Uncategorized
Essential ICD Codes for Pain: A Checklist for Clinic Owners

Introduction
The financial viability of healthcare practices, especially in pain management, hinges on a thorough understanding of ICD codes. These codes not only influence billing accuracy and reimbursement rates but also enhance communication among providers and patients, ultimately improving care quality.
Clinic owners face ongoing challenges in keeping up with the latest ICD codes, risking errors and compliance issues. This article presents a comprehensive checklist of essential ICD codes for pain, providing insights and best practices for navigating coding complexities in clinical settings.
Understand the Importance of ICD Codes for Pain
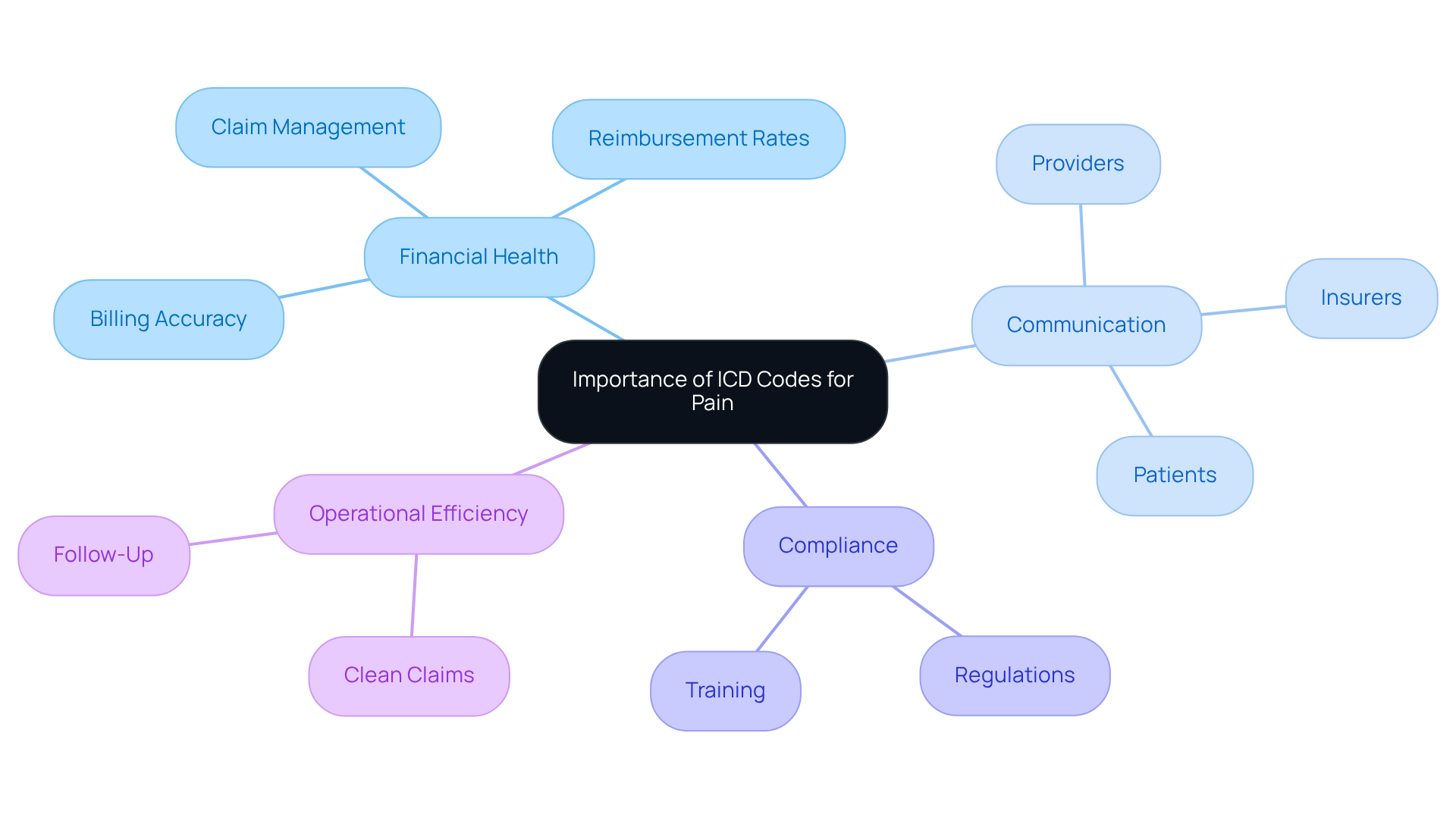
ICD codes play a critical role in the financial health of mental health practices, influencing billing accuracy and reimbursement rates. Effective management of patient statements is essential for addressing underpayments, unprocessed claims, and aging claims, all of which significantly impact revenue cycles. Furthermore, effective programming significantly lowers the risk of claim denials and audits, which can disrupt revenue cycles and result in financial losses. Precise programming reflects the complexity of care provided, a crucial factor for securing appropriate reimbursement from insurers.
Additionally, ICD codes facilitate effective communication among healthcare providers, insurers, and patients, enhancing the overall quality of care. Compliance with healthcare regulations is vital to avoid penalties and maintain the integrity of your practice, as inaccuracies can lead to audits and compliance concerns. Continuous training for programming personnel is crucial to stay updated with healthcare regulations and classification changes.
Examining rejected claims helps identify underlying issues, allowing for proactive steps to reduce risks related to mistakes in programming. High-risk medical coding errors can lead to substantial revenue loss and potential legal penalties. Therefore, concentrating on improving operations by ensuring clean claims and quick follow-up is essential for enhancing efficiency.
Identify Key ICD Codes for Pain Management
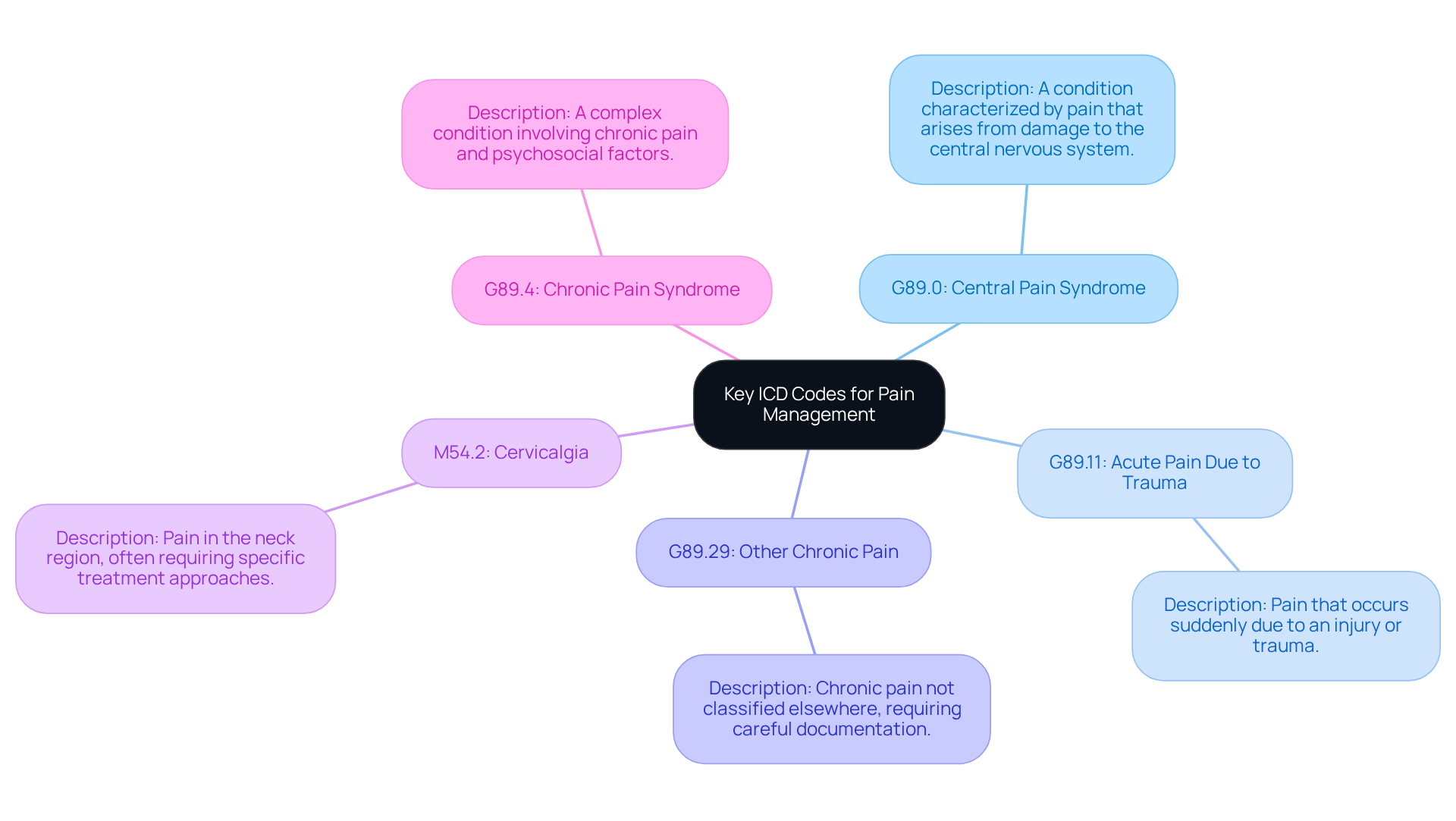
Understanding key ICD codes for pain is essential for effective clinical practice and compliance. Familiarize yourself with the following key ICD codes:
- G89.0: Central pain syndrome
- G89.11: Acute pain due to trauma
- G89.29: Other chronic pain
- M54.2: Cervicalgia (neck pain)
- G89.4: Chronic pain syndrome
It is crucial to maintain an updated list of ICD codes relevant to your practice’s pain management services, as precise programming directly affects billing and compliance. Frequently assess programming updates; the FY 2026 ICD-10-CM revision introduced 487 new diagnosis codes, modified 38 codes, and removed 28 codes. Staying informed ensures adherence to the latest guidelines and minimizes the risk of compliance issues.
Clinics that manage their coding practices effectively report improved revenue and reduced administrative burdens. For instance, clinics using the ICD code for pain, particularly G89 codes for chronic pain management, have observed improved record accuracy, aligning with ICD-10-CM guidelines.
Experts emphasize the importance of using the appropriate ICD code for pain based on patient records to maintain healthcare integrity. This approach not only safeguards against potential audits and legal consequences but also enhances the overall quality of healthcare documentation.
Follow Best Practices for Accurate Pain Coding
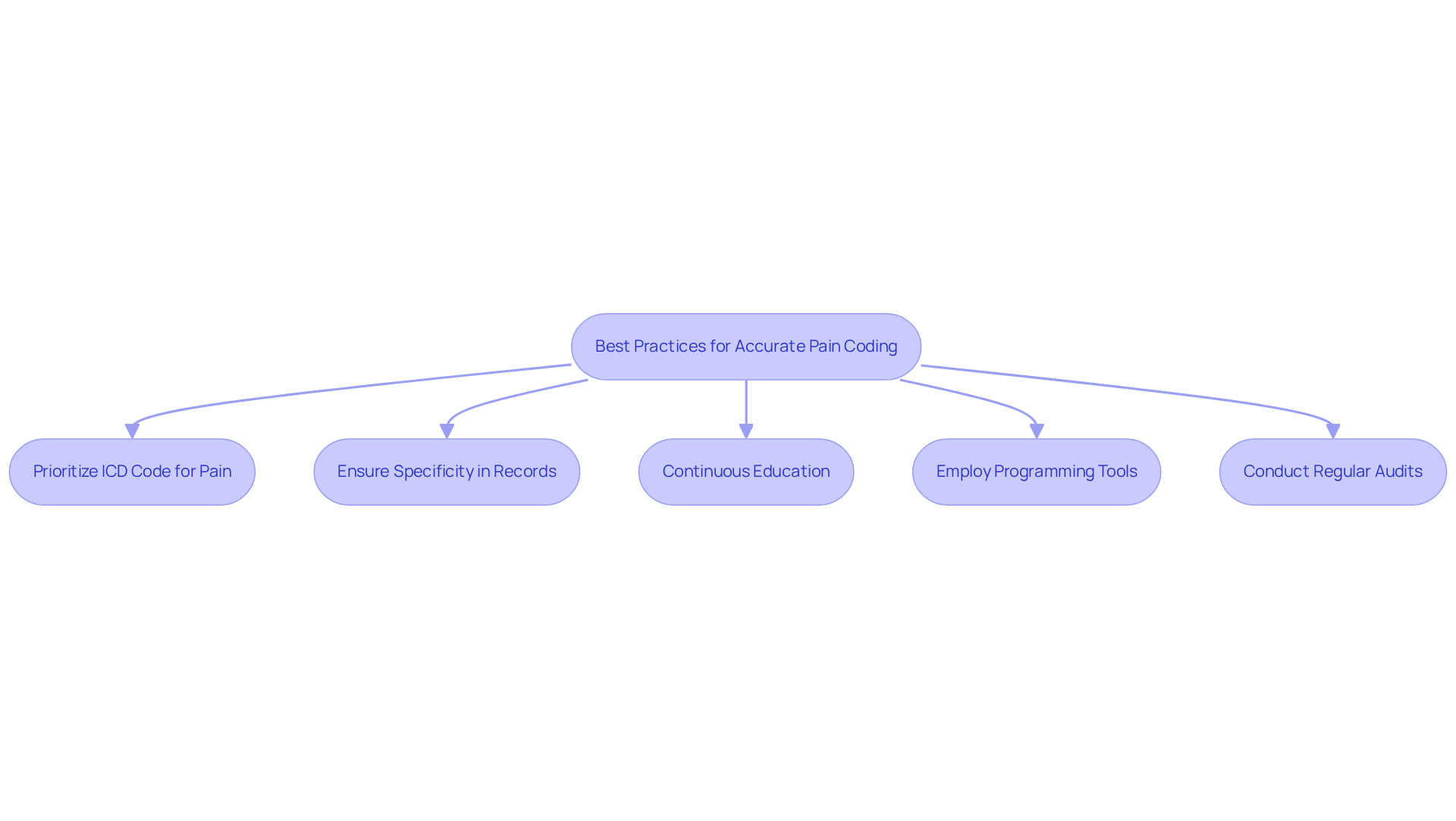
Prioritizing the icd code for pain is essential for effective pain management and accurate billing. Always sequence the icd code for pain first when the primary reason for the visit is pain management. This prioritization is vital for ensuring accurate billing and reimbursement.
Specificity in records is critical for the approval of claims and the prevention of denials. Ensure that documentation clearly supports the diagnosis codes used, as this clarity is essential for successful claims processing.
Continuous education is essential; failure to train programming staff following annual updates can lead to increased rejections. Educate personnel consistently on programming updates and optimal methods, as neglecting this training may result in significant financial implications.
Employ programming tools that recommend suitable codes based on clinical records, enhancing the precision and effectiveness of coding classification methods. This approach not only improves accuracy but also streamlines the coding process.
Conduct regular audits of programming practices to identify and rectify errors. Frequent internal reviews can uncover recurring issues and improve overall accuracy, ensuring that coding practices remain robust and reliable. Regular audits and training are not just beneficial; they are necessary to maintain the integrity of coding practices and minimize financial losses.
Ensure Proper Documentation for Pain Codes
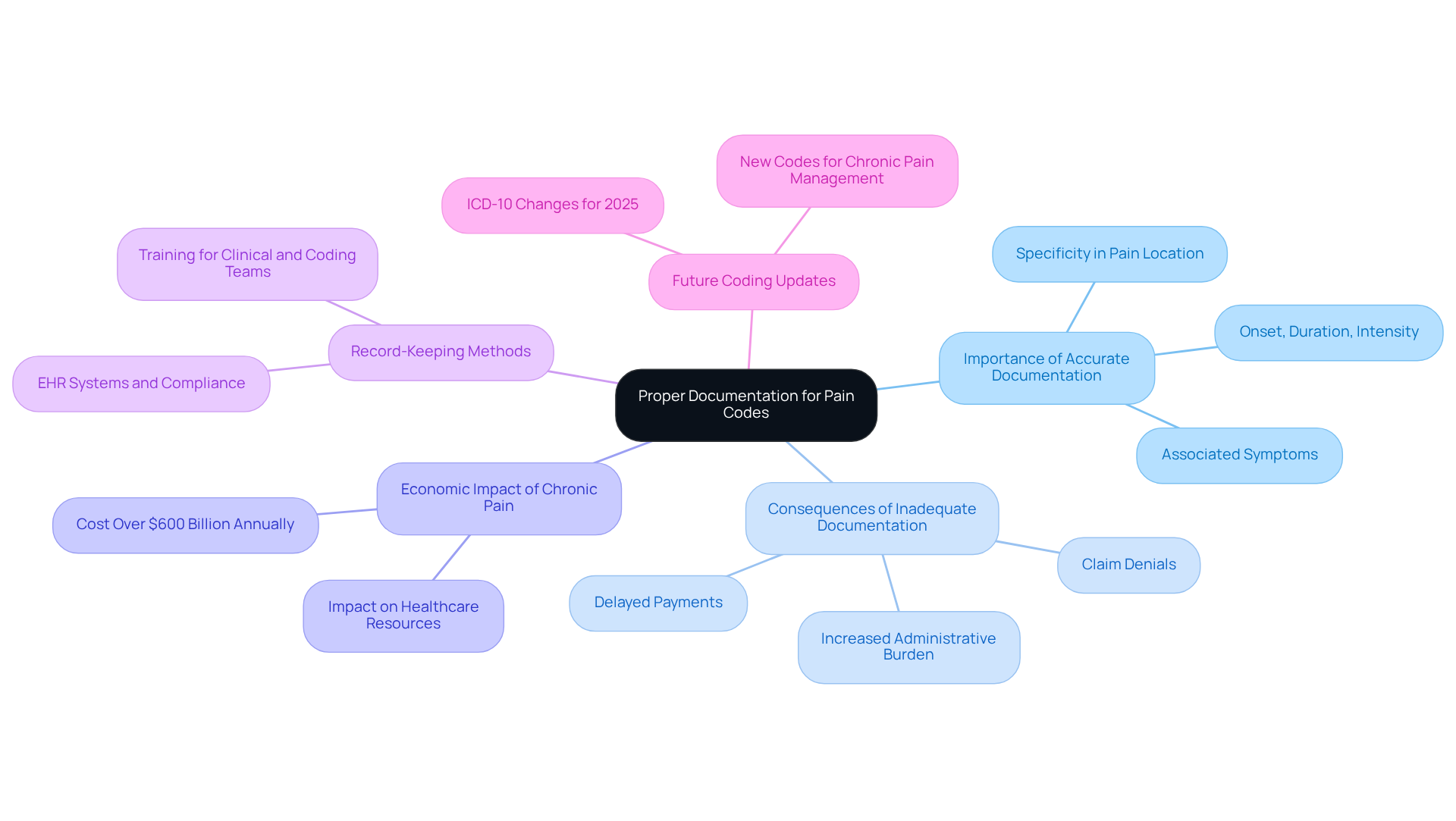
Accurate documentation of a patient’s pain history is crucial for effective coding, particularly when determining the ICD code for pain and reimbursement. Document the patient’s pain history, including onset, duration, and intensity, as this information is vital for accurate coding and reimbursement. Include specific details about the discomfort’s location, laterality, and any associated symptoms to avoid non-specific codes that can lead to claim denials.
Statistics indicate that 17 out of the 100 most frequently used diagnoses include the ICD code for pain. This underscores the need for comprehensive recording. Log the treatment plan and any interventions carried out, ensuring that records support medical necessity and align with payer requirements. Ensure that all records are legible and accessible for review. Inadequate documentation can lead to delays in payment and increased administrative burdens.
Chronic discomfort imposes a cost exceeding $600 billion on the US economy each year. This highlights the necessity for effective management classification. Frequently assess record-keeping methods to guarantee adherence to programming standards. Detailed records can diminish the chance of mistakes and improve overall patient care.
As Ashley Carson, CPC, CCS-P, notes, ‘In pain management, precise documentation can be the key to a smooth reimbursement process, avoiding costly denials.’ Stay informed about the upcoming ICD-10 coding updates for 2025, as these changes will impact how the ICD code for pain is used in documenting diagnoses. Staying updated on coding changes is vital to ensure compliance and optimize reimbursement outcomes.
Conclusion
The effective management of ICD codes is crucial for the financial viability of healthcare practices. These codes ensure accurate billing and compliance. They also enhance communication among providers, insurers, and patients. Effective use of ICD codes correlates with improved reimbursement rates and reduced administrative burdens, making it critical for clinic owners.
Key insights from this article highlight the necessity of staying informed about the latest ICD codes, such as G89 and M54 series, and adhering to best practices in coding and documentation. Regular audits and ongoing education are essential for reducing errors and improving operational efficiency. By prioritizing accurate coding and thorough documentation, clinics can safeguard against claim denials and financial losses, ultimately improving the quality of care provided to patients.
In conclusion, the significance of accurate ICD coding in pain management cannot be overstated. As the landscape of healthcare continues to evolve, it is essential for clinic owners to remain proactive in their coding practices. Emphasizing the importance of compliance, continuous training, and meticulous documentation will not only enhance financial health but also contribute to better patient outcomes. Ultimately, prioritizing accurate coding practices is essential for navigating the complexities of modern healthcare billing and ensuring optimal patient care.
Frequently Asked Questions
What is the role of ICD codes in mental health practices?
ICD codes are critical for the financial health of mental health practices as they influence billing accuracy and reimbursement rates.
How do ICD codes affect revenue cycles?
Effective management of patient statements related to ICD codes addresses issues like underpayments, unprocessed claims, and aging claims, all of which significantly impact revenue cycles.
What are the consequences of ineffective programming in relation to ICD codes?
Ineffective programming can increase the risk of claim denials and audits, which can disrupt revenue cycles and lead to financial losses.
Why is precise programming important for reimbursement?
Precise programming reflects the complexity of care provided, which is crucial for securing appropriate reimbursement from insurers.
How do ICD codes improve communication in healthcare?
ICD codes facilitate effective communication among healthcare providers, insurers, and patients, thereby enhancing the overall quality of care.
What are the compliance risks associated with inaccuracies in ICD coding?
Inaccuracies can lead to audits and compliance concerns, resulting in penalties and threatening the integrity of the practice.
Why is continuous training for programming personnel important?
Continuous training is essential for keeping programming personnel updated with healthcare regulations and classification changes.
How can examining rejected claims benefit a practice?
Examining rejected claims helps identify underlying issues, allowing practices to take proactive steps to reduce risks related to mistakes in programming.
What are the potential consequences of high-risk medical coding errors?
High-risk medical coding errors can lead to substantial revenue loss and potential legal penalties.
What strategies can enhance efficiency in managing ICD codes?
Concentrating on improving operations by ensuring clean claims and quick follow-up is essential for enhancing efficiency.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting