Mastering Medical Coding
10 Essential General Surgery Code Alerts for 2026 Compliance

Introduction
The upcoming changes in the CPT 2026 code set will significantly impact general surgery practices, necessitating immediate attention from practitioners. With the introduction of:
- 288 new codes
- 46 revisions
- 84 deletions
These updates will take effect on January 1, 2026. Practices that do not adapt to these changes may encounter serious billing inaccuracies and compliance issues. How can general surgery professionals effectively equip themselves to meet these new coding requirements and safeguard their practices against potential pitfalls?
CPT 2026 Coding Changes for General Surgery
The introduction of the CPT 2026 code set presents critical updates for general surgery professionals. This update includes:
- 288 new codes
- 46 revisions
- 84 deletions
Key changes consist of new codes for procedures like endoscopic sleeve gastroplasty. Additionally, existing codes have been updated to reflect advancements in surgical techniques. Notably, the term ‘peritoneoscopy’ has been removed from all instances in the CPT code set for 2026.
These modifications will take effect on January 1, 2026, requiring organizations to update their billing systems and training to ensure compliance and accuracy in invoicing. Organizations may face challenges in adapting to the new coding requirements. Failure to adapt could lead to billing inaccuracies and compliance issues.
Importance of Accurate CPT Coding in General Surgery
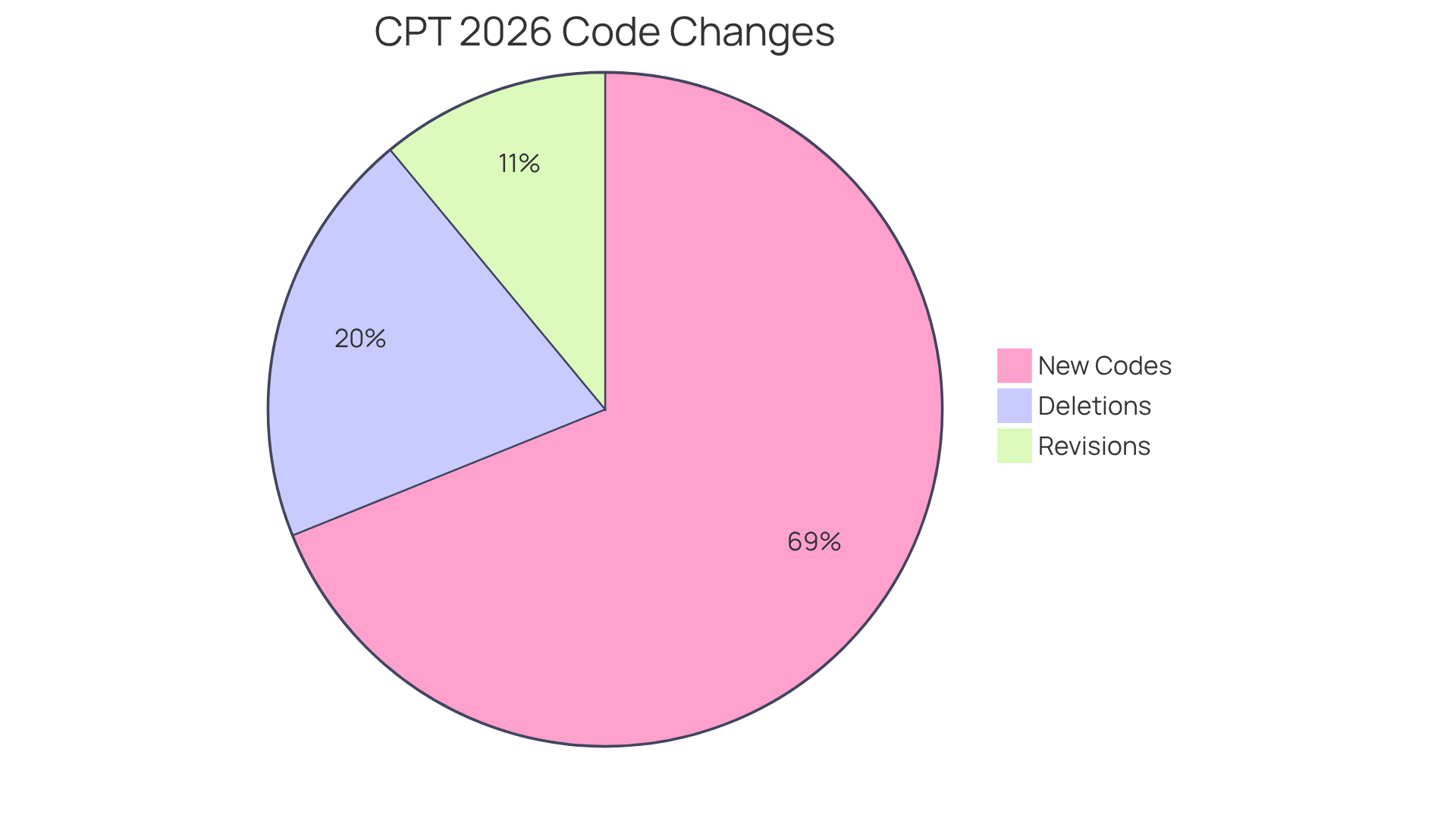
The financial health of general surgery practices depends on accurate CPT classification, particularly with the recent general surgery code alert. Flawed programming leads to significant operational challenges that strain resources and affect patient care. For instance, a denial rate exceeding 10 percent often indicates issues with documentation or programming that require immediate action. Ensuring that programming aligns with the services offered not only supports proper reimbursement but also enhances the overall efficiency of the practice.
Healthcare Partners Consulting examines and rectifies billing issues before claims are submitted, significantly reducing errors from the start. By adhering to payer-specific guidelines and staying current with CPT, ICD-10, and HCPCS updates, HPC assists in maintaining high standards of accuracy in classification. Our team is trained in the nuances of behavioral health classification, including:
- 90791/90837
- E/M codes
- Incident-to rules
- Supervision requirements
Ongoing training and audits, combined with quality assurance and peer reviews, help maintain compliance and ensure timely reimbursement. By prioritizing accurate classification, practices can safeguard their financial stability and enhance patient outcomes.
Impact of New Reimbursement Models on General Surgery
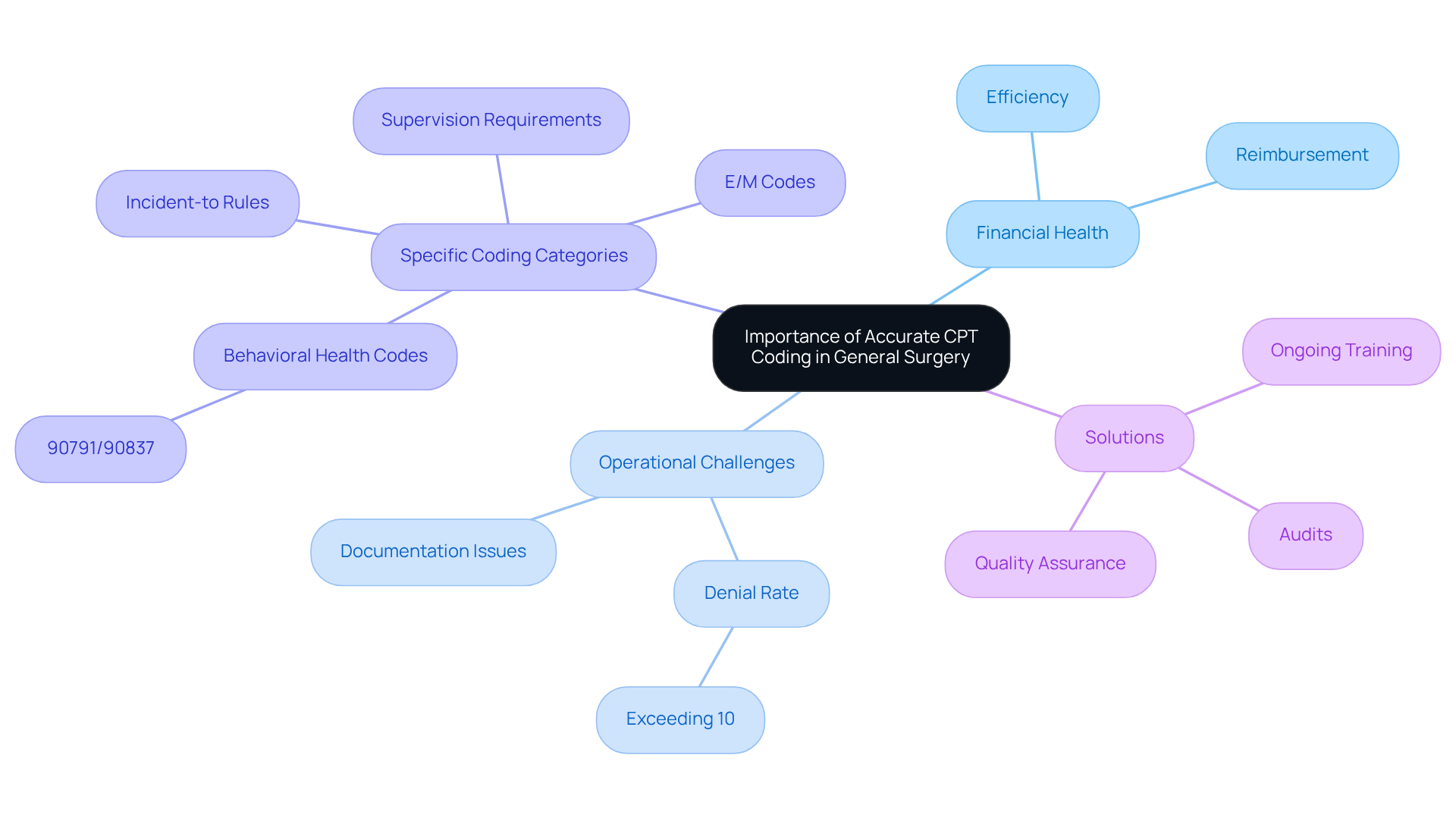
The emergence of value-based care and bundled payments has triggered a general surgery code alert that is reshaping the billing practices within general surgery. These models prioritize the quality of care delivered rather than the volume of services rendered, necessitating that surgeons heed the general surgery code alert and adjust their coding strategies accordingly.
Accurate documentation is essential; it must demonstrate the value of care provided, aligning with these innovative payment structures. This alignment enhances patient outcomes while simultaneously bolstering the financial viability of surgical practices.
For instance, strategies that effectively implement these models are likely to see improvements in reimbursement rates and operational efficiency. As the healthcare landscape evolves, surgeons who proactively embrace these reimbursement models will position themselves for success in an increasingly competitive healthcare market.
Regulatory Compliance Updates for General Surgery Practices
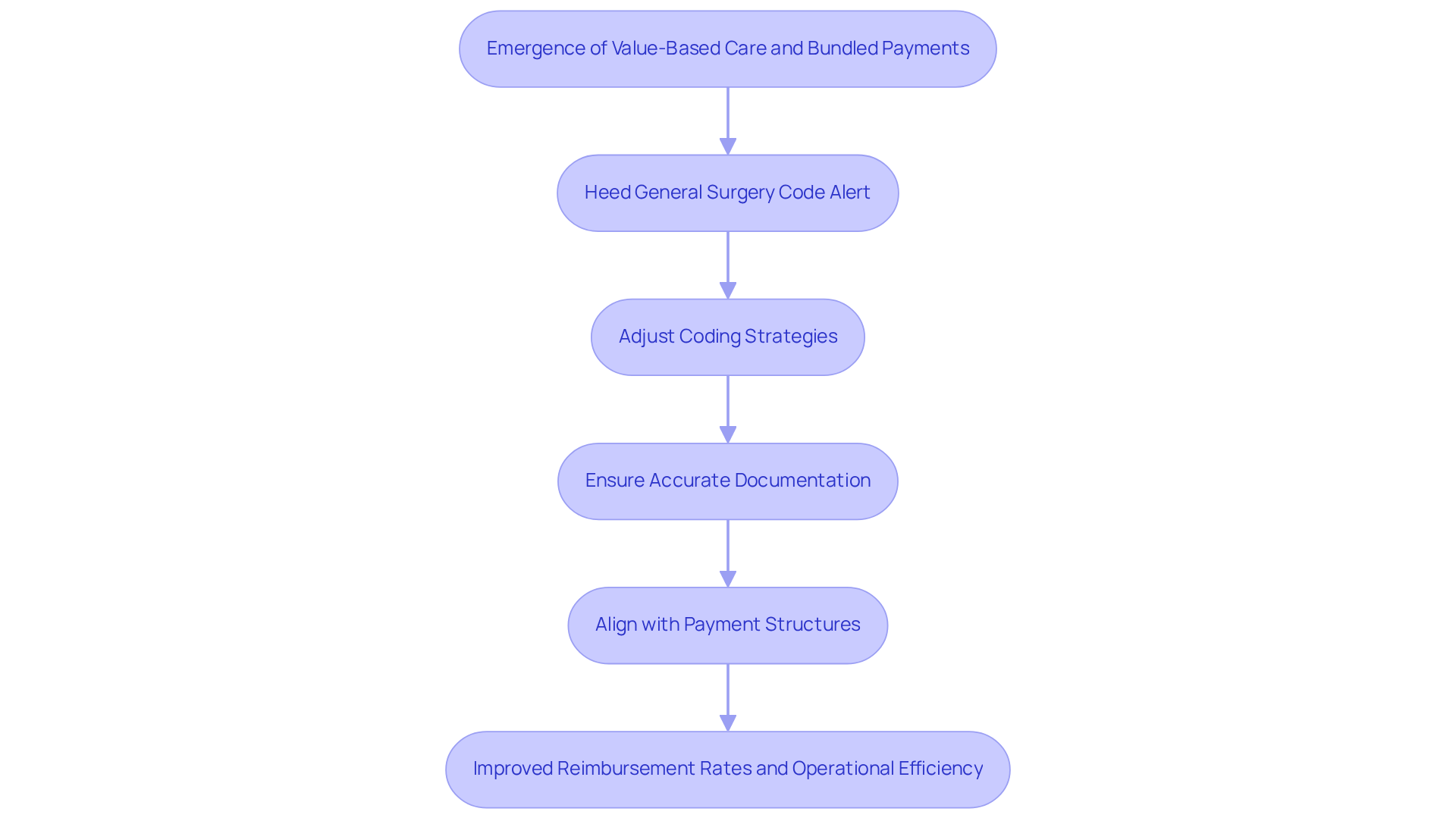
In 2026, the landscape of general surgical procedures will undergo significant regulatory changes that will impact billing methods directly. New record-keeping requirements and coding guidelines have been introduced to ensure alignment with the latest CPT codes, significantly impacting billing methods. These modifications necessitate that organizations establish robust adherence programs, which should include regular training sessions for staff to ensure they are well-informed about the updates. This proactive approach is crucial for addressing risks of non-compliance, which can lead to audits and financial penalties.
For instance, methods that do not meet the revised record standards may face increased scrutiny during audits, resulting in costly consequences. Furthermore, implementing effective denial management strategies – such as analyzing trends to address root causes and refining workflows – can lead to a 30-50% reduction in recurring denial types. This ultimately enhances revenue recovery and ensures smoother operations for healthcare providers. Thus, proactive adaptation to these changes is not merely beneficial but essential for sustaining compliance and operational success in the evolving healthcare environment.
Enhancing Documentation Quality for Accurate Coding
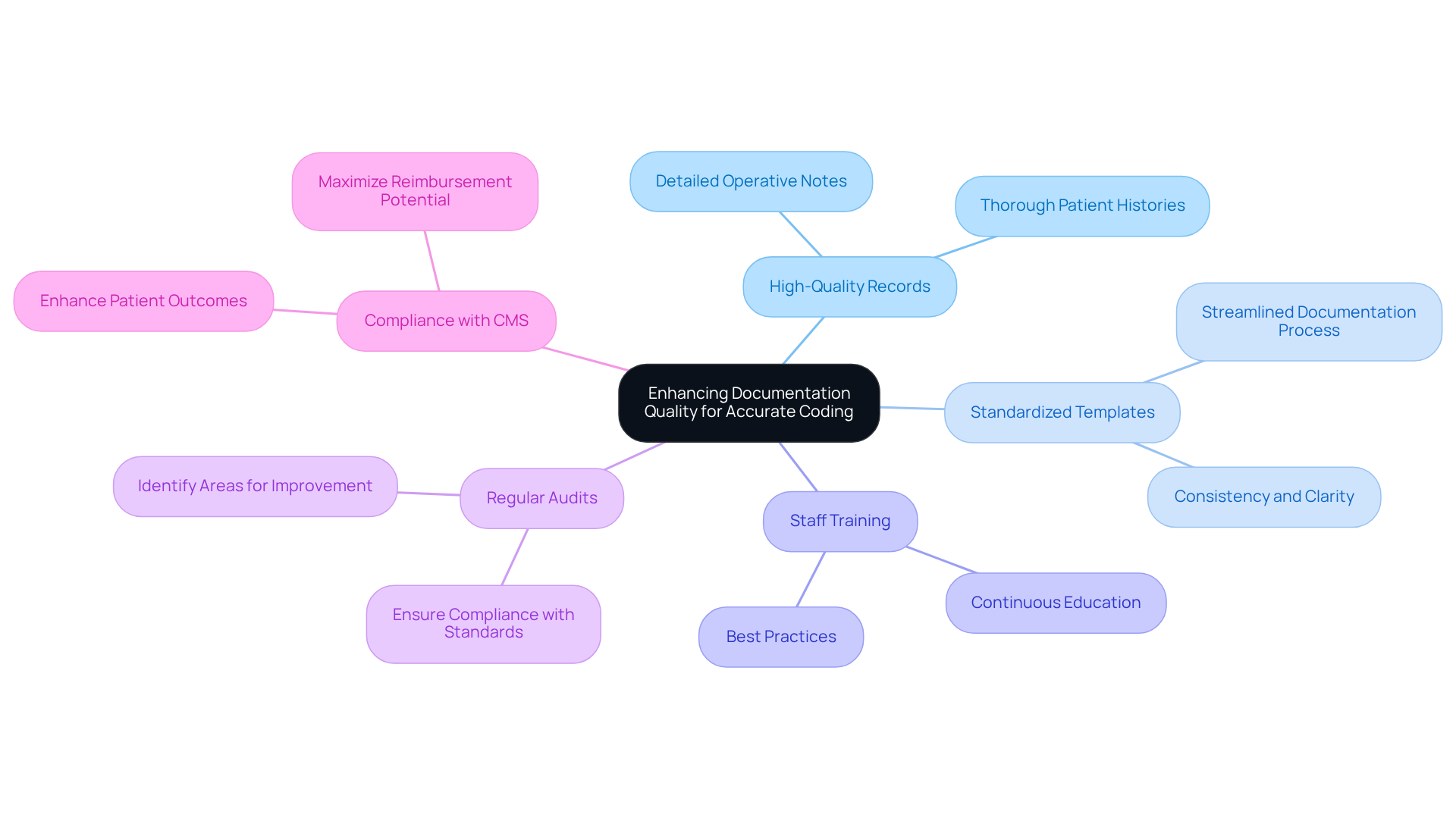
To attain precise recording in general surgery, methods must highlight the significance of high-quality records. This involves creating detailed operative notes with clear procedure descriptions and thorough patient histories. Standardized templates can streamline this process, ensuring consistency and clarity in documentation.
Regular staff training is crucial for keeping everyone informed about best practices and coding requirements. Additionally, regular audits are vital for identifying areas for improvement, ensuring compliance with regulatory standards and maximizing reimbursement potential.
The Centers for Medicare & Medicaid Services (CMS) highlights that maintaining compliance in clinical records is crucial for improving patient outcomes, emphasizing the need for precise record-keeping processes.
Case studies demonstrate that practices implementing these strategies see marked improvements in accuracy and financial outcomes, highlighting the critical role of meticulous record-keeping in surgical settings.
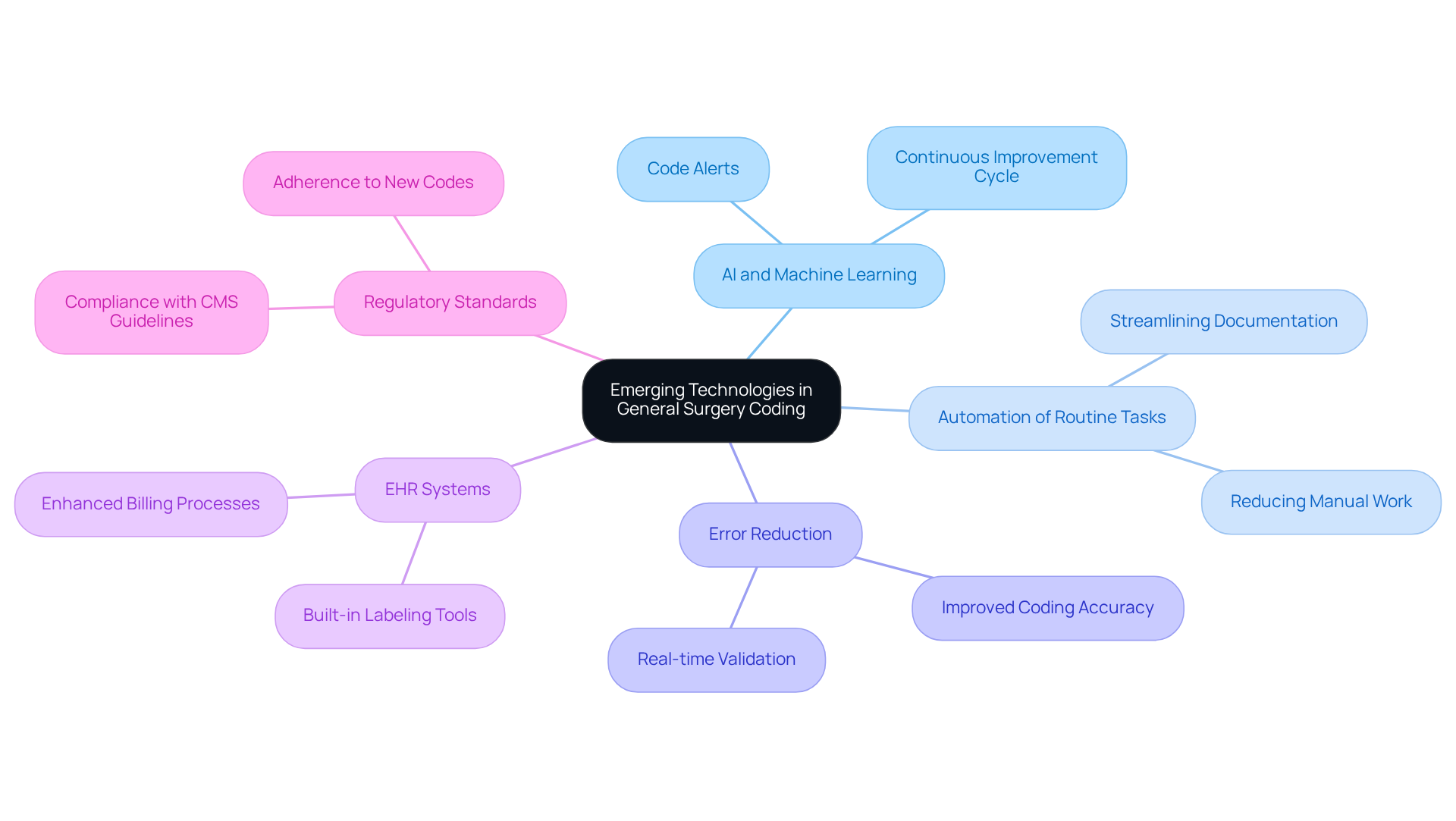
Emerging Technologies Impacting General Surgery Coding
The integration of emerging technologies in general surgery documentation presents both challenges and opportunities for improvement. Artificial intelligence (AI) and machine learning are transforming this field by automating routine tasks and enhancing accuracy. These technologies assist coders in identifying the correct codes through a general surgery code alert based on documentation, thereby reducing the likelihood of errors. Furthermore, electronic health record (EHR) systems equipped with built-in labeling tools simplify the labeling process, which leads to more effective billing and improved adherence to regulatory standards. Ultimately, the adoption of AI and machine learning in surgical documentation could redefine accuracy and efficiency in healthcare billing practices.
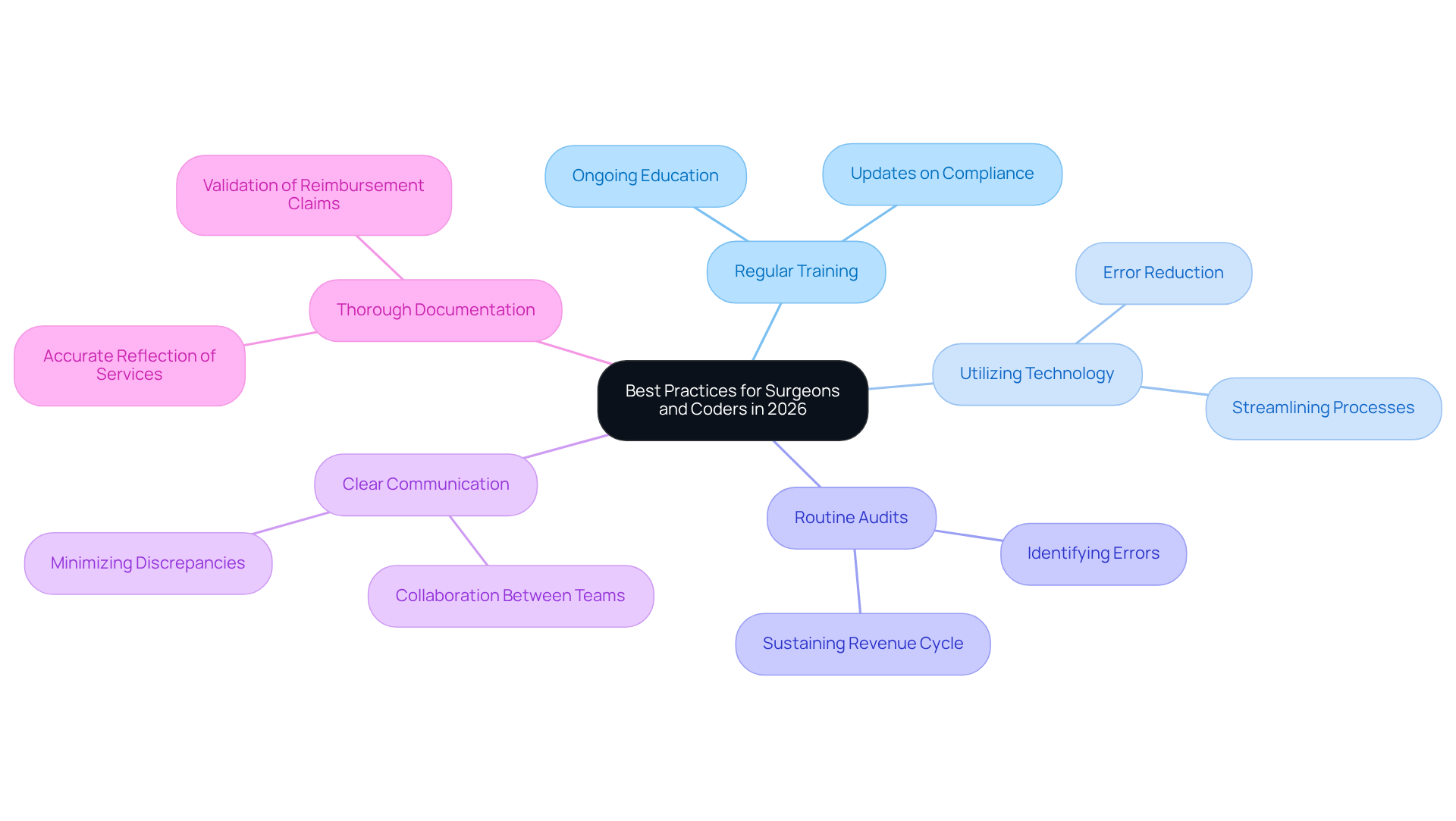
Best Practices for Surgeons and Coders in 2026
In the rapidly evolving landscape of healthcare coding, the implementation of best practices is essential for success in 2026. To enhance coding practices, surgeons and coders should implement several best practices:
- Regular Training: Ongoing education on new programming updates and compliance requirements is crucial. This training keeps coding professionals updated on changes, ensuring billing and documentation accuracy.
- Utilizing Technology: Leveraging advanced technology can streamline programming processes, reducing the likelihood of errors and improving efficiency. Automated systems can assist in maintaining compliance with evolving regulations.
- Routine Audits: Conducting regular audits is essential for identifying and rectifying programming errors. These audits help practices sustain a clear revenue cycle and evade possible penalties linked to inaccurate labeling.
- Clear Communication: Establishing effective communication between surgical teams and billing staff is vital. This collaboration ensures that all services provided are accurately documented and coded, minimizing discrepancies.
- Thorough Documentation: Maintaining comprehensive documentation that accurately reflects the services rendered is critical. This method not only enhances programming precision but also assists in validating reimbursement claims during audits.
Ultimately, these strategies not only enhance billing accuracy but also contribute to the financial health of surgical facilities.
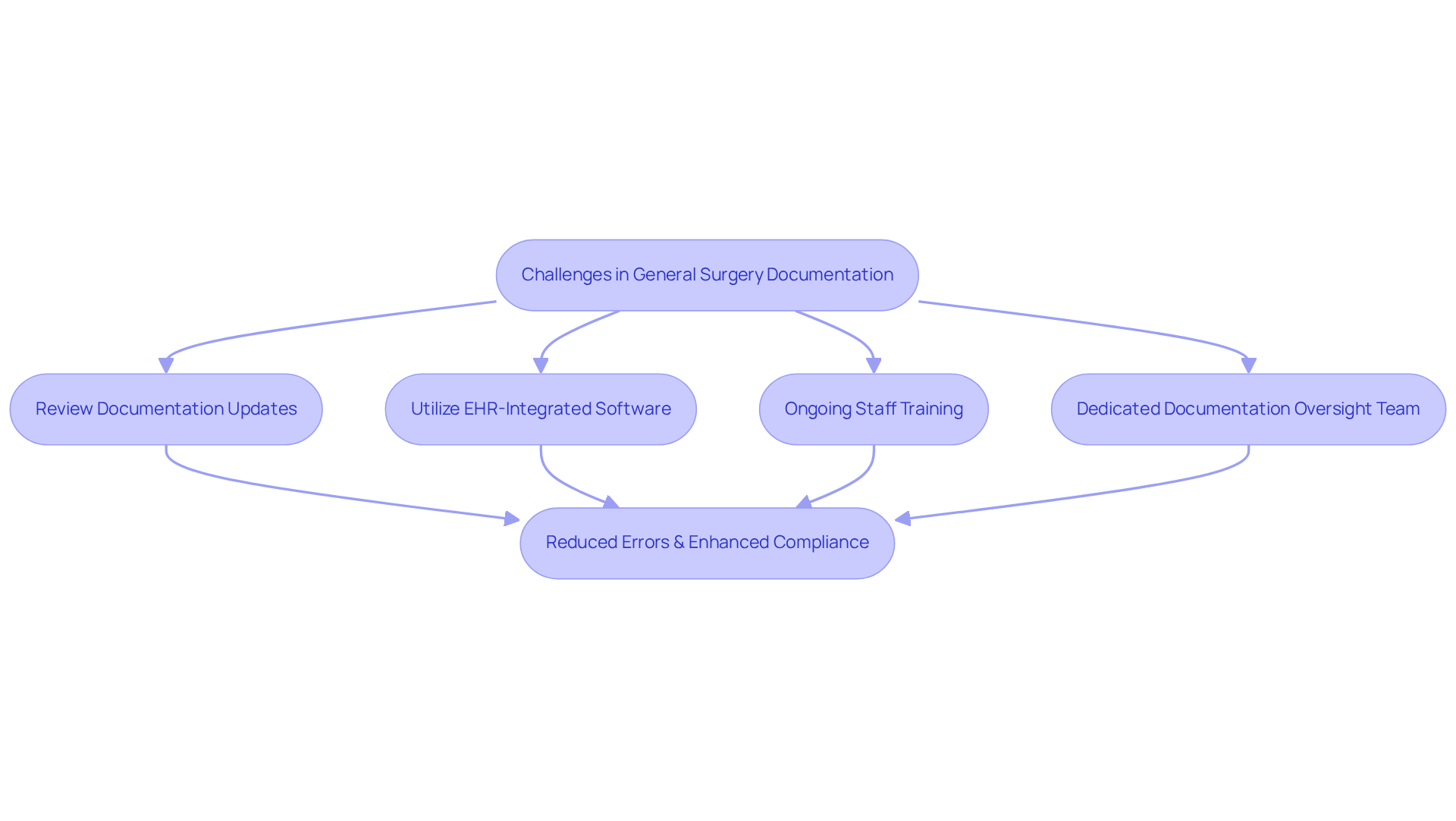
Navigating Coding Complexity in General Surgery
The intricate nature of general surgery classification presents challenges in maintaining accurate documentation. To address these challenges, a systematic approach is essential. This includes:
- Regularly reviewing updates in documentation
- Utilizing software that integrates with EHR systems
- Providing ongoing staff training
- Establishing a dedicated team to oversee documentation standards
Implementing these strategies not only mitigates errors but also enhances financial performance and compliance with regulations. Healthcare Partners Consulting optimizes operations for medical and mental health facilities, providing administrative assistance to manage these complexities effectively.
Healthcare Partners Consulting: Tailored Support for General Surgery Coding
Healthcare Partners Consulting (HPC) addresses the critical challenges faced by general surgery offices through the implementation of a general surgery code alert for managing coding and billing processes. Their comprehensive services include expert medical billing, customized management solutions, and dedicated virtual assistants who handle administrative tasks.
Collaborating with HPC enables surgical facilities to streamline operations effectively, thereby alleviating administrative burdens that detract from patient care. This partnership not only improves revenue cycle management but also leads to measurable enhancements in operational efficiency.
For instance, facilities utilizing HPC’s consulting services have documented significant enhancements in their revenue cycle management, with some achieving up to a 30% increase in revenue. Furthermore, surgical facilities leveraging HPC’s expertise in billing have experienced a 30-50% reduction in recurring denial categories and a 40% faster claims processing time.
HPC’s denial management strategies safeguard practice revenue by recovering previously denied claims and refining workflows to prevent future denials. As Kritesh Patel, Co-President of Operations at HPC, stated, “These innovative solutions will allow us to reduce administrative burdens and provide even greater value to our clients.”
For further insights into optimizing surgical billing processes and improving financial performance, please refer to our FAQ page or contact us directly.
Continuous Education for Coding Professionals in General Surgery
Continuous education is vital for professionals in general surgery, particularly in navigating the complexities of the evolving billing landscape. Participation in workshops, webinars, and certification courses focused on the latest programming updates and compliance requirements is crucial. Research indicates that investing in ongoing education leads to a significant reduction in programming errors, which correlates with improved financial outcomes. For instance, case studies show that surgical practices that regularly engage in educational programs report a 25% decrease in claim denials, highlighting the necessity of staying informed.
Furthermore, the latest workshops and webinars provide updates on programming changes, ensuring that professionals are equipped with the most current knowledge. Specialist insights emphasize that such training not only enhances programming accuracy but also fosters a culture of compliance within operations, ultimately leading to improved patient care and operational efficiency. Moreover, errors in medical coding can result in claim denials, delayed payments, and a heavier administrative burden. Healthcare Partners Consulting addresses these challenges by identifying and correcting coding issues before claims submission, ensuring adherence to payer-specific guidelines and remaining current on CPT, ICD-10, and HCPCS revisions. This proactive approach significantly reduces errors from the outset, enhancing accuracy and compliance in healthcare practices.
Conclusion
The impending changes in the CPT coding system for general surgery in 2026 present both challenges and opportunities for healthcare professionals. Surgical practices must proactively update their coding strategies in response to new codes, revisions, and deletions to prevent billing inaccuracies and compliance issues.
Throughout the article, several key points highlight the importance of accurate coding, including:
- The financial implications of coding errors
- The impact of new reimbursement models
- The need for continuous education and training
Emphasizing thorough documentation and integrating emerging technologies will significantly improve the accuracy of coding practices, ultimately leading to better patient care and financial health for surgical facilities.
As the healthcare landscape continues to evolve, embracing these changes is essential for success. Surgeons and coding professionals must prioritize ongoing education and implement best practices to navigate the complexities of coding effectively. By doing so, they can ensure compliance with the latest regulations, enhance their revenue cycle management, and ultimately provide higher quality care to their patients. Ultimately, those who embrace these changes will not only ensure compliance but also enhance the quality of care they provide.
Frequently Asked Questions
What are the main updates in the CPT 2026 code set for general surgery?
The CPT 2026 code set includes 288 new codes, 46 revisions, and 84 deletions, with notable changes such as new codes for procedures like endoscopic sleeve gastroplasty and the removal of the term ‘peritoneoscopy’ from all instances.
When do the changes to the CPT 2026 code set take effect?
The changes will take effect on January 1, 2026.
Why is accurate CPT coding important for general surgery practices?
Accurate CPT coding is crucial for the financial health of general surgery practices as it supports proper reimbursement, enhances operational efficiency, and reduces the risk of billing inaccuracies and compliance issues.
What challenges might organizations face with the new coding requirements?
Organizations may encounter difficulties in adapting their billing systems and training to comply with the new coding requirements, which could lead to billing inaccuracies and compliance issues if not addressed.
How can healthcare consulting services help with billing issues?
Healthcare Partners Consulting examines and rectifies billing issues before claims are submitted, reducing errors and ensuring that programming aligns with the services offered, which supports proper reimbursement.
What impact do new reimbursement models have on general surgery?
New reimbursement models, such as value-based care and bundled payments, require surgeons to adjust their coding strategies to prioritize the quality of care over the volume of services, enhancing patient outcomes and financial viability.
What is necessary for surgeons to align with new reimbursement models?
Surgeons must ensure accurate documentation that demonstrates the value of care provided, aligning with innovative payment structures to improve reimbursement rates and operational efficiency.
Need help applying this?
Talk to a billing specialist who knows your payer mix.
HPC manages the full revenue cycle for medical and mental-health practices across the U.S. Book a call to see what tightening claims, denials, and credentialing could mean for your numbers.
Schedule a meeting