Mastering Medical Coding
Master Speech Therapy Modifier Codes for Accurate Billing Success

Introduction
Understanding the complexities of speech therapy billing is essential, particularly regarding the pivotal role of modifier codes. These codes serve not merely as bureaucratic requirements; they are vital instruments that facilitate accurate claims processing and adherence to payer standards. The challenge, however, lies in mastering their application. A failure to do so can result in substantial revenue loss and increased administrative burdens. Thus, how can speech therapists effectively navigate this intricate landscape to optimize their billing practices and improve reimbursement outcomes?
Understand the Role of Modifier Codes in Speech Therapy Billing
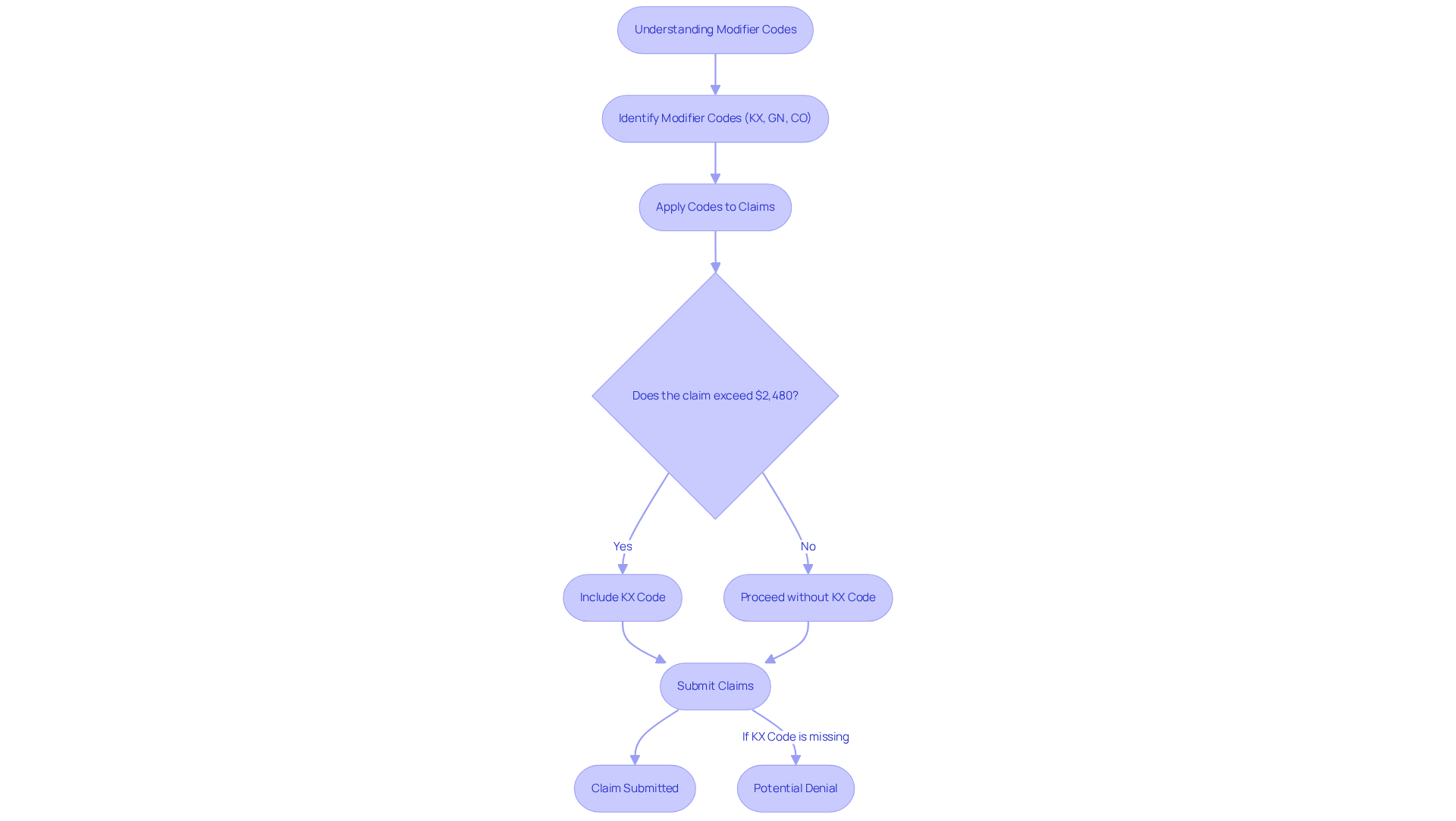
Speech therapy modifier codes are essential in invoicing for speech treatment, as they provide critical details about the services rendered, facilitating accurate claims processing. These codes are crucial for differentiating between similar services and indicating specific circumstances that may affect billing outcomes. For instance, the KX code is vital for confirming medical necessity when therapy costs exceed the annual threshold of $2,480 for combined Speech-Language Pathology and Physical Therapy services in 2026. Omitting this adjustment can lead to outright denials of requests, as Medicare requires it for submissions that surpass the threshold.
The impact of adjustment codes on denial rates is significant; requests that lack the appropriate adjustments can face denial rates of 10-15%, resulting in lost revenue and increased administrative burdens. Understanding and utilizing speech therapy modifier codes such as KX, GN, and CO is imperative for speech therapists, as these speech therapy modifier codes not only ensure compliance with payer standards but also enhance the likelihood of timely reimbursements. Moreover, if a patient’s combined treatment expenses exceed $3,000 within a calendar year, the request may be subject to further scrutiny.
By mastering the application of these adjustments, speech practices can improve their financial health and reduce the likelihood of request denials. Additionally, collaborating with Healthcare Partners Consulting can offer comprehensive accounts receivable management solutions that enhance revenue cycle efficiency. Their proactive follow-up with payers on unpaid claims, appeal submissions for denied claims, and coordination of structured payment plans can significantly alleviate administrative burdens, enabling clinics to concentrate more on patient care while ensuring improved cash flow and minimized denials.
Select and Apply Appropriate Modifier Codes for Accurate Billing
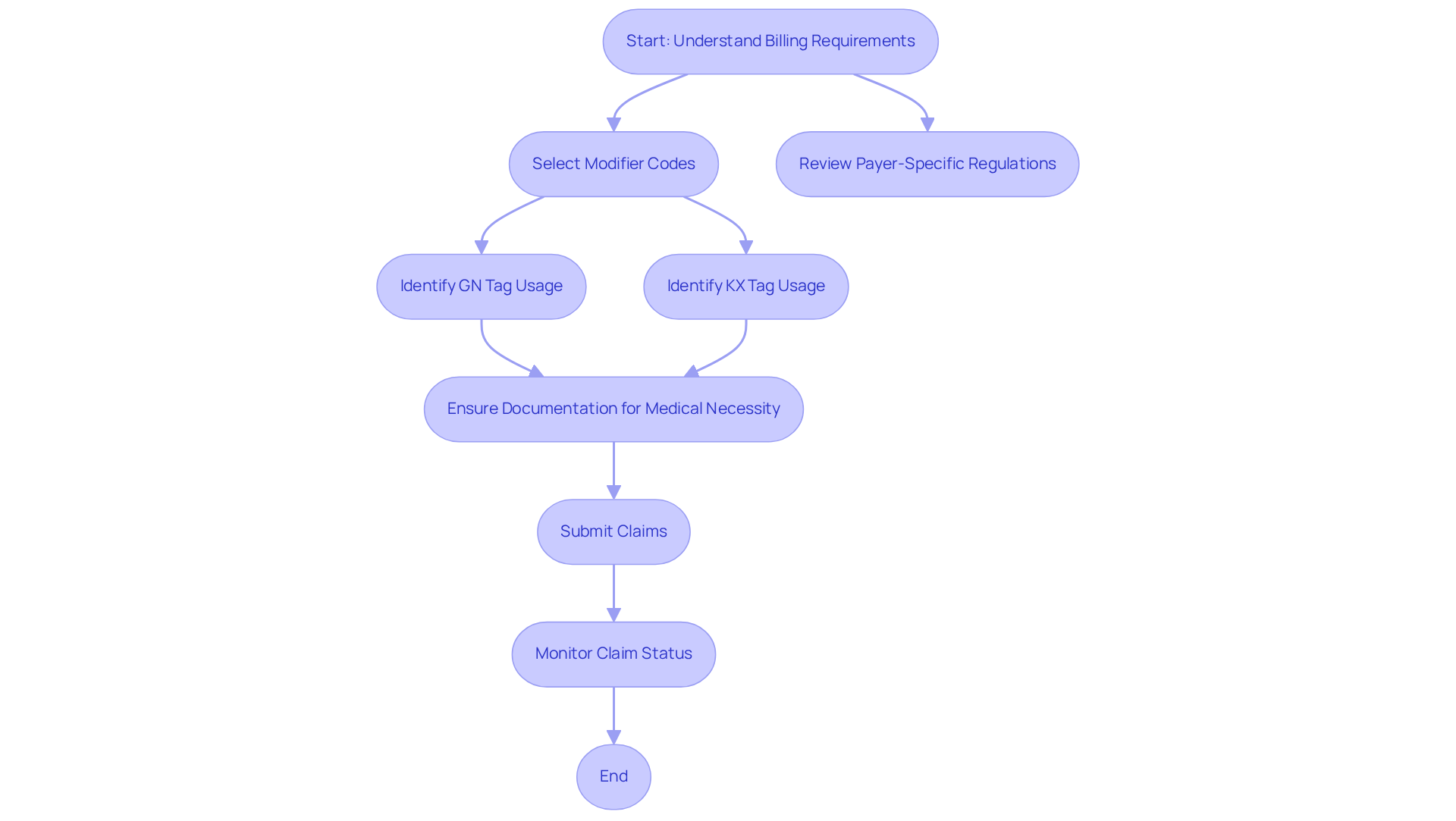
Precise invoicing in speech treatment hinges on the careful selection of speech therapy modifier codes that correspond with the services rendered. The GN tag is vital for denoting that the service was delivered under a speech-language pathology plan of care. In contrast, the KX tag becomes essential when therapy services exceed the annual threshold, thereby confirming medical necessity. Given that the incorrect application of adjustments is a leading cause of invoicing errors, it is imperative to familiarize oneself with payer-specific regulations.
Insurers often impose distinct criteria for the use of adjustments. Regular training sessions and updates on coding techniques are crucial for therapists, enabling them to remain informed about changes in payment codes and adjustments. This proactive approach significantly diminishes the risk of claim denials and ensures compliance with healthcare regulations.
Maintain Comprehensive Documentation to Support Modifier Usage
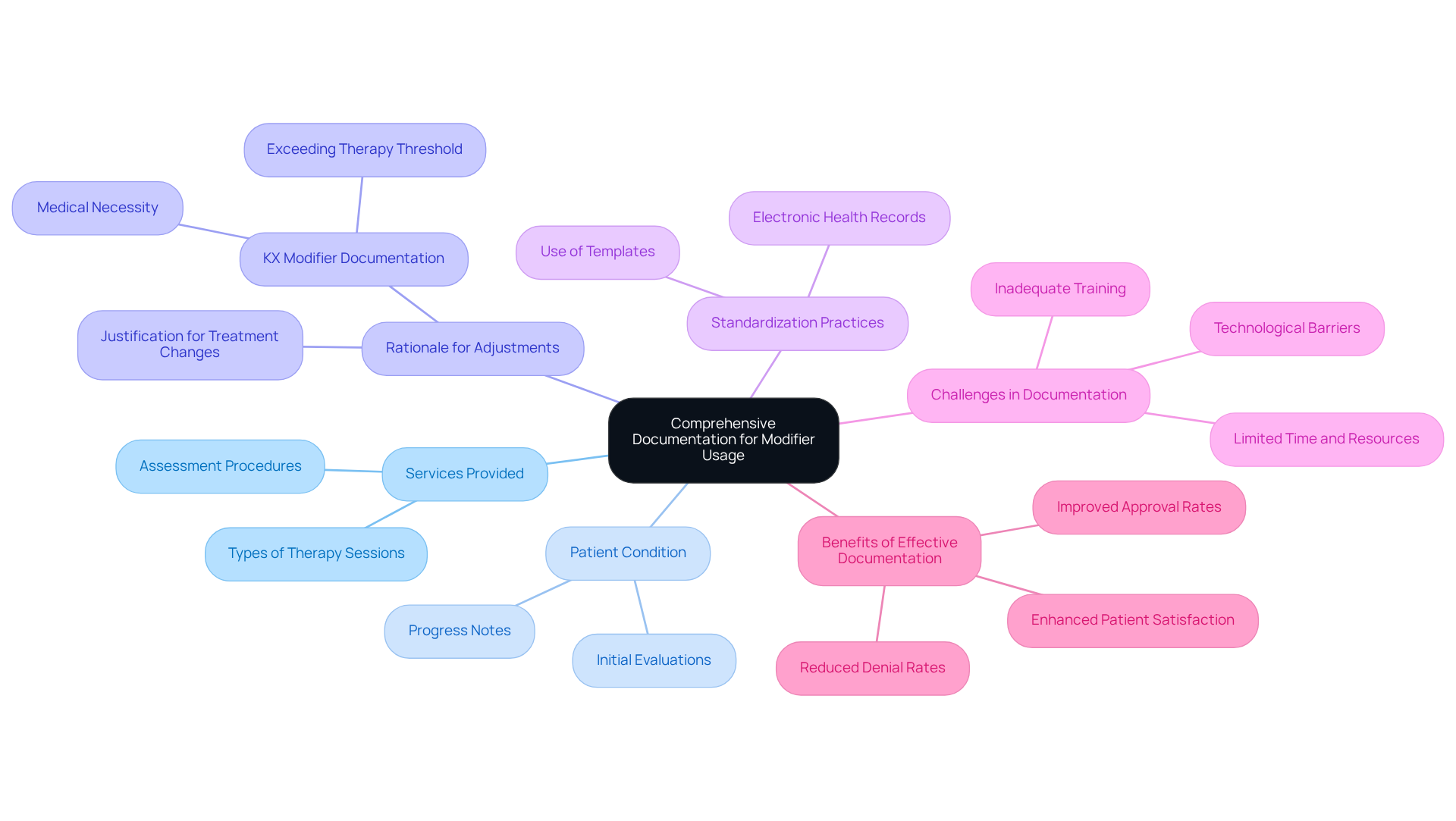
Thorough documentation is essential for the effective use of speech therapy modifier codes in speech treatment billing. Each treatment session must be meticulously recorded, capturing critical details such as:
- The services provided
- The patient’s condition
- The rationale for specific adjustments
For example, when applying the KX modifier, it is vital to document the medical necessity for exceeding the therapy threshold. This careful record-keeping not only supports claims but also safeguards against audits and potential penalties.
Standardizing documentation practices, such as utilizing templates or electronic health records, can streamline this process, ensuring that all relevant information is accurately captured. By prioritizing thorough documentation, therapists can enhance approval rates and maintain compliance with healthcare regulations. Moreover, leveraging Healthcare Partners Consulting’s medical billing solutions can significantly reduce denial rates by 20-30% and improve reimbursement timelines by 15-25%, ultimately boosting patient satisfaction and optimizing revenue cycle management.
Identify and Overcome Common Challenges in Modifier Code Application
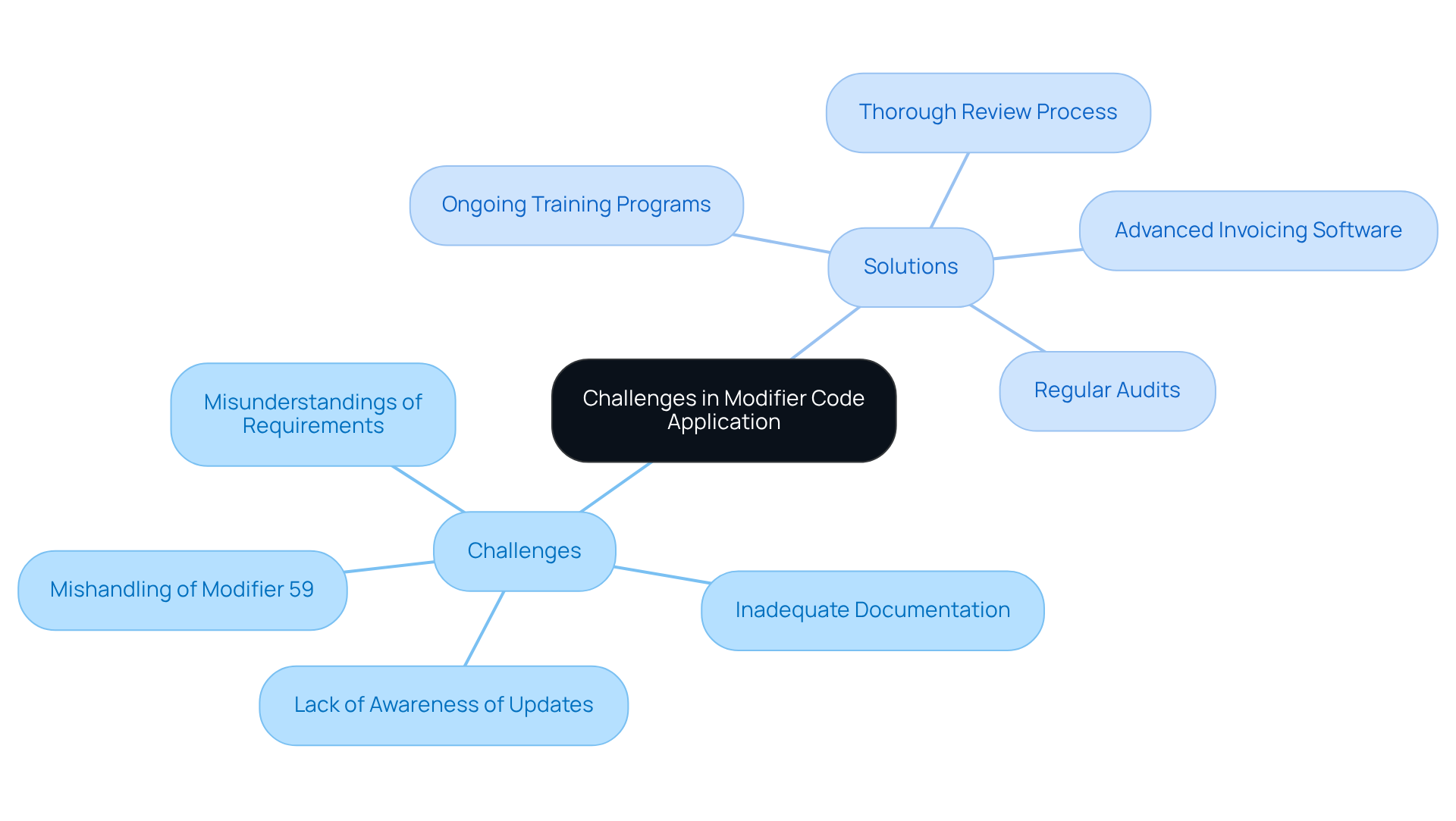
The challenges in applying speech therapy modifier codes are significant, primarily stemming from misunderstandings of specific requirements, inadequate documentation, and a lack of awareness regarding updates in coding guidelines. A common issue is the mishandling of Modifier 59, which often leads to an increase in denied requests.
To effectively address these challenges, it is essential to implement ongoing training programs for staff that emphasize coding practices and the nuances of speech therapy modifier codes usage. Furthermore, establishing a thorough review process for claims prior to submission can significantly reduce errors.
Employing advanced invoicing software that flags potential coding mistakes serves as another effective strategy to mitigate these challenges. Regular audits of billing practices can help identify persistent issues, enabling clinics to refine their processes and enhance overall billing accuracy.
Statistics indicate that approximately 68% of providers find submitting clean claims more challenging than in previous years. This underscores the necessity for proactive measures in training and documentation to improve success rates in claims processing.
Conclusion
Mastering speech therapy modifier codes is not merely a technical requirement; it is essential for ensuring accurate billing and maximizing reimbursement success. By comprehensively understanding and correctly applying these codes, speech therapists can effectively navigate the complexities of the billing process, ultimately enhancing the financial health of their practices.
This article underscores the significance of modifier codes such as KX, GN, and CO, which provide critical information about the services rendered and confirm medical necessity when required. Key strategies include:
- Maintaining thorough documentation
- Implementing ongoing training for staff
- Utilizing advanced invoicing software to minimize errors
Addressing common challenges such as misunderstandings regarding coding requirements and inadequate documentation is crucial for improving claims processing success rates.
Ultimately, prioritizing the mastery of speech therapy modifier codes and documentation practices not only enhances compliance and reduces denial rates but also fosters a more efficient revenue cycle. By embracing these best practices, speech therapy providers can concentrate more on patient care while ensuring their financial stability and operational efficiency in an increasingly complex healthcare landscape.
Frequently Asked Questions
What are speech therapy modifier codes?
Speech therapy modifier codes are essential codes used in invoicing for speech treatment that provide critical details about the services rendered, facilitating accurate claims processing.
Why are modifier codes important in speech therapy billing?
Modifier codes are important because they differentiate between similar services and indicate specific circumstances that may affect billing outcomes, ensuring compliance with payer standards and enhancing the likelihood of timely reimbursements.
What is the KX code and why is it significant?
The KX code is used to confirm medical necessity when therapy costs exceed the annual threshold of $2,480 for combined Speech-Language Pathology and Physical Therapy services in 2026. Omitting this code can lead to denials of claims as Medicare requires it for submissions that surpass this threshold.
What are the potential consequences of not using the appropriate modifier codes?
Not using the appropriate modifier codes can result in denial rates of 10-15%, leading to lost revenue and increased administrative burdens for speech therapy practices.
What other modifier codes should speech therapists be aware of?
Besides the KX code, speech therapists should also be aware of the GN and CO modifier codes, as they are crucial for compliance and successful billing.
What happens if a patient’s combined treatment expenses exceed $3,000 within a calendar year?
If a patient’s combined treatment expenses exceed $3,000 within a calendar year, the request may be subject to further scrutiny, potentially affecting the claims process.
How can speech practices improve their financial health regarding billing?
Speech practices can improve their financial health by mastering the application of modifier codes, which can reduce the likelihood of request denials.
What services does Healthcare Partners Consulting provide to assist with billing?
Healthcare Partners Consulting offers accounts receivable management solutions, including proactive follow-up with payers on unpaid claims, appeal submissions for denied claims, and coordination of structured payment plans, which can alleviate administrative burdens and improve cash flow.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting