Revenue Cycle Management Best Practices
10 Steps of the Revenue Cycle vs. Traditional Billing Practices

Introduction
As the healthcare landscape evolves, organizations must adapt their financial management strategies to remain viable. Revenue Cycle Management (RCM) provides a structured approach that not only streamlines billing but also enhances overall financial health, contrasting sharply with traditional billing practices that often lead to inefficiencies and delayed payments. Healthcare providers face significant challenges in navigating reimbursement complexities and ensuring patient care.
Can adopting RCM effectively address the challenges of financial sustainability and operational efficiency, or do traditional methods still have merit?
Define Revenue Cycle Management and Traditional Billing Practices
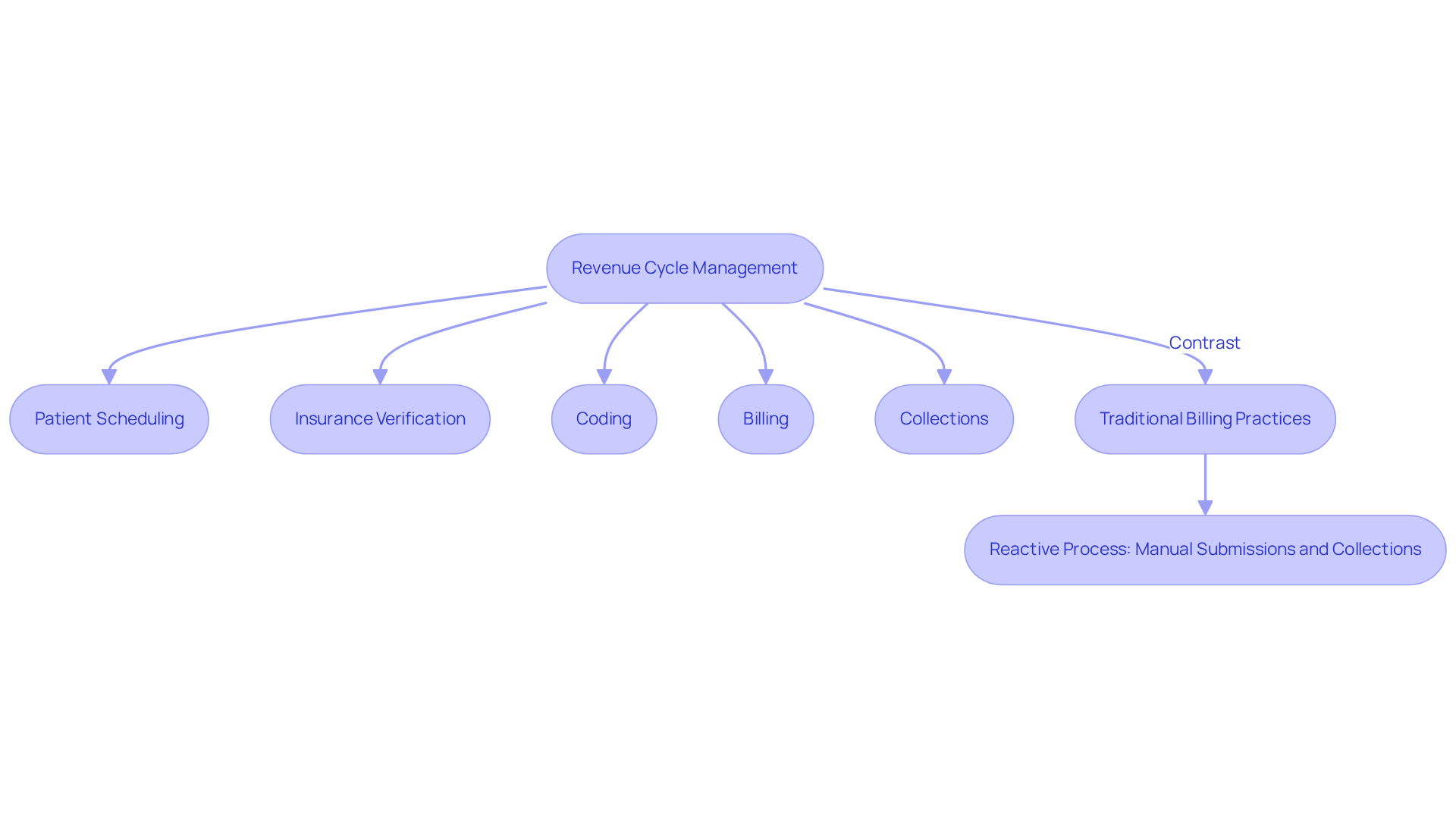
Revenue Cycle Management (RCM) serves as a vital framework for healthcare organizations, guiding them through the complexities of patient care episodes from registration to final payment. This process encompasses critical stages such as:
- Patient scheduling
- Insurance verification
- Coding
- Billing
- Collections
RCM aims to enhance healthcare providers’ financial performance. It does so by ensuring timely and accurate reimbursements while minimizing errors and denials.
Healthcare Partners Consulting provides accounts receivable management solutions that optimize RCM processes, leading to faster payments and less staffing burden. Their proactive follow-up with payers on unpaid or underpaid requests, along with appeal submissions for denied requests, significantly enhances revenue cycle efficiency. Additionally, features such as structured payment plans coordination and monthly reconciliation and AR trending analysis further support providers in maintaining financial health.
In contrast, traditional billing practices mainly focus on submitting requests and collecting payments after services have been provided. This approach often depends on manual processes, like paper billing and direct communication with insurers, leading to inefficiencies and added administrative burdens. Unlike RCM, traditional billing lacks proactive measures, rendering it reactive rather than strategic in managing revenue flow. Consequently, healthcare providers may encounter difficulties such as delayed payments and increased rejection rates.
Adopting a proactive revenue management strategy is essential for healthcare providers to navigate the challenges of delayed payments and rejection rates effectively.
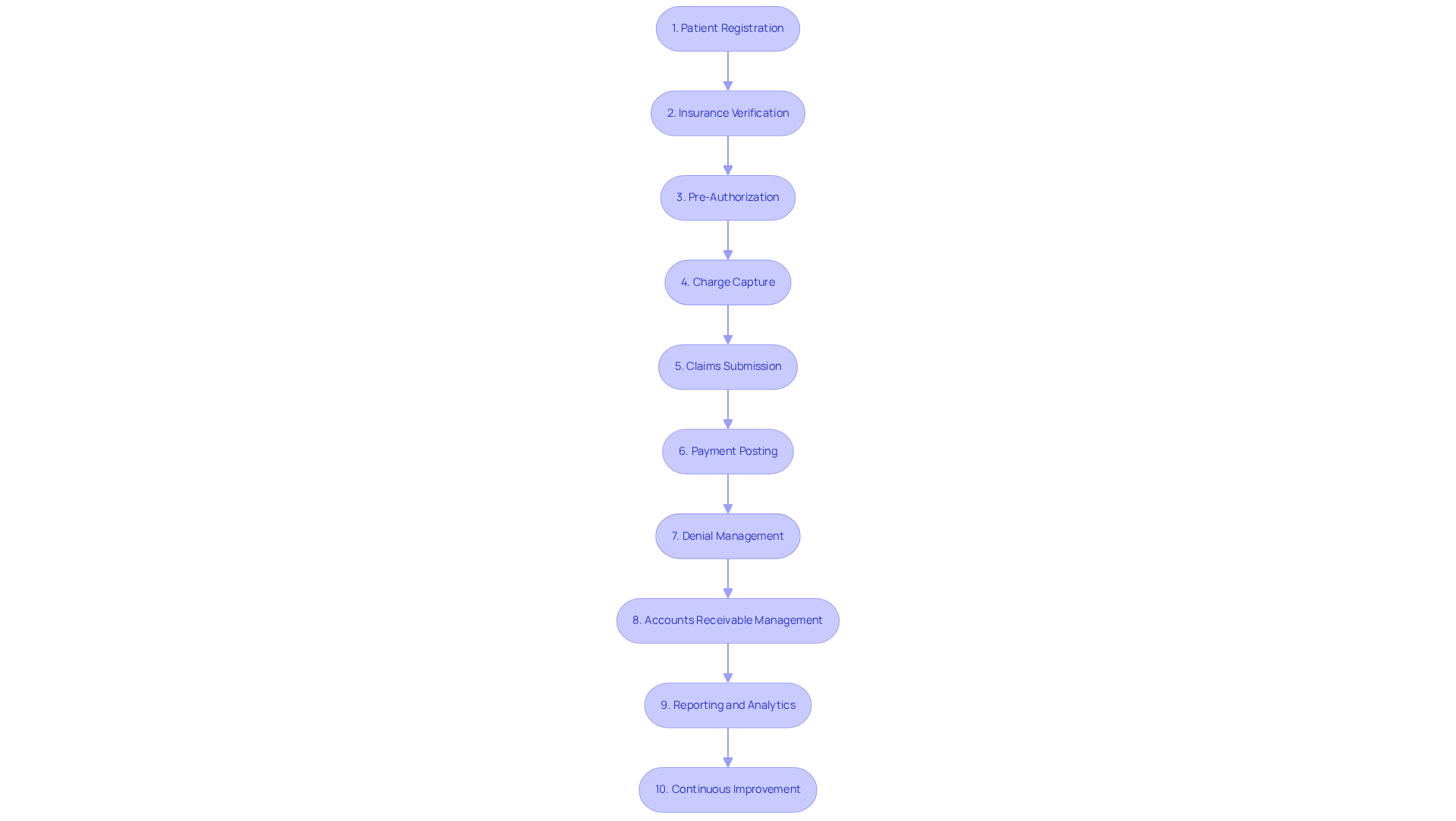
Outline the 10 Steps of Revenue Cycle Management
- Patient Registration: This initial step is crucial as it collects essential patient information and insurance details. It sets the foundation for accurate records and smooth coordination between staff and clinicians. Efficient enrollment methods can greatly minimize mistakes. These mistakes account for up to 35% of request refusals, costing healthcare institutions millions each year.
- Insurance Verification: Confirming patient eligibility and benefits with insurance providers is vital for preventing revenue leakage. In 2026, the average time taken for insurance verification is expected to be streamlined through automation. This will reduce the verification process to under five minutes in many clinics. Best practices include real-time validation and pre-visit benefit summaries to ensure that coverage is active and understood before services are rendered.
- Pre-Authorization: Securing required approvals for particular services prior to their provision aids in reducing the likelihood of reimbursement rejections. Organizations are increasingly adopting clinical decision support tools to streamline this process, which is expected to improve efficiency significantly.
- Charge Capture: Accurately documenting services provided ensures correct billing and maximizes revenue. This step is essential for maintaining compliance and optimizing reimbursement rates.
- Claims Submission: Sending claims to insurance companies for reimbursement is a critical phase where accuracy is paramount. Errors in this step can lead to delays and denials, emphasizing the need for meticulous attention to detail.
- Payment Posting: Recording payments received from insurers and patients is essential for maintaining accurate financial records. This step allows practices to track revenue flow effectively.
- Denial Management: Addressing and resolving any claims that are denied by insurers is crucial for maintaining cash flow. Proactive refusal management strategies can decrease refusal rates significantly. Organizations are encouraged to implement automated tools for tracking and resolving disputes.
- Accounts Receivable Management: Monitoring outstanding payments and following up on overdue accounts ensures that organizations maintain financial health. Effective management of accounts receivable can enhance cash flow and reduce the time it takes to collect payments. HPC’s proactive follow-up and dedicated AR specialists ensure faster payments and a significant reduction in days in accounts receivable.
- Reporting and Analytics: Analyzing financial data to identify trends and areas for improvement is vital for strategic decision-making. Organizations are encouraged to establish baselines for key metrics such as denial trends and aging accounts receivable to inform their revenue cycle strategies. Supported by HPC’s detailed monthly AR reports that provide insights and recommendations.
- Continuous Improvement: Implementing strategies to enhance the revenue cycle process based on performance metrics is essential for long-term sustainability. Regular audits and staff training are essential for adapting to the evolving challenges in healthcare. Leveraging HPC’s comprehensive management services can optimize patient revenue activities.
These steps illustrate the proactive nature of RCM, emphasizing the importance of the 10 steps of the revenue cycle in ensuring financial sustainability for healthcare practices. By refining each phase of the revenue cycle, healthcare practices can secure their financial future and enhance patient care.
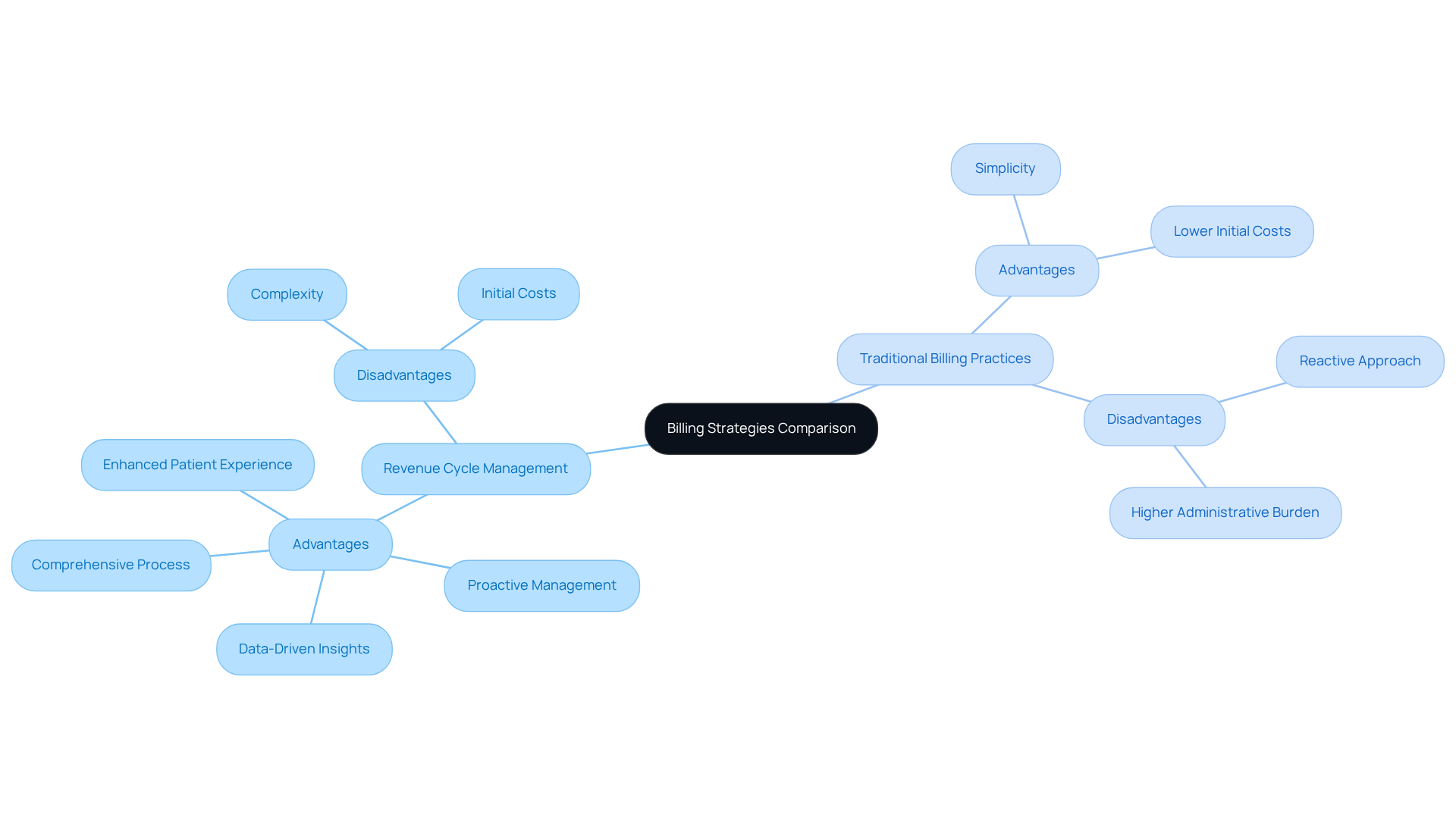
Compare Advantages and Disadvantages of Each Approach
When evaluating billing strategies, healthcare providers must weigh the advantages and disadvantages of Revenue Cycle Management against traditional billing practices.
Advantages of Revenue Cycle Management:
- Comprehensive Process: RCM encompasses all facets of the revenue cycle, ensuring thorough oversight. Healthcare Partners Consulting provides extensive accounts receivable management solutions that improve revenue cycle efficiency, ensuring that no request is overlooked.
- Proactive Management: By recognizing potential issues early, RCM helps alleviate cash flow disruptions. With Healthcare Partners Consulting’s proactive follow-up on unpaid or underpaid claims and appeal submission for denied claims, organizations can significantly lower their average claim denial rate, which is around 10-15% in 2026.
- Data-Driven Insights: RCM systems offer valuable analytics that enable organizations to make informed decisions. Monthly reconciliation and AR trending analysis from Healthcare Partners Consulting further support this data-driven approach.
- Enhanced Patient Experience: Streamlined billing processes lead to faster payments, significantly improving patient satisfaction. With dedicated AR specialists, structured payment plans, and timely patient statement generation, Healthcare Partners Consulting ensures that patients receive the support they need.
Disadvantages of Revenue Cycle Management:
- Complexity: For smaller practices, the complexity of RCM can feel overwhelming, which might create challenges during implementation.
- Initial Costs: The upfront investment required for RCM systems, including technology and training, can be substantial, posing a barrier for certain organizations.
Advantages of Traditional Billing Practices:
- Simplicity: Traditional billing methods are generally easier to understand and implement, making them more accessible for smaller practices with limited resources.
- Lower Initial Costs: These practices typically demand less investment in technology compared to RCM, making them financially appealing for smaller operations.
Disadvantages of Traditional Billing Practices:
- Reactive Approach: Traditional methods often result in delayed payments and increased claim denials due to a lack of proactive management strategies. This reactive strategy can significantly hinder cash flow, especially as claim denials increase in 2026.
- Higher Administrative Burden: When relying on manual billing, practices often face errors and inefficiencies that can hurt patient care and add to operational stress. Additionally, compliance with stricter regulations in 2026 necessitates accurate documentation, further complicating traditional billing methods.
This comparison emphasizes the need for healthcare providers to assess their operational capabilities and financial goals when choosing between RCM and traditional billing methods. Ultimately, the choice between RCM and traditional billing practices can profoundly impact a healthcare provider’s financial health and operational efficiency.
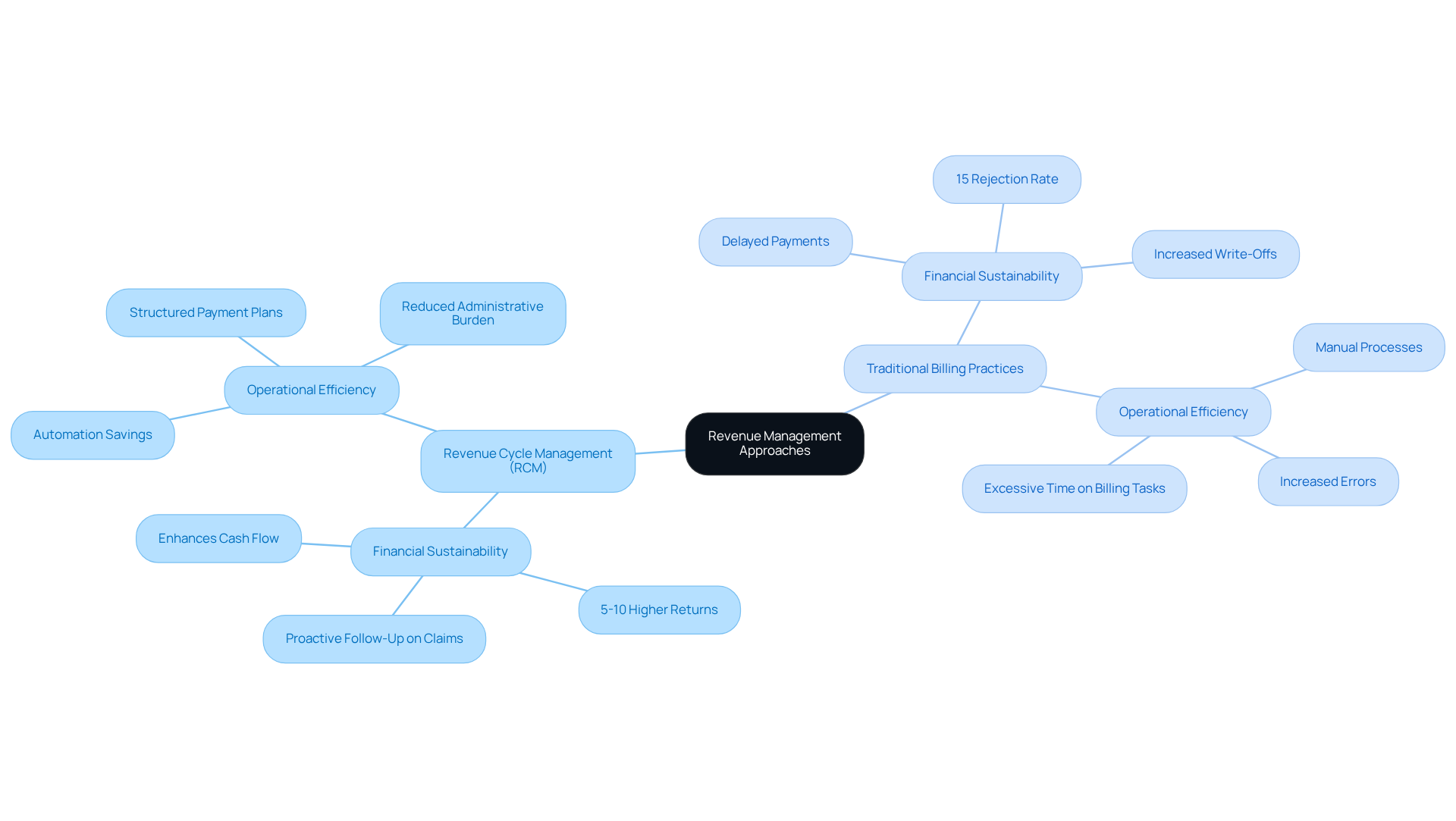
Evaluate Impact on Financial Sustainability and Operational Efficiency
Revenue Cycle Management:
- Financial Sustainability: RCM substantially enhances cash flow by shortening the interval between service delivery and payment collection. By efficiently reducing rejections and enhancing processing, practices can ensure a steady income flow, which is essential for long-term financial stability. Reports indicate that organizations leveraging advanced analytics achieve 5-10% higher returns on assets than their peers, underscoring the financial advantages of RCM. Proactive follow-up with payers on unpaid claims can significantly enhance this process, further supporting financial sustainability.
- Operational Efficiency: The structured methodology of RCM enhances workflows, alleviates administrative burdens, and enables staff to concentrate on patient care rather than paperwork. This transition enhances productivity and ensures more effective resource allocation. The integration of structured payment plans and eligibility preparedness into RCM processes contributes to operational efficiency. Automation in revenue cycle management could save the healthcare industry an estimated $22.3 billion annually, highlighting the potential for operational improvements.
Traditional Billing Practices:
- Financial Sustainability: Although traditional billing may appear cost-effective at first glance, its reactive nature often leads to delayed payments and increased write-offs due to denials. This inefficiency can jeopardize the financial stability of a business over time. The industry-average first-pass rejection rate is approximately 15%, illustrating the challenges faced by practices relying on outdated methods. Mistaken or insufficient medical coding can worsen these problems, resulting in denial of requests and heightened administrative workload. Healthcare Partners Consulting addresses these challenges by reviewing and correcting coding issues before claims are submitted, ensuring compliance and reducing errors from the start.
- Operational Efficiency: The manual processes inherent in traditional billing contribute to inefficiencies, increased errors, and elevated administrative costs. Staff may find themselves dedicating excessive time to billing tasks, which detracts from their ability to deliver quality patient care. As healthcare organizations increasingly outsource RCM functions, they can improve billing accuracy and accelerate cash flow, further enhancing operational efficiency. Healthcare Partners Consulting specializes in mental and behavioral health coding, ensuring that organizations receive customized support that enhances accuracy and compliance.
In summary, while traditional billing practices may offer initial simplicity and lower costs, RCM presents a more sustainable and efficient strategy for managing healthcare finances, ultimately fostering improved patient outcomes and supporting practice growth. Ultimately, embracing RCM not only enhances financial health but also positions practices for sustainable growth in a competitive landscape.
Conclusion
The transition from traditional billing practices to Revenue Cycle Management (RCM) signifies a pivotal change in optimizing financial health for healthcare organizations. RCM emerges as a comprehensive strategy that not only streamlines billing processes but also enhances the overall patient experience through proactive management and data-driven insights. Traditional billing practices create obstacles that hinder timely payments and increase administrative burdens, jeopardizing a healthcare provider’s financial sustainability.
Key arguments highlight the advantages of RCM, including its ability to ensure timely reimbursements, reduce errors, and improve operational efficiency. The ten steps of RCM – ranging from patient registration to continuous improvement – illustrate a systematic approach that fosters financial stability and enhances cash flow. By adopting RCM, healthcare providers can significantly lower their claim denial rates and improve their overall revenue cycle efficiency, ultimately leading to better patient outcomes and satisfaction.
As the healthcare landscape evolves, choosing between RCM and traditional billing practices becomes increasingly important. Embracing RCM not only positions healthcare organizations for sustainable growth but also empowers them to navigate the complexities of financial management effectively. Ultimately, the decision to adopt RCM will determine the ability of healthcare organizations to thrive in an increasingly complex financial landscape.
Frequently Asked Questions
What is Revenue Cycle Management (RCM)?
Revenue Cycle Management (RCM) is a framework for healthcare organizations that guides them through the stages of patient care episodes, from registration to final payment, with the aim of enhancing financial performance.
What are the critical stages involved in RCM?
The critical stages of RCM include patient scheduling, insurance verification, coding, billing, and collections.
How does RCM benefit healthcare providers?
RCM benefits healthcare providers by ensuring timely and accurate reimbursements, minimizing errors and denials, leading to improved financial performance.
What services does Healthcare Partners Consulting provide related to RCM?
Healthcare Partners Consulting provides accounts receivable management solutions that optimize RCM processes, including proactive follow-up with payers on unpaid or underpaid requests and appeal submissions for denied requests.
What features support financial health in RCM?
Features that support financial health in RCM include structured payment plans coordination, monthly reconciliation, and accounts receivable trending analysis.
How do traditional billing practices differ from RCM?
Traditional billing practices focus on submitting requests and collecting payments after services are provided, relying on manual processes and direct communication with insurers, which leads to inefficiencies and increased administrative burdens.
What are the drawbacks of traditional billing practices?
Drawbacks of traditional billing practices include delayed payments, increased rejection rates, and a lack of proactive measures, making it a reactive approach to managing revenue flow.
Why is adopting a proactive revenue management strategy important for healthcare providers?
Adopting a proactive revenue management strategy is essential for healthcare providers to effectively navigate challenges related to delayed payments and rejection rates.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting