigating the complexities of CPT classifications, especially with the introduction of new entries in 2026. Staying updated is crucial, as failure to adapt may lead to decreased reimbursement rates and operational inefficiencies.
What is the role of Healthcare Partners Consulting in relation to CPT codes?
Healthcare Partners Consulting offers a credentialing toolkit designed for mental wellness providers, which simplifies administrative processes. This toolkit includes features like streamlined credentialing, compliance tracking, and billing support, helping practices manage the intricacies of CPT classifications and improve operational efficiency.
Why is it critical for psychological care providers to stay informed about CPT codes?
As healthcare evolves, understanding CPT codes becomes increasingly important for navigating insurance claims and ensuring that providers receive fair compensation for their services. Accurate coding directly impacts financial outcomes for healthcare practices.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting