Telehealth Billing Insights
10 Essential Telehealth Billing Codes Every Clinic Owner Must Know

Introduction
As healthcare increasingly transitions to remote services, understanding the nuances of telehealth billing has become essential. Clinics that effectively master the necessary billing codes not only improve their revenue cycle but also ensure compliance with the ever-evolving regulations. Yet, with a multitude of codes and guidelines available, how can clinic owners successfully navigate this intricate landscape? This article explores ten critical telehealth billing codes that every clinic owner should be familiar with, equipping them to optimize their billing practices and reduce claim denials.
Healthcare Partners Consulting: Essential Support for Telehealth Billing
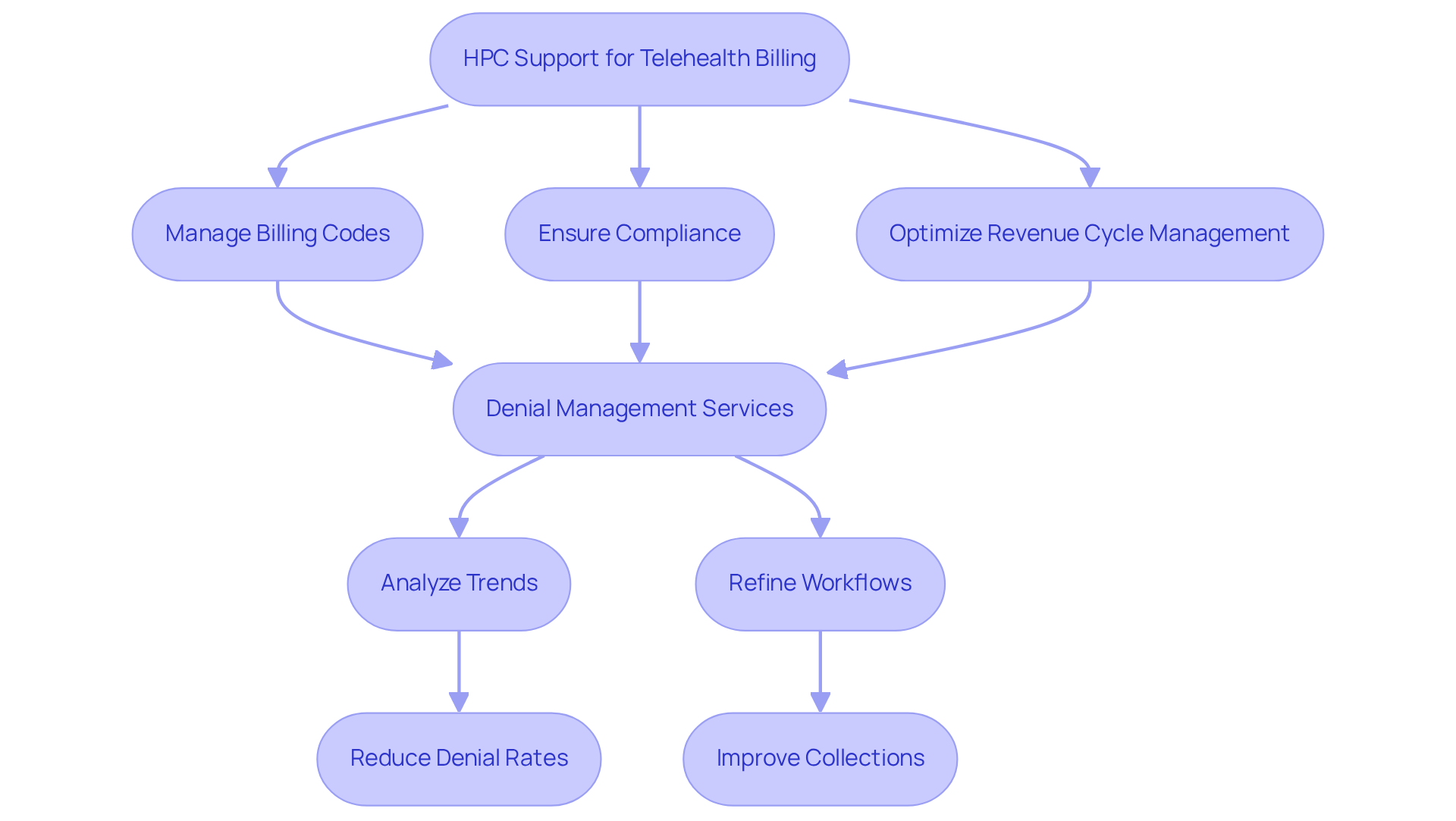
Healthcare Partners Consulting (HPC) is instrumental in supporting medical and mental health practices with remote health service payment. Their extensive administrative support allows clinics to focus on patient care, while HPC navigates the complexities of billing. This encompasses managing the evolving landscape of telehealth billing codes, ensuring compliance with payer requirements, and optimizing revenue cycle management.
HPC’s denial management services are vital, as each denied claim signifies a lost opportunity – often recoverable. By analyzing trends and refining workflows, HPC aids clinics in reducing administrative burdens and enhancing payment accuracy. This results in a 30-50% reduction in recurring denial types and improved collections from previously rejected claims. Many behavioral health organizations report denial rates below 10% and collection rates exceeding 97%, showcasing the effectiveness of HPC’s strategies.
By implementing robust invoicing practices, clinics can streamline their operations and safeguard their revenue, positioning HPC as a crucial partner in the evolving virtual healthcare landscape. Additionally, insights from industry experts, such as Davia Ward, highlight the persistent mental health payment crisis, underscoring the necessity for effective solutions in this domain.
CPT Codes for Telehealth Services: Key Codes to Know
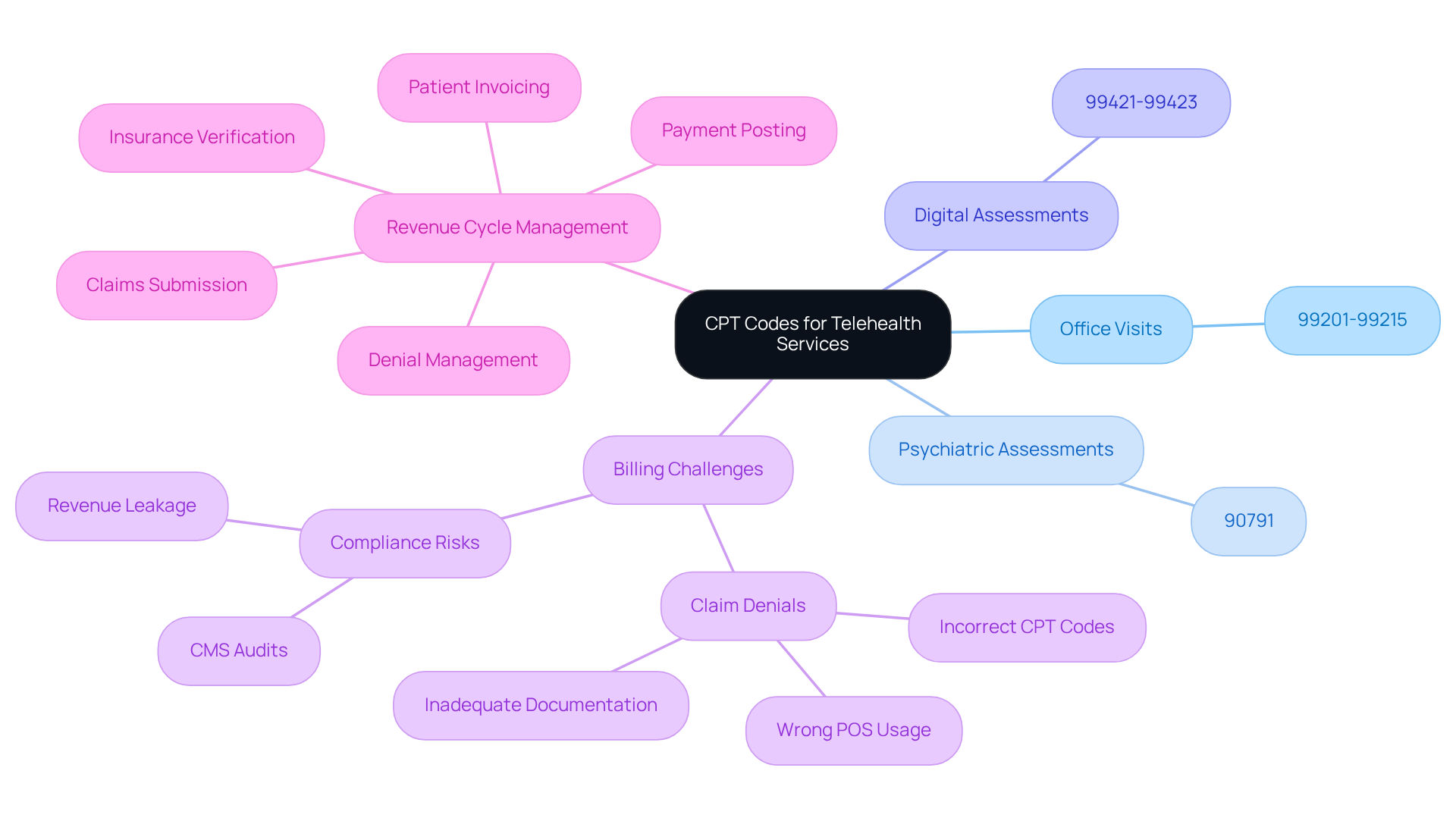
Knowledge of the proper CPT numbers is essential for effective invoicing using the telehealth billing code, as these codes directly influence reimbursement rates and compliance. Key codes include:
- 99201-99215: These codes represent office or other outpatient visits for both new and established patients, which are crucial for billing routine consultations.
- 90791: This identifier is utilized for psychiatric diagnostic assessments, a vital offering in mental health practices.
- 99421-99423: These numbers encompass online digital assessment and management offerings, reflecting the growing trend of virtual care.
The precise application of the telehealth billing code and other identifiers not only aids in securing appropriate reimbursement from payers but also minimizes the likelihood of claim denials. For instance, clinics that have implemented rigorous coding practices have reported revenue increases of up to 30%, underscoring the financial impact of accurate CPT coding. Furthermore, Healthcare Partners Consulting emphasizes the importance of comprehensive revenue cycle management solutions, which include insurance verification, claims submission, payment posting, denial management, and patient medical invoicing. As remote healthcare continues to evolve, staying informed about these essential regulations is critical for ensuring financial stability and compliance. Additionally, implementing proactive workflows and quality assurance processes can significantly enhance coding accuracy and reduce denials, thereby enabling practices to optimize their revenue cycle management effectively.
Understanding Place of Service (POS) Codes for Telehealth Billing
Understanding Place of Service (POS) Codes for Telehealth Billing
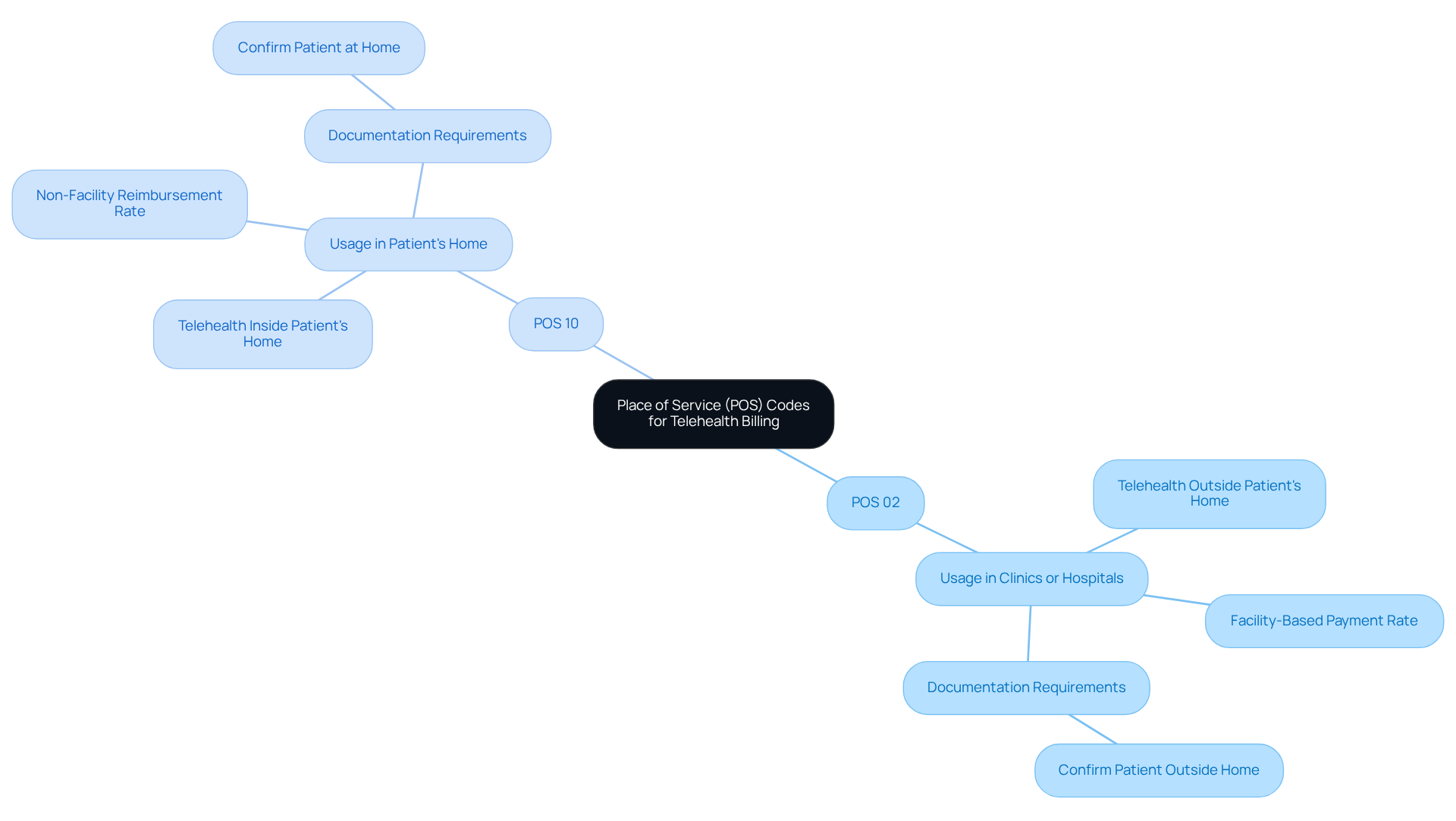
Place of Service (POS) codes serve as critical indicators of where healthcare services are delivered, playing a vital role in billing accuracy. For telehealth services, two codes are particularly significant:
- POS 02: This code is utilized when telehealth services are provided outside the patient’s home, such as in a clinic or hospital setting.
- POS 10: This code identifies remote healthcare services delivered in the patient’s residence, a practice that has become increasingly common.
The precise use of these POS classifications is essential for adherence to payer requirements and for minimizing the risk of claim denials. Clinics that correctly employ POS 02 and POS 10 have reported a notable decrease in claim rejections, underscoring the importance of accurate coding practices. As the telehealth landscape continues to evolve, staying informed about the latest trends in telehealth billing codes is crucial for maintaining revenue integrity and ensuring successful reimbursement. Experts emphasize that the proper application of POS codes not only aids in compliance during audits but also enhances the overall effectiveness of financial processes, ultimately benefiting both providers and patients.
To further assist mental health providers, Healthcare Partners Consulting offers a comprehensive toolkit designed to simplify administrative processes. This toolkit provides clear action steps and resources that can help therapists navigate the complexities of invoicing and coding, ensuring they are well-prepared to manage their practices effectively.
Telehealth Modifiers: Enhancing Billing Accuracy
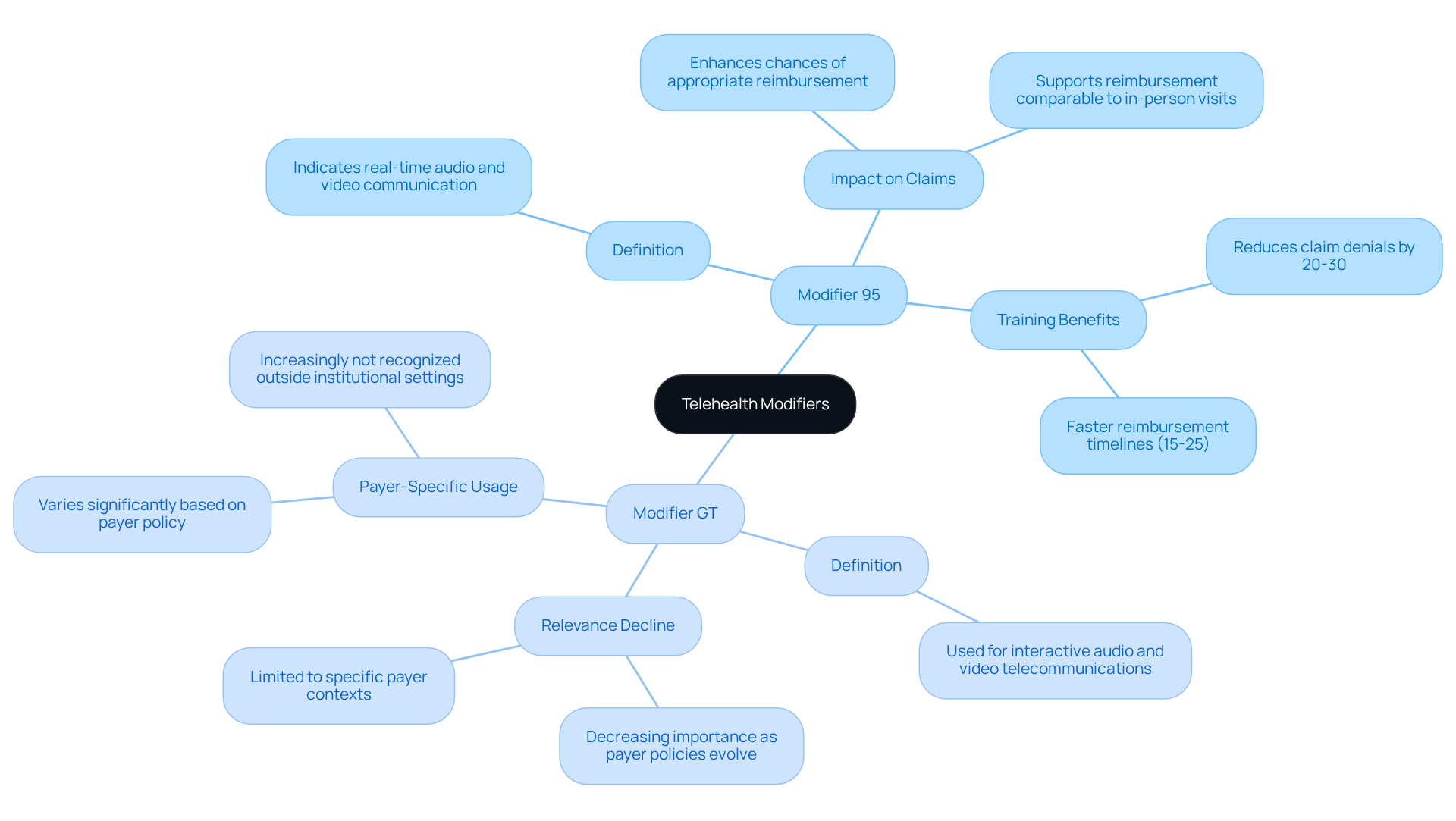
Modifiers play a crucial role in defining the characteristics of remote healthcare, directly impacting the accuracy of the telehealth billing code and reimbursement outcomes. Two key telehealth modifiers are:
- Modifier 95: This modifier indicates that the service was rendered via real-time audio and video communication, ensuring that claims are recognized as telehealth encounters.
- Modifier GT: Traditionally utilized for services delivered through interactive audio and video telecommunications, this modifier has seen a decline in relevance as payer policies evolve.
The correct application of the telehealth billing code is essential for minimizing claim denials. Clinics that have implemented rigorous training on modifier usage have reported significant reductions in claim rejections. Some have experienced a 20-30% reduction in claim denials and a 15-25% faster reimbursement timeline. By ensuring that documentation aligns with the requirements of Modifier 95, providers can enhance their chances of receiving appropriate reimbursement.
Current trends indicate that while Modifier 95 remains widely accepted, the use of Modifier GT is becoming increasingly payer-specific and limited. As invoicing practices adapt to these changes, ongoing education and adherence to updated payer policies are vital for maintaining compliance and optimizing revenue. Billing professionals emphasize that selecting the correct modifier and the appropriate telehealth billing code is one of the most effective strategies for reducing claim denials, underscoring the importance of precise documentation and understanding payer-specific requirements.
Audio-Only Telehealth Codes: What Providers Need to Know
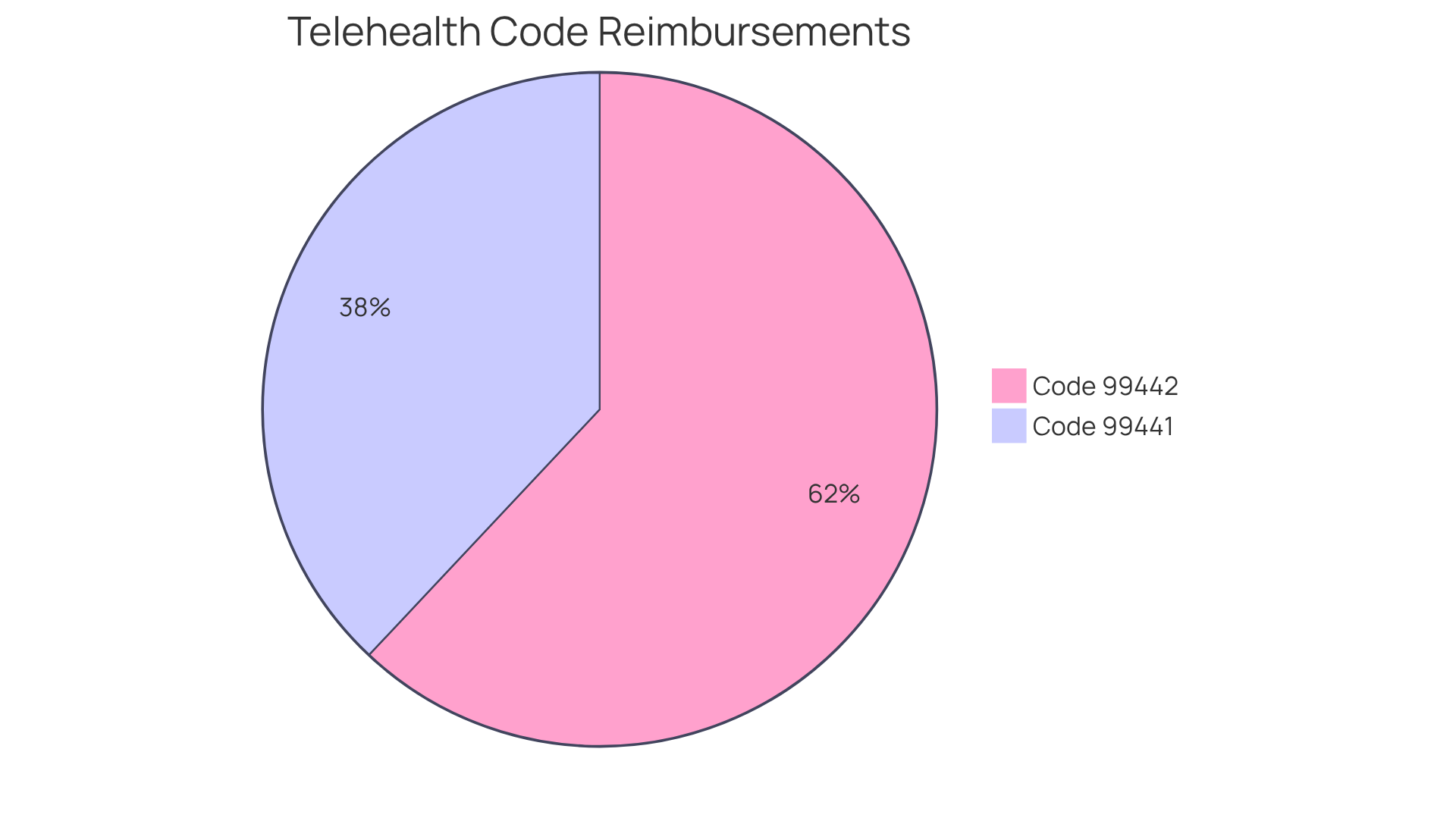
The increasing acceptance of audio-only telehealth options underscores the necessity for providers to be well-versed in the telehealth billing code and relevant billing guidelines. Two critical codes are:
- 99441: This code applies to telephone evaluation and management services rendered by a physician or qualified healthcare professional, offering reimbursement of $57 for 5 to 10 minutes of medical discussion.
- 99442: This designation relates to telephone evaluation and management services that require a higher level of medical decision-making, with a reimbursement rate of $93 for 11 to 20 minutes of discussion.
These regulations enable healthcare professionals to bill for assistance provided via phone, ensuring continuity of care for patients who may not have access to video technology. As remote healthcare becomes standard practice, comprehending these classifications is vital for maintaining financial viability and compliance. Recent legislative measures have extended essential remote healthcare flexibilities through the end of 2027, allowing providers to continue utilizing audio-only services, which are particularly advantageous for patients with chronic conditions.
To minimize telehealth denials in Medicare, it is imperative to verify CPT codes against the CMS telehealth list and confirm audio-only eligibility before using the telehealth billing code. Furthermore, providers must document the rationale for employing audio-only options to ensure compliance and mitigate the risk of audits. This shift highlights the importance of meticulous documentation and adherence to billing guidelines to prevent denials and secure appropriate reimbursement.
Healthcare Partners Consulting enhances healthcare efficiency through comprehensive medical billing solutions, ensuring accurate coding and timely reimbursement. Their expertise in preventing modifier errors, particularly those related to remote healthcare services, includes training billers on payer-specific requirements, utilizing internal checklists, and auditing high-risk claims. This thorough approach aids clinics in reducing denials and improving overall revenue cycle management.
Remote Patient Monitoring (RPM) Codes: Essential for Telehealth
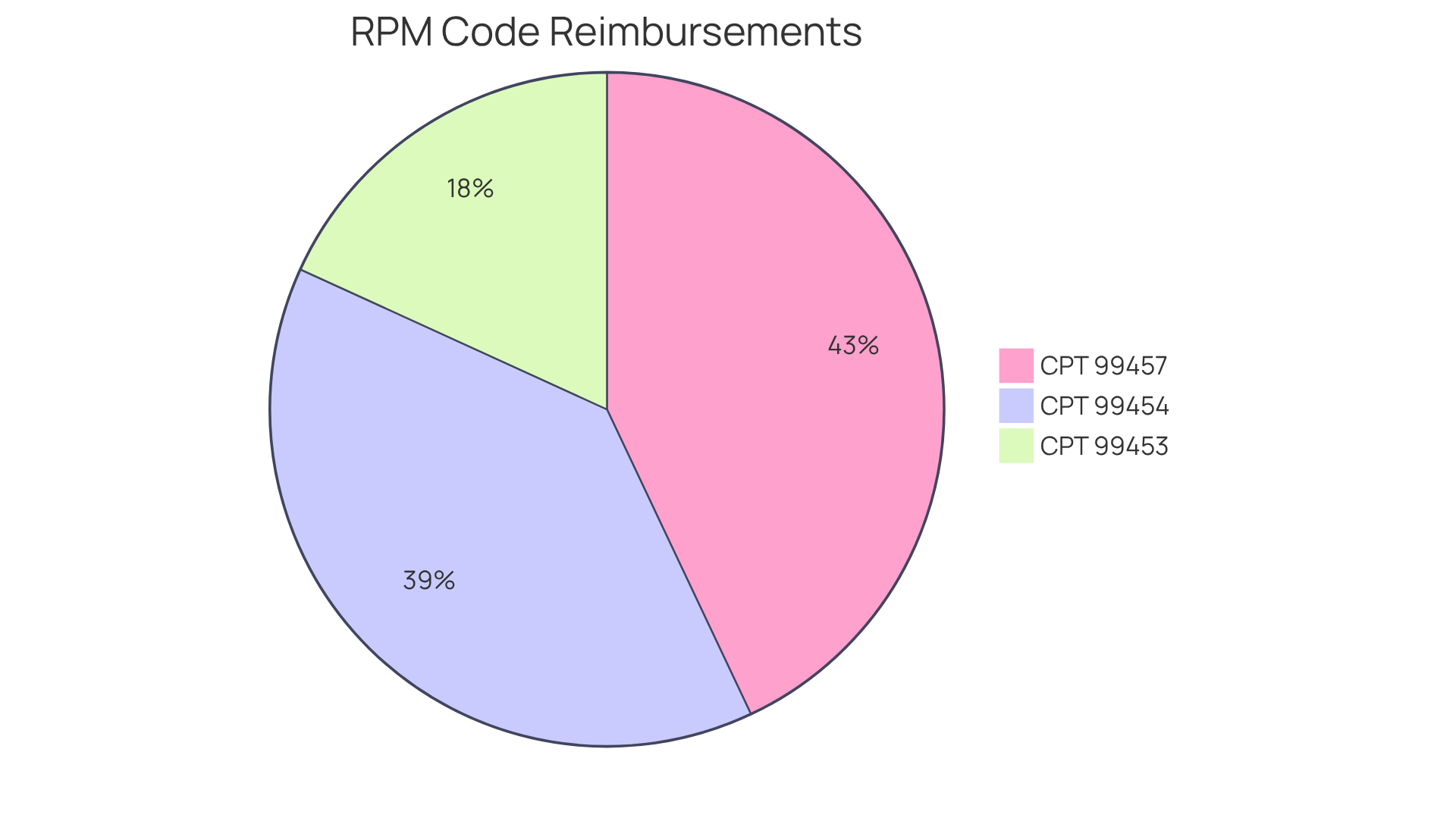
Remote Patient Monitoring (RPM) represents a crucial component of telehealth, allowing healthcare providers to effectively monitor patient health data from a distance. Key RPM codes include:
- CPT 99453: This code covers the initial setup and patient education regarding the use of RPM devices, with reimbursement set at approximately $22.
- CPT 99454: This pertains to device supply, facilitating daily recordings or program alerts, and offers a reimbursement rate of around $47 for monitoring periods lasting 16 to 30 days.
- CPT 99457: This encompasses remote physiologic monitoring treatment management services, with an average reimbursement of $52 for the first 20 minutes of management.
These systems assist clinics in invoicing for the ongoing management of patients’ health, thereby enhancing care continuity and improving patient outcomes. For example, clinics utilizing RPM classifications have reported notable improvements in patient engagement and health management, particularly for chronic conditions such as hypertension and diabetes. Recent updates to the telehealth billing code reflect a growing recognition of their importance in telehealth, as they provide more flexible payment options and better alignment with clinical needs.
Healthcare Partners Consulting (HPC) enhances this process by offering comprehensive medical invoicing solutions that streamline operations and reduce claim denials by 20 to 30%. Their services include denial management, performance reporting, and insurance eligibility verification, enabling healthcare providers to focus on patient care rather than financial complexities. The integration of RPM into practice not only supports improved patient outcomes but also streamlines administrative processes, allowing providers to prioritize delivering quality care. The ongoing evolution of RPM codes is expected to further reinforce their role in remote healthcare, ensuring that patients receive timely and effective care while minimizing administrative burdens for providers.
Documentation Practices: Ensuring Compliance in Telehealth Billing
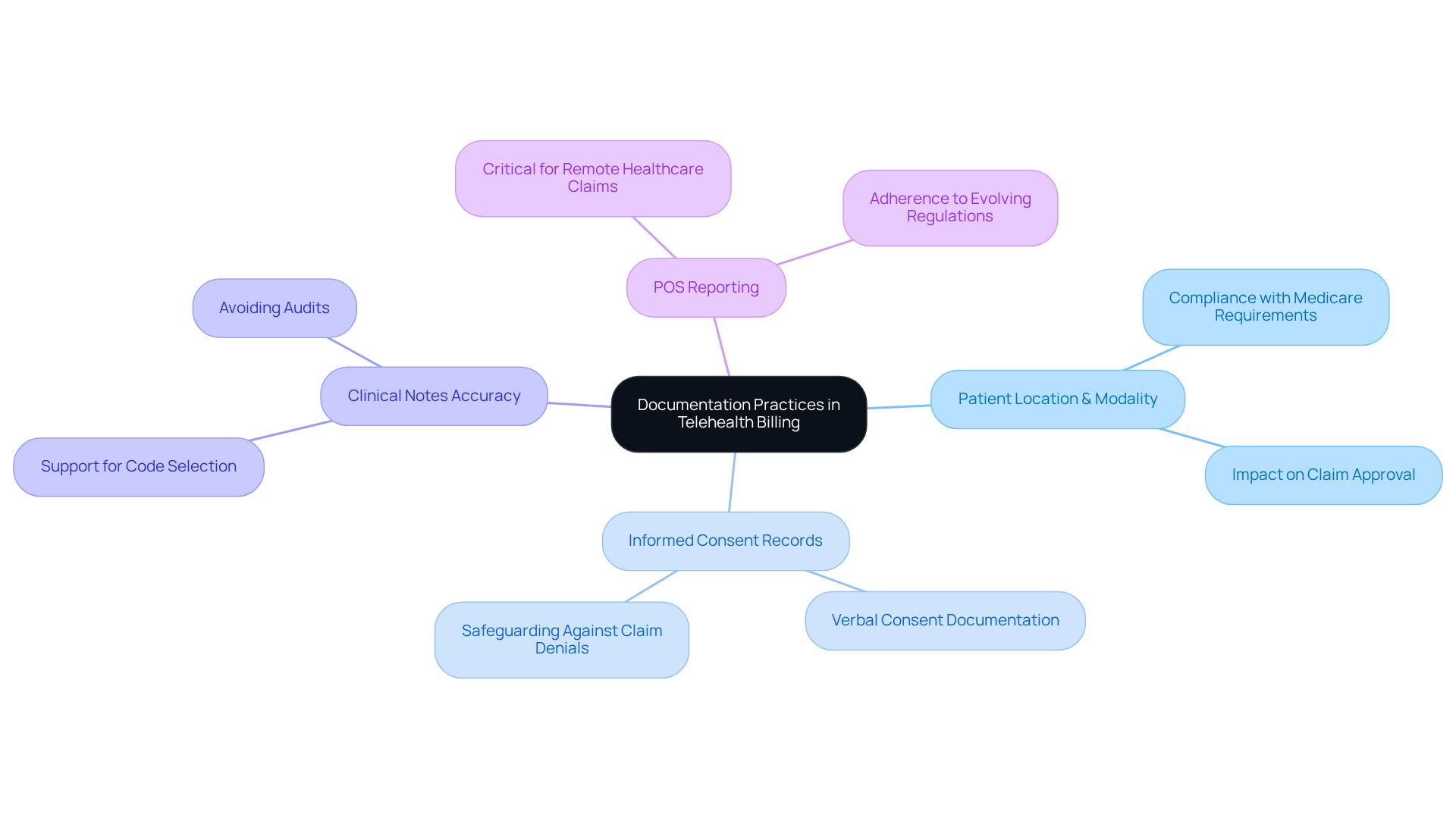
Precise documentation is crucial for effective remote healthcare billing, especially when applying the telehealth billing code in the evolving landscape of healthcare regulations. Key practices include:
- Documenting the patient’s location and the modality of service to ensure compliance with Medicare’s telehealth requirements.
- Maintaining comprehensive records of informed consent for telehealth services, which can be verbal if properly documented, is crucial to safeguard against claim denials associated with the telehealth billing code. Healthcare Partners Consulting emphasizes that their team reviews and corrects coding issues prior to claim submission, significantly minimizing errors from the outset.
- Ensuring that all clinical notes accurately reflect the services rendered and the rationale for care, as this documentation supports code selection and meets the necessary standards to avoid audits. Their certified medical coding specialists are well-versed in the nuances of behavioral health coding, ensuring that every claim submitted adheres to payer-specific guidelines.
These practices not only assist clinics in complying with payer requirements but also substantially mitigate the risk of audits and denials. For example, clinics that have adopted structured documentation protocols have reported enhanced compliance rates and a reduction in claim rejections. Furthermore, it is vital to note that only direct patient care time is billable for time-based remote healthcare services, excluding administrative tasks. Accurate POS reporting is also critical for remote healthcare claims in 2026, as it ensures adherence to evolving regulations. By prioritizing precise documentation, practices can enhance their invoicing processes and secure sustainable revenue streams by utilizing the telehealth billing code in the remote healthcare environment.
Common Telehealth Billing Mistakes: How to Avoid Revenue Loss
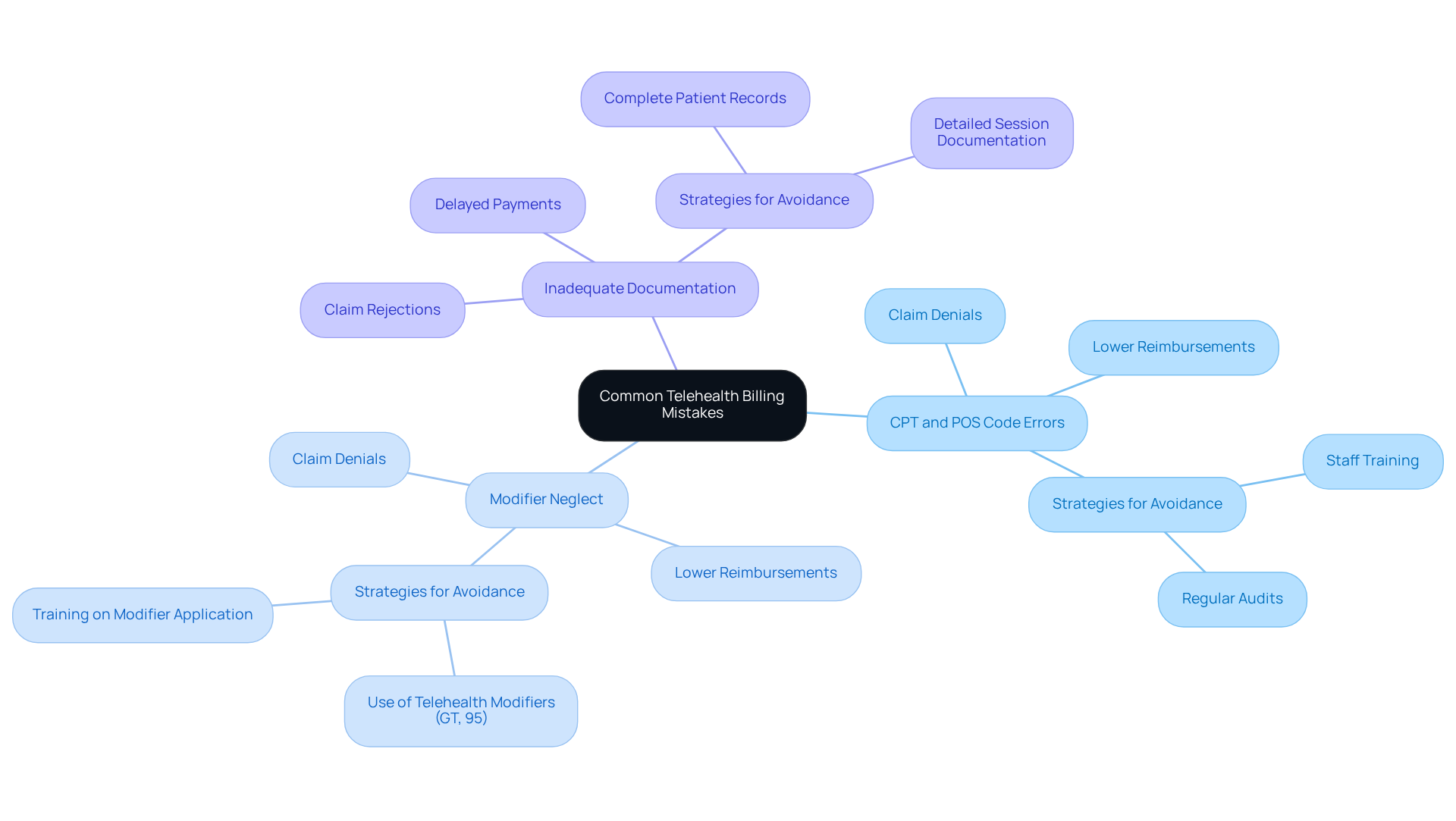
Common errors in remote healthcare billing can lead to significant revenue loss. Key errors to avoid include:
- Incorrect use of CPT and POS codes: Misapplication of these codes can result in claim denials. Studies indicate that up to 32% of claim denials stem from coding issues.
- Neglecting to utilize suitable modifiers: Modifiers specific to remote care, such as GT and 95, are crucial for recognizing provisions rendered through virtual healthcare. Incorrect application can lead to lower reimbursements or outright denials.
- Inadequate documentation: Insufficient documentation that fails to support billed offerings is a frequent pitfall. Approximately 80% of medical bills contain errors, and missing elements can lead to claim rejections.
By being aware of these pitfalls, clinic owners can implement strategies to minimize errors and ensure timely reimbursement. Investing in staff training on the telehealth billing code is essential, as nearly 30% of insurance claims are denied on first submission, with many denials being potentially avoidable. Regular audits and updates of credentialing records can help maintain compliance and reduce the risk of denied claims. Clinics that proactively address these issues can significantly enhance their revenue cycle management and protect their financial stability.
Healthcare Partners Consulting offers comprehensive accounts receivable management solutions that can significantly enhance revenue cycle efficiency. Their offerings include:
- Proactive follow-up with payers on unpaid or underpaid claims
- Appeal submissions for denied claims
- Aging report reviews
- Patient statement generation
- Structured payment plans coordination
By utilizing these services, clinics can enhance cash flow, decrease denials, and simplify compliance, ultimately safeguarding their financial stability.
Upcoming Changes in Telehealth Billing Codes: What to Expect
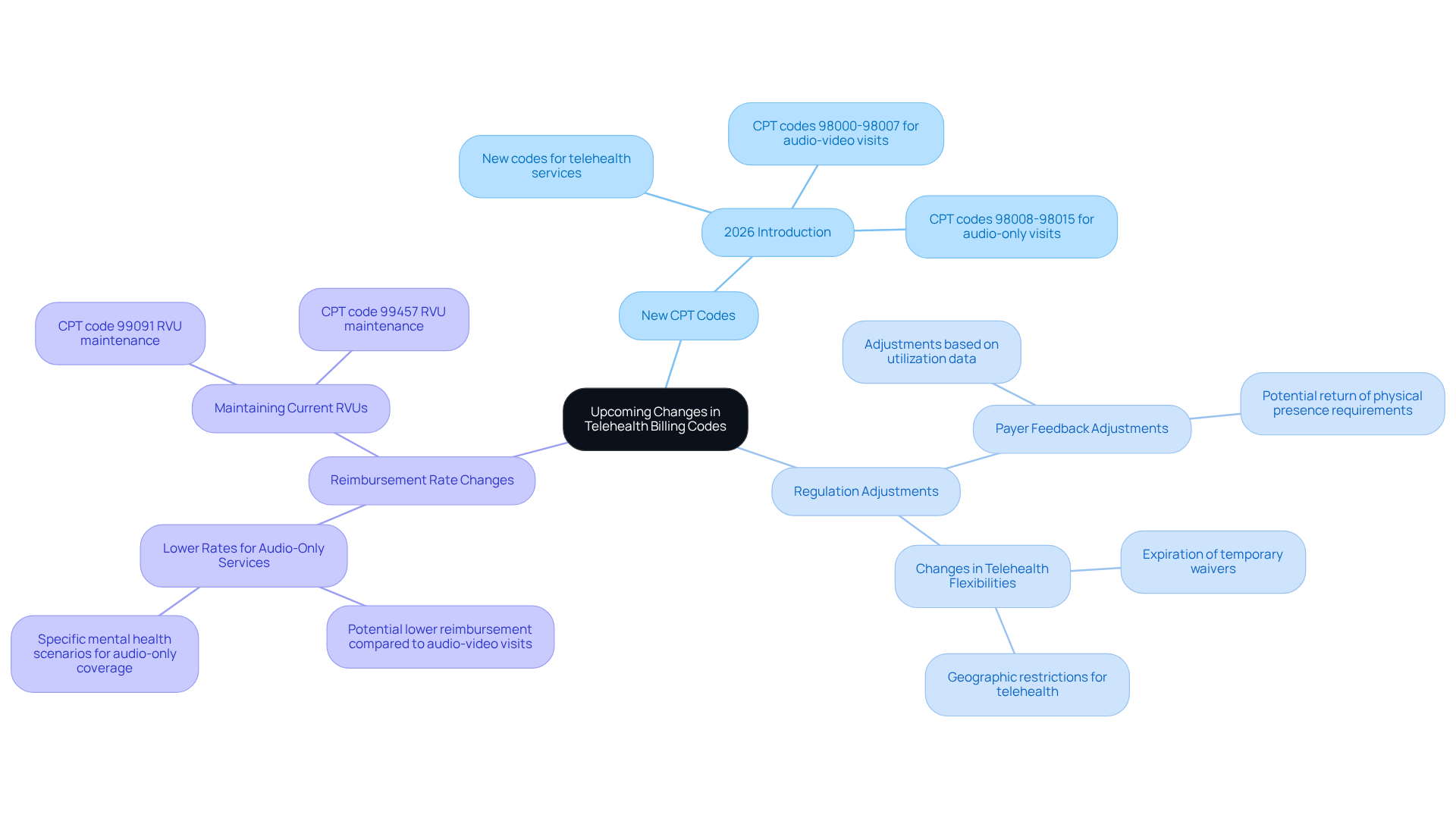
As remote healthcare evolves, it is essential for clinics to stay informed about updates in payment classifications to enhance their revenue and compliance. Key upcoming changes include:
- The introduction of new CPT codes for telehealth services in 2026, which will establish clearer billing guidelines.
- Adjustments to existing regulations based on payer feedback and utilization data, reflecting the ongoing enhancement of telehealth practices.
- Possible alterations in reimbursement rates, especially for audio-only services, which may be lower compared to audio-video visits.
Clinics must prepare for these changes by reviewing payer contracts, updating practice management software to integrate new place-of-service codes, and investing in training for coding and invoicing teams. Understanding these changes is crucial for maintaining stability in the evolving healthcare landscape and ensuring accurate invoicing practices.
Payer-Specific Guidelines: Navigating Telehealth Billing Requirements
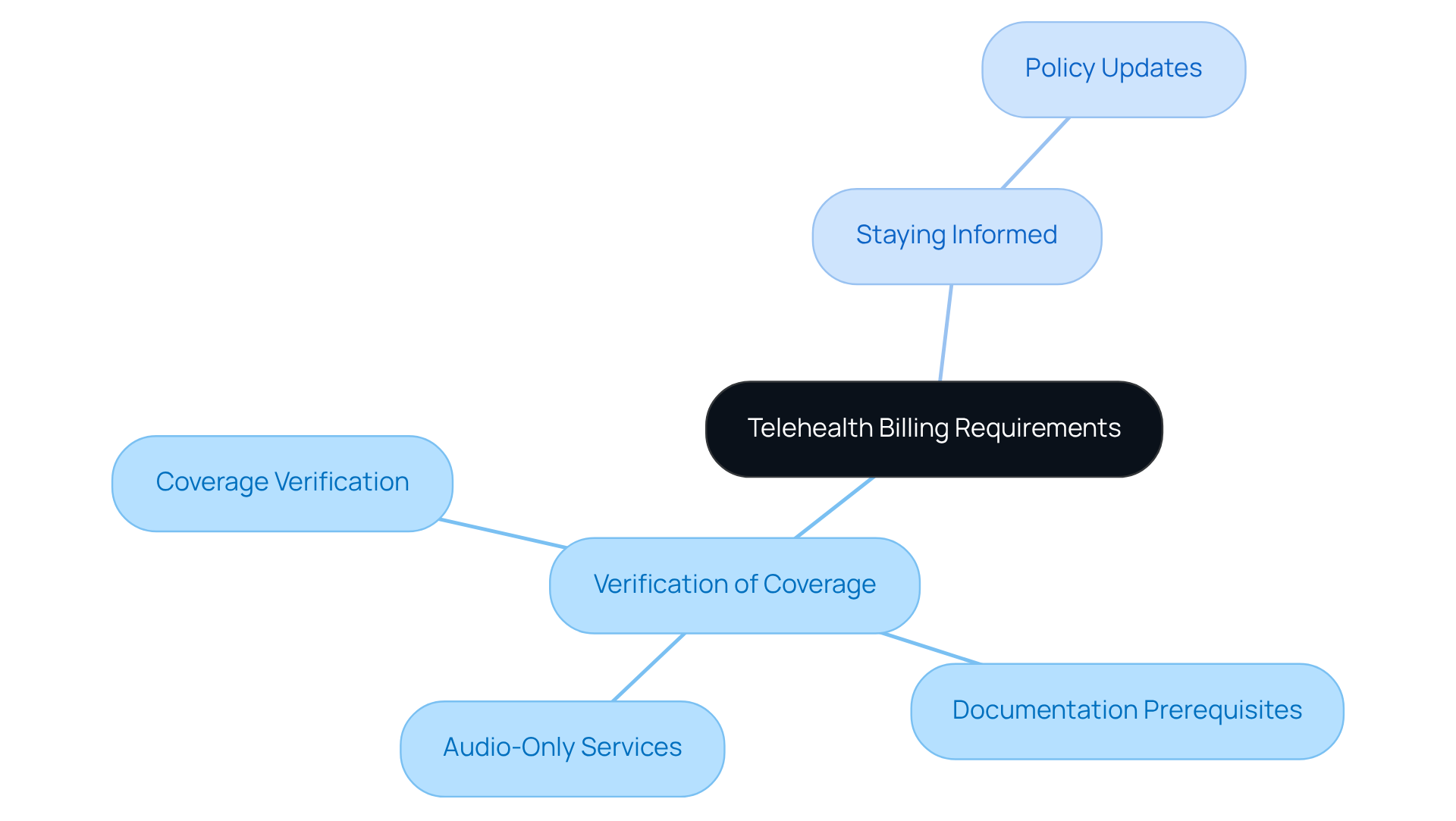
Navigating remote healthcare billing requirements presents a complex challenge, as each payer has distinct guidelines that clinics must comprehend to ensure compliance and optimize revenue. Key considerations include:
- Verification of Coverage: It is imperative for clinics to verify coverage for telehealth services with each payer, given that policies can differ significantly. This verification step is crucial to avert unforeseen denials and to ensure that the services provided are reimbursable. Understanding the specific documentation prerequisites and accepted billing classifications, including the telehealth billing code, for various insurers is essential. Many organizations face challenges due to a lack of comprehensive knowledge regarding complete code descriptions, particularly concerning time thresholds and category types. It is vital that documentation supports the use of audio-only services, especially when patients lack audio-video capabilities, to maintain compliance.
- Staying Informed: Clinics must remain updated on changes in payer policies related to virtual care reimbursement to adjust their invoicing processes accordingly. For example, as of early 2026, several states have revised their Medicaid reimbursement policies, reflecting a broader trend towards more inclusive telehealth coverage.
By adeptly navigating these guidelines, clinics can enhance their billing processes, improve compliance, and significantly mitigate the risk of claim denials. This proactive approach not only protects revenue but also ensures that patients receive the necessary care without unnecessary barriers.
Conclusion
Understanding the complexities of telehealth billing is essential for clinic owners aiming to optimize revenue and ensure compliance. This article outlines the critical telehealth billing codes that every clinic should know, highlighting the necessity of accurate coding practices to secure appropriate reimbursement and reduce claim denials. By utilizing specialized consulting services such as Healthcare Partners Consulting, clinics can effectively navigate billing complexities, improve revenue cycle management, and concentrate more on patient care.
Key insights include:
- The importance of proper CPT and POS codes
- The function of modifiers in enhancing billing accuracy
- The need for meticulous documentation practices
Furthermore, the article addresses common billing errors that can result in revenue loss and the forthcoming changes in telehealth billing codes that clinics must prepare for. Staying informed and proactive in these areas is vital for maintaining financial stability and ensuring that patients receive necessary care without unnecessary obstacles.
As the telehealth landscape evolves, it is crucial for healthcare providers to adapt by investing in training and resources that improve their billing practices. Implementing these strategies not only protects revenue but also reinforces the commitment to delivering high-quality care in a rapidly changing environment. By prioritizing telehealth billing education and compliance, clinics can position themselves for success in the future of remote healthcare.
Frequently Asked Questions
What services does Healthcare Partners Consulting (HPC) provide for telehealth billing?
HPC supports medical and mental health practices with remote health service payment by managing billing complexities, ensuring compliance with payer requirements, and optimizing revenue cycle management.
How does HPC help with denial management?
HPC’s denial management services analyze trends and refine workflows to reduce administrative burdens and enhance payment accuracy, resulting in a 30-50% reduction in recurring denial types and improved collections from previously rejected claims.
What are the reported denial and collection rates for organizations using HPC’s services?
Many behavioral health organizations using HPC’s strategies report denial rates below 10% and collection rates exceeding 97%.
What are the key CPT codes for telehealth services that clinics should know?
Key CPT codes include: 99201-99215: Office or outpatient visits for new and established patients. 90791: Psychiatric diagnostic assessments. 99421-99423: Online digital assessment and management offerings.
How does accurate CPT coding impact revenue for clinics?
Clinics that implement rigorous coding practices have reported revenue increases of up to 30%, highlighting the financial impact of accurate CPT coding.
What are Place of Service (POS) codes and why are they important for telehealth billing?
POS codes indicate where healthcare services are delivered and are crucial for billing accuracy. For telehealth, POS 02 is used for services outside the patient’s home, and POS 10 is for services delivered in the patient’s residence.
How can the correct use of POS codes affect claim rejections?
Clinics that correctly use POS 02 and POS 10 have reported a notable decrease in claim rejections, emphasizing the importance of accurate coding practices.
What additional resources does HPC provide for mental health providers?
HPC offers a comprehensive toolkit designed to simplify administrative processes, providing clear action steps and resources to help therapists navigate invoicing and coding complexities.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting