Revenue Cycle Management Best Practices
10 Essential Revenue Cycle Management Services for Mental Health Clinics

Introduction
In the intricate realm of mental health care, effective revenue cycle management is crucial for maintaining a clinic’s financial health. With rising patient demands and increasing administrative burdens, mental health facilities face significant obstacles, including claim denials and billing inaccuracies, that threaten their financial health. This article examines ten essential revenue cycle management services that streamline operations and enhance financial performance, ensuring that clinics can focus on what truly matters – providing high-quality patient care.
How can mental health practices effectively utilize these services to succeed in a dynamic healthcare landscape?
Healthcare Partners Consulting: Comprehensive Administrative Support for Revenue Cycle Management
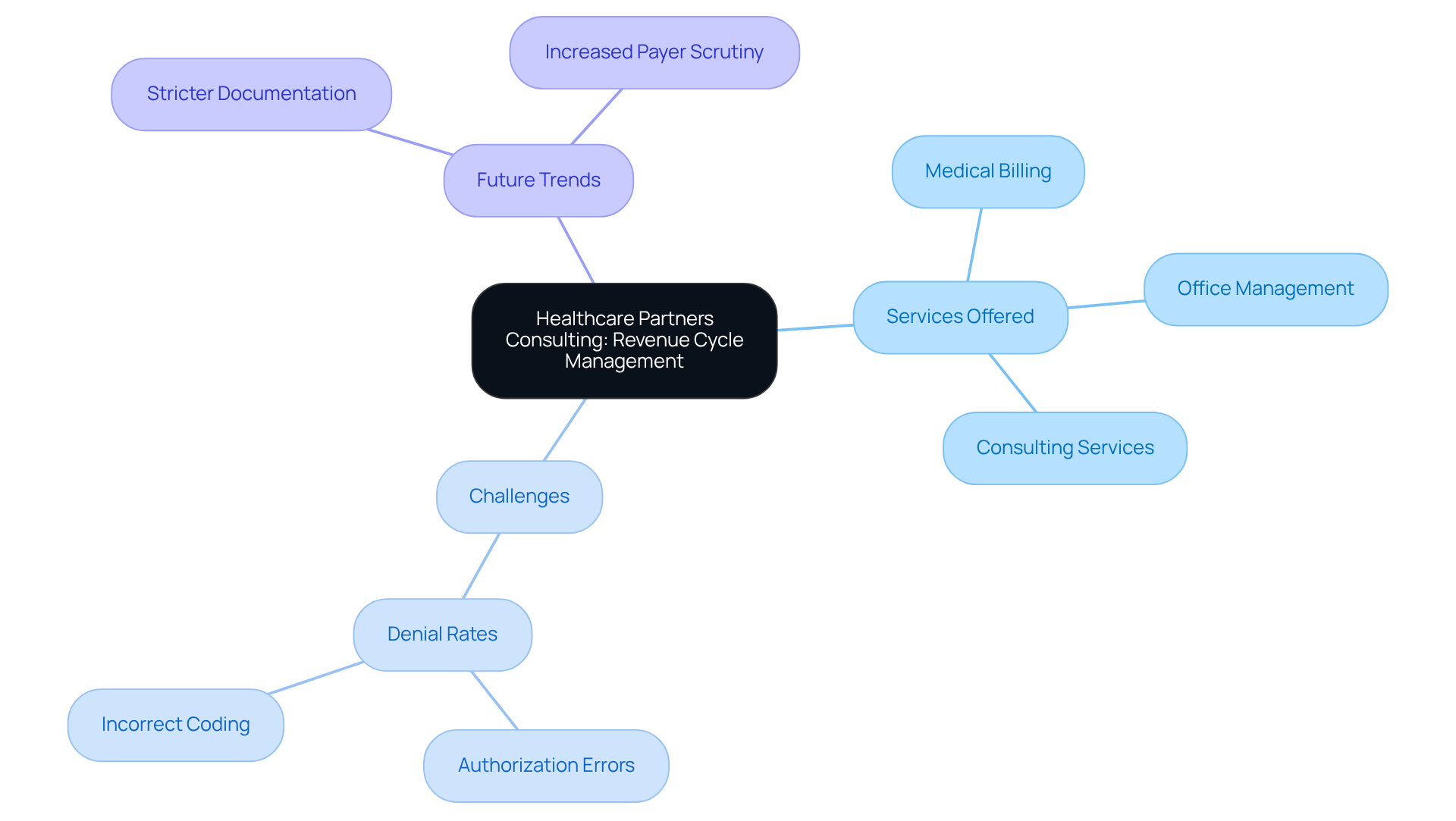
Healthcare Partners Consulting (HPC) addresses the critical challenges faced by wellness clinics in managing administrative and billing services across the United States. Their extensive offerings encompass medical billing, office management, and consulting services, all meticulously designed to reduce the administrative burdens that can detract from patient care. HPC optimizes operations, allowing mental wellness practices to concentrate on delivering high-quality care. This also helps them manage their revenue cycles more efficiently.
Comprehensive administrative support significantly influences revenue cycle management services. Mental wellness practices often encounter denial rates varying from 15 to 25 percent due to frequent issues such as authorization errors and incorrect coding. These denial rates can severely hinder cash flow and operational efficiency. Leveraging HPC’s expertise allows clinics to tackle these challenges head-on, ensuring accurate and efficient claims processing. This includes proactive follow-ups on aging claims and submitting appeals for denied or underpaid claims, which are crucial for improving cash flow and reducing write-offs.
Expert opinions underscore the necessity of robust administrative services in healthcare. As the demand for mental services continues to rise, with behavioral visits surpassing primary care appointments, the need for streamlined billing processes becomes increasingly critical. The successful implementation of HPC’s revenue cycle management services has been shown to enhance financial performance, allowing practices to maintain compliance with evolving regulations and focus on patient engagement.
In 2026, psychological billing will evolve, facing stricter documentation requirements and increased payer scrutiny. HPC’s comprehensive billing services not only assist facilities in navigating these complexities but also position them for sustainable growth. By outsourcing billing functions, psychological practices can achieve better financial results, reduce administrative overhead, and ultimately enhance patient care delivery. As the industry evolves, practices that adapt to these changes will not only survive but thrive in delivering exceptional patient care.
Expert Medical Billing Services: Ensuring Accurate Claims and Timely Payments
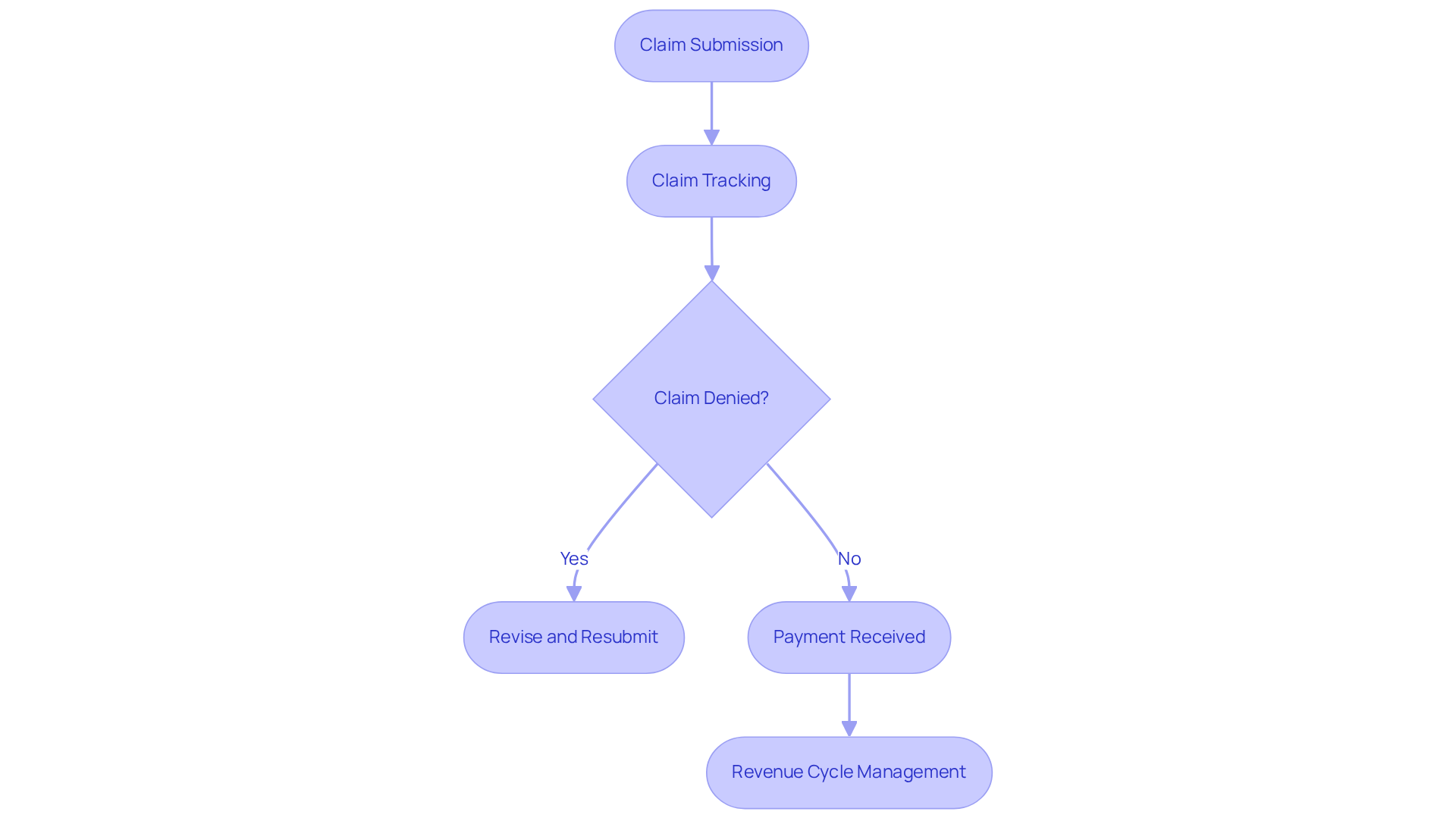
In the evolving landscape of mental health care, specialized medical billing services have become indispensable for ensuring financial viability. Healthcare Partners Consulting (HPC) employs experienced billing professionals who are well-versed in the complexities of mental health billing codes and payer requirements. This expertise significantly reduces claim denials, which have risen by 26% recently, while also accelerating cash flow and enhancing stability for practices.
The meticulous tracking of claims from submission to payment ensures that providers receive the revenue they deserve for their services. A billing expert emphasizes that without proactive measures, practices face the risk of denied claims, lost revenue, and compliance issues.
The integration of updated CPT codes and modifiers in 2026 will further streamline the billing process, necessitating that medical facilities adapt their workflows. Ultimately, the strategic use of revenue cycle management services not only safeguards revenue but also empowers practices to prioritize patient care.
Denial Management Services: Reducing Revenue Loss Through Effective Appeals
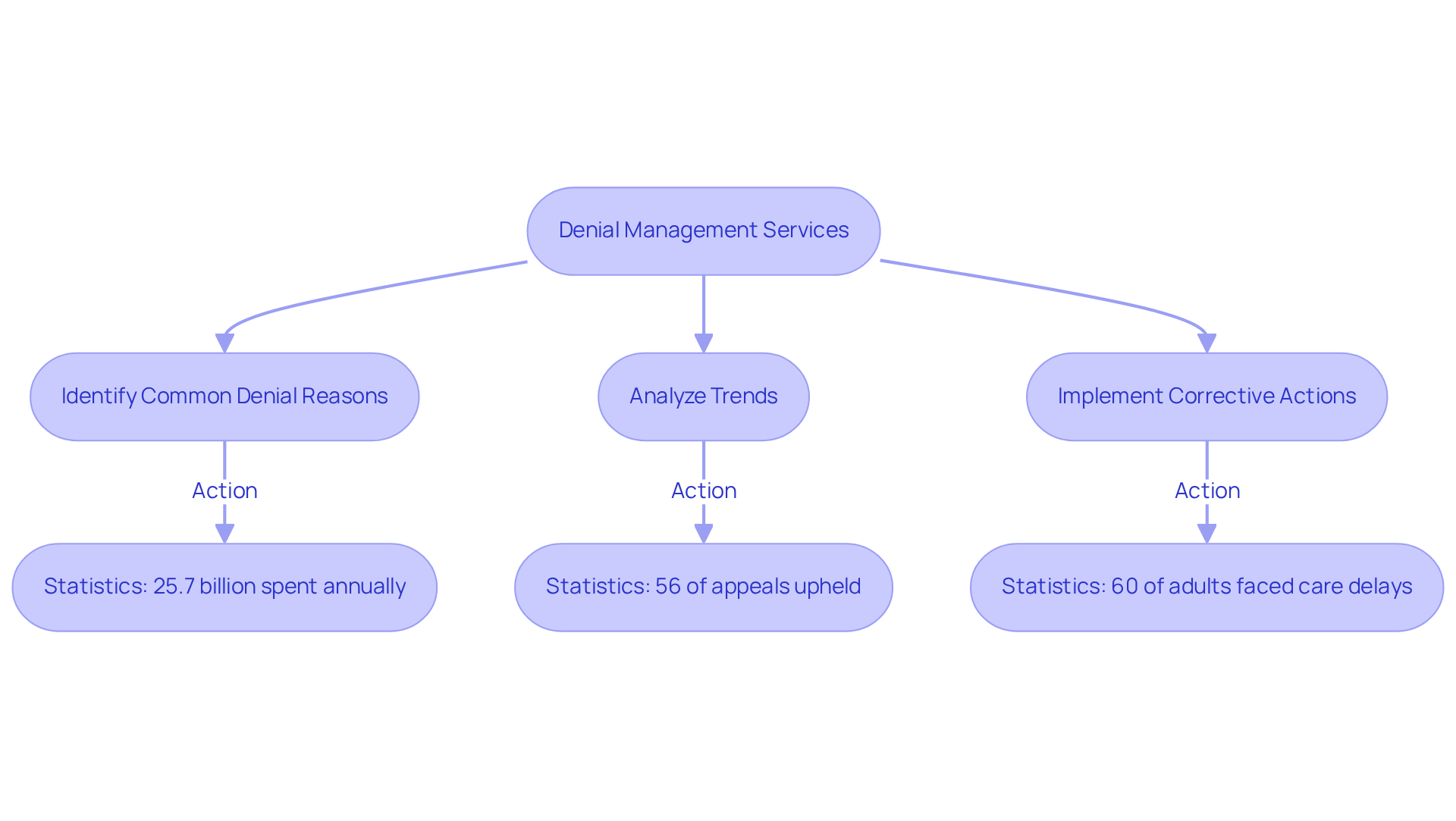
In the face of the ongoing mental health billing crisis, revenue cycle management services have become crucial for mental health facilities seeking to mitigate revenue loss. Healthcare Partners Consulting (HPC) provides robust denial management strategies that encompass:
- Identifying common denial reasons
- Analyzing trends
- Implementing corrective actions
The average appeal success rate for denied claims in healthcare is projected to be critical in 2026, with fewer than 1% of denied ACA marketplace claims appealed in 2023, and insurers upholding 56% of those appeals. Recent statistics underscore the significant financial burden denials impose on operational costs, with providers allocating around $25.7 billion each year on claim adjudication.
By creating effective appeal procedures, facilities can regain lost income and improve their overall economic performance. A proactive strategy not only protects income but also enhances the establishment’s reputation with payers, nurturing better relationships and enabling smoother future transactions. As monetary advisors highlight, “a structured appeals program can recover meaningful revenue,” particularly as many denied claims go unchallenged. Ultimately, a well-structured denial management approach not only safeguards revenue but also strengthens the facility’s standing with payers, paving the way for future financial success through revenue cycle management services.
Patient Billing and Collections: Streamlining Payments for Financial Stability
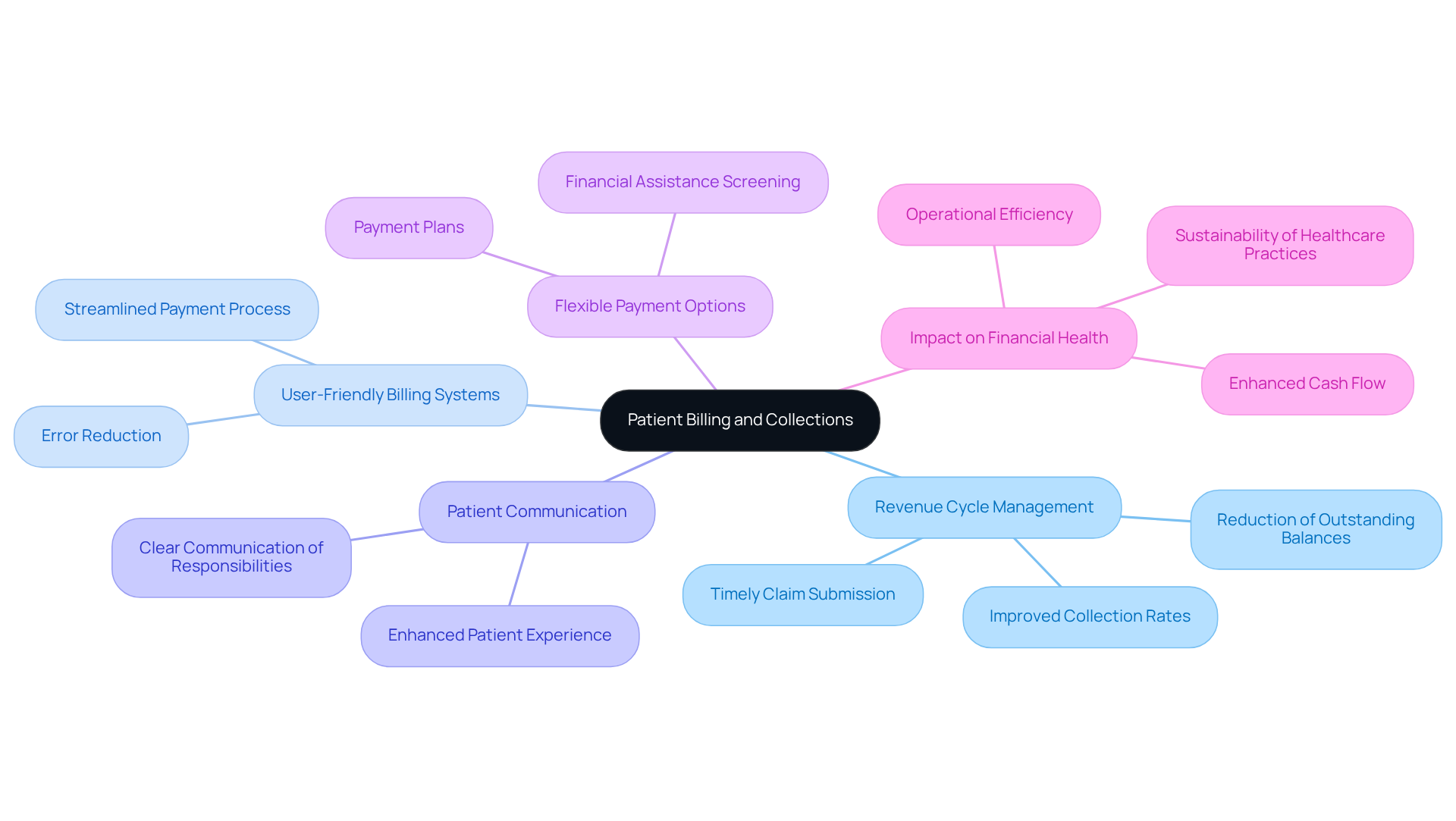
The financial health of mental wellness facilities hinges on optimizing their revenue cycle management services for patient billing and collections. Establishing user-friendly billing systems within our revenue cycle management services streamlines the payment process for patients, ensuring clear communication regarding monetary responsibilities and providing flexible payment options. This proactive approach enhances the patient experience and improves collection rates while reducing outstanding balances.
When facilities nurture trust and satisfaction among patients, they can enhance their cash flow, ultimately supporting their economic stability and operational efficiency. As patient payment responsibilities rise in 2026, effective patient collections will become essential for the sustainability of healthcare practices. Thus, the ability to adapt to rising patient payment responsibilities will determine the future viability of healthcare practices.
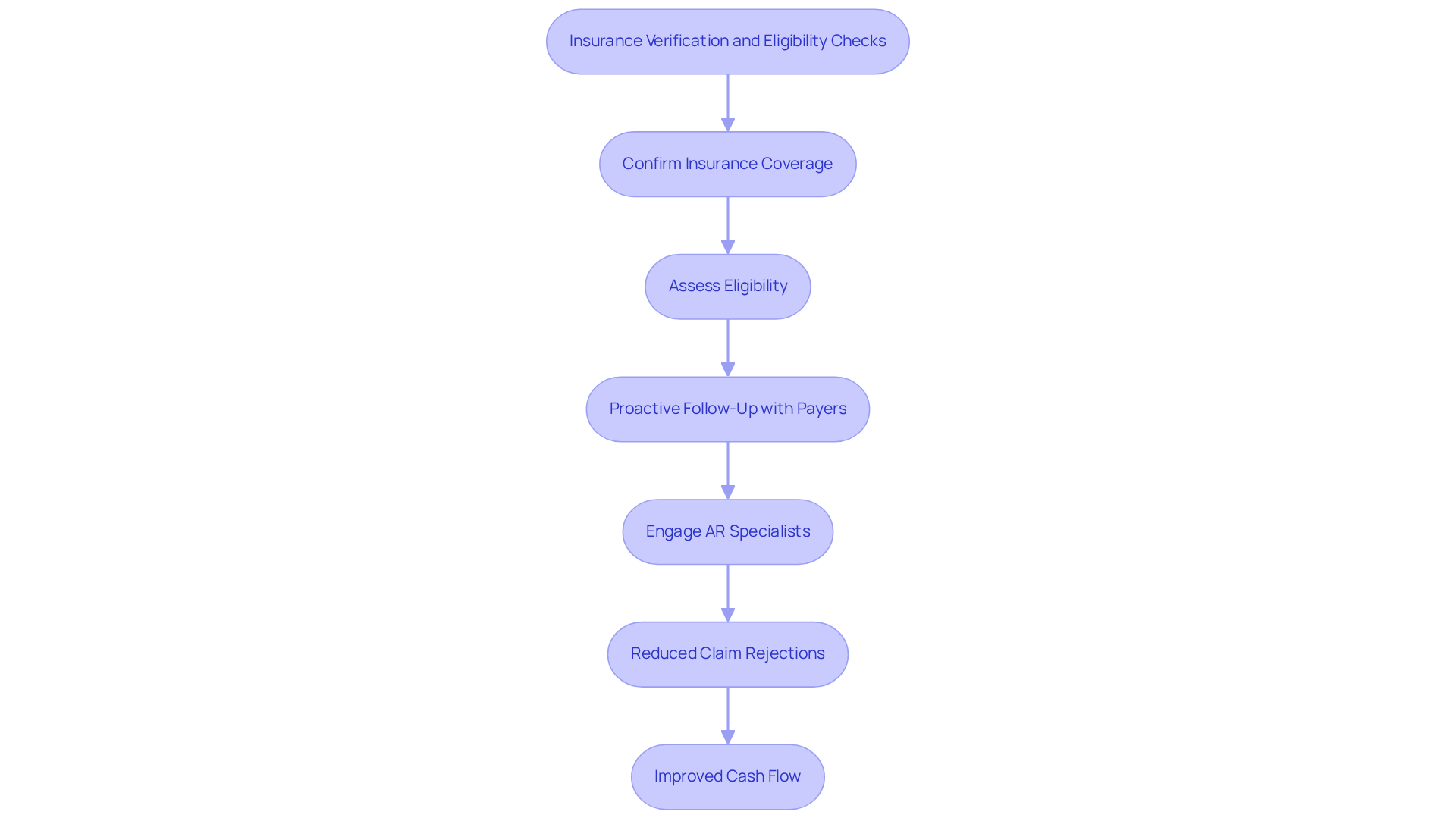
Insurance Verification and Eligibility Checks: Securing Financial Responsibility
In the realm of revenue cycle management services for mental wellness facilities, insurance verification and eligibility assessments play a pivotal role. In 2026, up to 49% of claims are affected by routine coding and documentation issues, underscoring the necessity of confirming patients’ insurance coverage before services are rendered. This proactive strategy reduces the likelihood of claim rejections, which have seen initial denial rates rise to 11.81%. It also ensures monetary accountability in advance, thereby improving cash flow for medical facilities.
Effective verification processes, along with proactive follow-up with payers and dedicated AR specialists from Healthcare Partners Consulting, significantly reduce administrative burdens related to billing discrepancies within revenue cycle management services. This allows practices to concentrate on delivering quality care.
Healthcare compliance experts emphasize the importance of implementing strong eligibility checks, as failure to do so can jeopardize financial stability and operational efficiency in today’s intricate healthcare environment.
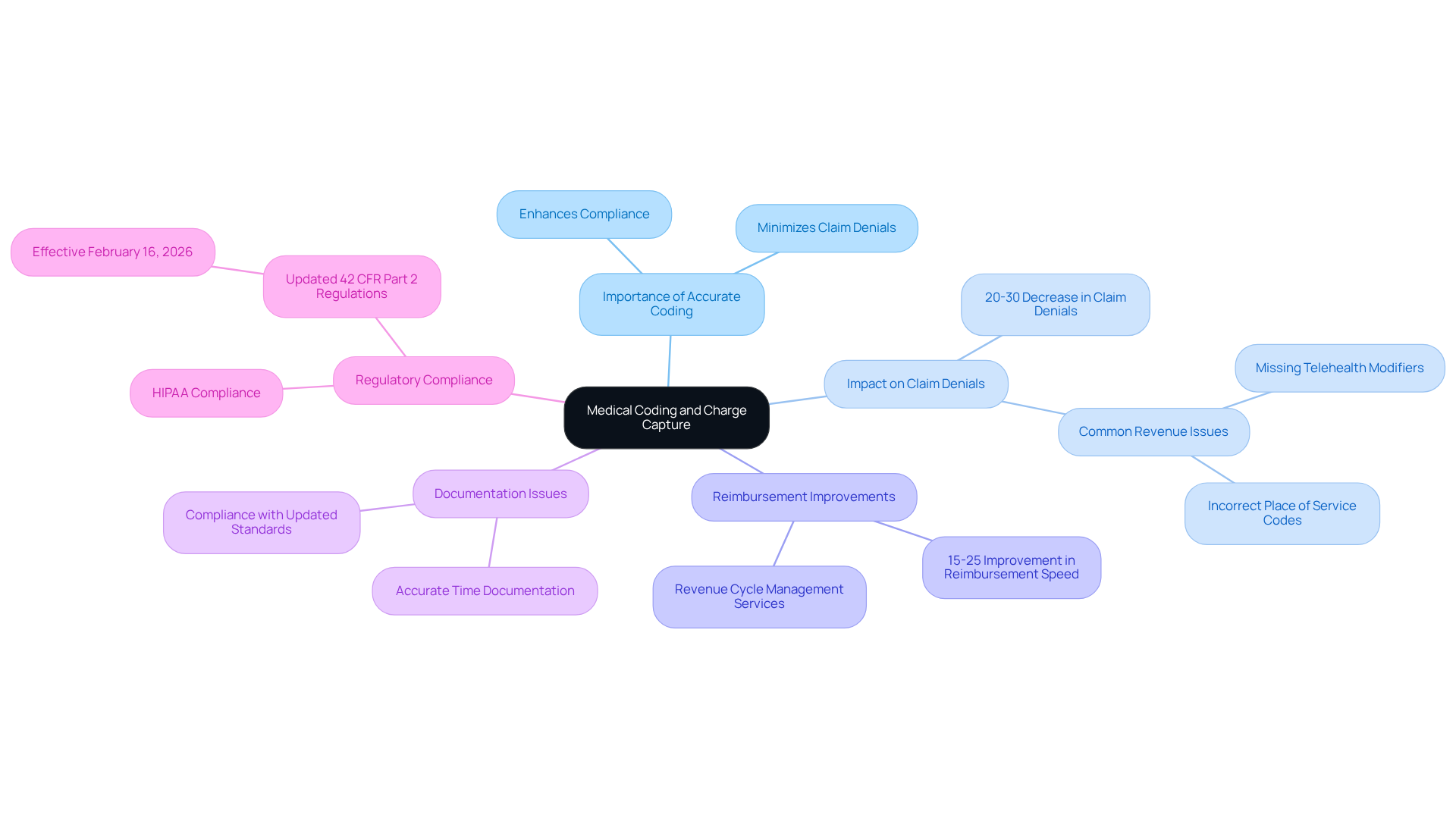
Medical Coding and Charge Capture: Ensuring Accuracy for Successful Claims
Medical coding and charge capture are essential for accurate billing and effective claims submission in behavioral facilities. At Healthcare Partners Consulting (HPC), certified coders are well-versed in the latest coding standards, including the new CPT and HCPCS codes set to take effect on January 1, 2026. This approach minimizes claim denials and accelerates reimbursement processes. Clients typically see a 20-30% decrease in claim denials and a 15-25% improvement in reimbursement speed thanks to our comprehensive revenue cycle management services.
Accurate documentation is crucial to prevent claim denials, particularly given common revenue issues such as missing telehealth modifiers and incorrect place of service codes. Prioritizing accurate coding and adhering to updated practices enhances revenue and ensures compliance with evolving healthcare regulations, including the full enforcement of updated 42 CFR Part 2 regulations effective February 16, 2026.
Effective charge capture methods, supported by our denial management and appeals processes, along with regular performance reporting, are vital for improving claim approval rates and maintaining the financial health of psychological practices through revenue cycle management services.
Payment Posting and Reconciliation: Tracking Revenue for Financial Clarity
Accurate payment posting and reconciliation are essential for maintaining financial integrity in mental wellness facilities. By accurately recording and reconciling all payments received from insurance companies and patients, healthcare practices can effectively utilize revenue cycle management services to track their revenue and identify discrepancies. This meticulous approach enhances fiscal oversight and empowers facilities to make informed operational decisions.
In 2026, over 50% of covered employees will participate in high-deductible insurance plans, emphasizing the need for revenue cycle management services to ensure accurate revenue monitoring amid increased economic scrutiny and patient expectations. Strong payment posting practices allow wellness facilities to maintain precise financial records, which enhances their revenue cycle management services and leads to improved operational efficiency.
Ultimately, the implementation of robust payment practices is crucial for navigating the complexities of modern healthcare finance.
![]()
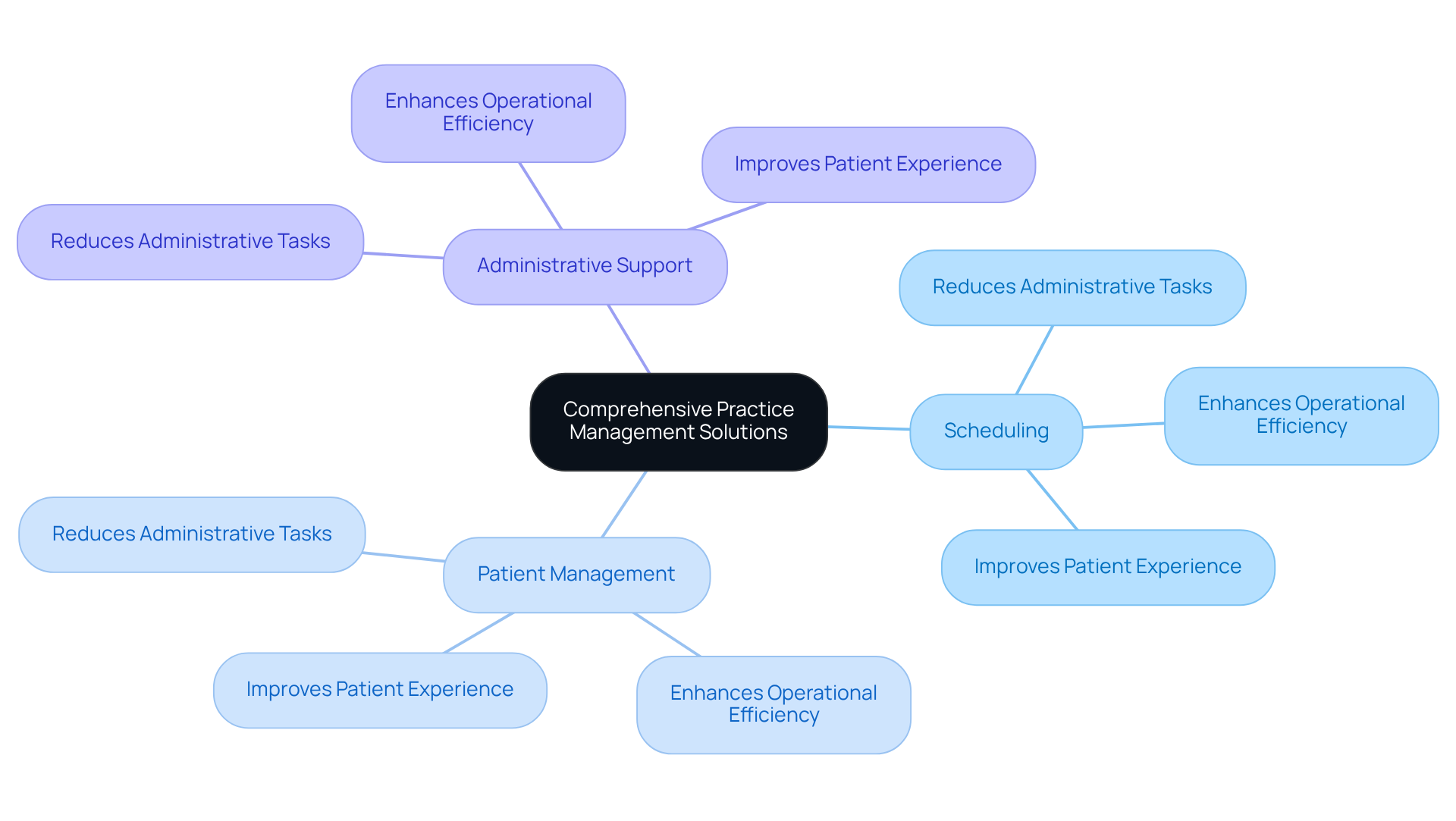
Comprehensive Practice Management Solutions: Streamlining Operations for Efficiency
Effective practice management solutions are essential for optimizing operations in psychological care facilities. At Healthcare Partners Consulting (HPC), we provide a suite of services, including:
- Scheduling
- Patient management
- Administrative support
These services are aimed at reducing administrative tasks for healthcare providers. Implementing these integrated solutions allows healthcare facilities to significantly enhance their operational efficiency, achieving a cost reduction of up to 22% and an efficiency gain of 30%. This comprehensive approach not only strengthens the center’s economic stability but also enhances the patient experience, enabling providers to focus on delivering high-quality care. Consequently, practices can anticipate enhanced clinical outcomes and streamlined workflows. This ultimately leads to increased patient satisfaction and retention.
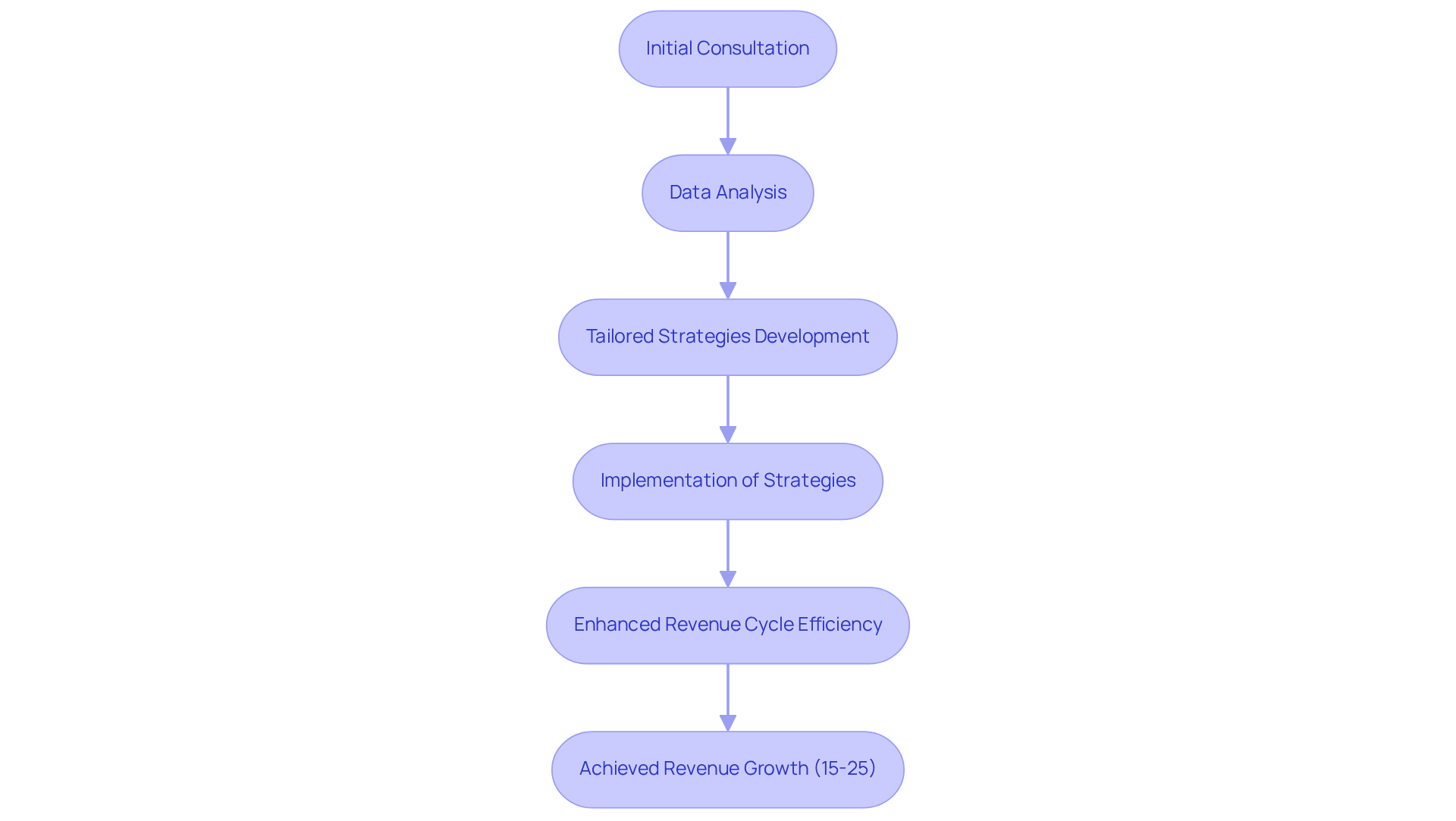
Strategic Consulting Services: Optimizing Revenue Cycle Management for Growth
Strategic consulting services are essential for optimizing revenue cycle management services amidst the complexities of mental health billing. Healthcare Partners Consulting (HPC) offers customized consulting solutions that thoroughly analyze existing practices to identify areas for enhancement.
We initiate our process with a consultation, followed by tailored strategies based on data-driven insights. Clinics can enhance revenue cycle efficiency and reduce costs by implementing automated eligibility verification and systematic denial management within their revenue cycle management services. This proactive approach strengthens economic stability and positions facilities for success in a competitive healthcare landscape.
Clinics that implement these consulting services typically experience an average revenue growth of 15-25% within the first 90 days, demonstrating the tangible benefits of informed decision-making and strategic planning. Healthcare consultant Bhushan Pawar emphasizes that ‘data-driven insights are vital for healthcare facilities seeking to improve their financial performance and operational efficiency.’
With HPC’s emphasis on customized assistance, psychological practices can manage the intricacies of billing with enhanced precision and effectiveness.
Technology Integration: Enhancing Revenue Cycle Management Through Innovation
The integration of technology is revolutionizing revenue cycle management services within mental health facilities. Healthcare Partners Consulting (HPC) leverages advanced software solutions that automate billing processes, streamline claims submissions, and enhance data accuracy. Adopting these advanced technologies enables healthcare facilities to reduce administrative burdens and errors, thereby improving operational efficiency.
HPC’s comprehensive revenue cycle management services encompass:
- Monthly reconciliation and AR trending analysis
- Structured payment plans coordination
- Timely reimbursements
This enables healthcare facilities to adapt to the changing dynamics of the healthcare sector. This integration positions clinics to maintain competitiveness and financial sustainability while improving cash flow and facilitating strategic growth.
Conclusion
Effective revenue cycle management services are essential for the sustainability of mental health clinics. By employing comprehensive strategies that encompass billing, denial management, patient collections, and technology integration, clinics can navigate the intricate financial landscape of healthcare while prioritizing patient care. The goal is to create a seamless experience that not only enhances financial stability but also fosters a supportive environment for mental health treatment.
Throughout the discussion, key points have highlighted the necessity of:
- Expert medical billing services
- Robust denial management strategies
- The importance of accurate coding and insurance verification
Each of these elements plays a crucial role in reducing claim denials, improving cash flow, and streamlining administrative processes. As mental health services continue to grow in demand, the need for innovative solutions and strategic consulting becomes increasingly vital for clinics aiming to thrive.
Ultimately, the integration of advanced technologies and tailored consulting services will empower mental health facilities to enhance their operational efficiency and financial performance. Investing in these strategies is not merely beneficial; it is essential for clinics to remain competitive and effective in delivering care.
Frequently Asked Questions
What services does Healthcare Partners Consulting (HPC) provide for wellness clinics?
HPC offers comprehensive administrative support that includes medical billing, office management, and consulting services designed to reduce administrative burdens and enhance patient care.
How does HPC help improve revenue cycle management for mental wellness practices?
HPC optimizes operations by addressing common issues like authorization errors and incorrect coding, which can lead to high denial rates. They ensure accurate claims processing, proactive follow-ups on aging claims, and submitting appeals for denied or underpaid claims.
What are the typical denial rates faced by mental wellness practices?
Denial rates can vary from 15 to 25 percent due to issues such as authorization errors and incorrect coding.
Why is robust administrative support necessary in healthcare, especially for mental health services?
As the demand for mental health services increases, streamlined billing processes become critical to maintaining cash flow and operational efficiency, allowing practices to focus on patient engagement.
What changes are expected in psychological billing by 2026?
Psychological billing will face stricter documentation requirements and increased payer scrutiny, making it essential for practices to adapt their billing processes to navigate these complexities.
How do expert medical billing services benefit mental health practices?
Expert billing services reduce claim denials, accelerate cash flow, and enhance financial stability by ensuring accurate claims and timely payments, which are crucial for the viability of practices.
What is the impact of denied claims on healthcare providers?
Denied claims can lead to lost revenue, compliance issues, and increased operational costs, with providers spending approximately $25.7 billion annually on claim adjudication.
What strategies does HPC employ for denial management?
HPC identifies common denial reasons, analyzes trends, and implements corrective actions to reduce revenue loss and improve financial performance.
What is the projected appeal success rate for denied claims in 2026?
The average appeal success rate for denied claims is anticipated to be critical, with fewer than 1% of denied ACA marketplace claims appealed in 2023 and insurers upholding 56% of those appeals.
How can a structured appeals program benefit healthcare facilities?
A structured appeals program can recover significant revenue, enhance the facility’s reputation with payers, and facilitate smoother future transactions, ultimately improving financial success through effective revenue cycle management.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting